Abnormal Development - Environmental: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| Line 48: | Line 48: | ||
* '''Recurrent pregnancy loss: A summary of international evidence-based guidelines and practice'''{{#pmid:30114870|PMID30114870}} "Recurrent pregnancy loss (RPL) is defined as two or more pregnancy losses. It affects <5% of couples. There are many proposed causes; however, in a significant proportion of cases, the cause is unknown. The aim of this paper is to provide a summary of the aetiology, investigations and management of RPL, which is based on the three most recent international guidelines on RPL (European Society of Human Reproduction and Embryology, 2017; American Society for Reproductive Medicine, 2012; and the Royal College of Obstetricians and Gynaecologists, 2011). Management of RPL should occur in a specialised clinic. Appropriate investigations include karyotyping of parents and products of conception, two-dimensional/three-dimensional ultrasonography with sonohysterography, thyroid function tests, and antibodies and testing for acquired thrombophilias. Management options encompass some lifestyle modifications for smoking, alcohol, illicit drug use and caffeine consumption. Acquired thrombophilias should be treated with unfractionated heparin and low-dose aspirin." | * '''Recurrent pregnancy loss: A summary of international evidence-based guidelines and practice'''{{#pmid:30114870|PMID30114870}} "Recurrent pregnancy loss (RPL) is defined as two or more pregnancy losses. It affects <5% of couples. There are many proposed causes; however, in a significant proportion of cases, the cause is unknown. The aim of this paper is to provide a summary of the aetiology, investigations and management of RPL, which is based on the three most recent international guidelines on RPL (European Society of Human Reproduction and Embryology, 2017; American Society for Reproductive Medicine, 2012; and the Royal College of Obstetricians and Gynaecologists, 2011). Management of RPL should occur in a specialised clinic. Appropriate investigations include karyotyping of parents and products of conception, two-dimensional/three-dimensional ultrasonography with sonohysterography, thyroid function tests, and antibodies and testing for acquired thrombophilias. Management options encompass some lifestyle modifications for smoking, alcohol, illicit drug use and caffeine consumption. Acquired thrombophilias should be treated with unfractionated heparin and low-dose aspirin." | ||
|} | |} | ||
{| class="wikitable mw-collapsible mw-collapsed" | {| class="wikitable mw-collapsible mw-collapsed" | ||
| Line 65: | Line 61: | ||
! Older papers | ! Older papers | ||
|- | |- | ||
| | | {{Older papers}} | ||
* '''Impact of sample collection participation on the validity of estimated measures of association in the National Birth Defects Prevention Study when assessing gene-environment interactions'''{{#pmid:29071735|PMID29071735}} "To better understand the impact that nonresponse for specimen collection has on the validity of estimates of association, we examined associations between self-reported maternal periconceptional smoking, folic acid use, or pregestational diabetes mellitus and six birth defects among families who did and did not submit buccal cell samples for DNA following a telephone interview as part of the National Birth Defects Prevention Study (NBDPS). Analyses included control families with live born infants who had no birth defects (N = 9,465), families of infants with anorectal atresia or stenosis (N = 873), limb reduction defects (N = 1,037), gastroschisis (N = 1,090), neural tube defects (N = 1,764), orofacial clefts (N = 3,836), or septal heart defects (N = 4,157). Estimated dates of delivery were between 1997 and 2009. ...These findings support the validity of observed associations in gene-environment interaction studies for the selected exposures and birth defects among NBDPS participants who submitted DNA samples. | |||
* '''Maternal genetic variation accounts in part for the associations of maternal size during pregnancy with offspring cardiometabolic risk in adulthood'''{{#pmid:24670385|PMID24670385}} "Maternal pre-pregnancy body-mass index (ppBMI) and gestational weight gain (GWG) are associated with cardiometabolic risk (CMR) traits in the offspring. The extent to which maternal genetic variation accounts for these associations is unknown. Maternal genetic risk scores (GRS) were created using a subset of SNPs most predictive of ppBMI, GWG, and each CMR trait, selected among 1384 single-nucleotide polymorphisms (SNPs) characterizing variation in 170 candidate genes potentially related to fetal development and/or metabolic risk." | |||
* '''Work and Pregnancy (UK)'''{{#pmid:23472500|PMID23472500}} "Most pregnant women are exposed to some physical activity at work. This Concise Guidance is aimed at doctors advising healthy women with uncomplicated singleton pregnancies about the risks arising from five common workplace exposures (prolonged working hours, shift work, lifting, standing and heavy physical workload). The adverse outcomes considered are: miscarriage, preterm delivery, small for gestational age, low birth weight, pre-eclampsia and gestational hypertension. Systematic review of the literature indicates that these exposures are unlikely to carry much of an increased risk for any of the outcomes, since small apparent effects might be explicable in terms of chance, bias, or confounding, while larger and better studies yield lower estimated risks compared with smaller and weaker studies. In general, patients can be reassured that such work is associated with little, if any, adverse effect on pregnancy." | * '''Work and Pregnancy (UK)'''{{#pmid:23472500|PMID23472500}} "Most pregnant women are exposed to some physical activity at work. This Concise Guidance is aimed at doctors advising healthy women with uncomplicated singleton pregnancies about the risks arising from five common workplace exposures (prolonged working hours, shift work, lifting, standing and heavy physical workload). The adverse outcomes considered are: miscarriage, preterm delivery, small for gestational age, low birth weight, pre-eclampsia and gestational hypertension. Systematic review of the literature indicates that these exposures are unlikely to carry much of an increased risk for any of the outcomes, since small apparent effects might be explicable in terms of chance, bias, or confounding, while larger and better studies yield lower estimated risks compared with smaller and weaker studies. In general, patients can be reassured that such work is associated with little, if any, adverse effect on pregnancy." | ||
Revision as of 07:41, 4 January 2019
| Embryology - 25 Apr 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
| Educational Use Only - Embryology is an educational resource for learning concepts in embryological development, no clinical information is provided and content should not be used for any other purpose. |
Introduction
Materal effects should really be called environmental (in contrast to genetic) removing the association of mother with the deleterious agent. Accepting this caveat, there are several maternal effects from lifestyle, environment and nutrition that can be prevented or decreased by change which is not an option for genetic effects.
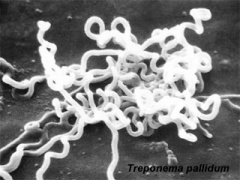
Infections, collectively grouped under the acronym TORCH for Toxoplasmosis, Other organisms (parvovirus, HIV, Epstein-Barr, herpes 6 and 8, varicella, syphilis, enterovirus) , Rubella, Cytomegalovirus and Hepatitis. See related pages on maternal hyperthermia, viral and bacterial infections.
Maternal diet the best characterised is the role of low folic acid and Neural Tube Defects (NTDs) see also abnormal neural development and Neural Tube Defects and the sample environmental effects listed below.
Maternal drugs effects either prescription drugs (therapeutic chemicals/agents, thalidomide limb development), non-prescription drugs (alcohol, smoking, herbal drugs), and illegal drugs (Cannabis/Marijuana, Methamphetamine/Amphetamine, Cocaine, Heroin, Lysergic Acid Diethylamide)
Environment (smoking, chemical, heavy metals) and maternal endocrine function (maternal diabetes, thyroid development) and maternal stress.
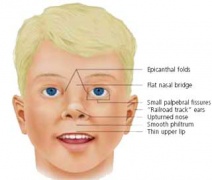
Different environmental effects can act individually or in combination on the same developing system. For example, neural development can be impacted upon by alcohol (fetal alcohol syndrome), viral infection (rubella) and/or inadequate dietry folate intake (neural tube defects). These effects may also not be seen as a direct effect on a system or systems but result in a reduced birth weight and the potential postnatal developmental effects.
Finally, when studying this topic remember the concept of "critical periods" of development that will affect the overall impact of the above listed factors. This can be extended to the potential differences between prenatal and postnatal effects, for example with infections and outcomes.
This current page provides only a general overview of the topic, use the links below to get detailed information about specific environmental effects.
| Bacterial Links: bacterial infection | syphilis | gonorrhea | tuberculosis | listeria | salmonella | TORCH | Environmental | Category:Bacteria |
| Abnormality Links: abnormal development | abnormal genetic | abnormal environmental | Unknown | teratogens | ectopic pregnancy | cardiovascular abnormalities | coelom abnormalities | endocrine abnormalities | gastrointestinal abnormalities | genital abnormalities | head abnormalities | integumentary abnormalities | musculoskeletal abnormalities | limb abnormalities | neural abnormalities | neural crest abnormalities | placenta abnormalities | renal abnormalities | respiratory abnormalities | hearing abnormalities | vision abnormalities | twinning | Developmental Origins of Health and Disease | ICD-11 | ||
|
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Environmental Abnormal Development <pubmed limit=5>Environmental Abnormal Development</pubmed> |
| Older papers |
|---|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
|
Critical Periods
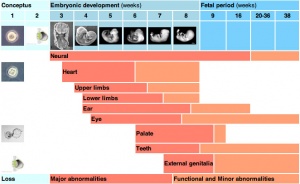
The table below identifies approximate windows of time, "critical periods", that following exposure to teratogens can lead to developmental abnormalities (anomalies, congenital). In general, the effects for each system are more severe (major anomalies) in the embryonic period during organogenesis in the first trimester. Later teratogen exposure are less severe (minor anomalies) in the fetal period during continued growth and differentiation in the second and third trimester.
| Critical Periods of Human Development | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Conceptus | Embryonic development (weeks) | Fetal period (weeks) | ||||||||||||||||||
|
||||||||||||||||||||
| Neural | ||||||||||||||||||||
| Heart | ||||||||||||||||||||
| Upper limbs | ||||||||||||||||||||
| Lower limbs | ||||||||||||||||||||
| Ear | ||||||||||||||||||||
| Eye | ||||||||||||||||||||
| Palate | ||||||||||||||||||||
| Teeth | ||||||||||||||||||||
| External genitalia | ||||||||||||||||||||
| Loss | Major abnormalities | Functional and Minor abnormalities | ||||||||||||||||||
| ||||||||||||||||||||
DevTox
The potential of a pesticide or biocide to cause adverse effects in the developing embryo or fetus is an important consideration in any health risk assessment for humans and wildlife.
Report of the 8th Berlin Workshop on Developmental Toxicity held in May 2014.[10]
- "The main aim of the workshop was the continuing harmonization of terminology and innovations for methodologies used in the assessment of embryo- and feto-toxic findings. The following main topics were discussed: harmonized categorization of external, skeletal, visceral and materno-fetal findings into malformations, variations and grey zone anomalies, aspects of developmental anomalies in humans and laboratory animals, and innovations for new methodologies in developmental toxicology. The application of Version 2 terminology in the DevTox database was considered as a useful improvement in the categorization of developmental anomalies."
- Links: DevTox
Travel
There is an increasing number of women travelling during pregnancy that may carry some additional environmental risks. The following information is summarised from a recent BMJ article.[11]
- second trimester of pregnancy is considered the safest in which to travel
- air travel may carry risk of miscarriage, preterm birth, and thromboembolism
- obstetric and neonatal care facilities at destinations is varied
- obtain adequate insurance and check with their airline for restrictions on travel
- communicable diseases acquired abroad may increase risks of perinatal morbidity
References
- ↑ Jacob S, Dötsch A, Knoll S, Köhler HR, Rogall E, Stoll D, Tisler S, Huhn C, Schwartz T, Zwiener C & Triebskorn R. (2018). Does the antidiabetic drug metformin affect embryo development and the health of brown trout (Salmo trutta f. fario)?. Environ Sci Eur , 30, 48. PMID: 30595998 DOI.
- ↑ Hong Li Y & Marren A. (2018). Recurrent pregnancy loss: A summary of international evidence-based guidelines and practice. Aust J Gen Pract , 47, 432-436. PMID: 30114870
- ↑ Jenkins MM, Reefhuis J, Herring AH & Honein MA. (2017). Impact of sample collection participation on the validity of estimated measures of association in the National Birth Defects Prevention Study when assessing gene-environment interactions. Genet. Epidemiol. , 41, 834-843. PMID: 29071735 DOI.
- ↑ Wander PL, Hochner H, Sitlani CM, Enquobahrie DA, Lumley T, Lawrence GM, Burger A, Savitsky B, Manor O, Meiner V, Hesselson S, Kwok PY, Siscovick DS & Friedlander Y. (2014). Maternal genetic variation accounts in part for the associations of maternal size during pregnancy with offspring cardiometabolic risk in adulthood. PLoS ONE , 9, e91835. PMID: 24670385 DOI.
- ↑ Palmer KT, Bonzini M & Bonde JP. (2013). Pregnancy: occupational aspects of management: concise guidance. Clin Med (Lond) , 13, 75-9. PMID: 23472500
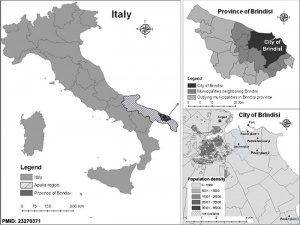
- ↑ Gianicolo EA, Bruni A, Rosati E, Sabina S, Guarino R, Padolecchia G, Leo C, Vigotti MA, Andreassi MG & Latini G. (2012). Congenital anomalies among live births in a polluted area. A ten-year retrospective study. BMC Pregnancy Childbirth , 12, 165. PMID: 23270371 DOI.
- ↑ Alexander PG & Tuan RS. (2010). Role of environmental factors in axial skeletal dysmorphogenesis. Birth Defects Res. C Embryo Today , 90, 118-32. PMID: 20544699 DOI.
- ↑ Zeller R. (2010). The temporal dynamics of vertebrate limb development, teratogenesis and evolution. Curr. Opin. Genet. Dev. , 20, 384-90. PMID: 20537528 DOI.
- ↑ West PR, Weir AM, Smith AM, Donley EL & Cezar GG. (2010). Predicting human developmental toxicity of pharmaceuticals using human embryonic stem cells and metabolomics. Toxicol. Appl. Pharmacol. , 247, 18-27. PMID: 20493898 DOI.
- ↑ Solecki R, Rauch M, Gall A, Buschmann J, Clark R, Fuchs A, Kan H, Heinrich V, Kellner R, Knudsen TB, Li W, Makris SL, Ooshima Y, Paumgartten F, Piersma AH, Schönfelder G, Oelgeschläger M, Schaefer C, Shiota K, Ulbrich B, Ding X & Chahoud I. (2015). Continuing harmonization of terminology and innovations for methodologies in developmental toxicology: Report of the 8th Berlin Workshop on Developmental Toxicity, 14-16 May 2014. Reprod. Toxicol. , 57, 140-6. PMID: 26073002 DOI.
- ↑ Hezelgrave, NL, Whitty, CJM, Shennan, AH, and Chappell, LC. Advising on travel during pregnancy BMJ 2011; 342:d2506 doi: 10.1136/bmj.d2506 (Published 28 April 2011) BMJ
Journals
- Environmental Health Perspectives (EHP) is a monthly journal of peer-reviewed research and news on the impact of the environment on human health. EHP | Pubmed EHP
Reviews
Sadler TW. (2017). Establishing the Embryonic Axes: Prime Time for Teratogenic Insults. J Cardiovasc Dev Dis , 4, . PMID: 29367544 DOI.
Foster WG, Evans JA, Little J, Arbour L, Moore A, Sauve R, Andrés León J & Luo W. (2017). Human exposure to environmental contaminants and congenital anomalies: a critical review. Crit. Rev. Toxicol. , 47, 59-84. PMID: 27685638 DOI.
Brent RL. (2004). Environmental causes of human congenital malformations: the pediatrician's role in dealing with these complex clinical problems caused by a multiplicity of environmental and genetic factors. Pediatrics , 113, 957-68. PMID: 15060188
Articles
Search Pubmed
June 2010 "teratogens" All (25401) Review (3026) Free Full Text (3991) "TORCH Infections" All (183) Review (37) Free Full Text (18)
Search Pubmed: teratogens | TORCH Infections | maternal abnormalities
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- REPROTOX - contains summaries on the effects of medications, chemicals, infections, and physical agents on pregnancy, reproduction, and development.
- DevTox
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 25) Embryology Abnormal Development - Environmental. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Abnormal_Development_-_Environmental
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G