2017 Group Project 4: Difference between revisions
No edit summary |
|||
| Line 222: | Line 222: | ||
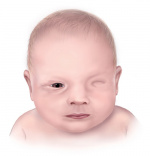
[[File:Anophthalmia.jpeg|150px|thumb|left|'''Figure 2.''' Anopthalmia birth defect]] | [[File:Anophthalmia.jpeg|150px|thumb|left|'''Figure 2.''' Anopthalmia birth defect]] | ||
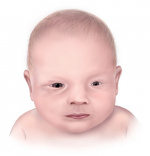
[[File:Microphthalmia-500px.jpg|150px|thumb|centre|'''Figure 3.''' Microphthalmia birth defect]] | [[File:Microphthalmia-500px.jpg|150px|thumb|centre|'''Figure 3.''' Microphthalmia birth defect]] | ||
[[File:Opac_figure_7.jpg|150px|thumb|right|'''Figure 4.''' Coloboma birth defect]] | |||
==Glossary== | ==Glossary== | ||
Revision as of 14:24, 5 October 2017
| 2017 Student Projects | |||
|---|---|---|---|
|
Eye Development
Mark Hill (talk) 16:09, 14 September 2017 (AEST) OK Feedback
- Timelines
- Embryonic contributions from germ layers and neural crest
- Cellular components
- Current research areas
- Get rid of the bold formatting for sub-headings.
- Animal models compared to human development
- Central neural pathway
Anatomy of the Adult Eye
The eye is a complex sensory structure which allows a variety of species to intake and process visual information from the world around us.
To discuss the key anatomical components of the eye, we will break down the eye in parts[1]:
Supporting Structures (Orbit, Extraoccular Muscles, Lacrimal Gland, Eyelid)
The orbit of the eye consists of a framework of bones and connective tissue which provide structural support and protection to the sensitive human eye. 7 bones contribute to the orbit of the eye: frontal, lacrimal, sphenoid, zygomtatic, ethmoid, maxilary, palatine. Several openings exist in the orbital structure, 2 key fissures are the superior orbital fissure and inferior orbital fissure and the posterior optic canal. These openings allow crainial nerves passageway.
A set of 6 extraoccular muscles allow for a strong voluntary control of the movement of the eye. These muscles include superior recuts, inferior rectus, lateral rectus, medial rectus, inferior oblique, superior oblique muscles. These muscles are some of the smallest in the human body and are designed to produce fast, controlled motion to focus on an object of interest.
The eyelid is the anterior covering of the eye, consisting of a thin fold of skin. It is controlled by the levitator palpabrae superioris muscle. Superio-laterally to the eyelid is the lacrimal gland, which serves to create a film of tear, an important component to keeping the anterior surface of the eye moist. The eyelid assists in this process by opening and closing, or blinking, which spreads the tear film across the surface of the eye. Tear film and debris caught in the tear film are excreted through the lacrimal duct which is located on the infero-medial surface of the eyelid.
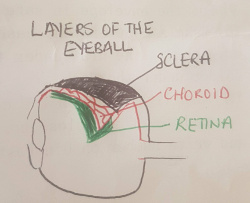
Layers of the Eyeball (Sclera, Choroid, Retina)
The superficial layers of the eyeball is the sclera, a thick fibrous layer which becomes thicker as it extends posteriorly. The sclera is the visible as the white part of our eye. It's function is to provide structural stability to the eye and serves as attachment for some extraoccular insertions. Deep to the sclera is the choroid, a vascular network which provides nourishment to the layers of the eyeball and plays a large role in the growth of the eye. Deep to the choroid is the retina, a network of nerve fibers which transmit visual information. The retina contains 2 types of photoreceptors which convert visible light into nerve impulses. Rods work best in low light environments while cones work best in high light enthronements and detect colour and sharp detail.[2]: The retina does not extend to the anterior part of the eyeball, unlike the sclera and choroid layers.
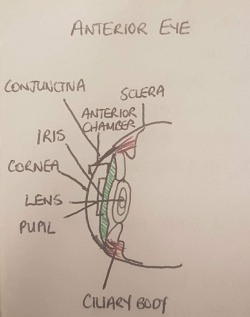
Anterior structure (Lens, Cornea, Pupil, Iris, Ciliary Body, Conjunctiva Anterior Chamber)
The most anterior component of the eyeball is the cornea, which is a multilayered avascular transparent structure who's major function to the refract light to assist image formation (contributes about 75% of total refraction). Continuous with cornea superiorly and inferiorly is the conjunctiva. Deep to the cornera is the iris, or the coloured ring visible in the eye. The iris consists of 2 muscles which act to enhance and diminish the size of the pupil, a hole in the middle of the iris allowing light to enter the eye. Deep to the pupil and iris is the lens, which is a transparent structure which contributes the other 25% of the eye's refractive power. The lens changes shape through accomodation controlled by the ciliary body muscles. The ciliary body is the anterior extension of the choroid. The function of the lens is to focus images by changing refractive power based on the position and depth of focal objects. In between the anterior surface of the lens and posterior surface of the cornea is the anterior chamber. This chamber is filled with aqueous humor supplied by the ciliary body, who's function is to provide nutrients to ocular structures and maintain intraocular pressure.
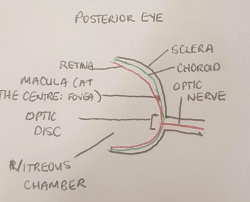
Posterior structure (Optic Nerve, Optic Disc, Macula, Fovea, Posterior Chamber)
In the posterior section of the retina is the macula, a central spot in which a high concentration of cone photoreceptors are found. The direct centre of the macula is called the fovea which contains solely cone photoreceptors. The fovea is only part of the eye which can conduct 'perfect' 20/20 vision. It has a high workload and hence a strong vascular supporting structure[3]:. The most posterior part of the eye is the optic nerve (along with the central retinal artery and central retinal vein), which is responsible for transporting nerve impulses to the cerebral cortex for processing. The opening of the optic nerve is called the optic disc, which contains no photoreceptors and is a blind spot of the eye. Between the posterior surface of the lens, the retina and the optic disc is the posterior chamber. The posterior chamber contains a vitreous humour, a jelly like substance with a high viscosity.
Overview of eye development
Timeline of embryonic development
| WEEK | DEVELOPMENT |
|---|---|
| 3-4 | Eye fields, Optic vesicles |
| 5-6 | Optic Cup, Lens Vesicle, Choroid Fissure, Hyaloid Artery |
| 7-8 | Cornea, Anterior Chamber, Pupillary Membrane, Lens, Retina |
| 8-10 | Eyelids |
| 9-15 | Iris, Ciliary Body |
Carnegie Stages
Carnegie Stages is a system of 23 stages used to describe developmental events of the vertebrate embryo. At stage 10 we see early signs related to eye development [4].
| STAGE | EVENTS |
|---|---|
| Stage 10 (22 days) | The optic primordium has developed. Two small grooves develop on each side of the developing forebrain in the neural folds - this is the optic grooves. The optic placode has begun to develop, which is seen by a small thickening of the surface ectoderm lateral to the hindbrain. |
| Stage 11 (24 days) | Optic vesicle begins to form from the optic groove. Otic pit has formed. |
| Stage 12 (26 days) | The optic vesicles have extended from the forbrain to the surface ectoderm. The optic vesicle now lies close to the surface ectoderm. |
| Stage 13 (28 days) | The optic vesicle interacts with the surface ectoderm and will induce this ectoderm to form the lens placode, which is the precursor of the lens. |
| Stage 14 (32 days) | The lens placode is indented by the lens pit and may be cup-shaped. |
| Stage 15 (33 days) | The lens pit will close and form a circle that separates from the surface ectoderm and becomes the lens vesicle. The lens vesicle and optic cub lie close to the surface ectoderm, which creates a slight elevation in the region of the eye. |
| Stage 16 (37 days ) | First indication of the development of the eyelids. |
| Stage 17 (41 days) | Retinal pigment is visible. The eyes are still laterally places, but starts to take a more anterior position. The lower eyelid fold has begun to form. |
| Stage 18 (44 days) | Mesenchyme invades the region between the lens epithelium and the surface ectoderm. The eyes has shifted to more anterior position. The groove above and below the eyes are deeper, but have not joined yet. Eyelid folds develop. |
| Stage 19 (48 days) | The upper and the lower eyelids now meet at the outer canthus. |
| Stage 20 (51 days) | The lens cavity is lost. The upper and lower lids meet laterally and medially. The eyelids now partly cover the eye. |
| Stage 21 (52 days) | |
| Stage 22 (54 days) | |
| Stage 23 (57 days) | The face is beginning to look human. |
Embryonic Contributions
The eyes are derived from four sources:
| Embryonic contributions | Eye component |
|---|---|
| Neuroectoderm of the forebrain | Retina, Posterior layers of the iris, The optic nerve |
| Surface ectoderm of the head | The lens of the eye, The corneal epithelium |
| Mesoderm between the neuroectoderm and the surface ectoderm | The fibrous and vascular coats of the eye |
| Neural crest cells | Choroid, Sclera, Corneal endothelium |
Short overview
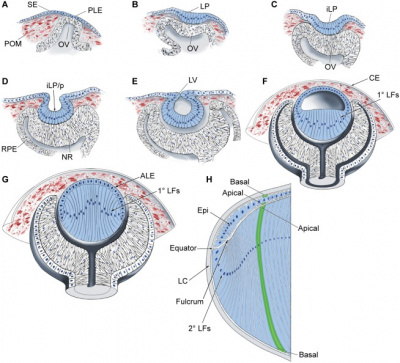
The eye starts to develop at 22 days. The optic grooves (sulci) appears in the neural folds at the cranial end of the embryo. When the neural fold fuse to form the forebrain, the optic grooves will form optic vesicles. The optic vesicles are continuous cavities from the cavity of the forebrain and project from the wall of the forebrain and into the mesenchyme. The optic vesicle extends from the diencephalon and will come in contact with the surface ectoderm of the head. This induces the formation of a lens placode. The surface ectoderm near the optic vesicles will thicken and form the lens placodes. The lens placodes will sink into the surface ectoderm and form lens pits. The edges of the lens pits will travel towards each other and fuse to form round lens vesicles, which will later lose connection with the surface ectoderm. The optic vesicles do also keep developing - they will form double-walled optic cups which are connected to the brain by the optic stalk. The two layers of the optic cup will differentiate in different directions. The cells of the outer layer will produce melanin pigment and later become the pigmented retina. The cells of the inner layer of the optic cup will proliferate fast and develop glia, ganglion cells, interneurons and light-sensitive photoreceptor neurons. These cells are in the neural retina. The ganglion cells of the retina are neurons that send signal to the brain. The axons of the ganglion cells of the neural retina will grow in the wall of the optic stalk. The cavity in the optic nerve will start disappearing, and instead, the axons of the ganglion cells will form the optic nerve.
The optic stalk is now the optic nerve [5]
The optic cups will fold inwards around the lens while the lens vesicles have grown inwards so they have fully lost their connection with the surface ectoderm, which locates them in the cavities of the optic cups. The retinal fissures (linear grooves) will develop and cover the ventral surface of the optic cups and down to the optic stalk. The retinal fissures contain vascular mesenchyme and hyaloid blood vessels will develop here. The hyaloid artery supplies the structures in the eye with blood and the hyaloid vein will return the blood from these structures.
Formation of the optic vesicle
It is a specific area of the neural ectoderm that will become the optic vesicle - this happens because of a group of transcription factors - Six3, Pax6, and Rx1. These transcription factors are expressed in the most anterior tip of the neural plate. This area will split into bilateral regions and form the optic vesicles. The Pax6 protein has shown to be especially important for the development of the lens and retina. This protein is important for photoreceptive cells in all phyla. Pax 6 is also present in the murine forebrain, hindbrain, and nasal placodes, but the eyes are most sensitive its absence [5].
The sonic hedgehog gene is important for the separation of the single eye field into two fields. If this gene is inhibited, the eye field will not split which will result in cyclopia, a single eye in the center of the face [5].
Development of the eye components
Lens
Human lens induction occurs at around 28 days and is completed around day 56. The surface ectoderm will thicken near the optic vesicle and create the lens placode and later form the lens vesicle [6]. Lens cells come from ectoderm and differentiate into either lens fibers or the lens epithelium. The anterior monolayer of epithelial cells of the lens will create the lens epithelium, which makes the sheet of cuboidal epithelium covering the anterior surface of the lens. The posterior lens vesicle cells will produce the linear primary fibre cells aligned parallel to the optic axis. These fibres will create the lens mass and form the embryonic lens nucleus. The lens epithelial cells will keep proliferating and produce new cells which generate a secondary lens fiber cells. This rows of cell will form the outer shells and keep the lens growing throughout life. This makes the eye lens unique - it will have an addition of new cells inside the surrounding capsule all the time [7].
Retina
5075778
Ciliary Body
The ciliary body is a muscular and secretory tissue and is located directly behind the lens. The ciliary body forms part of the anterior segment of the eye and is an important regulator of eye physiology and the vision. The ciliary body produces the aqueous fluid which fills the eyes and nourishes the lens and cornea - this aqueous fluid function to keep the eye in a pressurized and inflated state, which is important the vision.The ciliary body also synthesizes collagenIX and tenasin-C [8].
The ciliary body extends from the iris root (anteriorly) to the ora serrata (posteriorly). It consist of ciliary muscles and ciliary processes. Each ciliary process (fold) is covered by a double-layered secretory epithelium; the outer pigmented and the inner unpigmented (closes to the lens). The epithelial layers of the ciliary body comes from the retina of the optic cup. We see two different ciliary body epithelium: the inner non-pigmented ciliary epithelium which is connected with the neural retina and the outer pigmented ciliary epithelium which is connected with the retinal pigmented epithelium. The epithelium of the iris is the further anterior extension. The epithelial layers are associated with a stroma containing the ciliary muscle. The ciliary muscle is complex, but can be divided into three portions; anterior, posterior and internal [9].
In the chick eye development, we see the mesenchyme grow together on the margin of the optic cup and will form the stroma of the ciliary body and the iris, which is located more anteriorly. It is unknown how if the lens has a role in inducing the secretory ciliary body epithelium and the muscular iris epithelium [10].
Iris
The Iris develops at the end of the third month of development. The iris is a thin layer and derives from the anterior rim of the optic cup. In the anterior of the eye, the optic epithelium is nonneural and matures as ciliary body and iris epithelia.
Cornea
http://www.sciencedirect.com/science/article/pii/S1877117315000642
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1298807/pdf/taos00013-0203.pdf
Aqueous Chambers
5075309
Choroid and Sclera
5075309
Eyelids
5075309
Lacrimal Glands
5075309
Extraocular muscles
5075778
<pubmed>26410132</pubmed> <pubmed>23071378</pubmed>
We could talk briefly in this sections about the causes of short/long-sightedness and common causes of blindness at a developmental level - z3416557
Congenital Anomalies
We could talk briefly in this sections about the causes of short/long-sightedness and common causes of blindness at a developmental level - z3416557
Although quite rare, abnormalities can occur during the embryonic development that causes serious effects to the features of the eyes, its function as well as the further normal development after birth. These anomalies can occur unilaterally or bilaterally and it is also common for most reported cases to have more than one type of eye abnormalities at a time. Thus, the estimated prevalence statistics listed in the table can overlap.
| Congenital Anomalies | Description | Epidemiology |
|---|---|---|
| Anopthalmia | The absence of the eyes. | Prevalence: Anophthalmia-Microphthalmia Syndrome was estimated to be 5.3 per 100 000 cases [12] |
| Microphtalmia | Abnormal reduction in size of the eyeballs. | |
| Coloboma | A condition where parts of the eye is missing and failed to develop normally. | Prevalence: Occular coloboma was estimated to be 8.0 per 100 000 cases [12] |
| Aniridia | Complete or partial absence of the iris. | Prevalence: Estimated to be 1.5 per 100 000 cases [12] |
| Optic Nerve Hypoplasia | A condition where the optic nerves are underdeveloped. | Prevalence: Reported to be the most common abnormality [13]
|
Glossary
References
- ↑ Chen, J., 2011. Handbook of Visual Display Technology. Springer Berlin Heidelberg. Chapter 2.1
- ↑ Curcio CA, Hendrickson AE. Organization and development of the primate photoreceptor mosaic. Prog Ret Ret. 1991;10:89–120.
- ↑ <pubmed>6462623</pubmed>
- ↑ <pubmed>7364662</pubmed>
- ↑ 5.0 5.1 5.2 Gilbert SF. Developmental Biology. 6th edition. Sunderland (MA): Sinauer Associates; 2000. Available from: https://www.ncbi.nlm.nih.gov/books/NBK9983/
- ↑ <pubmed>20171212 </pubmed>
- ↑ <pubmed>25406393</pubmed>
- ↑ <pubmed>17275804</pubmed>
- ↑ <pubmed>12127103</pubmed>
- ↑ <pubmed>17275804</pubmed>
- ↑ <pubmed>23528534</pubmed>
- ↑ 12.0 12.1 12.2 Orphanet Report Series – Rare Diseases Collection. (2017). Prevalence of rare diseases: Bibliographic data (no. 2). Paris. France: Author. Retrieved from: http://www.orpha.net
- ↑ Ryabets-Lienhard, A., Stewart, C., Borchert, M., & Geffner, M. E. (2016). The Optic Nerve Hypoplasia Spectrum - Review of the Literature and Clinical Guidelines. Advances in Pediatrics, 63, 127-146. doi: 10.1016/j.yapd.2016.04.009
External links
z5075309 - <pubmed>26956898</pubmed>