Ectopic Implantation Research
| Embryology - 25 Apr 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
Ectopic pregnancy is a high-risk maternal medical condition with an approximate incidence of 1.5 to 2 % in reported pregnancies. There is some indication that the incidence may be increasing (United States has increased from 4.5 per 1,000 pregnancies in 1970 to an estimated 19.7 per 1,000 pregnancies in 1992[1])
Our research group has established a uterine tube Biobank in order to investigate factors and markers associated with ectopic pregnancies. This page introduces the project and provides some introductory information for students who may wish to carry out an Honours, Independent Research Project or higher degree in the research laboratory.
- Links: Implantation | Week 2 | Placenta - Abnormalities | Trophoblast | Trophoblast Protein Expression
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Ectopic Pregnancy <pubmed limit=5>Ectopic Pregnancy</pubmed> |
About Ectopic Pregnancy
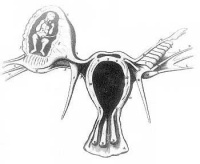
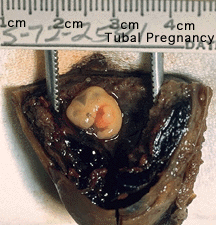
The risk factors for tubal ectopic pregnancy include: tubal damage by infection (particularly Chlamydia trachomatis) or surgery, smoking and in vitro fertilization therapy. Prolonged tubal damage is often described as pelvic inflammatory disease and "scarring" can affect the cilia-mediated transport of the blastocyst during the first week of development. This is also the most common cause of pregnancy-related deaths in the first trimester. A recent United Kingdom enquiry into maternal deaths[3], identified ectopic pregnancy as the fourth most common cause of maternal death (73% of early pregnancy deaths).
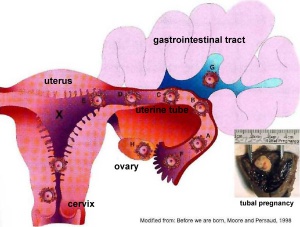
Ectopic sites are named according to the anatomical location: Tubal (Ampullary, Isthmic, Cornual), Cervical and Ovarian. A study of 1800 surgically treated ectopics between 1992 and 2001 identified implantation sites by frequency: interstitial (2.4%), isthmic (12.0%), ampullary (70.0%), fimbrial (11.1%), ovarian (3.2%) or abdominal (1.3%).[4]
International Classification of Diseases
The International Classification of Diseases (ICD) World Health Organization's classification used worldwide as the standard diagnostic tool for epidemiology, health management and clinical purposes.
The two main codes cover O00 Ectopic pregnancy and O01 Hydatidiform mole.
Note that there is an additional code covering complications of the clinical treatment O08 Complications following abortion and ectopic and molar pregnancy This code is provided primarily for morbidity coding. For use of this category reference should be made to the morbidity coding rules and guidelines in Volume 2.
- Links: O00 Ectopic pregnancy | O01 Hydatidiform mole | Chapter XV Pregnancy Childbirth | International Classification of Diseases
Methotrexate
(MTX, amethopterin) Drug with several different uses including the treatment of ectopic pregnancy[5] and for the induction of medical abortions. Acts as a antimetabolite and antifolate (folic acid antagonist) drug that inhibits DNA synthesis in actively dividing cells, including trophoblasts, and therefore has other medical uses include cancer and autoimmune disease treatment. Treatment success in ectopic pregnancy relates to serum β human chorionic gonadotropin (β-hCG) concentration.
- Links: Medline Plus
References
Reviews
<pubmed>20071358</pubmed> <pubmed>20023297</pubmed> <pubmed>16595714</pubmed>
Articles
<pubmed>7194809</pubmed> <pubmed>19978839</pubmed>
Search Pubmed
June 2010
- "ectopic pregnancy" All (14958) Review (1350) Free Full Text (1196)
- "tubal pregnancy" All (8010) Review (683) Free Full Text (630)
Search Pubmed: ectopic pregnancy | ectopic implantation | tubal pregnancy | tubal implantation
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 25) Embryology Ectopic Implantation Research. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Ectopic_Implantation_Research
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G