2017 Group Project 5
| 2017 Student Projects | |||
|---|---|---|---|
|
Lungs
Mark Hill (talk) 16:15, 14 September 2017 (AEST) OK Feedback
- Better progress than some (in specific sub-headings)
- Long list of sub-headings but only the first few topics populated.
- No reference sources on teh page or allocated to topics.
- Where is the research
- Glossary of words used here.
An introduction to the lungs...
On this page, we will be exploring the development of the lungs through the stages of embryonic growth.
Lung Anatomy
Medina -
Draw diagram of lung anatomy and upload picture
Lung Histology
Medina -
Draw diagram of lung histology and upload picture
Developmental origin overview
A brief summary of the embryonic development of the lungs:[1]
Day 22 - Lung development begins. Respiratory diverticulum forms from the ventral outpouching of the endodermal foregut.
Day 26-28 – Respiratory diverticulum undergoes bifurcation into right and left primary bronchial/lung buds.
Weeks 5-28 – Primary bronchial bugs undergo sixteen rounds of branching to generate the respiratory tree of the lungs. This produces secondary bronchial buds, the lung lobes, tertiary bronchial buds, bronchopulmonary segments of the mature lung, terminal bronchioles and respiratory bronchioles.
Week 36-Birth – Terminal branches of lungs are in a dense network of capillaries and are called terminal sac (primitive alveoli). They then begin to differentiate into mature alveoli which continue to form until 8 years old.
Developmental timeline
| The Embryonic stage is the first stage of lung development. It is identified by the emergence of lung buds in the ventral wall of the foregut; these lung buds will later divide to form lobar divisions.The endoderm is responsible for the epithelium of the lung buds which will later differentiate into specialised respiratory epithelium. The mesoderm is responsible for the mesenchyme surrounding the lung buds. | Christian Pander, Karl Ernst von Baer, and Heinrich Rathke were among the first to use a new wave of technology in embryology; involving the use of new staining techniques and improved microscopy. Their findings together identified the presence of primary germ layers (ectoderm, endoderm and mesoderm) and the development of early organs. [2] | ||
| The Pseudoglandular stage of lung development is named after its histological appearance which is much like compound tubular glands. This is due to the dichotomous branching of conducting airways in the lung which is repeated up until the 16th week where they will be fully formed [3]. However, these branchings do not yet have functional alveoli; instead, specialised respiratory cells begin to develop. Crucially important to the branching of the airways is the presence of bronchial mesoderm as proven by Spooner & Wessells in 1970 (see history). | In 1970, an experiment by Spooner and Wessells demonstrated the need for the presence of surrounding bronchial mesoderm for adequate bronchial branching. [4]. This was done through in vitro experiments with mice.
Additionally, In 1976 Masters published his work on the importance of epithelial-mesenchymal interactions during lung development. [5] This significance of this work is the discovery that the bronchial epithelium lining the primitive airways interacts with the mesenchyme, to then differentiate into specialised alveolar epithelium. | ||
Structure of respiratory network
Physiologically, the organ can be divided into two parts:
The Conducting system – consists of all tubular structures including the larynx, trachea and bronchi. (image)
The Functional unit – An alveolus containing specialised epithelial cells where gas exchange occurs.
By week 8 of development, the lungs are in the development of the pseudoglandular stage (refer to developmental timeline). The three germ layers formed in gastrulation all contribute to the development of the lung, including signalling for a cascade of events as well as branching of the bronchiole.
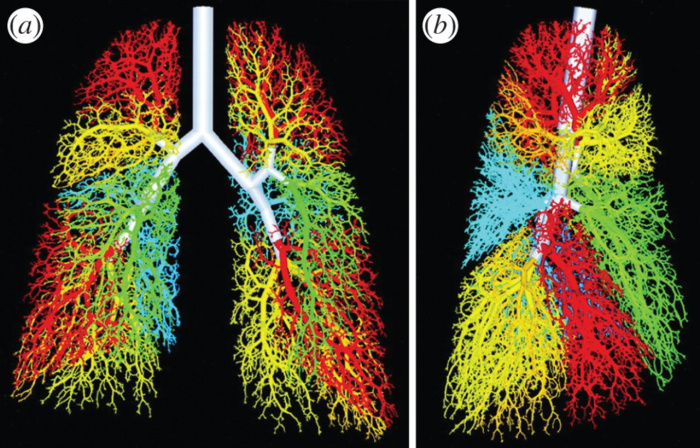
A three-dimensional fractal model of an airway tree with 54 611 branches; branches distal to different segmental bronchi are shown in same colour as segmental bronchus. (a) Anterior view and (b) right lateral view
The Conducting System
Branching morphogenesis is observed in many organ systems, including the lungs. It has been of great interest and has been studied in great detail. The bronchial tree arises from the sequential use of three simple modes of branching.
These modes include:
1. Domain branching
2. Planar bifurcation
3. Orthogonal bifurcation
Trifurcations have also been observed as contributing the backbone of the respiratory tree, however it is not as prevalent.
These branching structures involve are regulated by a network of signalling factors. To form a branched structure, signalling molecules have to form a pattern in space that precedes bud outgrowth. This is assisted with the molecule FGF10 and will be further explored. For direct elongation, FGF10 has a higher concentration at the distal tip of the lung bud allowing direct elongation of the structure. In terminal branching, there is a split localisation of FGF10 and results in a terminally branched structure. For lateral branching, FGF10 is restricted to being a single spots on the side allowing the structure to grow laterally. FGF10 appears to drive outgrowth of lung buds, as well as other organs.
With regards to early lung development, transitions from one mode of branching to the other occur to ultimately build the lung tree. In the domain branching mode, the lung bud elongates and new buds first appear on one side of the stalk, perpendicular to the main axis on either sides of the stalk. Domain branching is used to build the backbone of the respiratory tree.
Planar and orthogonal bifurcations represent two consecutive rounds of branching, however they differ in the second round as they branch in the same plane as planar bifurcations. Planar and orthogonal bifurcations create lobes surfaces and fill the interior. The branching process is controlled by genetic information and is tightly regulated. In the lung, dichotomous branching gives rise to two daughter branches with a smaller diameter than the mother branch.
In earlier studies, lung branching has been proposed to be influenced by the viscosity of amniotic fluid and the mesenchyme, separated by a ‘skin’ of surface tension, the epithelium. However, more recently this has been negated as branching can occur without a mesenchyme, without growth and the robustness of the branching process suggests that it is a highly controlled process. Signalling factors play a key role in branching morphogenesis. A recent study has shown that branching can still occur in the absence of mesenchyme, only if the appropriate signalling factors are added.
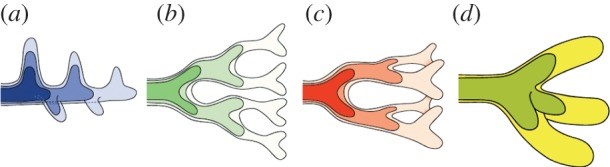
This image is a stylised representation of the modes of lung branching.
a) lateral branching, b) planar bifurcation, c) orthogonal bifurcation, d) trifurcation
This image is a stylised typical developmental branching pattern over time in a lung bud.
Alveolus: the functional unit
The alveolus are small "sac-like structures" in which gas exchange occurs across. Within the alveolus there are two types of cells that line the sacs. These are type I and type II alveolar cells, these cells must differentiate in a process known as alveolar differentiation and are both crucial for gas exchange.
Type I: Type I cells are flat and cover more than 90% of the alveolar surface in which gases diffuse across.
Type II: Type II cells are cuboidal shaped and synthesise pulmonary surfactants that hydrate and prevent the alveolar collapsing into itself by reducing surface tension.
It was previously thought that alveolar type I cells arise from type II cells, however more recent studies suggest that they both arise from a bipotent progenitor. After birth, type I cells are derived from rare, self-renewing, mature, long-living alveolar type II cells, that produce slowly, gradually expanding the the clonal foci of alveolar renewal.
Alveolar differentiation occurs in the distal region of the developing airway tree. Studies have found that over development there is an increase in alveolar differentiation and a decrease in branching morphogenesis as well as alveolar differentiation expanded distally over time.
ECAD (a cell junction protein stain) staining showed that undifferentiated cells at the branch tips were clustered and cuboidal, whereas differentiated alveolar cells (type1 and type 2) were at the non-branch tips and were flat and isolated cuboidal cells. This study suggests that in late lung stages branching continues at the distal edge of the airway tree whilst leaving behind cells undergoing alveolar differentiation. A genetic factor involved in alveolar differentiation is expression of hyperactive Kras, which expands the branching of lungs, however reducing the differentiation of alveolar cells and suppresses cell flattening, a hallmark of alveolar cells.
One study, suggested that mothers who are overweight when pregnant can potentially effect the fetus in terms of lung development and air breathing at birth. The study looked at sheep who over-nourished their young, and found that the after birth the lambs who had overweight mothers had a reduced capacity for surfactant production as well as altered transport mechanisms within cells. This research can assist with the diagnosing and preventing potentially detrimental conditions that can occur during pregnancy.
- Not complete more content to be added
Developmental signalling processes
The development of a mammalian lung is a multi-step and highly complex process involving signalling pathways. This hierarchy process, referred to as branching morphogenesis is essential to generate numerous airways and gas-exchanging units, and is critically regulated by interactions of signalling pathways in the epithelium and mesenchyme.
Several growth factors and chemical signals have been identified to influence lung development. The main signalling molecules include:
1. Fibroblast Growth Factor (FGF10) - serves as a signalling cue for epithelium outgrowth in the mesenchyme.
2. Sonic Hedgehog (SHH) - produced in the epithelium and is involved in regulating FGF10 expression, leading to the intertubular mesenchyme to facilitate growth and formation of epithelial buds.
3. Sox9 - promotes proper branching morphogenesis by balancing the proliferation and differentiation of epithelial tip progenitor cells, whilst regulating the extracellular matrix. It is expressed at the distal tips of branching epithelium and controls multiple aspects of lung branching.
4. Heparan Sulfate Glycosaminoglycans (HS-GAG) - interacts with SHH in order to produce epthelial cells and lung morphogenesis. There is still a lack of understanding in the role that HS plays in mammalian lung development.
During branching morphogenesis, the distal tips of the branching epithelium contain a distinct population of progenitor cells that give rise to all epithelial types in early lung development, but become developmentally restricted after embryonic day 16.5 in mice. Because this epithelium is highly proliferative population of cells, a balance between differentiation and proliferation must be maintained during lung development. After embryonic day 16.5, Sox9 is down-regulated as differentiation begins, with Sox9 being expressed in the highest concentration where two new buds will form, and lowest where the cleft forms. Two core signalling proteins consist of FGF10 and SHH. FGF10 has been shown to induce outgrowth of lung buds. FGF10 and SHH also engage in a negative feedback loop, in that FGF10 signalling induces SHH expression in the epithelium. This expression of SHH causes a repression in FGF10 expression in the mesenchyme of the tissue.
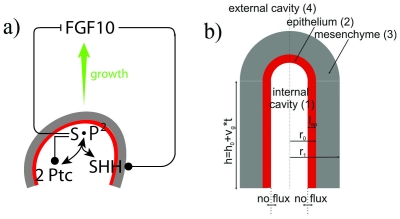
a) FGF10 is transcribed at high levels in the distal mesenchyme (grey area). FGF10 stimulates SHH expression in the epithelium (red), thus promoting proliferation and outgrowth shown by the green arrow. b) The epithelium and mesenchyme are shown in red and grey respectively, showing the outgrowth of mesenchyme after the signalling pathway between both FGF10 and SHH.
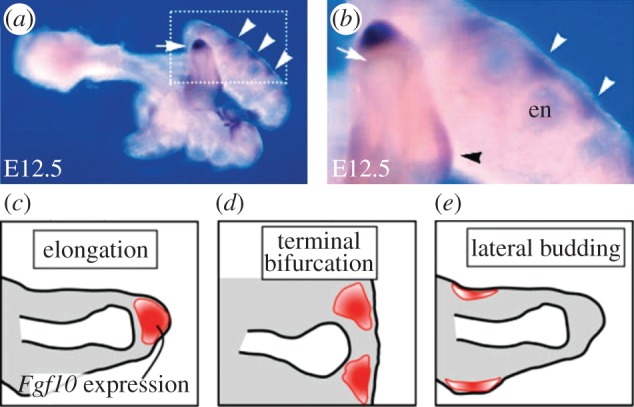
This image shows three spatial locations of where concentrations of FGF10 are expressed, in order to generate different branching modes c) elongation d) terminal bifurcation e) lateral budding. This model is used in modern research, outlining the development of the conducting system of the lung
A recent study found that the production of a biologically active form of SHH was decreased after a loss of HS-GAG in the epithelium, highlighting the crucial requirement of HS-GAG in SHH-producing epithelial cells to maintain SHH signalling activity in the event of lung morphogenesis.
The branching pattern and branching rate are sensitive to the changes in the mesoderm shape and volume. The growth of the epithelial tree is likely to adapt to fill the available space in the mesenchyme.
Current understandings and areas of research
include any relevant articles
Review and research articles
Movies
Animal models
Mouse models
Key pathways that maintain the mesenchymal-epithelial interactions that allow normal embryological lung development: VEGF, Bmp, Wnt.... Sox 2
1. Wnt7b/Fzd2
Wnt signaling pathway involves the binding of the Wnt ligand to the Frizzled family receptor that can elicit different effects depending on the type of Wnt pathway (noncanonical/calcium, canonical, noncanonical planar cell polarity). Canonical Wnt pathway has a signalling role in embryonic lung development and with the action of β-Catenin by trans-activating the LEF/TCF pathway, which advances epithelial proliferation, differentiation and tissue development. On the other hand, the noncanonical pathway has been suggested to be a modulator of epithelial cell shape and cytoskeletal structure. To examine the function of Fzd2, mouse models were developed by in attempt to delete the Fzd2 gene by crossing over Fzd2 flox/flox allele mice with Shh cre allele mice. In the embryonic chimeric mice, at day 12.5, expression of Fzd2 was absent and by day 14.5 large cysts were observed in the distal lung region. It was also noted that in Fzd2 mutant mice, airways were shorter and wider and presence of planar bifurcation, leading to large cysts rather than distal branching. There were also molecular changes in signalling processes for lung branching morphogenesis involving the factors Fgf10, Bmp4, Fgfr2, and Shh. From the data, it is evident of Wnt7b/Fzd2's role in the modulation of lung epithelial cell shape and initiation of branch points.
2. Sox 2
Sox 2 - branching morphogenesis and epithelial cell differentiation. - Sox 2 is a Sry related HMG - There is an increased expression of Sox 2 in unbranched lung epithelium and is absent in branching regions - Development of a transgenic mice with doxycycline inducible Sox2 continuously expressed in their lung epithelium - Results showed a diminution of branching airways and alveoli bronchiolization - Driving precursor-like cells to a committed state (cGRP positive neuroendocrine cells and ΔNp63 isoform expressing (pre-) basal cells)
3. GATA6
GATA6 - transcriptional factor
- visceral endoderm differentiation
- expressed in early development of bronchial epithelium
- required for regeneration of pulmonary epithelium
- Mouse model -->
4. Gli2 & 3
Abnormal development
Newborn Respiratory Distress Syndrome
Newborn respiratory distress syndrome (NRDS) is usually seen in preterm infants that are born before 34 weeks' gestation. They usually present with respiratory distress symptoms such as tachypnea, grunting and cyanosis immediately after birth. A chest radiography would show a diffuse ground-glass appearance with air bronchograms and hypoexpansion. [6] Usually, with treatment, infants with NDRS can recover wihout much long-term effects. In certain cases, bronchopulmonary dysplasia can occur and this will be talked about more in the next section.
Hyaline Membrane Disease
NRDS is often also called Hyaline Membrane Disease (HMD), as NRDS is usually due to a deficiency of pulmonary surfactant [7] and the terminal bronchioles and alveolar ducts are seen to be lined with hyaline membranes. If surfactant is absent in infants, the alveoli would be more likely to collapse and this would explain most of the clinical features of NRDS. [8]
Prematurity is the most significant cause of the deficiency in surfactant. At around 23 weeks of gestation, surfactant is first seen in small amounts, and only at 30 weeks can surfactant in the lungs be easily detectable. Usually before 34 weeks' gestation, there is insufficient surfactant for the lungs to work properly. [8] Also, the mechanism to replace surfactant might be too immature in preterm babies so when surfactant is lost during breathing, there is a lack of production to replace it.[8] Another important cause is destruction of surfactant in the lungs by asphyxia before, during or after birth. This results in either the destruction of surfactant-producing alveolar cells or allow for the secretion of fibrinogen, which is known to inactivate surfactant. [8]
Bronchopulmonary dysplasia
(BPD) was initially described almost 50 years ago as the chronic lung disease that developed when positive-pressure ventilation and oxygen therapy were used to treat “hyaline-membrane disease” or neonatal respiratory distress syndrome in preterm infants (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4469359/)
Meconium Aspiration Syndrome
Meconium-stained amniotic fluid is present in approximately 10% to 15% of deliveries, although the incidence of meconium aspiration syndrome is only 1%. Because meconium excretion often represents fetal maturity, meconium aspiration syndrome occurs in term and post-term newborns. Meconium is a conglomeration of desquamated cells, bile pigments, pancreatic enzymes, and amniotic fluid. Although sterile, it can lead to bacterial infection, irritation, obstruction, and pneumonia.
Meconium aspiration syndrome presents at birth as marked tachypnea, grunting, retractions, and cyanosis. Examination may reveal a barrel-shaped chest, with rales and rhonchi heard on auscultation. Chest radiography may show bilateral fluffy densities with hyperinflation. Treatment includes N-CPAP and supplemental oxygen. Ventilator support may be needed in more severe cases.
Perineal neonatal suctioning for meconium does not prevent aspiration. If the infant is hypotonic at birth, intubation and meconium suctioning are advised. Vigorous infants receive expectant management. (http://www.aafp.org/afp/2015/1201/p994.html)
CPAM (Congenital Pulmonary Airway Malformation)
A congenital pulmonary airway malformation is a rare disorder of the pulmonary airway and a hamartomatous mass of disorganized lung tissues with various degrees of cystic change (https://www.ncbi.nlm.nih.gov/pubmed/24715554)
CPAM is characterized by the lack of normal alveoli, an excessive proliferation and cystic dilatation of terminal respiratory bronchioles with various types of epithelial lining. Microscopically the cyst linings are composed of ciliated, cuboidal or columnar cells and those cysts have lack of normal architecture and are frequently devoid of cartilage. Type 2 CPAM that is associated with other congenital anomalies is seen more frequently than other types. (http://www.turkjpath.org/text.php3?doi=10.5146/tjpath.2013.01208)
Cystic Fibrosis
Lung Cardiovasculature
Future questions
Glossary
References
[9] [10] [11] [12] [13] [14] [15]
- ↑ Schoenwolf, G.C., Bleyl, S.B., Brauer, P.R., Francis-West, P.H. & Philippa H. (2015). Larsen's human embryology (5th ed.). New York; Edinburgh: Churchill Livingstone.
- ↑ Gilbert SF. Developmental Biology. 6th edition. Sunderland (MA): Sinauer Associates; 2000. Comparative Embryology. Available from: https://www.ncbi.nlm.nih.gov/books/NBK9974/
- ↑ DiFiore, J., & Wilson, J. (1994). Lung Development. Seminars in pediatric surgery, 3(4), 221.
- ↑ Spooner, B. S., & Wessells, N. K. (1970). Mammalian lung development: Interactions in primordium formation and bronchial morphogenesis. Journal of Experimental Zoology, 175(4), 445-454. doi:10.1002/jez.1401750404
- ↑ Masters, J. R. W. (1976). Epithelial-mesenchymal interaction during lung development: The effect of mesenchymal mass. Developmental Biology, 51(1), 10. doi:https://doi.org/10.1016/0012-1606(76)90125-1
- ↑ <pubmed>26760414</pubmed>
- ↑ <pubmed>4984152</pubmed>
- ↑ 8.0 8.1 8.2 8.3 <pubmed>PMC1840752</pubmed>
- ↑ <pubmed>24499815</pubmed>
- ↑ <pubmed>PMC3787747</pubmed>
- ↑ <pubmed>25114215</pubmed>
- ↑ <pubmed>18374910</pubmed>
- ↑ <pubmed>11171334</pubmed>
- ↑ <pubmed>PMC3839746</pubmed>
- ↑ <pubmed>28759122</pubmed>