2011 Lab 6 - Postnatal: Difference between revisions
No edit summary |
|||
| Line 18: | Line 18: | ||
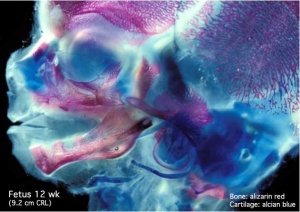
==Fetal Head Growth== | ==Fetal Head Growth== | ||
{| | |||
[[File:Fetal_head_growth_circumference_graph02.jpg| | | [[File:Fetal_head_growth_circumference_graph02.jpg|400px]] | ||
| [[File:Fetal_head_growth_circumference_graph01.jpg|400px]] | |||
[[File:Fetal_head_growth_circumference_graph01.jpg| | |} | ||
:'''Links:''' [[Book_-_Contributions_to_Embryology_Carnegie_Institution_No.48|Historic - Human Fetus (CRL 43mm) Skull]] | :'''Links:''' [[Book_-_Contributions_to_Embryology_Carnegie_Institution_No.48|Historic - Human Fetus (CRL 43mm) Skull]] | ||
Revision as of 10:36, 1 September 2011
| 2011 Lab 6: Introduction | Trilaminar Embryo | Early Embryo | Late Embryo | Fetal | Postnatal | Abnormalities | Online Assessment |
Introduction
The Skull is a unique skeletal structure in several ways: embryonic cellular origin (neural crest), form of ossification (intramembranous and endochondrial) and flexibility (fibrous sutures).
- The cranial vault (which encloses the brain) bones are formed by intramembranous ossification.
- While the bones that form the base of the skull are formed by endochondrial ossification.
- The bones enclosing the brain have large flexible fibrous joints (sutures) which allow:
- the head to pass through the birth canal
- postnatal brain growth
- ossification continues postnatally, through puberty until mid 20s.
- in old age the sutures separating the vault plates are often completely ossified.
- Flexible fibrous sutures allow growth of the brain to be accomodated by calvarial plate growth.
- Recent molecular studies have show that noggin (a BMP antagonist) is involved in closure of these sutures.
Fetal Head Growth
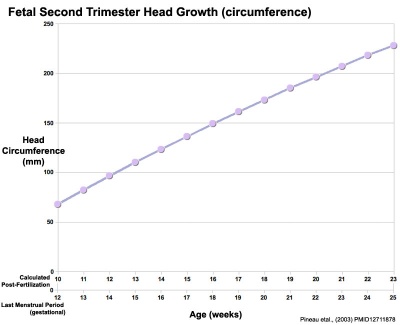
|
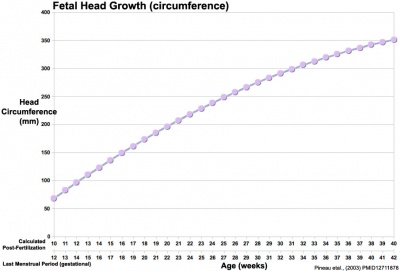
|
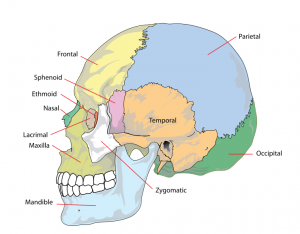
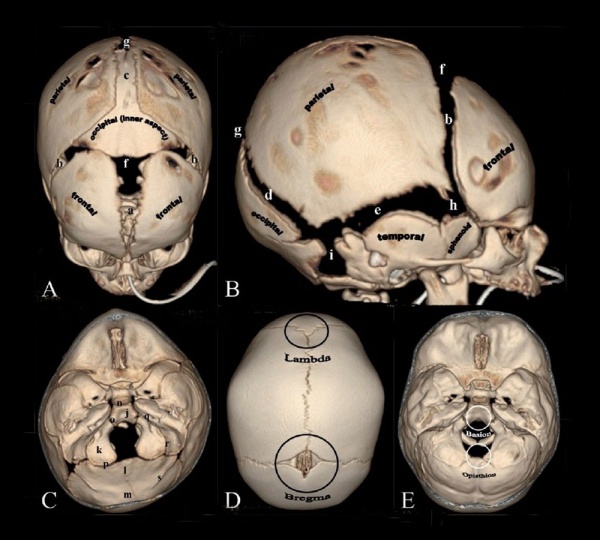
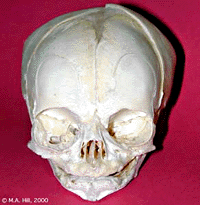
Skull Views
|

|

|
| anterior view | superior view | lateral view |
| showing anterior fontenelle, sutures, mandible | showing anterior fontenelle, sutures | showing suture, mandible |
Skull Sutures
The bones enclosing the brain have large flexible fibrous joints (sutures) which allow firstly the head to compress and pass through the birth canal and secondly to postnatally expand for brain growth. (More? Molecular Skull Sutures) These sutures gradually fuse at different times postnatally, firstly the metopic suture in infancy and the others much later. Abnormal fusion (synostosis) of any of the sutures will lead to a number of different skull defects, leading to disruption of brain development. (More? Abnormal Synostosis) In old age all these sutures are generally completely fused and ossified.
At the molecular level, accelerated suture intramembranous ossification can be mediated through a dual role of β-catenin in both the expansion of osteoprogenitors and the maturation of osteoblasts.[1] These researchers also show that disruption of Axin2/β-catenin signaling alters the regulation of the downstream transcription target, cyclin D1, in the canonical Wnt pathway.Pubmed: 21108844
coronal suture
lambdoid suture
metopic suture begins at nose and runs superiorly to meet sagittal suture and fuses during infancy (fusion beginning at 3 months and completes by 6 to 8 months of age) before all other cranial sutures.
sagittal suture
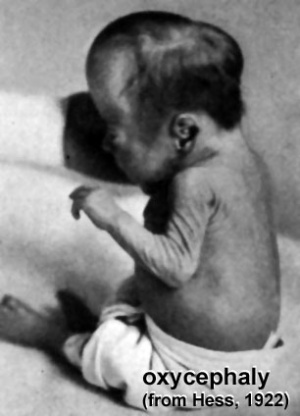
Abnormal Synostosis
There are several skull deformities caused by premature fusion (synostosis) of different developing skull sutures. Suture abnormalities are classified as either "simple" (only one suture involved) or "compound" (two or more sutures involved).
Craniosynostosis
Attenuation of signaling pathways stimulated by pathologically activated FGF-receptor 2 mutants prevents craniosynostosis.[2] "Craniosynostosis, the fusion of one or more of the sutures of the skull vault before the brain completes its growth, is a common (1 in 2,500 births) craniofacial abnormality, approximately 20% of which occurrences are caused by gain-of-function mutations in FGF receptors (FGFRs). ...These experiments show that attenuation of FGFR signaling by pharmacological intervention could be applied for the treatment of craniosynostosis or other severe bone disorders caused by mutations in FGFRs that currently have no treatment."
Craniofrontonasal Syndrome
Craniofrontonasal syndrome (CFNS) is a human X-linked developmental disorder caused by a mutation in ephrin-B1 affecting mainly females. Characterised by abnormal development of cranial and nasal bones, craniosynostosis (premature coronal suture fusion), and other extracranial anomalies (limb polydactyly and syndactyly).
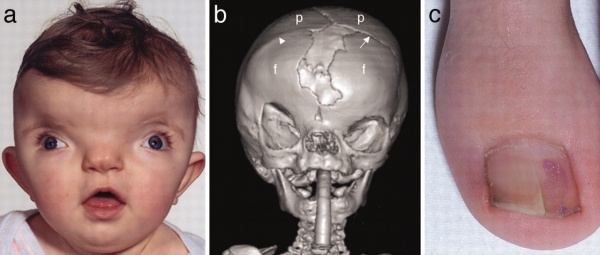
|
(a) Facial view showing marked hypertelorism, divergent squint, and central nasal groove (subject age, 1 year).
|
| Craniofrontonasal syndrome[3] | Links: OMIM - Craniofrontonasal Syndrome |
Skull Bone Histology
A histological image of a skull bone formation by Intramembranous ossification.
References
| 2011 Lab 6: Introduction | Trilaminar Embryo | Early Embryo | Late Embryo | Fetal | Postnatal | Abnormalities | Online Assessment |
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 19) Embryology 2011 Lab 6 - Postnatal. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/2011_Lab_6_-_Postnatal
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G