Abnormal Development - Genetic: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| Line 63: | Line 63: | ||
:'''Links:''' [[Genetic risk maternal age]] | | :'''Links:''' [[Genetic risk maternal age]] | {{Trisomy 21}} | [[Trisomy 18]] | [[Trisomy 13]] | [[Oocyte Development]] | ||
===Embryonic Aneuploidy=== | ===Embryonic Aneuploidy=== | ||
Revision as of 10:45, 23 July 2018
| Embryology - 19 Apr 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
| Educational Use Only - Embryology is an educational resource for learning concepts in embryological development, no clinical information is provided and content should not be used for any other purpose. |
Introduction
This page gives a general introduction to information about genetic abnormalities their relationship to age, ethnicity and prenatal testing. Use the listed links for more information about specific abnormalities. In developed countries with increasing maternal age comes the increased risk of age related genetic abnormalities, such as trisomy 21.
In order to detect some genetic abnormalities many countries offer genetic screening programs that include maternal serum screening (MSS, for detection of Down's syndrome and neural tube defects), embryonic and newborn screening (for phenylketonuria (PKU), hypothyroidism, cystic fibrosis and metabolic disorders).
In terms of maternal/paternal family history, some ethnic backgrounds have been shown to have disease-associated genetic variants, though most common genetic diseases are consistent across ethnic boundaries. For example: Caucasians of northern European ancestry and cystic fibrosis (CTFR gene), Mediterranean, Asian and Far Eastern ancestry with beta-thalassaemia.
Note that the development of in vitro fertilization techniques now allows cells from early stage blastocysts to be removed and genetically analysed prior to implantation. This has raised some ethical issues relating to what parameters will be in future used in blastocyst selection.
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Genetic Abnormal Development Search term: Genetic Abnormal Development <pubmed limit=5>Genetic Abnormal Development</pubmed> |
| Older papers |
|---|
|
ICD-11 Chromosomal Anomalies
The International Classification of Diseases (ICD) World Health Organization's classification used worldwide as the standard diagnostic tool for epidemiology, health management and clinical purposes.
| ICD-11 Chromosomal anomalies excluding gene mutations | |
|---|---|
| |
Sex chromosome anomalies
| |
| |
| LD7Y Other specified chromosomal anomalies, excluding gene mutations
LD7Z Chromosomal anomalies, excluding gene mutations, unspecified | |
genetic abnormalities
|
Human Oocyte Aneuploidy
- Frequency and distribution of chromosome abnormalities in human oocytes[9] "It was previously shown that more than half of the human oocytes obtained from IVF patients of advanced reproductive age are aneuploid, due to meiosis I and meiosis II errors. The present paper further confirms that 61.8% of the oocytes tested by fluorescent probes specific for chromosomes 13, 16, 18, 21 and 22 are abnormal, representing predominantly chromatid errors, which are the major source of aneuploidy in the resulting embryos. Almost half of the oocytes with meiosis I errors (49.3%) are prone to sequential meiosis II errors, which may lead to aneuploidy rescue in 30.8% of the cases. Half of the detected aneuploidies (49.8%) are of complex nature with involvement of two or more chromosomes, or the same chromosome in both meiotic divisions. The aneuploidy rates for individual chromosomes are different, with a higher prevalence of chromosome 21 and 22 errors. The origin of aneuploidy for the individual chromosomes is also not random, with chromosome 16 and 22 errors originating more frequently in meiosis II, and chromosome 18, 13 and 21 errors in meiosis I. There is an age dependence not only for the overall frequency of aneuploidies, but also for each chromosome error, aneuploidies originating from meiosis I, meiosis II, and both meiosis I and meiosis II errors, as well as for different types of aneuploidies. The data further suggest the practical relevance of oocyte aneuploidy testing for detection and avoidance from transfer of the embryos deriving from aneuploid oocytes, which should contribute significantly to the pregnancy outcomes of IVF patients of advanced reproduction age."
- Links: Genetic risk maternal age | Trisomy 21 | Trisomy 18 | Trisomy 13 | Oocyte Development
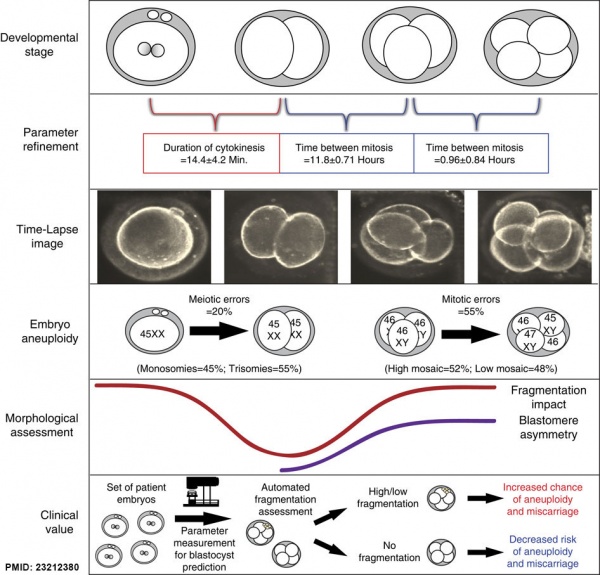
Embryonic Aneuploidy
Embryonic aneuploidy model based on fragmentation.[10] (See also Fragmentation Model and Monosomic Embryo Movie)
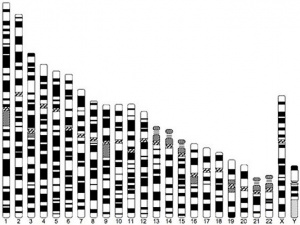
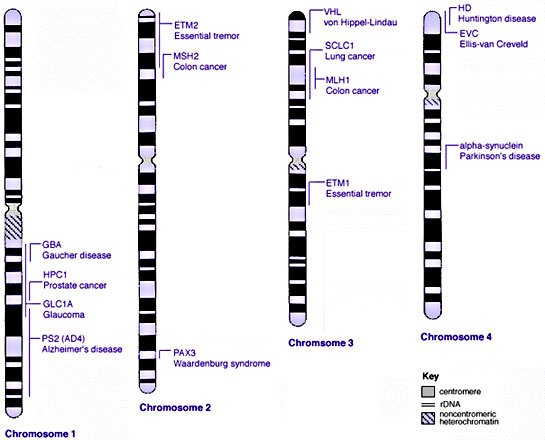
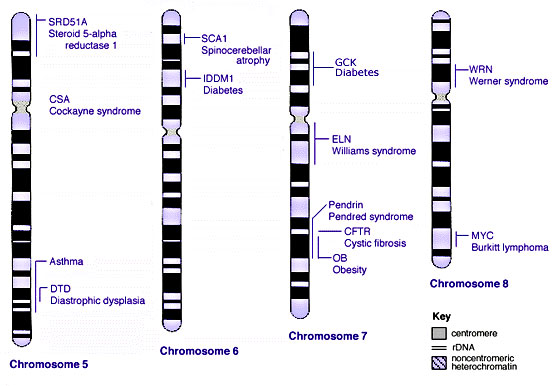
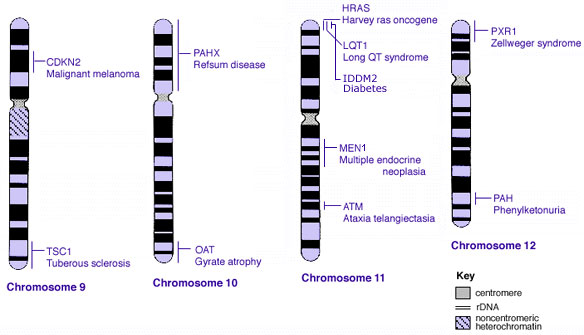
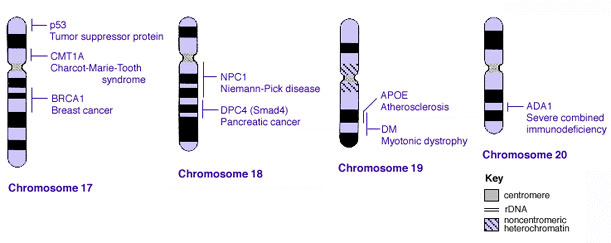
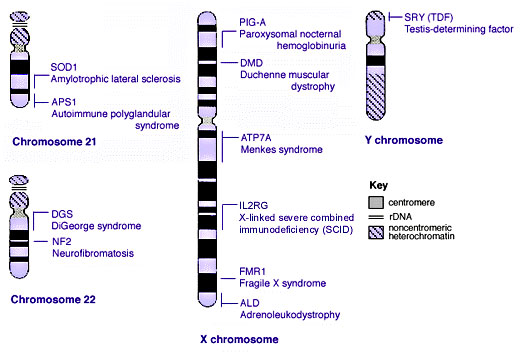
Some Human Disease Gene Locations
Genetic Inheritance
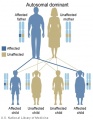
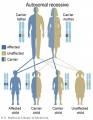
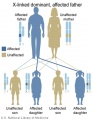
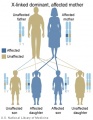
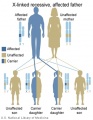
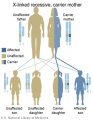
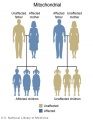
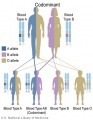
The figures below show the pattern of inheritance of a range of genetic disorders. In addition to these patterns are the known effects of increased maternal age and the effects of genetic mutations in the embryo and newborn.
- Inheritance Pattern images: Genetic Abnormalities | autosomal dominant | autosomal recessive | X-linked dominant (affected father) | X-Linked dominant (affected mother) | X-Linked recessive (affected father) | X-Linked recessive (carrier mother) | mitochondrial inheritance | Codominant inheritance | Genogram symbols | Genetics
An example of autosomal recessive traits are the majority of 50 or so lysosomal diseases, with two X-linked exceptions, that of Fabry disease and Mucopolysaccharidosis II.[11]
Genome-wide association study
The National Human Genome Research Institute (USA) lists publications as part of the genome-wide association study (GWAS) in an attempt to assay at least 100,000 single nucleotide polymorphisms (SNPs) in the initial stage.
Genetic Abnormality Topics
Genetic Risk Maternal Age
Table Data[12][13][14]
| |||
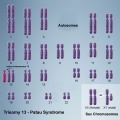
Trisomy
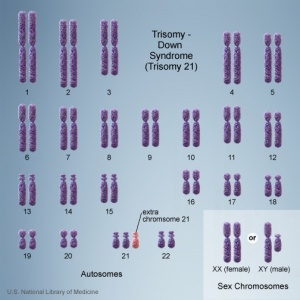
In humans, the most common trisomy is trisomy 21 or Down syndrome.
The term trisomy refers to the abnormal copy number of a specific chromosome, that is 3 copies instead of 2. The abnormality is identified by the chromosome that is present as 3 copies within the cell.
Trisomy 21 (male)
Trisomy 21 (female)
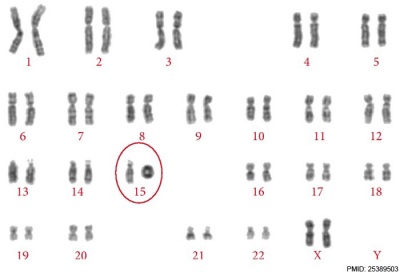
Ring Chromosome
Ring chromosomal 15
Selected Topics
Mutagen
A chemical or agent that can cause permanent damage to the genetic material, DeoxyriboNucleic Acid (DNA) in a cell. DNA damage in the human oocyte or spermatozoa may lead to reduced fertility, spontaneous abortion (miscarriage), birth defects and heritable diseases. DNA damage postnatally can lead to a variety of tumours.
There are a large number of known mutagenic agents including those that are physical, chemical or biological in origin.
Neonatal Testing
The main neonatal genetic test is the Bloodspot Test also known as the Guthrie Test.
Bloodspot Test or Guthrie Test
A blood screening test developed by Dr Robert Guthrie (1916-95) at University of Buffalo.[15] The test is carried out on neonatal (newborn) blood detecting markers for a variety of known disorders (phenylketonuria (PKU), hypothyroidism and cystic fibrosis).
- Links: Guthrie test | neonatal diagnosis
Australia - NSW Newborn Screening Programme
Each year test more than 90,000 babies and detects about 90 who need urgent assessment and treatment. In NSW and Victoria, the bloodspot cards are currently stored indefinitely.
- Phenylketonuria (PKU) - 1 in 10,000 live births (about 10 babies per year). PKU causes high blood levels of phenylalanine and severe intellectual disability. A diet low in phenylalanine, started in the first two to three weeks results in normal development.
- Primary congenital hypothyroidism - 1 in 3,500 live births (about 26 babies per year). It is caused by the absence or abnormal formation or function of the thyroid gland. This causes growth and intellectual disability if not treated. Medication with thyroid hormone started early, results in normal growth and development.
- Cystic Fibrosis (CF) - 1 in 2,500 live births (about 34 babies per year). Without treatment babies develop chest infections and often have very serious failure to thrive. Early institution of treatment greatly improves the health of babies with CF. Newborn bloodspot screening detects about 95% of babies with CF but also detects a few babies who may only be healthy carriers. For these babies a sweat test at about six weeks of age determines whether the baby has CF or is a healthy carrier.
- Galactosaemia - 1 in 40,000 births (about 1-3 cases per year). Babies cannot process galactose, a component of lactose. Life-threatening liver failure and infections can occur. A galactose-free diet instituted in the first week is life saving.
- Rarer metabolic disorders - Some fatty acid, organic acid and other amino acid defects can now be detected using Tandem Mass Spectrometry. These much rarer metabolic disorders affect about 15 – 18 babies per year. Early detection is important as diet and medications can treat most of these disorders. Without appropriate management they can cause severe disability or death.
Genetics services in NSW - coordinated by the NSW Genetics Service Advisory Committee, which is supported by the Statewide Services Development Branch of the Strategic Development Division, NSW Department of Health. (Information from NSW Health - Newborn Bloodspot Screening Policy 13-Nov-2006)
neonatal diagnosis | NSW Genetics Health
Science Student Projects 2011
The links below are to pages prepared as part of an undergraduate science student projects carried out in the Embryology course. Please note these are student submissions and may include inaccuracies in either description or understanding.
- 2011 Projects: Turner Syndrome | DiGeorge Syndrome | Klinefelter's Syndrome | Huntington's Disease | Fragile X Syndrome | Tetralogy of Fallot | Angelman Syndrome | Friedreich's Ataxia | Williams-Beuren Syndrome | Duchenne Muscular Dystrolphy | Cleft Palate and Lip
International Classification of Diseases
The International Classification of Diseases (ICD) World Health Organization's classification used worldwide as the standard diagnostic tool for epidemiology, health management and clinical purposes. This includes the analysis of the general health situation of population groups. It is used to monitor the incidence and prevalence of diseases and other health problems. Within this classification "congenital malformations, deformations and chromosomal abnormalities" are (Q00-Q99) but excludes "inborn errors of metabolism" (E70-E90).
Chromosomal abnormalities, not elsewhere classified (Q90-Q99)
- Q90 Down's syndrome
- Q90.0 Trisomy 21, meiotic nondisjunction
- Q90.1 Trisomy 21, mosaicism (mitotic nondisjunction)
- Q90.2 Trisomy 21, translocation
- Q90.9 Down's syndrome, unspecified Trisomy 21 NOS
- Q91 Edwards' syndrome and Patau's syndrome
- Q91.0 Trisomy 18, meiotic nondisjunction
- Q91.1 Trisomy 18, mosaicism (mitotic nondisjunction)
- Q91.2 Trisomy 18, translocation
- Q91.3 Edwards' syndrome, unspecified
- Q91.4 Trisomy 13, meiotic nondisjunction
- Q91.5 Trisomy 13, mosaicism (mitotic nondisjunction)
- Q91.6 Trisomy 13, translocation
- Q91.7 Patau's syndrome, unspecified
- Q92 Other trisomies and partial trisomies of the autosomes, not elsewhere classified Incl.: unbalanced translocations and insertions Excl.: trisomies of chromosomes 13, 18, 21 (Q90-Q91)
- Q92.0 Whole chromosome trisomy, meiotic nondisjunction
- Q92.1 Whole chromosome trisomy, mosaicism (mitotic nondisjunction)
- Q92.2 Major partial trisomy Whole arm or more duplicated.
- Q92.3 Minor partial trisomy Less than whole arm duplicated.
- Q92.4 Duplications seen only at prometaphase
- Q92.5 Duplications with other complex rearrangements
- Q92.6 Extra marker chromosomes
- Q92.7 Triploidy and polyploidy
- Q92.8 Other specified trisomies and partial trisomies of autosomes
- Q92.9 Trisomy and partial trisomy of autosomes, unspecified
- Q93 Monosomies and deletions from the autosomes, not elsewhere classified
- Q93.0 Whole chromosome monosomy, meiotic nondisjunction
- Q93.1 Whole chromosome monosomy, mosaicism (mitotic nondisjunction)
- Q93.2 Chromosome replaced with ring or dicentric
- Q93.3 Deletion of short arm of chromosome 4 Wolff-Hirschorn syndrome
- Q93.4 Deletion of short arm of chromosome 5 Cri-du-chat syndrome
- Q93.5 Other deletions of part of a chromosome Angelman syndrome
- Q93.6 Deletions seen only at prometaphase
- Q93.7 Deletions with other complex rearrangements
- Q93.8 Other deletions from the autosomes
- Q93.9 Deletion from autosomes, unspecified
- Q95 Balanced rearrangements and structural markers, not elsewhere classified Incl.: Robertsonian and balanced reciprocal translocations and insertions
- Q95.0 Balanced translocation and insertion in normal individual
- Q95.1 Chromosome inversion in normal individual
- Q95.2 Balanced autosomal rearrangement in abnormal individual
- Q95.3 Balanced sex/autosomal rearrangement in abnormal individual
- Q95.4 Individuals with marker heterochromatin
- Q95.5 Individuals with autosomal fragile site
- Q95.8 Other balanced rearrangements and structural markers
- Q95.9 Balanced rearrangement and structural marker, unspecified
- Q96 Turner's syndrome Excl.: Noonan's syndrome (Q87.1)
- Q96.0 Karyotype 45,X
- Q96.1 Karyotype 46,X iso (XQ)
- Q96.2 Karyotype 46,X with abnormal sex chromosome, except iso (XQ)
- Q96.3 Mosaicism, 45,X/46,XX or XY
- Q96.4 Mosaicism, 45,X/other cell line(s) with abnormal sex chromosome
- Q96.8 Other variants of Turner's syndrome
- Q96.9 Turner's syndrome, unspecified
- Q97 Other sex chromosome abnormalities, female phenotype, not elsewhere classified Excl.: Turner's syndrome (Q96.-)
- Q97.0 Karyotype 47,XXX
- Q97.1 Female with more than three X chromosomes
- Q97.2 Mosaicism, lines with various numbers of X chromosomes
- Q97.3 Female with 46,XY karyotype
- Q97.8 Other specified sex chromosome abnormalities, female phenotype
- Q97.9 Sex chromosome abnormality, female phenotype, unspecified
- Q98 Other sex chromosome abnormalities, male phenotype, not elsewhere classified
- Q98.0 Klinefelter's syndrome karyotype 47,XXY
- Q98.1 Klinefelter's syndrome, male with more than two X chromosomes
- Q98.2 Klinefelter's syndrome, male with 46,XX karyotype
- Q98.3 Other male with 46,XX karyotype
- Q98.4 Klinefelter's syndrome, unspecified
- Q98.5 Karyotype 47,XYY
- Q98.6 Male with structurally abnormal sex chromosome
- Q98.7 Male with sex chromosome mosaicism
- Q98.8 Other specified sex chromosome abnormalities, male phenotype
- Q98.9 Sex chromosome abnormality, male phenotype, unspecified
- Q99 Other chromosome abnormalities, not elsewhere classified
- Q99.0 Chimera 46,XX/46,XY Chimera 46,XX/46,XY true hermaphrodite
- Q99.1 46,XX true hermaphrodite 46,XX with streak gonads 46,XY with streak gonads Pure gonadal dysgenesis
- Q99.2 Fragile X chromosome Fragile X syndrome
- Q99.8 Other specified chromosome abnormalities
- Q99.9 Chromosomal abnormality, unspecified
References
- ↑ Arya S, Mulla ZD & Plavsic SK. (2018). Outcomes of Women Delivering at Very Advanced Maternal Age. J Womens Health (Larchmt) , , . PMID: 30016194 DOI.
- ↑ Wang S, Hassold T, Hunt P, White MA, Zickler D, Kleckner N & Zhang L. (2017). Inefficient Crossover Maturation Underlies Elevated Aneuploidy in Human Female Meiosis. Cell , 168, 977-989.e17. PMID: 28262352 DOI.
- ↑ Jaruthamsophon K, Sriplung H, Charalsawadi C & Limprasert P. (2016). Maternal Age-Specific Rates for Trisomy 21 and Common Autosomal Trisomies in Fetuses from a Single Diagnostic Center in Thailand. PLoS ONE , 11, e0165859. PMID: 27812158 DOI.
- ↑ De Wert G, Heindryckx B, Pennings G, Clarke A, Eichenlaub-Ritter U, van El CG, Forzano F, Goddijn M, Howard HC, Radojkovic D, Rial-Sebbag E, Dondorp W, Tarlatzis BC & Cornel MC. (2018). Responsible innovation in human germline gene editing: Background document to the recommendations of ESHG and ESHRE. Eur. J. Hum. Genet. , , . PMID: 29326429 DOI.
- ↑ Michalski AM, Richardson SD, Browne ML, Carmichael SL, Canfield MA, VanZutphen AR, Anderka MT, Marshall EG & Druschel CM. (2015). Sex ratios among infants with birth defects, National Birth Defects Prevention Study, 1997-2009. Am. J. Med. Genet. A , 167A, 1071-81. PMID: 25711982 DOI.
- ↑ Miller DT, Adam MP, Aradhya S, Biesecker LG, Brothman AR, Carter NP, Church DM, Crolla JA, Eichler EE, Epstein CJ, Faucett WA, Feuk L, Friedman JM, Hamosh A, Jackson L, Kaminsky EB, Kok K, Krantz ID, Kuhn RM, Lee C, Ostell JM, Rosenberg C, Scherer SW, Spinner NB, Stavropoulos DJ, Tepperberg JH, Thorland EC, Vermeesch JR, Waggoner DJ, Watson MS, Martin CL & Ledbetter DH. (2010). Consensus statement: chromosomal microarray is a first-tier clinical diagnostic test for individuals with developmental disabilities or congenital anomalies. Am. J. Hum. Genet. , 86, 749-64. PMID: 20466091 DOI.
- ↑ Jugessur A, Shi M, Gjessing HK, Lie RT, Wilcox AJ, Weinberg CR, Christensen K, Boyles AL, Daack-Hirsch S, Nguyen TT, Christiansen L, Lidral AC & Murray JC. (2010). Maternal genes and facial clefts in offspring: a comprehensive search for genetic associations in two population-based cleft studies from Scandinavia. PLoS ONE , 5, e11493. PMID: 20634891 DOI.
- ↑ Jefferson A, Colella S, Moralli D, Wilson N, Yusuf M, Gimelli G, Ragoussis J & Volpi EV. (2010). Altered intra-nuclear organisation of heterochromatin and genes in ICF syndrome. PLoS ONE , 5, e11364. PMID: 20613881 DOI.
- ↑ Kuliev A, Cieslak J & Verlinsky Y. (2005). Frequency and distribution of chromosome abnormalities in human oocytes. Cytogenet. Genome Res. , 111, 193-8. PMID: 16192694 DOI.
- ↑ Chavez SL, Loewke KE, Han J, Moussavi F, Colls P, Munne S, Behr B & Reijo Pera RA. (2012). Dynamic blastomere behaviour reflects human embryo ploidy by the four-cell stage. Nat Commun , 3, 1251. PMID: 23212380 DOI.
- ↑ Lee SS, Hadengue A, Girod C, Braillon A & Lebrec D. (1991). Divergent circulatory effects of betaxolol in conscious and anesthetized normal and portal hypertensive rats. J. Hepatol. , 12, 157-61. PMID: 2050994
- ↑ Hook EB. (1981). Rates of chromosome abnormalities at different maternal ages. Obstet Gynecol , 58, 282-5. PMID: 6455611
- ↑ Hook EB, Cross PK & Schreinemachers DM. (1983). Chromosomal abnormality rates at amniocentesis and in live-born infants. JAMA , 249, 2034-8. PMID: 6220164
- ↑ Schreinemachers DM, Cross PK & Hook EB. (1982). Rates of trisomies 21, 18, 13 and other chromosome abnormalities in about 20 000 prenatal studies compared with estimated rates in live births. Hum. Genet. , 61, 318-24. PMID: 6891368
- ↑ GUTHRIE R & SUSI A. (1963). A SIMPLE PHENYLALANINE METHOD FOR DETECTING PHENYLKETONURIA IN LARGE POPULATIONS OF NEWBORN INFANTS. Pediatrics , 32, 338-43. PMID: 14063511
Reviews
Articles
Search Pubmed
Search Pubmed: genetic developmental abnormality
Terms
- anaphase - (Greek, ana = up, again) Cell division term referring to the fourth mitotic stage, where the paired chromatids now separate and migrate to spindle poles. This is followed by telophase.
- Mitosis Phases: prophase - prometaphase - metaphase - anaphase - telophase
- anaphase B - Cell division term referring to the part of anaphase during which the poles of the mitotic spindle move apart. (More? Cell Division - Mitosis)
- aneuploidy - Genetic term used to describe an abnormal number of chromosomes mainly (90%) due to chromosome malsegregation mechanisms in maternal meiosis I.
- disomy - Genetic term referring to the presence of two chromosomes of a homologous pair in a cell, as in diploid. See chromosomal number genetic disorders uniparental disomy and aneuploidy. Humans have pairs usually formed by one chromosome from each parent.
- meiosis I (MI) The first part of meiosis resulting in separation of homologous chromosomes, in humans producing two haploid cells (N chromosomes, 23), a reductional division.
- Meiosis I: Prophase I - Metaphase I - Anaphase I - Telophase I
- meiosis II - (MII) The second part of meiosis. In male human spermatogenesis, producing of four haploid cells (23 chromosomes, 1N) from the two haploid cells (23 chromosomes, 1N), each of the chromosomes consisting of two sister chromatids produced in meiosis I. In female human oogenesis, only a single haploid cell (23 chromosomes, 1N) is produced.
- Meiosis II: Prophase II - Metaphase II - Anaphase II - Telophase II
- prometaphase - (Greek, pro = before) Cell division term referring to the second mitotic stage, when the nuclear envelope breaks down into vesicles. Microtubules then extend from the centrosomes at the spindle poles (ends) and reach the chromosomes. This is followed by metaphase.
- Philadelphia chromosome - (Philadelphia translocation) Genetic term referring to a chromosomal abnormality resulting from a reciprocal translocation between chromosome 9 and 22 (t(9;22)(q34;q11)). This is associated with the disease chronic myelogenous leukemia (CML).
- prophase - (Greek, pro = before) Cell division term referring to the first mitotic stage, when the diffusely stained chromatin resolves into discrete chromosomes, each consisting of two chromatids joined together at the centromere.
- telophase - Cell division term referring to the fifth mitotic stage, where the vesicles of the nuclear envelope reform around the daughter cells, the nucleoli reappear and the chromosomes unfold to allow gene expression to begin. This phase overlaps with cytokinesis, the division of the cell cytoplasm.
- uniparental disomy - Genetic term referring to cells containing both copies of a homologous pair of chromosomes from one parent and none from the other parent.
| Cell Division Terms (expand to view) | ||
|---|---|---|
meiosis | mitosis
| ||
|
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- Australia NHMRC - Genetics in Family Medicine: The Australian Handbook for General Practitioners Testing and pregnancy PDF (2007)
- Online Mendelian Inheritance in Man
- NHGRI Catalog of Published Genome-Wide Association Studies | PDF
- Genome-Wide Associations (GWA) Karyogram
- Idiogram Album David Adler
- NSW Centre for Genetics Education - Fact Sheets
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 19) Embryology Abnormal Development - Genetic. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Abnormal_Development_-_Genetic
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G