Cardiovascular System - Ductus Venosus: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| (13 intermediate revisions by the same user not shown) | |||
| Line 3: | Line 3: | ||
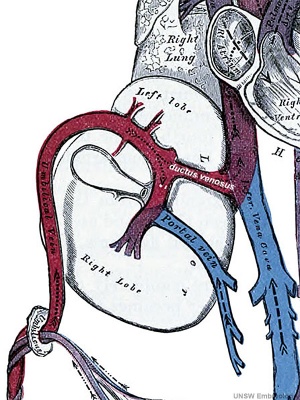
[[File:Fetal ductus venosus cartoon 01.jpg|thumb|300px|alt=Fetal ductus venosus cartoon|Fetal Ductus Venosus]] | [[File:Fetal ductus venosus cartoon 01.jpg|thumb|300px|alt=Fetal ductus venosus cartoon|Fetal Ductus Venosus]] | ||
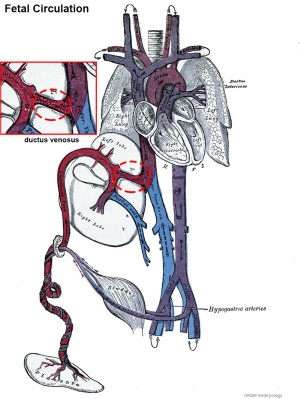
[[File:Fetal ductus venosus cartoon.jpg|thumb|300px|alt=Fetal ductus venosus cartoon|Fetal circulation]] | [[File:Fetal ductus venosus cartoon.jpg|thumb|300px|alt=Fetal ductus venosus cartoon|Fetal circulation]] | ||
The ductus venosus describes the vitelline blood vessel lying within the liver that connects (shunts) the portal and umbilical veins to the inferior vena cava and also acts to protect the fetus from placental over-circulation. | The {{ductus venosus}} describes the vitelline blood vessel lying within the {{liver}} that connects (shunts) the portal and placental (umbilical) veins to the inferior vena cava and also acts to protect the fetus from placental over-circulation. Blood flow within the ductus venosus is sensitive to changes in placental venous pressure, blood viscosity, and the regulation of ductus venosus diameter. | ||
During the second and third trimester, the mean fraction of placental blood shunted through the ductus venosus reduces from 30% to 20%, suggesting a fetal liver priority of circulation.. {{#pmid:11254155|PMID11254155}} | |||
Postnatally this shunt functionally closes (93% of infants at 2 weeks) then structurally closes and degenerates to form it the ligamentum venosum. A comparison | Postnatally this shunt functionally closes (93% of infants at 2 weeks) then structurally closes and degenerates to form it the ligamentum venosum. A comparison at day 3 of postnatal shunt closures; 94% of infants have a closed ductus arteriosus, while only 12% had a closed ductus venosus.{{#pmid:9377136|PMID9377136}} | ||
Abnormalities include an absence or patently. Absence can cause hydrops fetalis and the umbilical vein then drains directly into the inferior vena cava or right atrium. A patent or persistent ductus venosus describes postnatal failure of this vessel to close. | Abnormalities include an absence or patently. Absence can cause hydrops fetalis and the umbilical vein then drains directly into the inferior vena cava or right atrium. A patent or persistent ductus venosus describes the postnatal failure of this vessel to close. | ||
See also the related pages [[Cardiovascular - Arterial Development|Arterial Development]], [[Cardiovascular - Venous Development|Venous Development]], [[Placenta_-_Villi_Development#Placental_Villi_Blood_Vessels|Placental Villi Blood Vessels]] and | See also the related pages {{Foramen ovale}}, {{Ductus arteriosus}}, [[Cardiovascular - Arterial Development|Arterial Development]], [[Cardiovascular - Venous Development|Venous Development]], [[Placenta_-_Villi_Development#Placental_Villi_Blood_Vessels|Placental Villi Blood Vessels]] and {{Coronary circulation}}. | ||
{{Heart Links}} | {{Heart Links}} | ||
:Historic - Ductus Venosus: [[Paper - The ductus venosus in the fetus and in the adult|1923 Ductus Venosus]] | |||
==Some Recent Findings== | ==Some Recent Findings== | ||
| Line 21: | Line 24: | ||
|-bgcolor="F5FAFF" | |-bgcolor="F5FAFF" | ||
| | | | ||
* ''' | * '''Review - Embryology, Ductus Venosus'''{{#pmid:31613539|PMID31613539}} "The ductus venosus is a shunt that allows oxygenated blood in the umbilical vein to bypass the liver and is essential for normal fetal circulation. Blood becomes oxygenated in the placenta and travels to the right atrium via umbilical veins through the ductus venosus, then to the inferior vena cava. This oxygenated blood then passes through the foramen ovale, an opening between the atria, into the left atrium to be distributed systemically." | ||
* '''Patent Ductus Venosus and Congenital Heart Disease: A Case Report and Review'''{{#pmid:30344833|PMID30344833}} "In utero, the ductus venosus connects the left portal vein to the inferior vena cava, allowing a portion of the venous blood to bypass the liver and return to the heart. After birth, the ductus venosus closes due to changes in intracardiac pressures and a decrease in endogenous prostaglandins. Failure of the ductus venosus to close may result in galactosemia, hypoxemia, encephalopathy with hyperammonia, and hepatic dysfunction. We report an infant with complex congenital heart disease (CHD) who developed coagulopathy and hyperammonia during the preoperative period secondary to patent ductus venosus (PDV). Previous reports of PDV in CHD are presented, its etiology and clinical consequences reviewed, and options for therapeutic treatment discussed." | |||
* '''Normal variants of ductus venosus spectral Doppler flow patterns in normal pregnancies'''{{#pmid:30153762|PMID30153762}} "Ductus venosus (DV) Doppler examinations in pregnancy have a widespread use for several important indications and play a crucial role in order to determine the fetal well-being. DV is usually visualized by the color Doppler mapping. We observed the instantaneous spectral flow type changes in pulsed Doppler examinations in spite of performing with the correct technique published by several authors. The variability of the pattern makes the sonographer/physician to be unsure for the correct placements of the sample gate despite fulfilling the all the criteria required for the vessel sampling. This prospective study was conducted between January 2016 and February 2017. We think that the fetal circulation is complicated more than estimated. There might be some endocrine agents released in the instantaneous physiologic reactions and changing the venous return abruptly or due to decreasing of the cardiac output directed to the placenta after 34 weeks influence the volume of the circulating blood in the fetus and so thereby the flow velocities instantaneously. The spectral waveform recognition approach is not reliable to identify if the DV spectral Doppler pattern is not the classic (standard) type and the DV should be visualized by wide-band color Doppler techniques particularly in the third trimester for the pulsed Doppler examinations. Studies are needed to evaluate the normal spectral variants of the flows correlated with the physiological compensatory mechanisms." | |||
* '''Maternal diabetes alters the development of ductus venosus shunting in the fetus'''{{#pmid:29752712|PMID29752712}} "Despite adequate glycemic control, the risks of fetal macrosomia and perinatal complications are increased in diabetic pregnancies. Adjustments of the umbilical venous (UV) distribution, including increased ductus venosus (DV) shunting, can be important fetal compensatory mechanisms, but the impact of pregestational diabetes on UV and DV flow is not known. In pregnancies with pregestational diabetes mellitus, prioritized UV distribution to the fetal liver, and lower DV shunt capacity, both reduce the compensatory capability of the fetus and may represent an augmented risk during hypoxic challenges during late pregnancy and birth." {{maternal diabetes}} | |||
|} | |} | ||
{| class="wikitable mw-collapsible mw-collapsed" | {| class="wikitable mw-collapsible mw-collapsed" | ||
! More recent papers | ! More recent papers | ||
|- | |- | ||
| [[File:Mark_Hill.jpg|90px|left]] {{Most_Recent_Refs}} | | [[File:Mark_Hill.jpg|90px|left]] {{Most_Recent_Refs}} | ||
Search term: [http://www.ncbi.nlm.nih.gov/pubmed/?term=Ductus+Venosus ''Ductus Venosus''] | Search term: [http://www.ncbi.nlm.nih.gov/pubmed/?term=Ductus+Venosus ''Ductus Venosus''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Patent+Ductus+Venosus ''Patent Ductus Venosus''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=hydrops+fetalis ''hydrops fetalis''] | ||
|} | |} | ||
{| class="wikitable mw-collapsible mw-collapsed" | |||
! Older papers | |||
|- | |||
| {{Older papers}} | |||
* '''Reference ranges for ductus venosus velocity ratios in pregnancies with normal outcomes'''{{#pmid:24449737|PMID24449737}} "Singleton pregnancies from 11 to 38 weeks with exactly established gestational ages (GAs) were recruited for the study. A total of 902 velocity wave ratios and ductus venosus PIVs were used for reference ranges. The S/v, S/D, and v/D ratios were not changed with GA (P > .05 for all). The PIV and S/a, v/a, and D/a ratios were reduced with GA (P < .0001 for all). Significant reductions in the means and standard deviations of the PIV and S/a, v/a, and D/a ratios were observed between 17 and 18 weeks' gestation. Therefore, nomograms were separately created between 11 and 17 weeks and 18 and 38 weeks." | |||
|} | |||
==Embryonic Development== | ==Embryonic Development== | ||
===Stage 13=== | ===Stage 13=== | ||
| Line 69: | Line 82: | ||
==Abnormalities== | ==Abnormalities== | ||
===Patent Ductus Venosus=== | ===Patent Ductus Venosus=== | ||
Failure of the ductus venosus to close may result in a range of down-stream effects including: galactosemia, hypoxemia, encephalopathy with hyperammonia, and hepatic dysfunction.{{#pmid:30344833|PMID30344833}} | |||
Patent or Persistent ductus venosus (postnatal 8 years) connecting the left portal vein to the inferior vena cava.{{#pmid:24688239|PMID24688239}} | Patent or Persistent ductus venosus (postnatal 8 years) connecting the left portal vein to the inferior vena cava.{{#pmid:24688239|PMID24688239}} | ||
| Line 82: | Line 96: | ||
| {{Ultrasound patent ductus venosus movie}} | | {{Ultrasound patent ductus venosus movie}} | ||
|} | |} | ||
:'''Links:''' [[Computed Tomography]] | [http://www.omim.org/entry/601466 OMIM 601466 Patent Ductus Venosus] | :'''Links:''' [[Computed Tomography]] | [http://www.omim.org/entry/601466 OMIM 601466 Patent Ductus Venosus] | ||
| Line 87: | Line 103: | ||
<references/> | <references/> | ||
=== | ===Reviews=== | ||
{{#pmid:31613539}} | |||
{{#pmid:11254155}} | |||
===Articles=== | ===Articles=== | ||
{{#pmid:9377136}} | {{#pmid:9377136}} | ||
===Search Pubmed=== | ===Search Pubmed=== | ||
| Line 106: | Line 126: | ||
{{Footer}} | {{Footer}} | ||
[[Category:Cardiovascular]] | [[Category:Cardiovascular]][[Category:Blood Vessel]] | ||
Latest revision as of 14:01, 3 December 2021
| Embryology - 19 Apr 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
The ductus venosus describes the vitelline blood vessel lying within the liver that connects (shunts) the portal and placental (umbilical) veins to the inferior vena cava and also acts to protect the fetus from placental over-circulation. Blood flow within the ductus venosus is sensitive to changes in placental venous pressure, blood viscosity, and the regulation of ductus venosus diameter.
During the second and third trimester, the mean fraction of placental blood shunted through the ductus venosus reduces from 30% to 20%, suggesting a fetal liver priority of circulation.. [1]
Postnatally this shunt functionally closes (93% of infants at 2 weeks) then structurally closes and degenerates to form it the ligamentum venosum. A comparison at day 3 of postnatal shunt closures; 94% of infants have a closed ductus arteriosus, while only 12% had a closed ductus venosus.[2]
Abnormalities include an absence or patently. Absence can cause hydrops fetalis and the umbilical vein then drains directly into the inferior vena cava or right atrium. A patent or persistent ductus venosus describes the postnatal failure of this vessel to close.
See also the related pages foramen ovale, ductus arteriosus, Arterial Development, Venous Development, Placental Villi Blood Vessels and coronary circulation.
- Historic - Ductus Venosus: 1923 Ductus Venosus
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Ductus Venosus | Patent Ductus Venosus | hydrops fetalis |
| Older papers |
|---|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
|
Embryonic Development
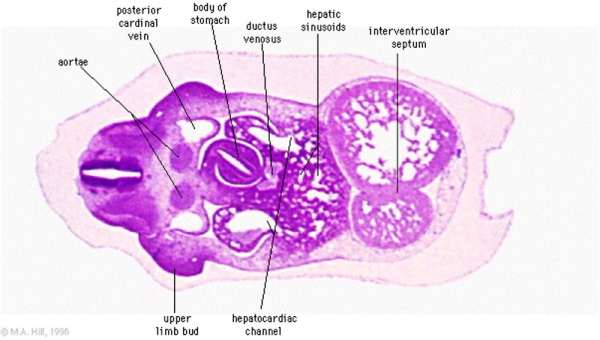
Stage 13
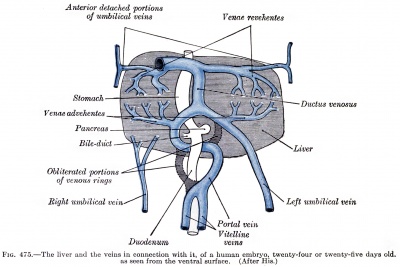
|
Human Embryo Liver and Associated Veins
Human embryo liver ventral surface view. Figure after {{His)).
|
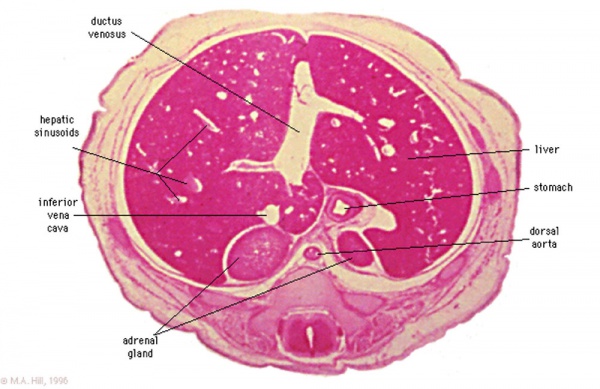
Stage 22
Fetal Development
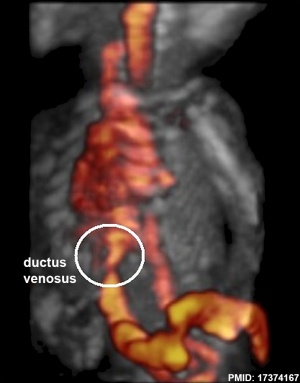
Fetal ductus venosus ultrasound[8]
- Links: ultrasound
Physiology
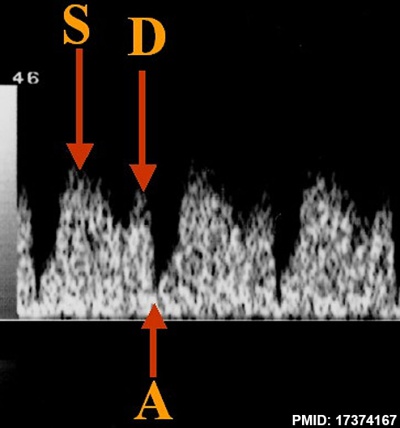
Fetal ductus venosus pressure wave
Abnormalities
Patent Ductus Venosus
Failure of the ductus venosus to close may result in a range of down-stream effects including: galactosemia, hypoxemia, encephalopathy with hyperammonia, and hepatic dysfunction.[4]
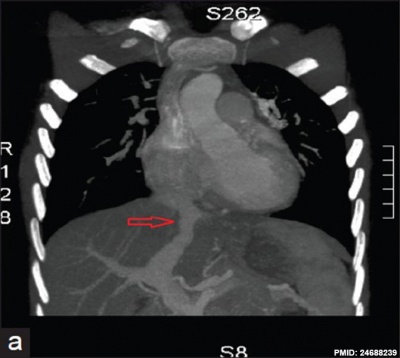
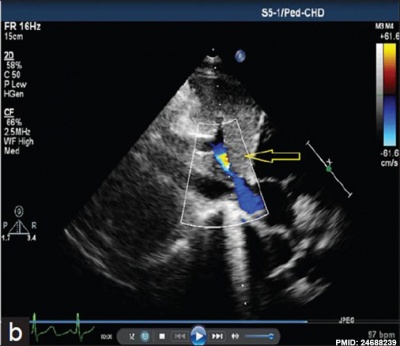
Patent or Persistent ductus venosus (postnatal 8 years) connecting the left portal vein to the inferior vena cava.[9]
|
| |||
| Tomography | Two-dimensional echocardiography | |||
|
References
- ↑ Kiserud T. (2001). The ductus venosus. Semin. Perinatol. , 25, 11-20. PMID: 11254155
- ↑ Fugelseth D, Lindemann R, Liestøl K, Kiserud T & Langslet A. (1997). Ultrasonographic study of ductus venosus in healthy neonates. Arch. Dis. Child. Fetal Neonatal Ed. , 77, F131-4. PMID: 9377136
- ↑ Sidhu PS & Lui F. (2019). Embryology, Ductus Venosus. , , . PMID: 31613539
- ↑ 4.0 4.1 Poeppelman RS & Tobias JD. (2018). Patent Ductus Venosus and Congenital Heart Disease: A Case Report and Review. Cardiol Res , 9, 330-333. PMID: 30344833 DOI.
- ↑ Gürses C, Karadağ B & İsenlik BST. (2018). Normal variants of ductus venosus spectral Doppler flow patterns in normal pregnancies. J. Matern. Fetal. Neonatal. Med. , , 1-7. PMID: 30153762 DOI.
- ↑ Lund A, Ebbing C, Rasmussen S, Kiserud TW & Kessler J. (2018). Maternal diabetes alters the development of ductus venosus shunting in the fetus. Acta Obstet Gynecol Scand , , . PMID: 29752712 DOI.
- ↑ Turan OM, Turan S, Sanapo L, Willruth A, Wilruth A, Berg C, Gembruch U, Harman CR & Baschat AA. (2014). Reference ranges for ductus venosus velocity ratios in pregnancies with normal outcomes. J Ultrasound Med , 33, 329-36. PMID: 24449737 DOI.
- ↑ da Silva FC, de Sá RA, de Carvalho PR & Lopes LM. (2007). Doppler and birth weight Z score: predictors for adverse neonatal outcome in severe fetal compromise. Cardiovasc Ultrasound , 5, 15. PMID: 17374167 DOI.
- ↑ Subramanian V, Kavassery MK, Sivasubramonian S & Sasidharan B. (2013). Percutaneous device closure of persistent ductus venosus presenting with hemoptysis. Ann Pediatr Cardiol , 6, 173-5. PMID: 24688239 DOI.
Reviews
Sidhu PS & Lui F. (2019). Embryology, Ductus Venosus. , , . PMID: 31613539
Kiserud T. (2001). The ductus venosus. Semin. Perinatol. , 25, 11-20. PMID: 11254155
Articles
Fugelseth D, Lindemann R, Liestøl K, Kiserud T & Langslet A. (1997). Ultrasonographic study of ductus venosus in healthy neonates. Arch. Dis. Child. Fetal Neonatal Ed. , 77, F131-4. PMID: 9377136
Search Pubmed
Search Pubmed: Ductus Venosus
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 19) Embryology Cardiovascular System - Ductus Venosus. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Cardiovascular_System_-_Ductus_Venosus
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G