2014 Group Project 5
| 2014 Student Projects | ||||
|---|---|---|---|---|
| 2014 Student Projects: Group 1 | Group 2 | Group 3 | Group 4 | Group 5 | Group 6 | Group 7 | Group 8 | ||||
| The Group assessment for 2014 will be an online project on Fetal Development of a specific System.
This page is an undergraduate science embryology student and may contain inaccuracies in either description or acknowledgements. | ||||
Integumentary
--Mark Hill (talk) 15:16, 26 August 2014 (EST) OK you have some headings, how about some content, references, sources for each section. See Lab 3 Assessment.
--Mark Hill (talk) 11:48, 6 September 2014 (EST) This is a start. Less textbook referencing please, more research/reviews from the published literature. Textbooks should not be used as primary sources, I am happy for them to be listed as related literature.
Introduction
This page concerns the development of the integumentary system in the fetal stage of development, particularly its organs i.e. the skin, glands, hair, teeth, and nails. It explores the mechanism of development as well as the timeline of development. This page also outlines some recent findings on the development of the integumentary system, as well as historic findings. Finally, this page also explores some of the congenital abnormalities of the integumentary system, its mechanism or pathogenesis, clinical manifestations, and how they are treated or managed.
Development Overview
Skin
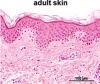
The skin consists of 2 layers: the outer layer (epidermis) and a deeper connective tissue layer (dermis).
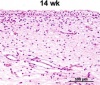
- The epidermis is derived from the ectoderm. Initially it exists as only a single layer of ectodermal cells at 7-8 days of gestation. However, by about 13-14 weeks after gestation, a 3- layered structure of fetal epidermis exists- consisting of the stratum basale, 1 or 2 intermediate layers and the periderm. The peridermal cells eventually become desquamated and form part of the vernix cervix.
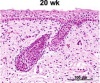
- The 5 definitive layers of the adult skin are evident in the human fetus after 22-24 weeks of gestation. Indirect influences form the dermis help differentiate the epidermis into: stratum basale, stratum spinosium, stratum granulosum, stratum lucidum and stratum corneum.
- The somatic mesoderm is the embryonic origin of the dermis. The mesoderm of the dermatones of the body, also contribute to the development of the dermis. Specifically though, in the head and neck region of the body, the dermis is derived from neural crest cells.
- The dermis is initially composed of just mesenchymal cells- loosely aggregated mesodermal cells. These mesenchymal cells later develop into fibroblasts- which function to secrete collagen and lay-down elastic fibers into the extracellular matrix.
3 other specialised cells of the epidermis also exists- these include melanoblasts, Langherhan cells and Merkel cells.
- Melanoblasts- are derived from neural crest cells that have migrated into the stratum basale. Mid-pregnancy, melanosomes are observed, differentiating the melanoblasts into melanocytes
- Langheran cells- are derived from bone marrow (originally form mesoderm) and migrate into the epidermis. They have the function of antigen presentation.
- Merkel cells- still have an uncertain origin. They have a function related to mechanoreception.
<pubmed>19701759</pubmed> <pubmed>PMC2113922</pubmed>
Glands
- Mammary glands develop from the mammary ridge- a downgrowth of the epidermis (ectoderm) into the underlying dermis (mesoderm). This occurs at about week 6 of development. Prior to puberty, the mammary glands are anatomically indistinguishable.
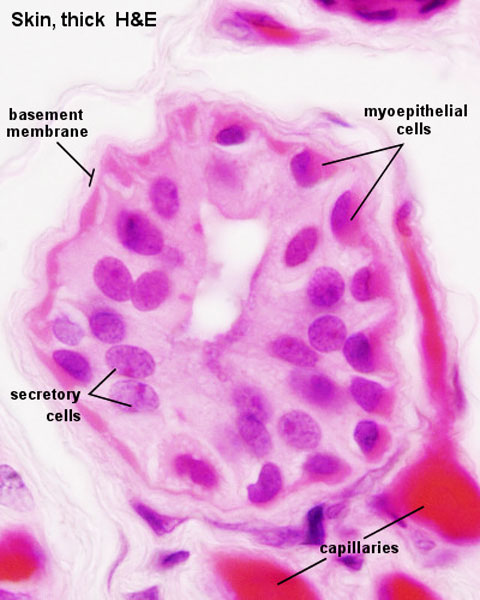
- Eccrine and apocrine sweat glands develop from the downgrowths of the epidermis into the underlying dermis. It has been seen and detected in studies from week 21.
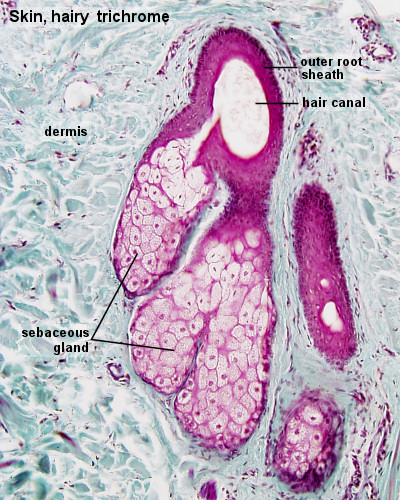
- Sebaceous glands develop from the epithelial wall of the hair follicle
- Cite this page: Hill, M.A. (2014) Embryology Integumentary System - Gland Development. Retrieved October 7, 2014, from https://php.med.unsw.edu.au/embryology/index.php?title=Integumentary_System_-_Gland_Development
- Vernix caseosa
Vernix caseosa is a material produced by sebaceous glands in the foetus in the last trimester of development [1] and is characterised by it’s cheese-like appearance around the neonate at birth. The functions of vernix caseosa include:
- thermal regulation [1]
- barrier to water loss (to keep fetal skin hydrated)[2][1]
- acid mantle development [1]
- prevents the epidermis from water contact while epidermal cornification and formation of the stratum corneum occursCite error: Closing
</ref>missing for<ref>tag
Presently, ACC is managed via conservative treatments or surgical treatments. Conservative treatments refer to basic wound treatments and preventing infection with the use dressings and antibiotics. Surgical treatments, specifically scalp reconstruction procedures, aim to reconstruct the damage to the skin through skin grafts, local scalp flaps, and pericardial scalp flaps. Large defects are often treated using surgical treatments.[3]
Harlequin Ichthyosis
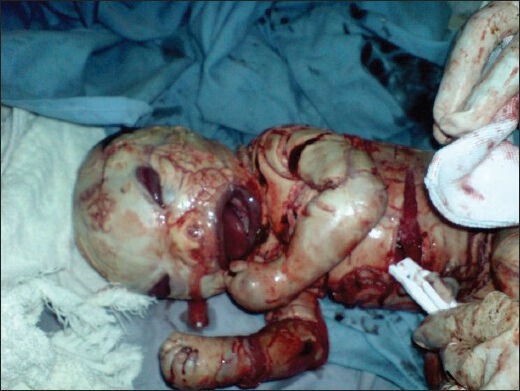
Congenital ichthyosis is an autosomal recessive disease of the skin, characterised by visible and excessive scaling of the skin and hyperkeratosis, i.e. thickening of stratum corneum layer of the epidermis and in some cases, hypohidrosis, i.e. the lack of ability to sweat. [5] Harlequin ichthyosis (HI) occurs only in 1 in 1,000,000 babies. It is life-threatening in the first few weeks and/or months of the neonate.[5] The thick skin can restrict movement of the baby and sometimes constrict extremities and lead to necrosis then autoamputation.[6] Babies with HI are also characterised by bilateral ectropion (everted eyelids), eclabium (everted lips), and underdeveloped nose.[6] In 50% of HI cases, respiratory failure is often the cause of death.[7] This disease is caused by a nonsense mutation in the ATP-binding-cassette A12 (ABCA12) gene, which is responsible for encoding a lipid transporter essential for the regulation of lamellar bodies. [5][6][7]
There is currently no known cure for this disease. Management techniques include:
- Monitoring in neonatal intensive care units.
- -Temperature within the incubator is controlled to avoid fluctuation in body temperature and to stop sweating. [5]
- Mechanical removal of excess scales from the skin [5]
- Bathing to remove excess scales from the skin[5]
- Topical therapy - to reduce hyperkeratosis. [5][7]
- Use of oral retinoids - known to have high rates of survival.[7]
Hypohidrotic Ectodermal Dysplasia
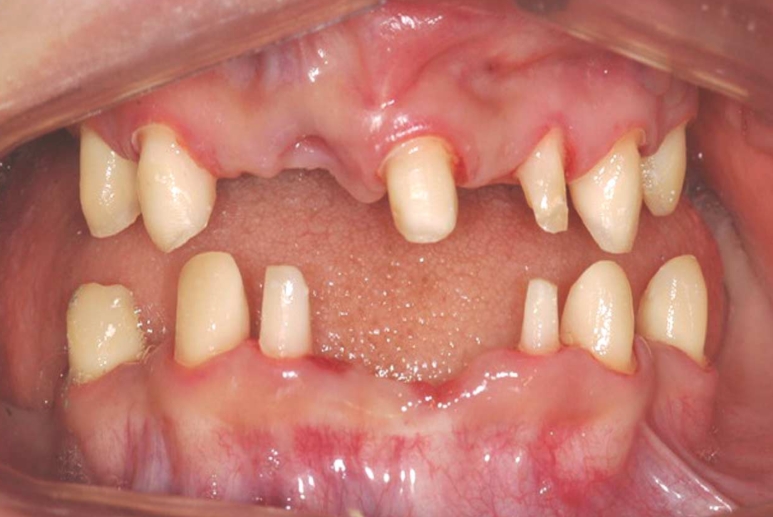
Hypohidrotic ectodermal dysplasia (HED) is the most of all ectodermal dysplasias, caused by an abnormality in the development of ectodermal tissues, which inlude skin, hair, teeth, sweat glands, and nails.[9][10] Patients with ectodermal dysplasia often have sparse hair and oligodontia, which is a condition where teeth are missing and are poorly developed.[9][10] Sweating is a very important function in the body in terms of thermoregulation. HED is mainly characterised by hypohidrosis due to the lack of sweat glands in the skin, which could lead to hyperpyrexia and sometimes death. In neonates, the mortality rate of HED reaches up to 30%, with the first year of life having the highest risk. [9] HED is caused by a genetic abnormality of the ectodysplasin A gene (EDA) and passed on by X-linked inheritance. The mutations of this gene results in the poor sweating ability or none at all in a person. The effects of this abnormality is usually more severe in males than in females. [11][10]
There is currently no pharmacological therapies for HED but there are methods applied to prevent the disease from aggravating. Neonates with HED are placed in incubators and monitored to prevent them from overheating. Management of this disease gets easier as the patient ages. Adults with HED can control their thermoregulation by staying in cool environments or drinking cold drinks to lower the body temperature. Currently, there are studies that aim to find a cure for this abnormality, e.g. gene replacement therapy in animal models.[10]
Congenital Alopecia Areata
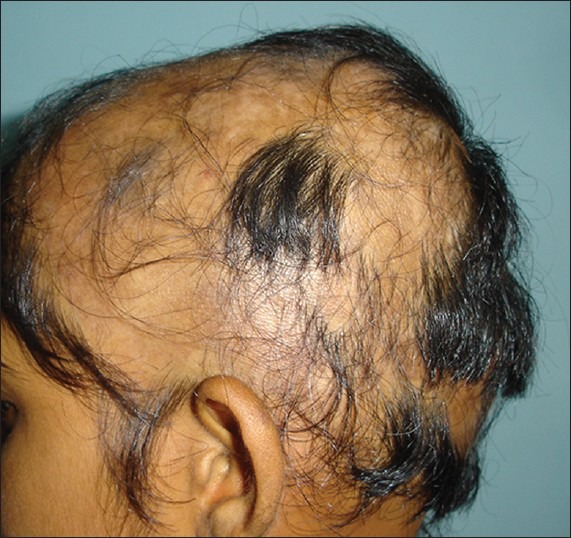
Alopecia areata (AA) is an abnormality of the hair affecting anagen hair follicles, characterised by well-demarcated patches of hair loss. It is non-scarring and can occur on the scalp and/or the body. 90% of AA cases occur on the scalp. 5%-10% of patients with AA lose all hair on their scalp; this is called alopecia totalis. While others lose all of their body hair, this is called alopecia universalis. [13] Its pathogenesis is considered to be both genetic and autoimmune. There is an abnormality with the genes related to the immune system and to the hair follicles. And histopathology shows signs of lymphatic infiltration of the hair follicles and the loss of these scalp lymphocytes allow hair follicles to recover.[14] High frequencies of catagen and telogen hair follicles are also present in areas affected by AA.[13]
There is currently no cure for AA. There are several treatments to combat AA but none of these have led to remission of the disease, the most effective being corticosteroids and topical immunotherapy.[13] A new method of treating alopecia areata is currently being studied. Transepidermal drug delivery (TED) is a new treatment that functions by creating micro-channels in the epidermis. By doing so, drug delivery to the skin is improved. This treatment was highly effective and had lower rates of side effects, e.g. pain, compared to previous treatments.[15]
References
- ↑ 1.0 1.1 1.2 1.3 <pubmed>15830002</pubmed>
- ↑ <pubmed>21504444</pubmed>
- ↑ <pubmed>23147310</pubmed>
- ↑ <pubmed>24520234</pubmed>
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 <pubmed>19824737</pubmed>
- ↑ 6.0 6.1 6.2 <pubmed>23419760</pubmed>
- ↑ 7.0 7.1 7.2 7.3 <pubmed>24124810</pubmed>
- ↑ <pubmed>21165248 </pubmed>
- ↑ 9.0 9.1 9.2 <pubmed>20682465</pubmed>
- ↑ 10.0 10.1 10.2 10.3 <pubmed>24678015</pubmed>
- ↑ <pubmed>21357618</pubmed>
- ↑ <pubmed>23960401</pubmed>
- ↑ 13.0 13.1 13.2 <pubmed>17269961</pubmed>
- ↑ <pubmed>16338213</pubmed>
- ↑ <pubmed>25260052</pubmed>