2012 Group Project 2
Somatosensory Development
Introduction
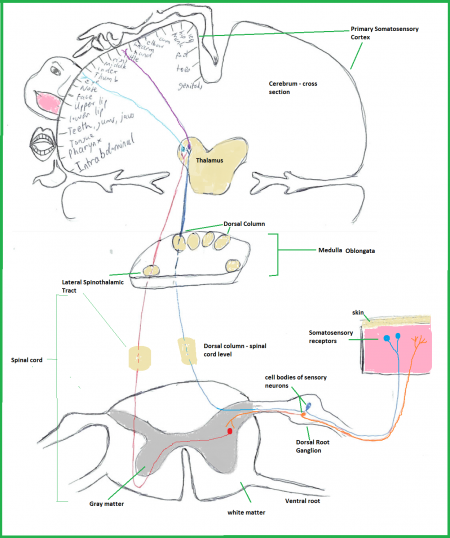
The somatosensory system is an important subdivision of the somatic nervous system comprising of a collection of receptors, tracts and nuclei. The system components convey the sensations of vibrations, light touch, pain and temperature to the consciousness (Creath, Kiemel, Horak, & Jeka, 2008) The system is important in conveying information about the body position and movements with significant influence on the body balance (Wong, Collins, & Kaas, 2010). The somatosensory system also plays an important role in motor control through conveying of feedback information about the muscular system dynamics including velocity of muscles, tension, length, joint position and movement and contact with the external environment. The system comprises of receptors in the muscles, skin, viscera and joints (Marani, 1994). The following picture shows the general organization of the somatosensory system.
(Lagercrantz, Hanson, Evrard & Rodeck, 2001)
Understanding the development of this systems both structurally and functionally during the fetal life is crucial in understanding how a fetus develops the capacity to receive and experience sensations delivered by thermal, mechanical, tactile and noxious stimuli (Willis, 2007).
The somatosensory systems development begins during the gestation period specifically the third week into the gestation period. By the end of the 9th week the fetus has a fully developed nervous system with sensory and receptors present at the skin level (Stiles, Reilly, Levine, Trauner, & Nass, 2012). Development of the system entails development of nerve fibers and receptors in the fetus body system. Development of the somatosensory system involves progressive changes in the structural alignment, neurochemical and functional changes with majority of the development changes taking place during the gestation period. Somatosensory receptors develop in the various parts of the body to enable detection and reception of stimuli which is then transmitted through the nerve fibers to the central nervous system (Nakamura & Morrison, 2008). Development of the somatosensory system also entails subsequent development of pathways including the dorsal column-medial lemniscal system.
This project looks at the anatomy, function and development of the central somatosensory system and a range peripheral receptors on the skin.
History of Discoveries
Weber recognized for his role in the study of the nervous system including the establishment of the Weber’s law (Giclu, 2007). Some of the historical research conducted by Weber concerned the various aspects of nervous system including inhibition of impulse transmission, summation, adaptation and fusion. The shift from philosophy to physiology can be attributed to Weber’s research work through which he influenced the view on the human system. Other discoveries that followed Weber’s discoveries about the somatosensory system include the discovery that most receptor endings in the skin, the connection between the system and the spinal cord. The other important historical discovery about the somatosensory system include the discovery of different kinds of electrical potential in the nervous systems not covered by Weber as the pioneer in the understanding of the nervous system (Deco & Rolls, 2006).
Central Somatosensory Differentiation
Adult Central Somatosensory systems:
Ascending components of the Central Somatosensory system include;
- the primary somatosensory cortex of the brain,
- the trigeminal system: – receives sensory signals from the face; [1]
- the dorsal column system and lateral spinothalamic tract:– receive signals from the rest of the body. [2] [3]
Dorsal column system and Lateral Spinothalamic tract:
Peripheral sensory neurons enter the spinal cord via the dorsal root ganglion. The sensory signal then get passed onto collateral fibres in the spinal cord which ascend via the dorsal column or lateral spinothalamic tract up the spinal cord. [3] From there, fibres go the lateral regions of the ventroposterior nucleus (VP) of the thalamus. From the thalamus, 3rd order neurons project out and into the primary somatosensory cortex so information can be processed. [3]
Trigeminal System:
Sensory signals from the face are passed through the trigeminal nerve which passes signals to the trigeminal sensory nucleus. Axons from this trigeminal sensory nucleus go to the medial regions of the VP of the thalamus. From there fibres conduct the signals to the primary somatosensory cortex.[4]
Development of the Primary Somatosensory Cortex:
Development of the primary somatosensory cortex is thought be controlled by both intrinsic factors and extrinsic factors. [5] Development of this region begins in late embryonic period and continues post-natally. The primary somatosensory cortex has separate functional groups of layer IV neurons called ‘barrels’. [6] In the adult, the barrels are arranged in a pattern, isomorphic to the pattern of somatosensory receptors on the face and body surface (see figure). [7] This patterning of the somatosensory cortex is the key step in its development. These layer IV neuron barrels receive inputs from the afferents coming from the ventroposterior nucleus (VP) thalamus and the posterior thalamic complex (POm). [8] These thalamocortical afferents of the VP and POm provide information that patterns the developing primary somatosensory cortex. [8] The extrinsic signalling by the VP and POm afferents from the thalamus may cause graded gene expression in the cortical neurons to pattern the somatosensory cortex. [8]
VP afferents develop just prior to the development of the area of the somatosensory cortex that will process the information from these VP afferents. [4] The VP afferents receiving information from the face and jaw differentiate before birth. [4] Then the lateral regions of the somatosensory cortex develop. Within 24hrs after birth, the VP afferents receiving sensory information from the rest of the body develops. [4] This will be followed by the development of the medial regions of the somatosensory cortex that processes the information from the body. [4] Consequently, there’s a lateral to medial gradient of somatosensory cortex development which controlled by the VP afferents from the thalamus.
Making Connections between Afferent Sensory Fibres and the Central Nervous System (CNS)
This is the process where sensory afferents synapse the neurons in the spinal cord so peripheral somatosensory information can be transmitted through the spinal reflex arc or up to the primary somatosensory cortex where the information can be processed. Sensory afferents from the periphery, with their cell bodies (soma) in the dorsal root ganglion, grow towards the spinal cord in stages to make these connections with the CNS.[9]
Stage 23;
- Axons of primary afferent neurons extend to the spinal cord. When these afferent neurons reach the CNS, axons of these afferent neurons bifurcate and begin to extend into the Primordium of the dorsal funiculus [9]
Stage 24:
- the afferent axons have extended 1 segment rostrally and 1 segment caudally relative to the axons' point of entry [9]
- the afferents start to grow within the white matter (periphery of Spinal Cord)[9]
Stage 28 –
- unbranched afferent axonal fibres invade gray matter at the border of Dorsal horn [9]
- axonal fibres extend rostrally and caudally and start sending fine collateral fibres into the gray matter of spinal cord (the cellular, central region of spinal cord)[9]
Stage 29:
- afferent fibres have extended 100-200μm into gray matter of the Dorsal Horn [9]
Touch
The sense of touch allows individuals to perform a myriad of functions through the receptors deep within dermal and epidermal layers of the skin. This sensory modality, though it’s development is not greatly understood among the five acknowledged sense subsets, it is essential for survival and development throughout life.[10]
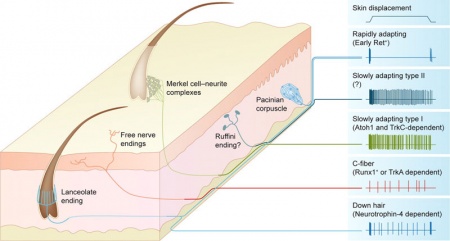
Receptors that are established throughout embryonic development linked to touch are mechanoreceptors/transducers such as Pacinian Corpuscle, Meissner’s Corpuscle, Merkel-cell-neurite complexes and Ruffini endings. Function and development of these receptors will be discussed in this section.
[10]
Touch Receptors
Pacinian Corpuscle
These receptors and nerve endings are found in the subcutaneous tissue of the skin and are also referred to as lamellar corpuscles. When stimulated these nerve endings result in action potentials which respond to the detection of changes in pressure against the skin in relation to vibrations sensations. This can allow for the ability of individuals to establish distinctions between rough and smooth surfaces.
Meissner’s Corpuscle
With similar sensory function as the Pacinian Corpuscle, these receptors are responsible for the detection of vibrations. However, Meissner's (tactile) corpuscles are more sensitive, and able to detect light touch sensations. Found in the dermal papillae under the epidermis of the skin, these receptors are distributed in many areas of the body, specifically the fingertips and lips.
Merkel-cell-neurite complexes
Similarly to the Meissner's Corpuscles these skin receptors are able to detect 'light touch' sensations via somatosensory afferents. However, specifically, these receptors are involved in spatial differentiation; establishment of shapes, sizes, textures of objects, in relation to touch. These receptors are also located in the epidermis of the skin in the stratum basale, in close proximity to the fingertips of mammals. This particular cells has been associated with abnormalities of growth and therefore in rare cases leads to Merkel-cell carcinoma.
Ruffini Endings
These mechanoreceptors are found within the dermal and subcutaneous layers of the skin and contribute to touch sensations in response to changes in joint movement, stretching of the skin and pressure applied to skin surfaces. This allows human beings to effectively hold and grip objects via these dendritic endings that are located within the fingers of individuals. Alterations in pressure and mechanics of the skin, joints and fingers, such as the sensation of an object slipping from one's hand are recognized by these receptors.
Neural Components
Mechanoreceptors are involved with the primary afferent pathways and terminals, which allow for the detection of tactile sensation. With particular reference to the receptors of touch; found in the skin, action potentials are triggered through alterations in skin, such as stretch, vibrations or larger or small stimuli. Ruffini Endings, Pacian and Meissner’s Corpuscles are activated via the surrounding components of their terminals. These mechanoreceptors are surrounded by a single capsules and specific cells and tissues (such as laminar ells in the Meissner’s corpuscles). [11] Primary/ first-degree afferents from the peripheral nerves of the posterior spinal cord and cranial ganglia act upon the surrounding tissues/components resulting in alterations in sodium and potassium channels, which in tactile sensation.
Pain
With the current advancements in study and research on the nervous system, the mechanisms responsible for the sensation or the sensory component of pain are now well understood. Different nerve fibres involved in the transmission of the pain impulse have been identified including the A-delta fibres, C fibres and A-beta fibres (Nakamura & Morrison, 2008). The A-delta fibres have been identified with response to mechanical or thermal stimulation such as pin prick or scald while C fibres respond to thermal, mechanical and chemical stimulation (Silberstein, 2003). The C fibres are slower in response to simulation and particularly transmit the dull, thudding pain of injury, inflammation or disease. On the other hand, the A-beta fibres transmit touch and play a crucial role in the sensation of pain. Current research in the development of pain fibres has seen the classification of pain into fast and slow pain and the pain fibres responsible for transmission of the pain. Fast pain is transmitted by the A-delta fibers with the stimulus being more superficial stimulus. Slow pain starts one second or more after stimulation and increases slowly over seconds or minutes and has been found to be associated with tissue distraction as well as being felt in both superficial and deep tissues. The various nerve fibers carry somatosensory information from the body periphery to the spinal cord. According to Medina and Lebovic (2009), studies have revealed that some nerve fibers present in the endometriotic tissues are responsible for pain severity.
Development of Nociceptors
| Embryonic Stage in Mice | Nociceptor Development |
| E11.5 | Specification of Nociceptors in the Dorsal Root Ganglia |
| E13 | Axons of Nociceptors begin extending to the periphery and towards the spinal cord |
| E14.5 | Substance P and CGRP are produced. Levels increase after nociceptors make contact with their target tissue in E18.5 |
| E15-17 | Functional synaptic junctions form between nociceptors and interneurons as part of the reflex arc |
| E17 | TTX resistant voltage-gated sodium channel Nav1.8, responsible for hyperexcitability of nociceptors, are expressed |
| E18.5 | Axons reach their peripheral Tissue |
| E18-20 | Axons reach dorsal horn of the spinal cord |
| P2 | TRPV1 capsaicin receptor expressed |
| P4-10 | NGF increases the sensitivity of Nociceptors |
| 3 weeks Postnatal | Fully functional reflex arcs form |
Nociceptor Specification:
Birth of nociceptors occurs in the DRG at E11.5 (embryonic day 11.5) in mice. [12] Much of sensory neuron differentiation is done via neurotrophin signalling. [13] Neurotrophin are growth factors that act by binding to neurotrophin receptors called Tyrosine kinase (Trk) receptors. Expression of Tyrosine kinase A (TrkA) receptors in Dorsal Root Ganglion (DRG) cells determines their fate as unmyelinated Nociceptors. [14] This because TrkA enables TrkA+ neurons to respond to certain neurotrophins, called nerve growth factor (NGF), that enable nociceptor differentiation. [15] TrkA signalling promotes the development of sensory channels in the nociceptors and this allows the nociceptors to respond to noxious stimuli. [16] One study has shown that mice without TrkA receptor are born without nociceptors. [13] Expression of TrkA receptors in nociceptors is up-regulated by the transcription factor Runx1. [17] Cells without the Runx1 gene result in an absence of TrkA receptors and were unable to develop to mature nociceptors. [17]
Nociceptor Survival
Once nociceptors are specified, receiving nerve growth factors (NGF) via the TrkA receptors increase the chance of their survival. This was shown by a study where NFG levels were over-expressed in transgenic mice and this caused the number of TrkA+ neurons to double. [18] [19] Nociceptors that do not receive enough NGF will not survive. [13]
Growth of Axons - to the Spinal Cord and Periphery
Increases in axon length, width and branching are all controlled by neurotrophins such as NGF. [20] These processes begin at embryonic day 11 to 13. [20] [21] By embryonic day 14, small c fibres such as nociceptors have reached the periphery target tissue such as the hindlimb of mice. [22] After activation of the Trk receptors by NGF, downstream signalling molecules cause these changes in axon. [21] These molecules include:
- Molecules in the Ras-Raf-ERK cascade – results in Elongation of the Axons
- PIK3 and Akt – increase the Diameter of the Axons
- Akt – can also increase the branching of the axon [21]
During embryonic days 18-20, axons of centrally directed nociceptors extend into the grey matter (dorsal horn) of the spinal cord. [22] The axons project into the dorsal horn while maintaining in a somatotopic pattern. [23] Similarly, as axons of sensory neurons such as nociceptors grow from the dorsal root ganglia to the periphery, the axons travel via specific pathways so that 1 spinal nerve innervates 1 region of skin. [24] This gives rise to the dermatomes. [24]
Extracellular signalling molecules direct the growth of the axons to ensure they reach their correct targets. NGF increases sprouting of axons but this may lead to excessive nociceptive innervation of the peripheral tissue. [25] This issue is overcome by factor Semaphorin 3A which inhibits aberrant nociceptor axon growth. [25] By embryonic day 18.5, neurons reach their peripheral target tissues. [26]
Determination of the Physiological Phenotype of Nociceptors
A lot of this functional development occurs postnatally. For example, TRPA1, a receptor that detects noxious temperature and chemical stimuli, are expressed by postnatal day 2 nociceptors . [27] These receptors play a role in detecting mechanical and thermal stimuli during inflammation. On the other hand, tetrodotoxin (TTX) resistant voltage-gated sodium channel Nav1.8 is expressed as early as embryonic day 17 (E17). [28] These channels play an important role in generating chronic pain because they control the hyperexcitability of the neurons including nociceptors. However, adult levels of these sodium channels are not reached until postnatal day 7 (P7). [28]
Development of the Chemical Phenotype of Nociceptors
In nociceptors, as well as other small diameter neurons, neuropeptides such as substance P (SP) and calcitonin gene-related peptide CGRP, are expressed. [26] Expression of these neuropeptides that characterize nociceptors, are controlled by both intrinsic and extrinsic cues. These neuropeptides SP and CGRP rise as early as embryonic day 14.5 – at this stage nociceptors have not made contact with their target tissues. [26] Thus nociceptors do not require contact with peripheral target tissues to express some levels of SP and CGRP. However, studies also show that number of CGRP expressing nociceptors increased under the influence of epidermal cells. [26] [29] Thus extrinsic cues, through the contact with target tissues, enhance the development of the chemical phenotype of nociceptors.
Increase in the Nociceptor Innervation Density
Sensory neurons, including the TrkA+ nociceptors, increases their innervation density due to access to local growth factors such as NGF and brain derived growth factor. [30] This increase in innervation density involves an increase in both the innervation of the tissue by the endings of an individual sensory neuron and the number of neurons. [30]
Increase in Nociceptor Sensitivity
Nociceptor sensitisation to noxious stimuli such as heat and capsaicin occurs postnatally. [31] This process involves NGF activating TrkA receptor which initiates a signalling pathway that results in the sensitisation of the receptor, TRPV1 to heat and capsaicin. [32] It has been shown that NGF is able to sensitise nociceptors during postnatal day 4-10. [31] NGF is unable to increase the sensitivity of nociceptors before this stage. Bradykinin, however, can increase the nociceptor sensitivity in neonatal neurons. [31]
Hot/Cold
In addition to sensory modalities such as pressure and pain, the human body is able to detect the temperature of its surrounding environment. This is called thermoreception, and is extremely important for a variety of reasons. The ability to sense temperature is important for maintaining homeostasis in many biological processes. It is also of practical safety use, we are able to reliably avoid stimuli that are either too hot or too cold and may do us harm.
The sensation of temperature is made through free nerve endings in the epidermis of the skin. These free nerve endings contain specialised ion channels called temperature activated transient receptor potential ion channels[33]. We will refer to them as ThermoTRP’s. These receptors are able to generate action potentials in response to changes in temperatures in the environment surrounding the nerve ending in the skin. The nerve impulse generated by these receptors is conveyed along the nerve fibre and into the dorsal root ganglion. There are two main types of ThermoTRP, those that are activated by warm stimuli and those that are activated by cold stimuli[33].
Warm
There are four main ThermoTRP receptors responsible for the perception of warm stimuli, both innocuous and noxious[34]. They are called TRPV1, TRPV2, TRPV3, and TRPV4. Each receptor unresponsive to mechanical stimuli, but can be excited by some chemicals such as the capsaicin in the chili plant. The firing of each receptor is inhibited by falling temperatures.
- TRPV1. This receptor is responsible by the sensation of mild heat. The receptor is activated by temperatures over 30 ˚C. As temperatures rises the rate of nerve impulses also increases, reaching a maximum rate at 42 ˚C[34]. Either side of 42 ˚C, the firing rate of the nerve decreases, forming a bell shaped curve. This means that the firing rate of the receptor conveys information relating to the environments temperature back to the central nervous system.
- TRPV2. This receptor only fires an action potential when in contact with temperatures sufficient to cause harm .This is generally temperatures over 52 ˚C [33] [34].
- TRPV3. Activated strongly by temperatures in the 34-38 ˚C range.
- TRPV4. Activated at 27 – 34 ˚C.
Cold
Cold thermoreceptors essentially work in an identical manner to warm thermoreceptors. Instead of being activating by rising temperatures, they are stimulated by falling temperatures. There are two main receptors responsible for perception of cold stimuli.
- TRPM8. This receptor is responsible for the perception of innocuous cold temperatures, that is, temperatures that will not cause the body harm. They are activated when the temperature of the environment surrounding the nerve ending falls to between 25 and 28 ˚C. As seen with the TRPV1 receptor, the stimulation of TRPM8 by a range of temperatures produces a bell shaped curve with a maximum firing rate seen around 25-26 ˚C. [33] [34].
- ANKTM1. Noxious or damaging cold temperatures are those at or below the 17 ˚C mark. These extreme temperatures are able to activate the ANKTM1 receptor[33].
Embryology and Development
Stay tuned!
Pressure
The development of pressure receptors takes place during the gestation period with the rapidly adapting pressure receptors developing first then followed by the slow adapting pressure receptors (Kinkelin, Stucky, L & Koltzenburg, 1999). Although these pressure receptors are present throughout the fetal life to adulthood, their depolarization responses to chemical irritants, mechanical injury and inflammatory mediators are been found to be similar in both the fetus and adults. Pressure-sensitive receptors of different types found in the skin where they detect changes in pressures. They respond to physical contact such as brushing against a wall, mosquito landing site or any form of touch on the skin. Bunched receptors known as Merkel’s discs have been found to specialize in conveying information about continuous pressure exerted on the surface of the skin (Ragert, Nierhaus, Cohen & Villringer, 2008). Pacinian corpuscles respond to quick changes in touch or pressure by firing off rapid bursts of signals before they decrease with time (Irie, Kato, Yakushji, Hirose & Mizuta, 2011). Baroreceptors are special pressure receptors found in the right atrium of the heart and play the role of detecting changes in blood pressure enabling the body to control the pressure and the amount of blood flowing into the heart (Ino-Oka, Sekino, Kajikawa, Inooka, Imai & Hashimoto, 2008). Different studies have established urinary bladder mechanoreceptors as responsible for detecting changes in bladder volume or intravesical pressure (Downie & Armour, 1992). Discovery of the pressure receptor locations in human bodies has been exploited in nursing interventions including the touch therapy or massage (Field, 1998). Massage therapy has been found to be effective in enhancing various clinical conditions including reduction of pain, diminishing of depression, enhancing attentiveness, promotion of immune function as well as promotion of growth and development of pre-term infants (Sanders, 2010). According to Field (1998), intentional stimulation of pressure receptors during massage therapy results in enhanced vagal activity associated with the diverse benefits accrued from massage therapy. Understanding of pressure receptors has been discovered to be important in the treatment of balance disorders. The pressure receptors in the skin detect bodily contact with the environment enabling control of the contact during treatment of balance disorders (George & Athanasios, 1999).
- Pressure receptors consists of nerve endings encapsulated by specialized connective tissue
- A-beta receptors:
- Ruffini endings respond to pressure in both hairy and glabrous skin (slow adapting receptor)
- Krause corpuscle respond to pressure in lips, tongue and genitals
- Merkel cells respond to pressure of the skin, epidermis of globrous skin
- Pacinian corpuscles:
- Found in the deeper layers of the skin
- Rapidly adapting receptors
- Consists of a nerve ending with layers of connective tissue wrapped around it
- When the connective tissue is deformed due to pressure, it presses on the nerve endings which trigger an electrical impulse
- Respond to transient pressure
- Development is dependent on sensory innervations
- Corpuscles form in the dermis, hypodermis, surfaces of muscles, tendons and aponeuroses
- First appear during the fourth foetal month of development
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1244282/?page=2
http://onlinelibrary.wiley.com/doi/10.1002/dvdy.20156/full#sec1-4
Current Research
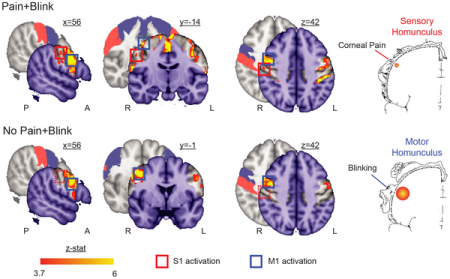
Somatosensory Activation by Corneal Pain:
Investigation is currently done on to localize somatotopic representation of pain from the cornea. [35] This type of research gives insight into the mechanism of chronic pain development in various eye conditions. [35] This study shows processing of corneal pain information occur in localized regions of the primary somatosensory cortex. [35] When the cornea pain receptors are stimulated, these localized regions o the somatosensory cortex are activated. [35] The region of the somatosensory cortex that deals with corneal pain, also deals with blinking or photophobia. Such finding has been achieved using functional Magnetic Resonance Imaging (fMRI).[35] See figure
Glossary
- Innocuous
- A stimulus that poses no threat of harming the tissues and structures of the body.
- Noxious
- A stimulus that me be toxic to the tissues of the human body. An example of this would be the extremely hot temperatures of a fire, which are perceived as noxious by thermorecepters in the skin.
References
- ↑ <pubmed> 8440772</pubmed>
- ↑ <pubmed> 14485390</pubmed>
- ↑ 3.0 3.1 3.2 <pubmed>1127457</pubmed>
- ↑ 4.0 4.1 4.2 4.3 4.4 <pubmed>7962713</pubmed>
- ↑ <pubmed>10764649</pubmed>
- ↑ <pubmed>4141363</pubmed>
- ↑ <pubmed>7721983</pubmed>
- ↑ 8.0 8.1 8.2 <pubmed>2461788</pubmed>
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 9.6 <pubmed>2918087</pubmed>
- ↑ 10.0 10.1 <pubmed>20956378</pubmed>
- ↑ <pubmed>19538631</pubmed>
- ↑ <pubmed>490183</pubmed>
- ↑ 13.0 13.1 13.2 <pubmed>8145823</pubmed>
- ↑ <pubmed>8835730</pubmed>
- ↑ <pubmed>15247919</pubmed>
- ↑ <pubmed>22787056</pubmed>
- ↑ 17.0 17.1 <pubmed>16429136</pubmed>
- ↑ <pubmed>9283812</pubmed>
- ↑ <pubmed>8126547</pubmed>
- ↑ 20.0 20.1 <pubmed>9920667</pubmed>
- ↑ 21.0 21.1 21.2 <pubmed>12123609</pubmed>
- ↑ 22.0 22.1 <pubmed>10701827</pubmed>
- ↑ <pubmed>2442203</pubmed>
- ↑ 24.0 24.1 <pubmed>7175742</pubmed>
- ↑ 25.0 25.1 <pubmed>14749426</pubmed>
- ↑ 26.0 26.1 26.2 26.3 <pubmed>9092599</pubmed>
- ↑ <pubmed>16630838</pubmed>
- ↑ 28.0 28.1 <pubmed>11487631</pubmed>
- ↑ <pubmed>12733058</pubmed>
- ↑ 30.0 30.1 <pubmed>10407031</pubmed>
- ↑ 31.0 31.1 31.2 <pubmed>15201308</pubmed>
- ↑ <pubmed>12815188</pubmed>
- ↑ 33.0 33.1 33.2 33.3 33.4 <pubmed>12838328</pubmed>
- ↑ 34.0 34.1 34.2 34.3 <pubmed>19822171</pubmed>
- ↑ 35.0 35.1 35.2 35.3 35.4 <pubmed>PMC3433421</pubmed>
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
Link to Pacinian Corpuscle image
1. http://thediagram.com/3_1/pacinian.html
2. http://www.biologymad.com/nervoussystem/nerveimpulses.htm
Links to Meissner’s Corpuscle Images
1. http://www.siumed.edu/~dking2/intro/images/IN038b.jpg
2. http://www.virtualworldlets.net/Worlds/Listings/BodySenses/Texture-MeissnerCorpuscle.jpg
--Mark Hill 12:22, 15 August 2012 (EST) Please leave the content listed below the line at the bottom of your project page.
2012 Projects: Vision | Somatosensory | Taste | Olfaction | Abnormal Vision | Hearing