ANAT2341 Lab 4 - Implantation and Villi Development
| ANAT2341 Lab 4: Introduction | Implantation and Villi | Decidua and Cord | Abnormal Placenta | Cardiovascular | Online Assessment | Group Project |
Early Placenta
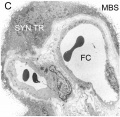
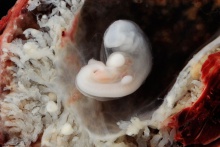
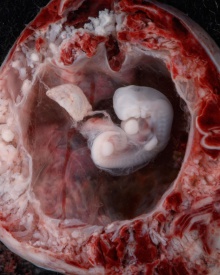
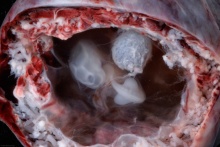
| Implantation | Uterine surface view of implantation site | |

|
|
|
|
|
|
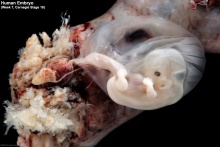
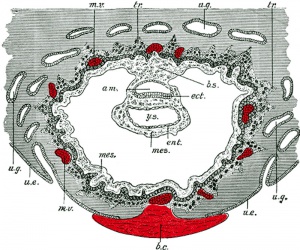
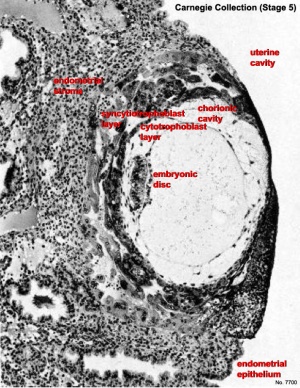
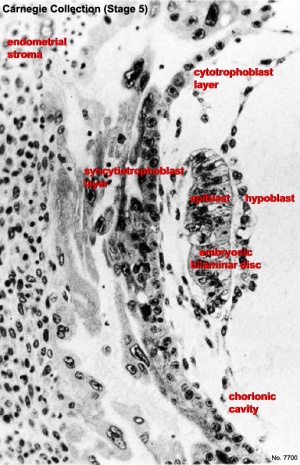
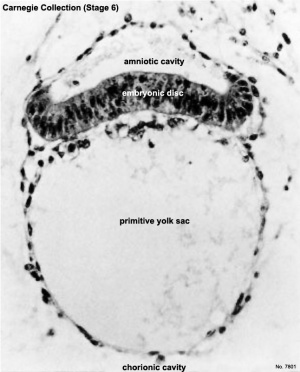
| Human Embryo - early implantation (stage 5) | Bilaminar Embryo (detail) | Bilaminar Embryo (stage 6) |
Simplified Cartoons
Movies
|
|
|
|
Chorionic Villi
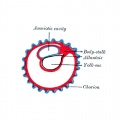
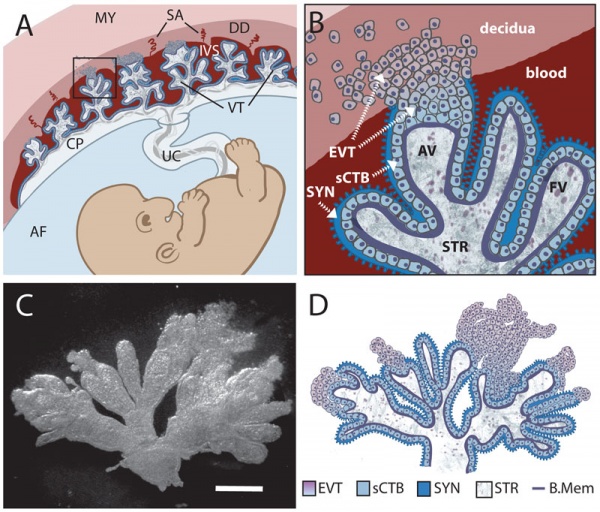
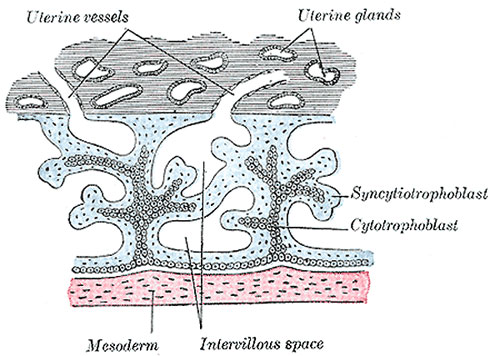
Primary villiWeek 2 - first stage of chorionic villi development. Trophoblastic shell cells (syncitiotrophoblasts and cytotrophoblasts) form finger-like extensions into maternal decidua. |
|
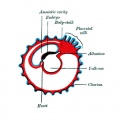
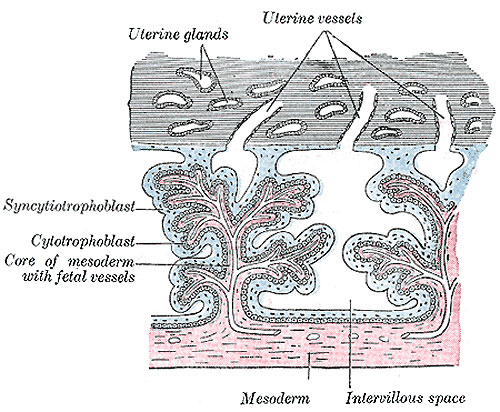
Secondary villiWeek 3 - second stage of chorionic villi development Extra-embryonic mesoderm grows into villi, covers the entire surface of chorionic sac. Basal region will form chorionic plate. |
|
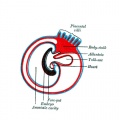
Tertiary villiWeek 4 - third stage of chorionic villi development. Mesenchyme differentiates into blood vessels and cells, forms arteriocapillary network, fuse with placental vessels, developing in connecting stalk. |
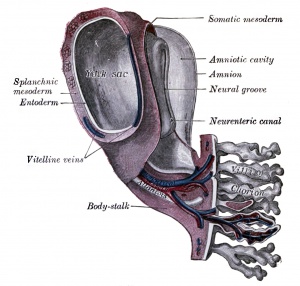
|
- stem villi - or anchoring villi, cytotrophoblast cells attached to maternal tissue.
- branched villi - grow from sides of stem villi, region of main exchange, surrounded by maternal blood in intervillous spaces.
- terminal villi - not active outgrowths caused by proliferation of the trophoblast. Passive protrusions induced by capillary coiling due to growth of the fetal capillaries within the mature intermediate villi (third trimester).
- chorionic plate - region of membrane at the base of the villi through which placental arteries and vein passes.
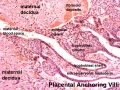
Anchoring Villi
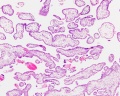
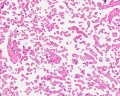
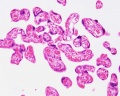
| Placental Villi Histology
|
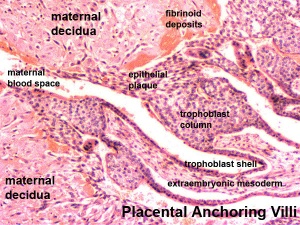
|
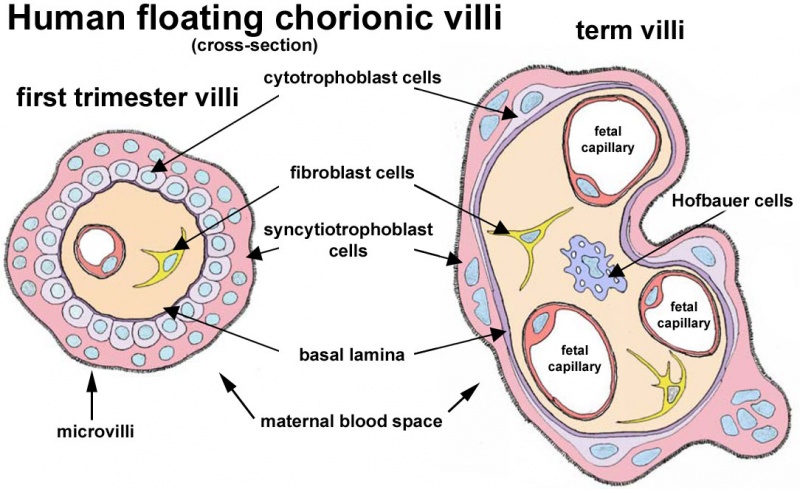
Villi Development
| First Trimester | Third Trimester |
|---|---|
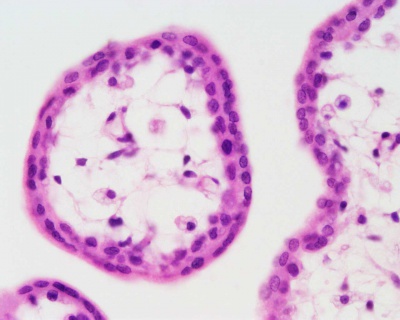
|
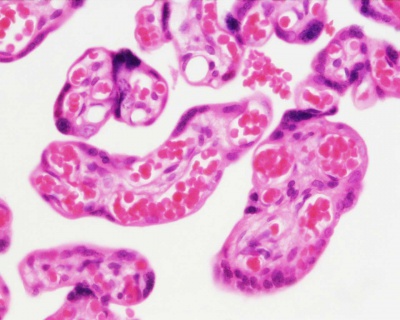
|
Virtual Slide
We will now look at an example of first trimester placentation in a Virtual Slide.
Please note that there are additional slides listed in the current set, only the first placenta slide and the cord cross-section will be covered in detail in the practical class.
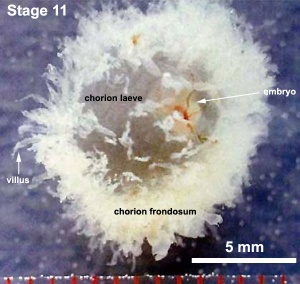
Chorionoic Villi Location
Originally villi cover entire chorionic surface and then become restricted to decidua basalis region forming 2 regions:
- Frondosum - "leafy" where villi are mainly located.
- Capsularis - smooth chorion, where villi are absent or not abundant.
|
|
|
|
|
|
|
Terms
- adplantation - The term used to describe the initial process of the blastocyst (conceptus) attachment to the uterine endometrium wall at the site of implanation following hatching from the zona pellucida.
- cytotrophoblast - The "cellular" trophoblast layer surrounding (forming a "shell") the early implanting conceptus. Beginning at uterine adplantation, proliferation and fusion of these cells is thought to form a second outer trophoblast layer, the syncytiotrophoblast. The cytotrophoblast layer contributes to formation of the placental villi, the functional component of the fetal placenta.
- decidua basalis - The term given to the uterine endometrium at the site of implantation where signaling transforms the uterine stromal cells (fibroblast-like) into decidual cells. This forms the maternal component of the placenta, the decidualization process gradually spreads through the remainder of the uterus, forming the decidua parietalis.
- decidualization - The process by which uterine stromal cells differentiate in response to both steroid hormones and embryonic signals into large epitheliod decidual cells. This process is essential for the progress of implantation and establishing fetal-maternal communication.
- endometrial gland - The mucous secreting gland associated with the epithelium lining the uterus. These glands develop and secrete each menstrual cycle and are thought to provide initial blastocyst nutrition prior to implantation.
- endometrium - The epithelium lining of the non-pregnant uterus. During pregnancy this epithelium undergoes changes described as the decidual reaction and is renamed the "decidua".
- extraembryonic coelom - The space found outside the embryo, amniotic cavity, yolk sac and chorionic cavity.
- extraembryonic mesoderm - Cells from the conceptus that contribute to placenta and fetal membranes. Described as "extraembryonic" because it is tissue lying outside the embryonic trilaminar disc (ectoderm, mesoderm and endoderm) and "mesoderm", because of the connective tissue cellular organization. In animal models, this extraembryonic mesoderm has been shown to arise from the same source as embryonic mesoderm during gastrulation.
- haemochorial - The type of placenta where the chorion comes in direct contact with maternal blood. This is the type of human placentation.
- implantation - The term used to describe the process of conceptus invasion of the uterus endometrium (epithelium and underlying stroma) by the blastocyst (conceptus). This process follows conceptus adplantation (attachment) to the endometrium. Abnormal implantation is where this process does not occur in the body of the uterus (ectopic) or where the placenta forms incorrectly. In humans, implantation occurs during the second week of development.
- placenta - (Greek, plakuos = flat cake) The developmental organ formed from maternal and fetal contributions in animals with placental development. In human, the placenta at term is a discoid shape "flat cake" shape; 20 cm diameter, 3 cm thick and weighs 500-600 gm. Placenta are classified by the number of layers between maternal and fetal blood (Haemochorial, Endotheliochorial and Epitheliochorial) and shape (Discoid, Zonary, Cotyledenary and Diffuse). The functional exchange region are the placental villi or chorionic villi. The placenta has many different functions including metabolism, transport and endocrine.
- syncytiotrophoblast - A multinucleated cell currently thought to form by the fusion of another trophoblast cell the cytotrophoblasts, within the trophoblast layer (shell) of the implanting conceptus. In early development, these cells mediate implantation of the conceptus into the uterine wall and secrete the hormone (human Chorionic Gonadotrophin, hCG) responsible for feedback maintainance of the corpus luteum (in maternal ovary) and therefore maintaining early pregnancy.
- villi - Plural of villus, which is a thin projection from a surface. A term used to describe the many functional units together of the fetal placenta.
- villous cytotrophoblast - (VCT) Trophoblast cells located on chorionic villi (as opposed to extravillous cytotrophoblasts) that can also fuse to form the syncytiotrophoblasts.
| ANAT2341 Lab 4: Introduction | Implantation and Villi | Decidua and Cord | Abnormal Placenta | Cardiovascular | Online Assessment | Group Project |
Additional Information
| Additional Information - Content shown under this heading is not part of the material covered in this class. It is provided for those students who would like to know about some concepts or current research in topics related to the current class page. |
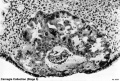
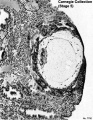
Carnegie Stage 5
Historically this early implantation stage was divided into 3 separate sub-stages (a-c).
Stage 5a
Stage 5b
Stage 5c
Maternal Immune
How does the implanting conceptus avoid immune rejection by the maternal immune system? There are a number of maternal and embryonic mechanisms that are thought to act to prevent immune rejection of the implanting conceptus, though the complete mechanism(s) are unknown. This is particularly relevant to Assisted Reproductive Technologies involving donor eggs.
Below are some examples of research on this topic.
Decidual Immune Cells
- Specialised immune cells.
| Decidual Macrophages (Mϕ) | Decidual T cells | Uterine Natural Killer cells |
|---|---|---|
|
|
|
Chemokine Gene Silencing
- Remove the attraction of maternal immune cells.
A mouse study[1] has shown that the normal immune response to inflammation, accumulation of effector T cells in response to chemokine secretion does not occur during implantation. This is prevented locally by epigenetic silencing of chemokine expression in the decidual stromal cells.
Corticotropin-Releasing Hormone
- Kill the maternal immune cells.
Both maternal and implanting conceptus release CRH at the embryo implantation site. This hormone then binds to receptors on the surface of trophoblast (extravillous trophoblast) cells leading to expression of a protein (Fas ligand, FasL) that activates the extrinsic cell death pathway on any local maternal immune cells ( T and B lymphocytes, natural killer cells, monocytes and macrophages).[2] (Note - This cannot be the only mechanism, as mice with dysfunctional FasL proteins are still fertile).
Human Villi Timeline
The placental vill development data below is based upon a recent immunochemistry confocal laser scanning microscope (CLSM) study.[1]
Note that the paper uses clinical gestational age (GA) from last menstrual period (LMP) and has been corrected for post-conception (fertilization) age, approximately 14 days later.
| Fertilization Age
(weeks) |
Gestational Age
(weeks) |
Vessel Lumen Diameter
(range in microns, µm) |
Features |
| 3 to 4 | 5 and 6 | 10 - 15 |
|
| 5 to 6 | 7 and 8 | 10 - 26 |
|
| 7 to 8 | 9 and 10 | 60 - 75 two central vessels
26 - 34 capillary network |
|
| 9 to 10 | 11 and 12 | 70 - 90 two central vessels
26 - 34 capillary network |
|
Reference
- ↑ <pubmed>17545656</pubmed>
Cytotrophoblast Layer
There is a new interpretation of the changes that are occuring in the cytotrophoblast (CTB) layer during early to full-term human placenta development. Traditionally the interpretation was that the cytotrophoblast layer thinned and became discontinuous towards term. The thinning is thought due to the epithelium surface expanding at a faster rate than its volume. Two recent studies suggest that while the cytotrophoblast layer does indeed thin, it does not become discontinuous.
Syncytiotrophoblast Layer
The syncytiotrophoblast (STB) layer forms the epithelial covering of the entire villous tree. These cells are multinucleated, terminally-differentiated syncytium formed by the fusion of the underlying progenitor cytotrophoblast (CTB) cells. The process is described as "syncytialization" and is mediated by syncytin-1, an envelope protein of a human endogenous retrovirus W (HERV-W). The differentiation is regulated by chorionic gonadotropin (hCG) and the fusion of cytotrophoblast cells is ongoing during placental development.
Cellular parts derived from the syncytiotrophoblasts (apoptotic nuclei and microparticulate debris) can be shed into the maternal blood in which they are bathed. The apototic process appears to be part of the fusion mechanism between cytotrophoblast and the overlying multinucleate syncytiotrophoblast layer.
Studies have suggested that these cells are transcriptionally inactive. A recent study using a number of different detection techniques now suggests that at least some of the cells nuclei may still be transcriptionally inactive.
| ANAT2341 Lab 4: Introduction | Implantation and Villi | Decidua and Cord | Abnormal Placenta | Cardiovascular | Online Assessment | Group Project |
| ANAT2341 Course Timetable | |||
|---|---|---|---|
| Week (Mon) | Lecture 1 (Mon 1-2pm) | Lecture 2 (Tue 3-4pm) | Practical (Fri 1-3pm) |
| Week 2 (1 Aug) | Introduction | Fertilization | Lab 1 |
| Week 3 (8 Aug) | Week 1 and 2 | Week 3 | Lab 2 |
| Week 4 (15 Aug) | Mesoderm | Ectoderm | Lab 3 |
| Week 5 (22 Aug) | Early Vascular | Placenta | Lab 4 |
| Week 6 (29 Aug) | Gastrointestinal | Respiratory | Lab 5 |
| Week 7 (5 Sep) | Head | Neural Crest | Lab 6 |
| Week 8 (12 Sep) | Musculoskeletal | Limb Development | Lab 7 |
| Week 9 (19 Sep) | Renal | Genital | Lab 8 |
| Mid-semester break | |||
| Week 10 (3 Oct) | Public Holiday | Stem Cells | Lab 9 |
| Week 11 (10 Oct) | Integumentary | Endocrine | Lab 10 |
| Week 12 (17 Oct) | Heart | Sensory | Lab 11 |
| Week 13 (24 Oct) | Fetal | Birth and Revision | Lab 12 |
|
ANAT2341 2016: Moodle page | ECHO360 | Textbooks | Students 2016 | Projects 2016 | |||