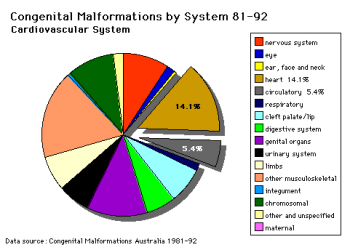
Cardiovascular System - Patent Ductus Arteriosus: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| Line 15: | Line 15: | ||
|-bgcolor="F5FAFF" | |-bgcolor="F5FAFF" | ||
| | | | ||
* '''Noninvasive technique for the diagnosis of patent ductus arteriosus in premature infants by analyzing pulse wave phases on photoplethysmography signals measured in the right hand and the left foot'''<ref name=PMID24892695><pubmed>24892695</pubmed></ref> "To evaluate the impact of patent ductus arteriosus (PDA) on the pulse phase difference (PPD) between the left foot (postductal region) and the right hand (preductal region). PPD was determined from arterial photoplethysmography signals (pulse waves) measured by infrared sensors routinely used for pulse oximetry in 56 premature infants less than 32 weeks gestation. Only infants with significant PDA (sPDA) diagnosed by echocardiography were treated with ibuprofen (for 3 days). ...In this study, PPD was correlated with ductus arteriosus status evaluated by echocardiography, indicating involvement of the ductal shunt in the mechanism of redistribution in systemic vascular territories. PPD can be considered for the diagnosis of hemodynamically significant PDA." | |||
* Cochrane Database - Ibuprofen for the treatment of patent ductus arteriosus in preterm and/or low birth weight infants<ref name=PMID23633310><pubmed>23633310</pubmed></ref> "Indomethacin is used as standard therapy to close a patent ductus arteriosus (PDA) but is associated with reduced blood flow to several organs. Ibuprofen, another cyclo-oxygenase inhibitor, may be as effective as indomethacin with fewer side effects. Twenty-seven studies are included in this review. ...Ibuprofen is as effective as indomethacin in closing a PDA and reduces the risk of NEC and transient renal insufficiency. Given the reduction in NEC ibuprofen currently appears to be the drug of choice. Oro-gastric administration of ibuprofen appears at least as effective as iv administration. Too few patients have been enrolled in studies assessing the effectiveness of a high dose of ibuprofen versus the standard dose and early versus expectant administration of ibuprofen to make recommendations. Studies are needed to evaluate the effect of ibuprofen compared with indomethacin treatment on longer-term outcomes in infants with PDA." | * Cochrane Database - Ibuprofen for the treatment of patent ductus arteriosus in preterm and/or low birth weight infants<ref name=PMID23633310><pubmed>23633310</pubmed></ref> "Indomethacin is used as standard therapy to close a patent ductus arteriosus (PDA) but is associated with reduced blood flow to several organs. Ibuprofen, another cyclo-oxygenase inhibitor, may be as effective as indomethacin with fewer side effects. Twenty-seven studies are included in this review. ...Ibuprofen is as effective as indomethacin in closing a PDA and reduces the risk of NEC and transient renal insufficiency. Given the reduction in NEC ibuprofen currently appears to be the drug of choice. Oro-gastric administration of ibuprofen appears at least as effective as iv administration. Too few patients have been enrolled in studies assessing the effectiveness of a high dose of ibuprofen versus the standard dose and early versus expectant administration of ibuprofen to make recommendations. Studies are needed to evaluate the effect of ibuprofen compared with indomethacin treatment on longer-term outcomes in infants with PDA." | ||
* '''Treatment of patent ductus arteriosus with bidirectional flow in neonates'''<ref><pubmed>21402454</pubmed></ref> "We identified 20 neonates with bidirectional flow out of 317 cases in which medical closure of patent ductus arteriosus was attempted. There was no significant increase in overall complications due to closure of a bidirectional patent ductus arteriosus [40% (8/20)] versus ones with left to right shunting [38% (111/297) p=0.82]. Death occurred in 15% (3/20) with bidirectional PDA compared to 11% (34/297) in the left to right group, p=0.72." | * '''Treatment of patent ductus arteriosus with bidirectional flow in neonates'''<ref><pubmed>21402454</pubmed></ref> "We identified 20 neonates with bidirectional flow out of 317 cases in which medical closure of patent ductus arteriosus was attempted. There was no significant increase in overall complications due to closure of a bidirectional patent ductus arteriosus [40% (8/20)] versus ones with left to right shunting [38% (111/297) p=0.82]. Death occurred in 15% (3/20) with bidirectional PDA compared to 11% (34/297) in the left to right group, p=0.72." | ||
Revision as of 23:16, 25 June 2014
| Embryology - 19 Apr 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
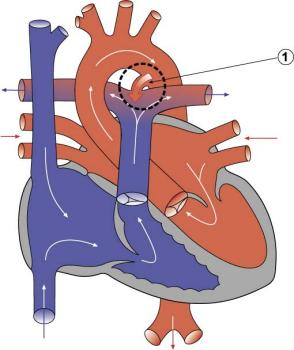
Introduction
Patent ductus arteriosus (PDA), or Patent arterial duct (PAD), or common truncus, occurs commonly in preterm infants, and at approximately 1 in 2000 full term infants and more common in females (to male ratio is 2:1). Can also be associated with specific genetic defects, trisomy 21 and trisomy 18, and the Rubinstein-Taybi and CHARGE syndromes.
The opening is asymptomatic when the duct is small and can close spontaneously (by day three in 60% of normal term neonates), the remainder are ligated simply and with little risk, with transcatheter closure of the duct generally indicated in older children. The operation is always recommended even in the absence of cardiac failure and can often be deferred until early childhood.
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Patent Ductus Arteriosus <pubmed limit=5>Patent Ductus Arteriosus</pubmed> |
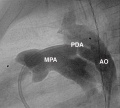
Diagnostic Images
Cardiovascular Abnormalities
Heart defects and preterm birth are the most common causes of neonatal and infant death. The long-term development of the heart combined with extensive remodelling and post-natal changes in circulation lead to an abundance of abnormalities associated with this system.
A UK study literature showed that preterm infants have more than twice as many cardiovascular malformations (5.1 / 1000 term infants and 12.5 / 1000 preterm infants) as do infants born at term and that 16% of all infants with cardiovascular malformations are preterm. (0.4% of live births occur at greater than 28 weeks of gestation, 0.9% at 28 to 31 weeks, and 6% at 32 to 36 weeks. Overall, 7.3% of live-born infants are preterm)[4]
"Baltimore-Washington Infant Study data on live-born cases and controls (1981-1989) was reanalyzed for potential environmental and genetic risk-factor associations in complete atrioventricular septal defects AVSD (n = 213), with separate comparisons to the atrial (n = 75) and the ventricular (n = 32) forms of partial AVSD. ...Maternal diabetes constituted a potentially preventable risk factor for the most severe, complete form of AVSD." [5]
In addition, there are in several congenital abnormalities that exist in adults (bicuspid aortic valve, mitral valve prolapse, and partial anomalous pulmonary venous connection) which may not be clinically recognized.
Classification
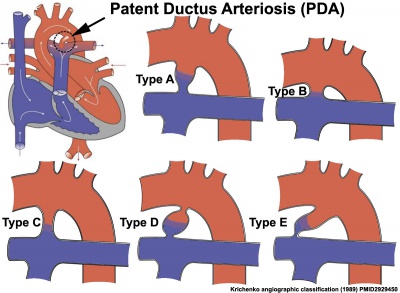
Patent Ductus Arteriosus (PDA) classification system on the basis of angiogram appearance by Krichenko.[6]
|
|
A recent publication suggests one based on angiographic size and haemodynamic sound significance.[7]
| Type | Size | Haemodynamics |
|---|---|---|
| Silent PDA | usually less than 1.5 mm | without audible murmur of PDA |
| Very small PDA | less than 1.5 mm | a murmur of PDA is present |
| Small PDA | 1.5–3.0 mm | a murmur of PDA is present |
| Moderate PDA | 3–5 mm | a murmur of PDA is present |
| Large PDA | greater than 5 mm | a murmur of PDA is present |
The Aristotle Comprehensive Complexity (ACC) score has been suggested as a clinical tool for complexity adjustment in the analysis of outcome after reparative congenital heart surgery.[8][9]
References
Reviews
<pubmed>21532100</pubmed>
Articles
<pubmed>21829408</pubmed> <pubmed>21532789</pubmed>
Search Pubmed
Search Pubmed: Patent Ductus Arteriosus
Search OMIM: Patent Ductus Arteriosus
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- OMIM
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 19) Embryology Cardiovascular System - Patent Ductus Arteriosus. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Cardiovascular_System_-_Patent_Ductus_Arteriosus
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G