BGDA Practical 3 - Implantation: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| Line 73: | Line 73: | ||
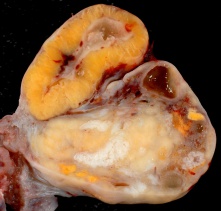
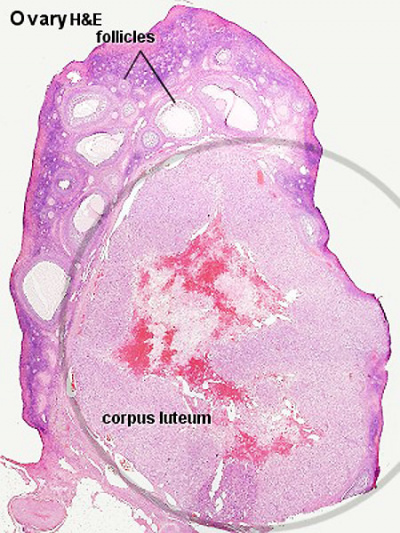
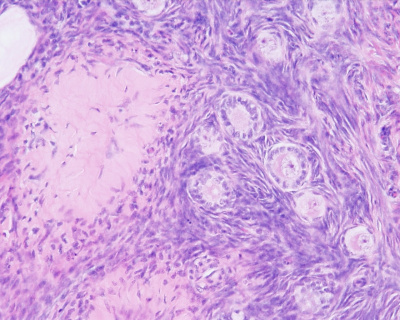
== Corpus Luteum == | == Corpus Luteum == | ||
[[File:Ovary_corpus_luteum.jpg| | {| | ||
| [[File:Ovary_corpus_luteum.jpg|500px|alt=Corpus Luteum in ovary]] | |||
| [[File:Corpus luteum lutein cells.jpg|500px|alt=Corpus Luteum histology]] | |||
{| | {| | ||
| width=240px|{{SlideOvaryCorpusLuteum}} | | width=240px|{{SlideOvaryCorpusLuteum}} | ||
Revision as of 11:18, 6 May 2019
| Practical 3: Oogenesis and Ovulation | Gametogenesis | Fertilization | Early Cell Division | Week 1 | Implantation | Week 2 | Extraembryonic Spaces | Gastrulation | Notochord | Week 3 |
Introduction
Trophoblast cells at the site of adplantation proliferate and form an additional layer the syncitiotrophoblast layer. This layer of cells rapidly divide, secrete enzymes that degrade the endometrial extracellular matrix and secrete human Chorionic Gonadotropin (hCG). Trophoblast cells also disperse through the maternal decidua and are associated with the open maternal blood vessels and the anchoring villi attachment (trophoblast column).
Implantation Dynamics
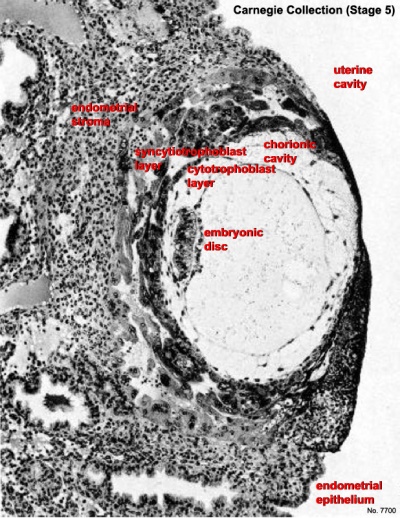
The uterine epithelium (white cells) are invaded by the trophoblast cells (green, syncitiotrophoblasts) with the inner cell mass now having 2 layers: an epiblast (blue) and hypoblast (yellow). The blastoceol is covered in cytotrophoblast cells (green).
Later in the movie the amniotic cavity forms adjacent to the epiblast layer(blue) and spaces in the syncitiotrophoblast layer are filled with maternal blood, lacunae.
| <html5media height="580" width="500">File:Week2_001.mp4</html5media> |
This animation shows the process of implantation, occurring during week 2 (GA week 4) of development in humans. The beginning of the animation shows adplantation to the the uterus lining (endometrium epithelium). The hatched blastocyst with a flat outer layer of trophoblast cells (green), the inner cell mass which has formed into the bilaminar embryo (epiblast and hypoblast) and the large fluid-filled space (blastocoel).
|
Identify the embryoblast and trophoblast layers of the conceptus.
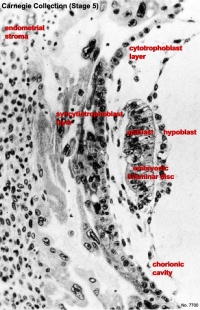
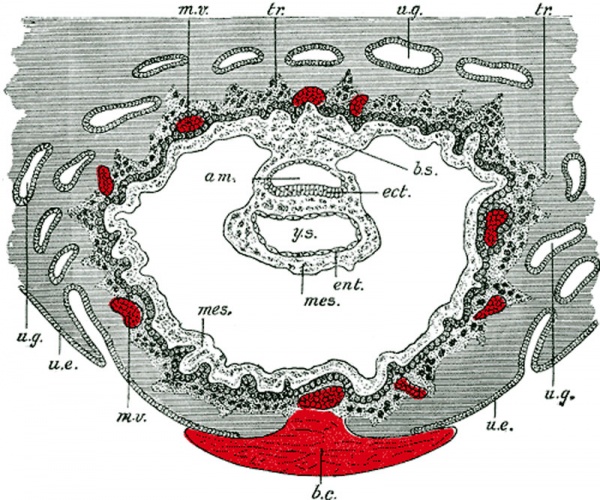
Carnegie Stage 4 represents the beginning of implantation. The blastocyst initially attached to the uterine endometrium (adplantation), syncitiotrophoblasts then secrete enzymes that digest extracellular matrix, allowing the blastocyst to sink into the uterine wall, eventually being completely enclosed within the uterine wall. Note the majority of growth occurs in the trophoblastic shell. The inner cell mass divides initially into 2 layers; epiblast and hypoblast (bilaminar embryo). Hypoblast cells migrate around the original blastoceol cavity forming the primary yolk sac. A second cavity (amniotic) forms between the inner cell mass and the cytotrophoblast shell; this cavity is lined by epiblast cells.
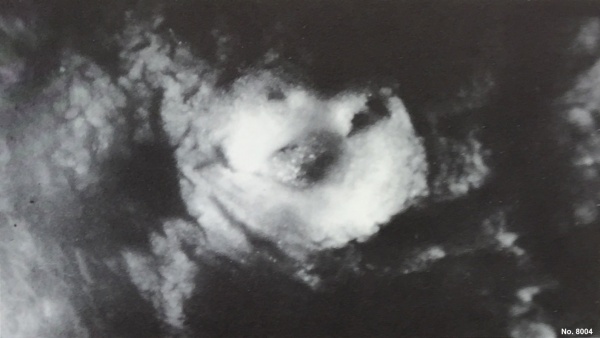
This is a uterine surface view showing the site of implantation (pale region in centre of image). The conceptus can be identified located at the dark central region within the pale region.
Corpus Luteum
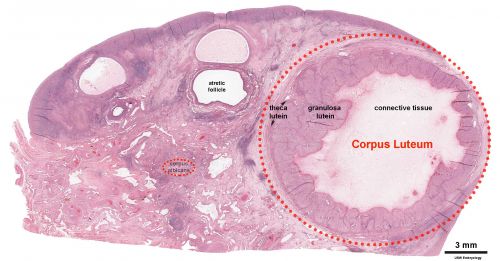
|
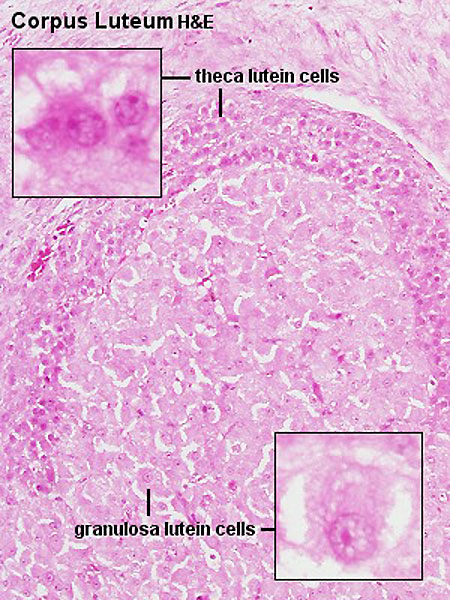
HistologyCorpus AlbicansThe degenerating remnant of the ovulating follicle.
Additional Information
Complications in Early PregnancyPontius E & Vieth JT. (2019). Complications in Early Pregnancy. Emerg. Med. Clin. North Am. , 37, 219-237. PMID: 30940368 DOI. Early in pregnancy women frequently experience nausea, vomiting, and vaginal bleeding. Nausea and vomiting can be mild, managed by dietary modifications and medications, or severe, requiring intravenous fluids and medications. Care should be used when selecting medications for nausea to avoid additional side effects or potential harm to the developing fetus. When evaluating vaginal bleeding in early pregnancy, ectopic pregnancy must be ruled out. If an intrauterine pregnancy is seen, threatened miscarriage should be considered and the patient appropriately counseled. If neither intrauterine pregnancy nor ectopic pregnancy can be established, a management algorithm for pregnancy of unknown location is presented.
Pelvic Inflammatory Disease and Ectopic PregnancyRates of pelvic inflammatory disease and ectopic pregnancy in Australia, 2009-2014[1]
Birth ControlThere are a number of different chemical and mechanical methods of birth control. The most comon is the "birth control pill" taken daily and made up of two hormones, estrogen and progestogen and these stop a woman's ovaries from releasing an egg each month (ovulation), which means that a pregnancy cannot begin. Recently the drug RU486, which is an abortive rather contraceptive drug, has been the centre of political and medical discussions in Australia. Chemical
Maternal ImmuneHow does the implanting conceptus avoid immune rejection by the maternal immune system? There are a number of maternal and embryonic mechanisms that are thought to act to prevent immune rejection of the implanting conceptus, a few mechanisms are shown below. Chemokine Gene Silencing - Remove the attraction of maternal immune cells. A mouse study[2] has shown that the normal immune response to inflammation, accumulation of effector T cells in response to chemokine secretion does not occur during implantation. This is prevented locally by epigenetic silencing of chemokine expression in the decidual stromal cells. Corticotropin-Releasing Hormone - Kill the maternal immune cells. Both maternal and implanting conceptus release CRH at the embryo implantation site. This hormone then binds to receptors on the surface of trophoblast (extravillous trophoblast) cells leading to expression of a protein (Fas ligand, FasL) that activates the extrinsic cell death pathway on any local maternal immune cells ( T and B lymphocytes, natural killer cells, monocytes and macrophages).[3] This cannot be the only mechanism, as mice with dysfunctional FasL proteins are still fertile. Links: implantation
Terms
References
Glossary Links
Cite this page: Hill, M.A. (2024, April 19) Embryology BGDA Practical 3 - Implantation. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/BGDA_Practical_3_-_Implantation
|
||||||||||||||||||||||||||||||||