2017 Group Project 3
| 2017 Student Projects | |||
|---|---|---|---|
|
Heart
Help:Copyright Tutorial Help:Editing Basics
Mark Hill (talk) 16:06, 14 September 2017 (AEST) OK Feedback
- This is very early stage of content development. Of all the possible topics this is definitely the MOST researched topic to date. You have this week to make significant progress on this page.
- Where is the timeline of development.
- Where is the timeline of key discoveries
- Splanchnic mesoderm and neural crest contribution
- Differentiation of different cardiac cell types
- Cardiac conduction system development
- Cardiomyocyte differentiation/function
- Cardiac stem cells
Introduction
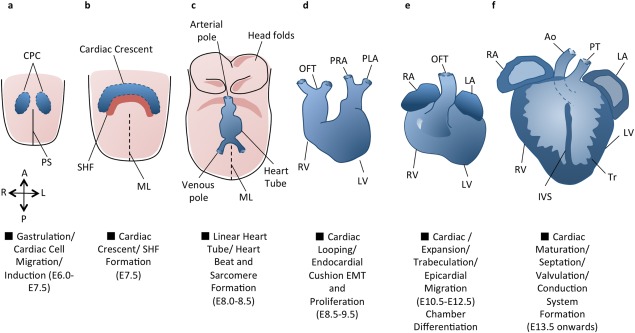
The cardiovascular system is the first system to develop and function in the human embryo. Rapid cardiac development is essential as the growing embryo can no longer receive oxygen and essential nutrients via diffusion alone, hence a circulatory system and a contractile heart mechanism is required to supply the embryo. We recognise the hearts normal development is vital for foetal life, and hence we have chosen to document the development of the heart from gastrulation to birth. Any defects occurring during the developmental processes can lead to congenital heart abnormalities. However, early cardiac development is a multifaceted procedure and is associated with other developmental processes such as: embryonic folding, coelom formation, and vascular development [1].
Through researching the advances in technology, coupled with the biological use of suitable animal models [2] our understanding of embryological cardiac development has evolved, and we are piecing together the mechanism underlying this development. This page will outline the importance of how heart abnormalities arise, the treatments available and the possible treatments to be developed in the future. Due to the major knowledge gaps in current embryological heart research, we acknowledge that this will impact our assignment, and aim to address further research concepts that will improve our understanding.
Developmental Origin
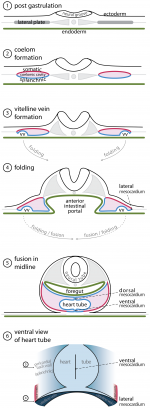
In the developing embryo the lateral plate mesoderm splits into somatic and splanchnic layers, the latter is comprised of cardiac progenitor cells [3]. The somatic mesoderm lines the ectoderm, the splanchnic mesoderm lines the endoderm, and in between lies an embryonic coelom [4] . At the end of week three, the heart develops from splanchnic mesoderm of the cardiogenic region of the embryonic plate. At the cranial end of the embryo, anterior to the developing neural tube is the initial origin of heart formation.
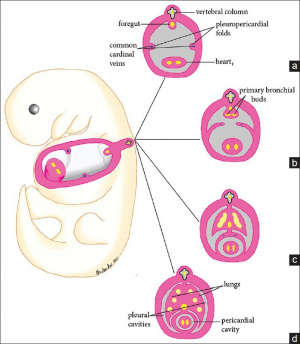
Originally, as seen in figure 2 the cardiogenic region forms laterally of the paraxial mesoderm and primitive streak of the embryonic disc. Due to the natural mesenchymal cell organisation of the mesoderm, cells ‘migrate’ and fuse at the midline of the cranial end of the embryo forming the cardiac crescent just prior cardiac tube formation and folding. As in figure 2, endoderm surrounding the primitive gut contracts, and brings the cardiogenic precursor regions of the splanchnic region towards the midline. At this time, early heart formation occurs in the form of angioblastic cords of the splanchnic mesoderm. The angioblastic cords develop into separate endochondral heart tubes moving closer together as the foregut pinches together and the yolk sac contracts into the embryo. Fusion of the two heart tubes is facilitated by apoptosis [5] . The origin of the primitive heart is in the early pericardial coelom, which is later developed into the pericardial cavity, through fusion of the pleuropericardial folds to separate the pleural cavities at the later development of the lungs (see figure 4) [6].
Z5076019 (talk) 14:19, 26 August 2017
Developmental Timeline
Historic Developmental Timeline
z5178463
Embryonic Developmental Timeline
| WEEK | DEVELOPMENT |
|---|---|
| 2 | Bilateral cardiogenic areas form |
| 3 | Mesoderm splits, Heart tubes are brought to the midline, Heart tube fusion, Heart beat |
| 4 | Heart looping, Neural crest migration commences, Dorsal and ventral endocardial cushions fuse |
| 5 | Foramen primum closed, Septum secundum srtats developing, Muscular interventricular septum develops, Bulbar ridges and trabeculation become evident |
| 6 | Aortic and pulmonary trunks cleave |
| 7 | Valves develop |
Primary Heart Field and Heart Tube Formation
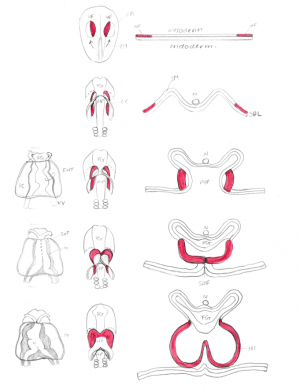
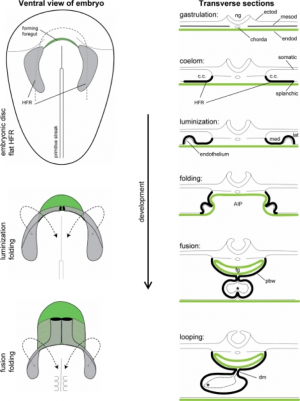
At around day 15 of human development, the first cells start to migrate through the primitive streak to the anterior and lateral sections of the cranial end of the embryonic disc, forming bilateral primary heart fields. These primary heart fields resemble a crescent shape, as seen from Figure ().
At around day 18, the lateral plate mesoderm is split into two layers, namely the splanchnic mesoderm, facing the endoderm and the somatic mesoderm, facing the ectoderm. The former portion of the mesoderm gives rise to the heart. The portion between the splanchnic and somatic mesoderm is the presumptive pericardial space. Cells from the splanchnic mesoderm will merge to form 2 lateral endocardial tubes (also known as angioblastic cords) and as they form a lumen, are enveloped by myocardium. These endocardial tubes are as of now located inferior to the presumptive pericardial space.
At around 19-21 days, the embryonic disc starts to fold. This folding begins cranially and extends in a caudal direction. The endocardial tubes fuse and is now located between the pericardial space and newly formed foregut that becomes surrounded by pericardial space (also known as the pericardial coelom). At this stage, the myocardium does not completely engulf the endocardial tubes. Instead, it remains in a continuous attachment with the non-cardiac splanchnic mesoderm through a structure called the dorsal mesocardium.
At this point, the primitive heart tube is bilaterally symmetrical and resembles an inverted Y shape. Starting from the inflow tract, there is the right and left sinus venouses that receives blood from the embryo, followed by the primitive atrium, primitive ventricle, bulbus cordis and then the truncus asteriosus which gives rise to the aortic and pulmonary trunk.
<pubmed> PMC1767747</pubmed> Z5178463
Secondary Heart Field and Cardiac Looping
The search for the heart fields dates to mapping studies carried out on embryos in the 1940’s was the beginning of identifying lateral plate mesoderm that gives rise to cardiogenic cells and has the potential to for myocardium [9] [1]. The heart field regions lie laterally to the primitive streak, with the subpharyngeal mesodermal progenitor cells of the secondary heart field (SHF) located medially and ventrally to the primary heart field (PHF) cells that give rise to the primary linear heart tube. The PHF and the SHF are adjacent within the heart field region of the lateral plate mesoderm and cardiac crescent (refer to student figure 2). It is understood that in the pharyngeal mesoderm the cardiac regions are “prepatterned” in the progenitor cell population [10], hence being termed “specified but undifferentiated”. It is the patterning of cells within the soon to become myocardium, that is responsible differentiation into chamber-specific myocytes (atrial and ventricular) and conduction cells [11].
As the SHF remains as specified but undifferentiated cardiogenic mesoderm, the first heart field forms the initial heart tube, differentiating into contractile myocardium. Most of the other cells from the secondary heart field are then added to the elongating tube. It is essential that the SHF cells remain undifferentiated and do not add prematurely to the heart tube [12] [2]. In the early embryo, the same progenitor cells that constitute the SHF are responsible for rapid growth occurs during cardiac looping morphogenesis [13]. Looping is essential for cardiac development as it assist further growth of the originally straight heart tube, and ensures it fits within the pericardial celom. Additionally, looping of the heart tube is known to be the first visual evidence of embryonic asymmetry. After formation of the primary heart tube, cells from the SHF migrate to the cranial caudal ends of the tube to continue elongation [14] [3].
The SHF gives rise to endocardial, myocardial and smooth muscle cells through expression of transcription factor islet -1 [15]. It also contributes to the right ventricle, inflow regions and outflow tract (OFT) [16]. The OFT is the point of exit from the heart via structures of early cardiac development that give rise the essential structures of the aorta and pulmonary artery [17] this will be discussed later in further detail. The SHF unambiguously involves the splanchnic mesoderm that gives rise to the most distal OFT myocardium of the ventricular outflow and the proximal smooth muscle of the great arteries and semilunar valves that meet at the arterial pole of the heart [18] [4]. The SHF of the forming heart and its contribution the arterial pole involves complex and interconnected signalling pathways that will be covered later in further detail.
Cardiac Looping Steps
- Straight heart tube continues to elongate
- Rapid growth of the bulbus cordis and the primitive ventricle causes ventral bending and right rotation = C shaped loop (convex side on the right)
- The ventricular bend continues to move caudally, the inflow and outflow tracts are brought together at the atrial pole of the heart = S shape
- The truncus arteriosus if formed by adding myocardial cells at the top end of the heart. This portion will form roots and the proximal portion of the aorta and the pulmonary artery.
[19] <pubmed> PMID16479500 </pubmed>
[20] <pubmed>PMC2794420</pubmed>
[23] <pubmed> PMC2794420 </pubmed>
[25] <pubmed> PMC1767747 </pubmed>
[29] <pubmed> PMC2794420 </pubmed>
Cardiac Septation
This stage of heart morphogenesis refers to the development of the four main cardiac chambers from the primitive atrium and ventricle. Cardiac septation is comprised of three main events:
- Division of the atrioventricular canal
- Atrial septation
- Ventricular septation
Division of the atrioventricular canal
Division of the atrioventricular canal (AVC) begins with the formation of the superior and inferior endocardial cushions, which are located on the dorsal and ventral aspects of the AVC respectively.[5] These cushions develop as mesenchymal cells invade and proliferate within swollen regions of cardiac jelly of the AVC; this mesenchyme is derived from endothelial cells that have transdifferentiated in the process of epithelial-mesenchymal transformation (EMT) [1,2]. Throughout the fifth week of development, the endocardial cushions project inwards and eventually fuse to partition the AVC into the left and right atrioventricular canals [1,2]. These canals will serve as the orifices in which the tricuspid and mitral valves are situated [1,2].
Atrial septation
As the AVC is undergoing division, a muscular outgrowth, referred to as the septum primum, extends inferiorly from the roof of the primordial atrium [3]. This septum partially divides the atrial chamber into left and right halves, leaving a temporary communication located between the inferior border of septum primum and the endocardial cushions known as the foramen primum [1]. As the size of the foramen primum diminishes, perforations in the superior portion of the septum primum develop as a result of apoptosis, forming a second communication between the atrial chambers called the foramen secundum [2]. Concurrently, an additional muscular septum, known as the septum secundum, projects inferiorly to the right of the septum primum [1]. Eventually, the septum secundum will extend beyond the length of the foramen secundum, generating a partial division of the atria that forms the upper boundary of the foramen ovale [3]. The development of the foramen ovale is critical as it allows oxygen-rich blood from the placenta to bypass pulmonary circulation of the embryo and directly enter systemic circulation [4]. Following birth, the foramen ovale is obliterated as the septum primum and septum secundum fuse, resulting in complete formation of the interatrial septum [1].
Ventricular septation
As with atrial septation, differentiation of the ventricles is initiated within week 4 of development [1]. A muscular ridge, referred to as the interventricular septum primordium, develops and extends superiorly from the caudal aspect of the primitive ventricular chamber [2]. Growth of the septum is attributed to the expansion of the ventricles, which involves the development of muscular trabeculae as cardiomyocytes proliferate within the chamber walls [3]. The end result is a partial division between the left and right ventricles, which forms the muscular portion of the interventricular septum [2]. A communication between the ventricles, known as the interventricular foramen, remains until approximately week 7 of development [5]. The foramen is obliterated by the fusion of the septum intermedium and the bulbar ridges of the bulbus cordis; this constitutes the membranous portion of the interventricular septum [1].
[1] Partitioning the heart: mechanisms of cardiac septation and valve development https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3424040/
[2] Development of the heart: (2) Septation of the atriums and ventricles https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1767797/
[3] An overview of cardiac morphogenesis http://www.sciencedirect.com/science/article/pii/S1875213613002817
[4] Patent foramen ovale. https://www.ncbi.nlm.nih.gov/pubmed/27188965
[5] Review of medical embryology: Ben Pansky https://discovery.lifemapsc.com/library/review-of-medical-embryology/chapter-120-septation-of-ventricles-truncus-arteriosus-and-conus-cordis
z5059996
Cardiac Neural Crest and Outflow tract
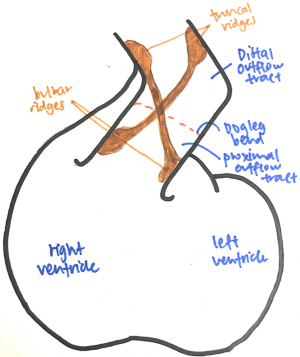
The outflow tract is a tube that runs from the right ventricle to the aortic sac and presents with a distinctive dog-leg bend that separates the proximal (bulbus cordis) and distal (truncus arteriosus) ends of the tract. The endocardial jelly that lines the lumen of the outflow tract concentrates to form the endocardial cushion facing each other that spirals in a 180-degree twist through the length of the outflow tract. Like the outflow tract, these endocardial cushions can be divided into distal and proximal moieties. The distal endocardial cushions are also known as the truncal ridges and the proximal ones are also known as the bulbar ridges. Cells from the cardiac neural crest migrates out of the neural tube, through the pharyngeal arches and aortic sac and into the outflow tract, where it condenses in the ridges to support the septation of the outflow tract.
The fusion of the endocardial cushions starts from the distal end of the outflow tract and proceeds proximally. Fusion of the truncal endocardial cushions forms the aorticopulmonary septum that separates the truncus into an aortic and pulmonary trunk. The bulbar endocardial cushions fuse as they extend towards the interventricular septum, separating the proximal outflow tract into the prospective aortic and pulmonary trunks. As the outflow tract separates, the aortic trunk leads to the 3rd and 4th pharyngeal arch arteries and the pulmonary trunk leads to the 6th pharyngeal arch artery.
Outflow Tract Anatomy. This image portrays an image of the outflow tract viewed in a distal and proximal manner. The tubular endocardial cushions are located in the distal end and the bulbar endocardial cushions are located in the proximal end. The proximal end of the outflow tract extends from the right ventricle. This image is based upon <pubmed>PMC1767864</pubmed>
<pubmed> PMC1767864</pubmed>
(Z5178463)
Proepicardium and Coronary Heart Development
Coronary vasculature arises when the fourth layer of the primary heart tube is formed. This fourth layer is known as epicardium that surrounds the myocardium which allows the development of vascular structures over the heart surface.
The monolayered embryonic epicardium derives from mesothelial cells of the septum transversium and mainly from clustered of proepicardium cells. The process involves either of these two mechanisms, one is by detaching of these cells and attach to the pericardial cavity and spread over the heart surface or two is by directly attaching the proepicardium to the myocardium forming a permanent tissue bridge. The spreading of the monolayered embryonic epicardium over the bare myocardium initiates the vascularisation of coronary system. A new extracellular matrix (ECM) layer, the subepicardium forms between the epicardium and the myocardium actively promotes the development of coronary blood vessels. The coalescence of three lineages of the coronary vessel cells: smooth muscle, endothelial and connective tissue and fusion of vascular cell progenitors (angioblasts) form a vascular structure de novo via the process of vasculogenesis. They then migrate onto the primary heart tube between day 22 and day 28 of human development. [6],[7]
z5018962
Developmental Signalling Processes
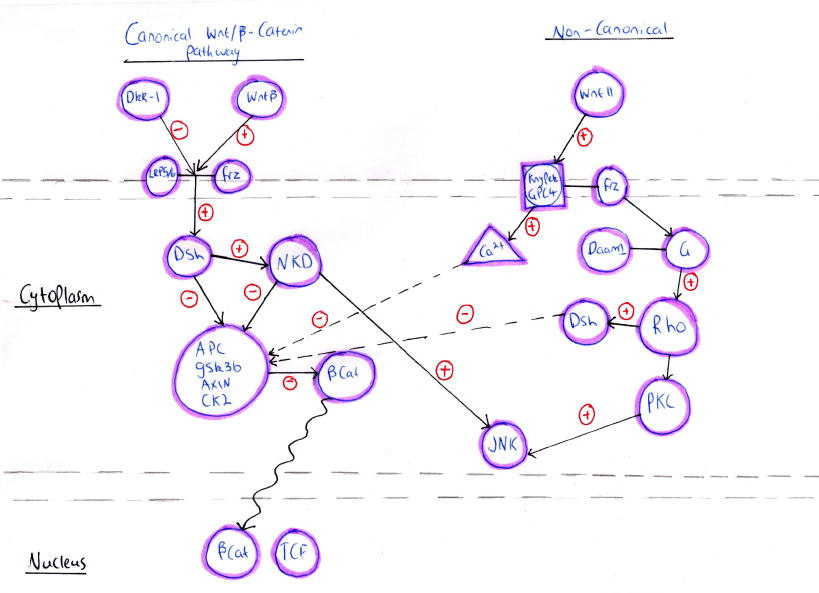
Heart development is a very complicated and dynamic process that requires a high degree of control and regulation. This control is achieved by several temporally regulated signalling cascade (Fig. 1) expressed at different stages of heart development.
Wnt signalling
According to the primary mode of action, Wnt signalling pathways have been divided into two major classes, canonical and non-canonical Wnt signalling pathways. Both the pathways have a role in different stages of cardiac development which could be overlapping or independent of each other. The canonical Wnt signalling pathway involves β-catenin and is activated by a number of ligands such as Wnt-1, Wnt-2, Wnt-3A, Wnt-8A, Wnt-8B, Wnt-8C, Wnt-10A, and Wnt-10B. However, the non-canonical signalling pathway is associated with planar cell polarity and Wnt/Ca2+ pathways that are activated by different ligands such as Wnt4, Wnt5A, Wnt5B, Wnt6, Wnt7A, Wnt7B, and Wnt11 [9].
Canonical/β -catenin signaling is essential for mesoderm formation. Upon binding of the Wnt ligands to the Frizzled receptor, a seven-transmembrane receptor, or the co-receptor LRP-5/6, the Canonical signaling pathway is activated. This leads to cytoplasmic accumulation of β -catenin in one side of the embryo and its translocation to the nucleus where it drives the activation of transcription factors required to determine the site at which mesoderm and endoderm formation will occur in the embryo. Animal studies have shown that the lack of nuclear accumulation of β -catenin results in inability of axis formation and mesoderm development whereas overexpression of β -catenin leads to the formation of secondary axis and ectopic expression of mesoderm signals. Also, homozygous deletion of β -catenin in mouse models results in absence of primitive streak and mesoderm formation [10].
Once mesoderm formation proceeds, the β -catenin signal must be shut down by inhibiting factors otherwise cardiac mesoderm formation will be stopped. This indicates that canonical signaling act as a switch that either induces or suppresses cardiac development. One of the inhibiting factors include dickkopf-1(DKK1) which is an extracellular Wnt inhibitor promotes the expression of cardiac-inducing factor in the endoderm such as Hex. The latter activates paracrine factors to direct adjoining cells towards cardiac fate [11].
Transforming growth factor-β
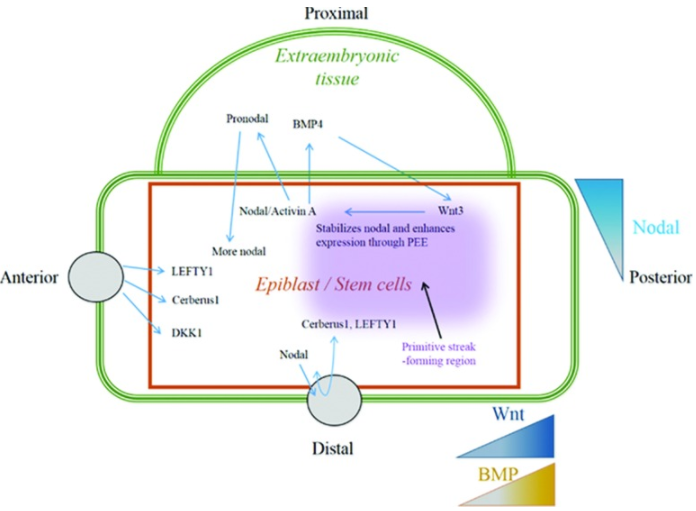
Transforming growth factor-β superfamily involves a large number of growth factors that are structurally related. These growth factors, including Nodal or its mimic Activin, bone morphogenic protein (BMP) and growth and differentiation factors, signal through SMAD-dependent and SMAD-independent pathways <pubmed>18290874</pubmed>. Nodal and its mimic Activin act through SMAD-2 and -3 to activate transcription. During embryo development, epiblast cells produce high levels of Nodal growth factors leading to a gradient of nodal in these cells. This gradient is important for mesoderm patterning (left-right asymmetric heart development) and lineage specification. For this reason, this gradient is maintained by Nodal antagonist secreted from the anterior visceral endoderm or by BMP-4 and Wnt-3 feedback loop in the extraembryonic tissues (Fig.3) <pubmed>25813860</pubmed>. Nodal/Activin’s important role in heart formation is demonstrated by animal models. Presence of Activin in amphibian embryo lead to activation of heart formation whereas the absence of Nodal co-receptor in, called Cripto, in mouse embryo resulted in failure of ES cells differentiation into cardiomyocytes <pubmed>20830688</pubmed>. Also, knocking out copies of SMAD-2 alone or both SMAD-2 ND -3 result in inappropriate specification of axial mesoderm <pubmed>12842913</pubmed>.
FGF signalling
The Notch pathway
Sonic Hedgehog
Retinoic Acid
Z5076466
Current Research And Findings
http://journals.plos.org/plosgenetics/article?id=10.1371/journal.pgen.1006985
Z5018962 (talk)z5018962Z5018962 (talk)
Animal Models
z5076466
Abnormal Development
Ventricular Septal Defect
[34] - ventricular septal defect (Penny and Vick)
Atrial Septal Defect
[35] - atrial septal defects (Giva, Martins & Wald)
Atrioventricular Septal Defect
Misc. References
z5059996
Future Questions
What is the secreted protein that flows across the node, and what is the mechanism that ensures that the loop turns in rightward direction?
Glossary of Terms
References
- ↑ <pubmed> PMC2794420 </pubmed>
- ↑ <pubmed> PMC2794420 </pubmed>
- ↑ <pubmed> PMC1767747 </pubmed>
- ↑ <pubmed> PMC2794420 </pubmed>
- ↑ <pubmed>PMC3424040</pubmed>
- ↑ Pérez-Pomares J, Pires-Gomes A, (2013) The Epicardium and Coronary Artery Formation, Journal of Developmental Biology, Vol.1(3), pp.186-202, ISSN: 2221-3759, E-ISSN: 2221-3759, https://doaj.org/article/b3f5aa0ae8df409ab1664975469b95d1
- ↑ Martinsen B, Lohr J, (2005) Cardiac Development, Handbook of Cardiac Anatomy, Physiology and Devices Iaizzo, P.A. (Ed.), http://www.springer.com/cda/content/document/cda_downloaddocument/9781588294432-c2.pdf?SGWID=0-0-45-387660-p173728389
- ↑ <pubmed>12781678</pubmed>
- ↑ <pubmed>25813860</pubmed>
- ↑ <pubmed>16860783</pubmed>
- ↑ <pubmed>4533091</pubmed>
<pubmed>PMC2691808</pubmed>
<pubmed>PMC4374196</pubmed>
[38] <pubmed>PMC1767747</pubmed>
[39] <pubmed> PMC2691808 </pubmed>