2011 Lab 1: Difference between revisions
| Line 342: | Line 342: | ||
{{Template:Menstrual Links}} | {{Template:Menstrual Links}} | ||
== Fertilization Dynamics == | ==Fertilization== | ||
Fertilization is a complex interaction between the two haploid gametes (oocyte and spermatozoa) resulting in a single diploid cell (zygote). Following entry of the spermatazoa into the oocyte a series of changes occur within the oocyte and zona pellucida that block further fertilization by additional bound spermatozoa (polyspermy). | |||
Due to both scientific and medical research on this process, this can now occur outside the body (''in vitro fertilization'') as well as fertility therapies to aid normal (''in vivo fertilization''). In addition, our understanding of fertilization has led to the development of a number of alternative fertility control methods. | |||
=== Fertilization Dynamics === | |||
{| border='0px' | {| border='0px' | ||
Revision as of 13:27, 27 July 2011
Gametogenesis and Fertilization
Introduction
This first lab class will have 2 main parts.
- An introduction to the basics of gametogenesis and Fertilization.
- An opportunity to set up your own student page and begin learning some basic editing for your individual assessment page. I will demonstrate by making a Test Student 2011 page.
Objectives
- Work through exercises associated with gametogenesis and fertilization (fertilisation).
- Introduce the online support materials.
- Introduce the individual assessments (including your first in this Lab class).
- Introduce the group assessment project.
Introduction
This page covers gametogenesis and fertilization. With the help of the tutors and other students you will work your way through identifying features described in the text.
Begin by looking at the ovary and the formation of the follicle containing the egg which matures and is released upon ovulation. The images are arranged in series so that progressive stages of the maturing follicle can be seen. The final image on this current page is a link to a movie showing follicle development and ovulation. Use the series of images of the cat ovary below to identify the key features described in the associated text.
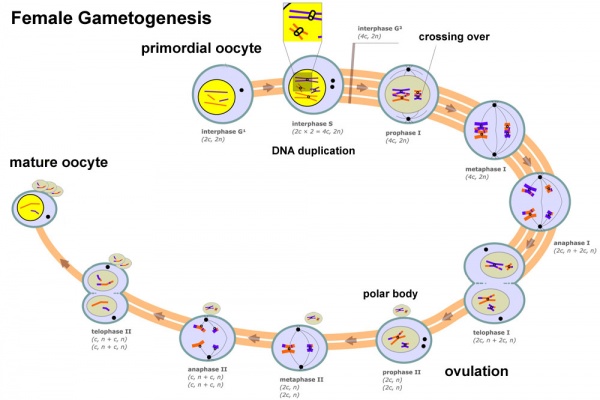
Female Gametogenesis
In females, the total number of eggs ever to be produced are present in the newborn female.
- All eggs are arrested at an early stage of the first meiotic division as a primary oocyte (primordial follicle). Following purberty, during each menstrual cycle, pituitary gonadotrophin stimulates completion of meiosis 1 the day before ovulation.
- In meiosis 1, a diploid cell becomes 2 haploid (23 chromosomes) daughter cells, each chromosome has two chromatids. One cell becomes the secondary oocyte the other cell forms the first polar body.
- The secondary oocyte then commences meiosis 2 which arrests at metaphase and will not continue without fertilization.
- At fertilization meiosis 2 completes, forming a second polar body. Note that the first polar body may also undergo this process forming a third polar body.
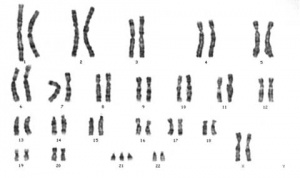
Female Abnormalities
Meiotic non-disjunction resulting in aneuploidy, most are embryonic lethal and not seen. The potential for genetic abnormalities increase with maternal age.
- Autosomal chromosome aneuploidy
- trisomy 21 - Down syndrome
- trisomy 18 - Edwards syndrome
- trisomy 13 - Patau syndrome
- Sex chromosome aneuploidy
- monosomy X - Turner's Syndrome
- trisomy X - Triple-X syndrome
- 47 XXY - Klinefelter's Syndrome
Male Gametogenesis
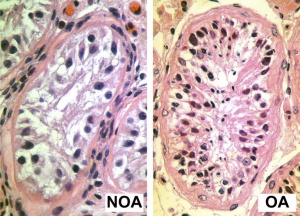
In males, sperm continues to be generated throughout life from a stem cell population in the testis. Spermatozoa maturation involves two processes meiosis and spermiogenesis
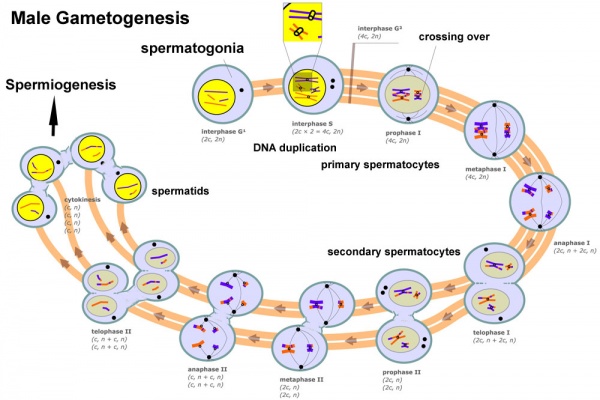
The above figure compares meiosis to the female (the polar bodies have been removed and labelling updated).
Human Spermatozoa Development
- Spermatogenesis process of spermatagonia mature into spermatazoa (sperm).
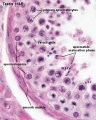
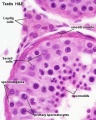
- Continuously throughout life occurs in the seminiferous tubules in the male gonad- testis (plural testes).
- At puberty spermatagonia activate and proliferate (mitosis).
- about 48 days from entering meiosis until morphologically mature spermatozoa
- about 64 days to complete spermatogenesis, depending reproduction time of spermatogonia
- follicle stimulating hormone (FSH) - stimulates the spermatogenic epithelium
- luteinizing-hormone (LH) - stimulates testosterone production by Leydig cells
Links: Spermatozoa Development | MBoC - Sperm | MBoC - Highly simplified drawing of a cross-section of a seminiferous tubule in a mammalian testis | MBoC - Cytoplasmic bridges in developing sperm cells and their precursors
Puberty
- In humans at puberty, hormonal and morphological changes occur within the gonad and other systems (secondary sex characteristics).
- Within the testis the immature Sertoli cells cease to proliferate and differentiate.
- Spermatogonium proliferate and spermatogenesis begins.
- It takes about 70 days for cells to mature from the diploid spermatogonium to a primary spermatocyte.
- This maturation occurs in waves along the seminiferous tubules.
Ejeculate
- release of spermatozoa and accessory gland secretions from the male genital tract (3.5 ml)
- 200-600 million sperm, by volume less than 10 % spermatozoa
- Accessory Gland secretions - 60 % seminal vesicle, 30 % prostate and 10 % bulbourethral
Male Abnormalities
- Oligospermia - (Low Sperm Count) less than 20 million sperm after 72 hour abstinence from sex
- Azoospermia - (Absent Sperm) blockage of duct network
- Immotile Cilia Syndrome - lack of sperm motility
Differences in Mammalian Meioses
| Female Oogenesis | Male Spermatogenesis | |
| Meiosis initiated | once in a finite population of cells | continuously in mitotically dividing stem cell population |
| Gametes produced | 1 / meiosis | 4 / meiosis |
| Meiosis completed | delayed for months or years | completed in days or weeks |
| Meiosis Arrest | arrest at 1st meiotic prophase | no arrest differentiation proceed continuously |
| Chromosome Equivalence | All chromosomes exhibit equivalent transcription and recombination during meiotic prophase | Sex chromosomes excluded from recombination and transcription during first meiotic prophase |
| Gamete Differentiation | occurs while diploid (in first meiotic prophase) | occurs while haploid (after meiosis ends) |
Male Gametogenesis
In males, sperm continues to be generated throughout life from a stem cell population in the testis. Spermatozoa maturation involves two processes meiosis and spermiogenesis

The above figure compares meiosis to the female (the polar bodies have been removed and labelling updated).
Human Spermatozoa Development
- Spermatogenesis process of spermatagonia mature into spermatazoa (sperm).
- Continuously throughout life occurs in the seminiferous tubules in the male gonad- testis (plural testes).
- At puberty spermatagonia activate and proliferate (mitosis).
- about 48 days from entering meiosis until morphologically mature spermatozoa
- about 64 days to complete spermatogenesis, depending reproduction time of spermatogonia
- follicle stimulating hormone (FSH) - stimulates the spermatogenic epithelium
- luteinizing-hormone (LH) - stimulates testosterone production by Leydig cells
Links: Spermatozoa Development | MBoC - Sperm | MBoC - Highly simplified drawing of a cross-section of a seminiferous tubule in a mammalian testis | MBoC - Cytoplasmic bridges in developing sperm cells and their precursors
Puberty
- In humans at puberty, hormonal and morphological changes occur within the gonad and other systems (secondary sex characteristics).
- Within the testis the immature Sertoli cells cease to proliferate and differentiate.
- Spermatogonium proliferate and spermatogenesis begins.
- It takes about 70 days for cells to mature from the diploid spermatogonium to a primary spermatocyte.
- This maturation occurs in waves along the seminiferous tubules.
Ejeculate
- release of spermatozoa and accessory gland secretions from the male genital tract (3.5 ml)
- 200-600 million sperm, by volume less than 10 % spermatozoa
- Accessory Gland secretions - 60 % seminal vesicle, 30 % prostate and 10 % bulbourethral
Male Abnormalities
- Oligospermia - (Low Sperm Count) less than 20 million sperm after 72 hour abstinence from sex
- Azoospermia - (Absent Sperm) blockage of duct network
- Immotile Cilia Syndrome - lack of sperm motility
Differences in Mammalian Meioses
| Female Oogenesis | Male Spermatogenesis | |
| Meiosis initiated | once in a finite population of cells | continuously in mitotically dividing stem cell population |
| Gametes produced | 1 / meiosis | 4 / meiosis |
| Meiosis completed | delayed for months or years | completed in days or weeks |
| Meiosis Arrest | arrest at 1st meiotic prophase | no arrest differentiation proceed continuously |
| Chromosome Equivalence | All chromosomes exhibit equivalent transcription and recombination during meiotic prophase | Sex chromosomes excluded from recombination and transcription during first meiotic prophase |
| Gamete Differentiation | occurs while diploid (in first meiotic prophase) | occurs while haploid (after meiosis ends) |
Oogenesis
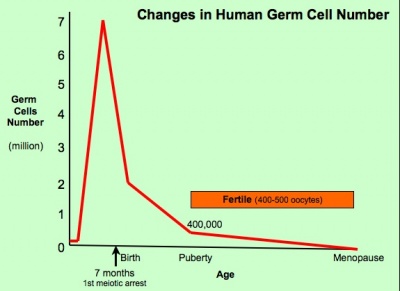
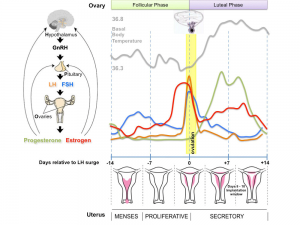
The graph below shows the changes in human germ cell numbers in the ovary with age, peaking at about 7 million (occuring in early fetal development) and then decreasing by apopotic cell death. At puberty there remain only about 400,000 and only about 10% of these will be released through reproductive life. (More? Menstrual Cycle)
(Based on data from: Hassold, etal., Environ Mol Mutagen 1996. 28: 167-175)
In the developing human ovary, oocytes remain at the diplotene stage of the first meiosis from fetal life through postnatal childhood, until puberty when the lutenizing hormone (LH) surges stimulate the resumption of meiosis.
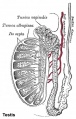
Whole Ovary
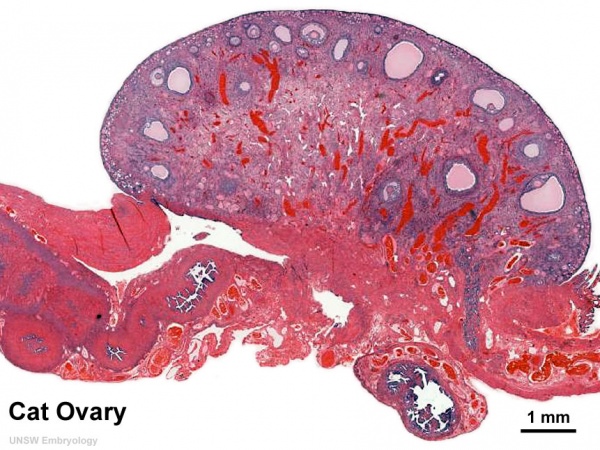
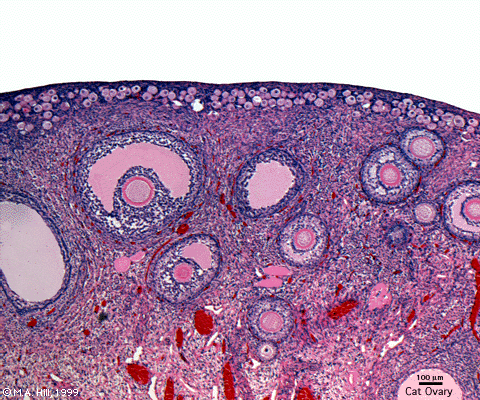
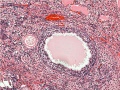
Ovary (cat, cross-section) showing histology and maturation of follicle.
Image (low magnification) showing cortical primordial follicles with primary (preantral) and secondary (antral) follicles lying deeper. Mesovarium at lower right and blood vessels in medullary region.
At this magnification, the overall organization of the ovary can be observed, cortex/medulla organization and arrangement of the maternal blood vessels, but few specific follicle details can be seen.
The next image is of the ovarian cortical region.
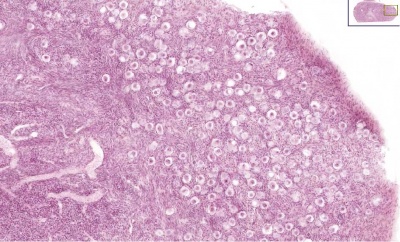
Ovary Cortex (low power)
Ovary cortex showing primordial follicles.
At the top of the image, is the outside of the ovary.
The thick connective tissue outer layer is the tunica albuginea. Over which a single layer of cells called the germinal epithelium (not visible) cover the surface of the ovary.
The next layer contains the earliest primordial follicles, single cells with pale cytoplasm and darkly stained nuclei.
The next layer contains many growing follicles at various stages of maturity and development. There is also evidence of degeneration as atretic follicles.
At the bottom of the image, is the medullary region of the ovary. Note the large number of maternal blood vessels which are the circulatory conduits for the estrogens and progesterones produced by the theca surrounding the ovarian follicles.
Note: germinal epithelium, tunica albuginea, primordial and atretic follicles. Note larger preantral follicle with (from the centre out) nucleus of maturing oocyte, oocyte cytoplasm, zona pellucida (pink ring), follicle cells, stromal cells.
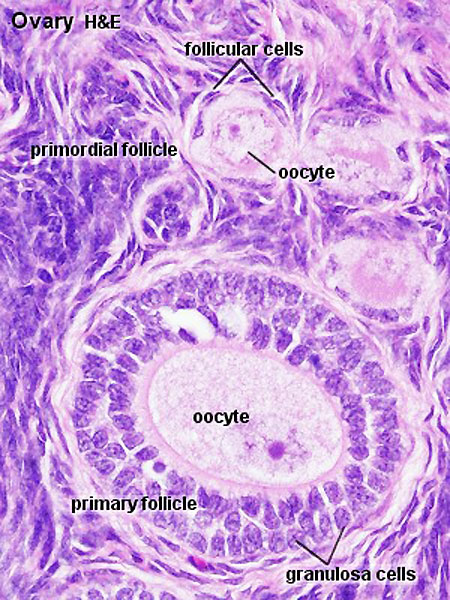
Ovary Cortex Primordial and Primary Follicles
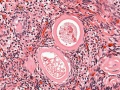
View of cortical ovary region showing primordial follicles and a single preantral follicle, with atretic follicle to its left. Bottom of picture shows outer cells of antral follicle.
High power view of ovary cortical region showing primordial follicles and a single preantral follicle.
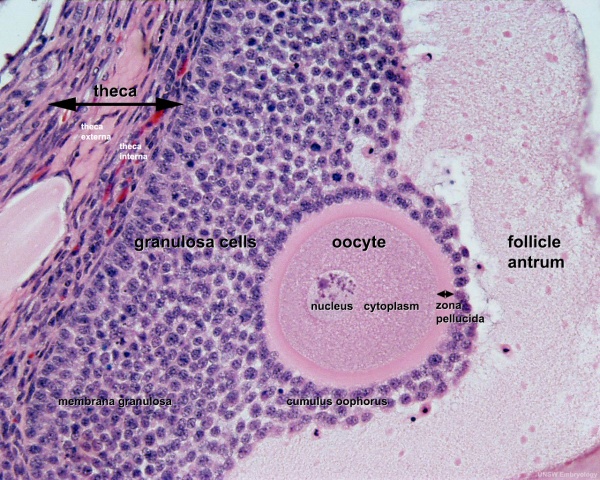
Features: germinal epithelium, tunica albuginea, preantral follicle, nucleus of oocyte, oocyte cytoplasm, zona pellucida, Call-Exner body, stratum granulosa, basement membrane, theca, blood vessels surrounding follicle in theca layer.
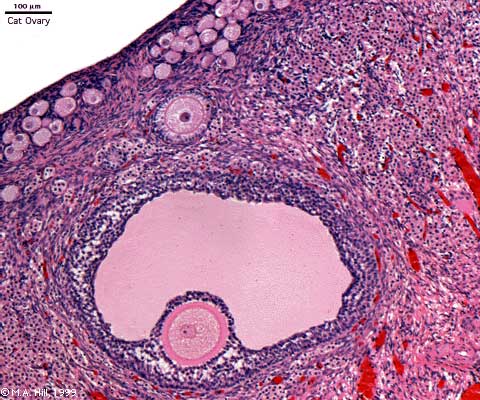
Ovary Cortex and Medulla
Low power view of ovary cortex and medullary region and high power image within an antral follicle.
In the low power image note 3 stages of follicle development (primordial, preantral and antral).
Features:
- cortical primordial follicles
- oocyte
- follicular cells
- stromal cells
- preantral follicle- zona pellucida, stratum granulosa, theca
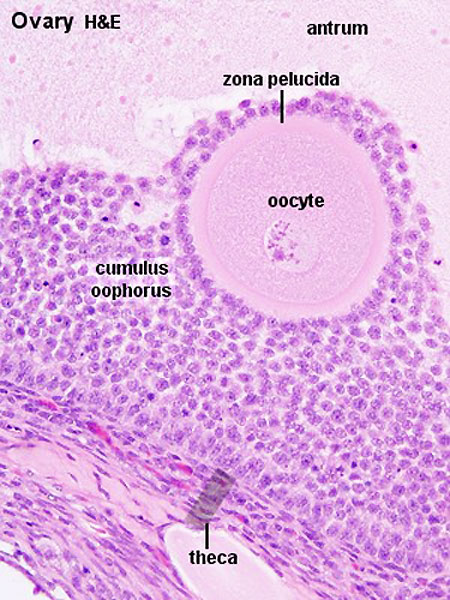
- early preovulatory follicle (Graafian) - oocyte, zona pellucida, corona radiata, cumulus oophorus, liquor folliculi, stratum granulosa, theca interna, theca externa, blood vessels surrounding follicle
Follicle Development
The development of a primordial follicle to a preovulatory follicle takes in excess of 120 days. After it has become a primary follicle of about 0.2 mm diameter it takes about 65 days to develop into a preovulatory follicle. Cohorts of follicles continually develop but only one is most sensitive to hormonal stimulation and is "selected", becoming the dominant follicle. All others in this cohort will undergo atresia.
Fertility Treatments
Superovulation therapy is a fertility drug treatement (oral clomiphene citrate and/or injectable FSH with or without LH) aimed at stimulating development/release of more than one follicle during a single menstrual cycle.
Follicle Classification
The above images show the histological changes that occur with follicle development (folliculogenesis). In humans, this entire process occurs over the timecourse of at least 3 menstrual cycles. This means that within the ovary during each cycle (at any point in time) many follicles can be either developing (folliculogenesis), regressing (atresis) and only a single follicle will be selected as ready for release. The selected follicle readied for release, generally one of the largest antral follicle, and can be classifed or described as: an antral preovulatory follicle or Graafian follicle or type 8 follicle (depending upon the classification used).
Classification systems - There are several different nomenclatures for the stages of follicle maturation (shown below) all of which makes the literature very confusing. The simplest is primordial, preantral, antral, Preovulatory (Graffian). You can also use the 5 step follicle classification: Primordial, Primary, Secondary, Tertiary, Preovulatory. Note that some classifications refer to the antral follicle as a secondary follicle and do not use the term tertiary follicle.
- Primordial Follicle - Alternative nomenclature: small follicle or type 1, 2, 3 (25 cells) less than 50 micron diameter
- Preantral Follicle - Alternative nomenclature: preantral follicle or type 4 (26-100 cells), type 5 (101-300 cells) up to 200 micron diameter
- Antral Follicle - Alternative nomenclature: small antral type 6 (301-500 cells), large antral type 7 (501-1000 cells) small antral 500 micron diameter, large antral 1000-6000 micron diameter
- Preovulatory Follicle - Alternative nomenclature: largest antral follicle or Graafian follicle or type 8 (>1000 cells) greater than 6000 micron diameter
Atresia
At any one time the majority of follicles are destined not to complete maturation and at any stage (from type 4-7) degeneration of the follicle can occur, this process is called atresia.
Ovulation
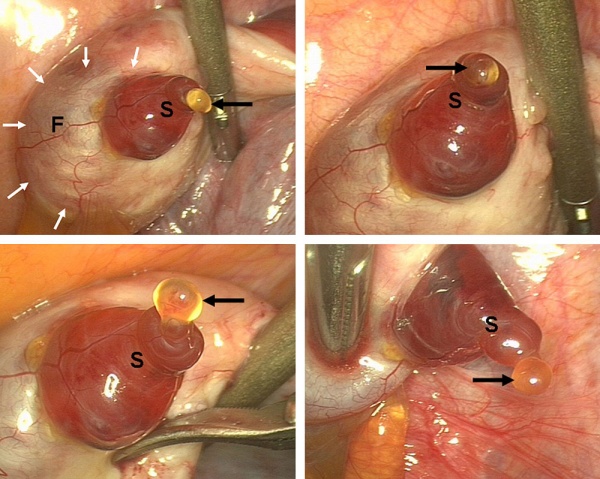
Human Ovulation
Movie (click image to play) showing process of ovulation (release of oocyte and follicular fluid). Click on movie to start.
Note that following ovulation the remnant of the follicle will degenerate if implantation does not occur (non-pregnant) forming a corpus albicans or following implantation (pregnancy) a corpus luteum which provides endocrine support to the uterus.
An endocrine signal (hCG human Chorionic Gonadotropin) from the implanting conceptus syncitiotrophoblasts maintains the corpus luteum, which in turn supports the uterine functional lining, preventing menstruation.
Fertilization
Fertilization is a complex interaction between the two haploid gametes (oocyte and spermatozoa) resulting in a single diploid cell (zygote). Following entry of the spermatazoa into the oocyte a series of changes occur within the oocyte and zona pellucida that block further fertilization by additional bound spermatozoa (polyspermy).
Due to both scientific and medical research on this process, this can now occur outside the body (in vitro fertilization) as well as fertility therapies to aid normal (in vivo fertilization). In addition, our understanding of fertilization has led to the development of a number of alternative fertility control methods.
Fertilization Dynamics
Sperm Events
- Capacitation - removal of glycoprotein coat and seminal proteins, alteration of sperm mitochondria
- Binding - ZP3 acts as receptor for sperm
- Acrosome reaction - exyocytosis of acrosome contents (Calcium ion mediated), enzymes to digest the zona pellucida, exposes sperm surface proteins to bind ZP2
- Membrane fusion - between sperm and egg, allows sperm nuclei passage into egg cytoplasm
Egg Events
- Sperm membrane fusion - causes depolarization of egg membrane, primary block to polyspermy
- Cortical reaction - IP3 pathway elevates intracellular Calcium, exocytosis of cortical granules, enzyme alters ZP3 so it will no longer bind sperm plasma membrane (cortical reaction)
- Second meiotic division - completion of 2nd meiotic division, forms second polar body
Sperm Penetration
The animation shows:
|
Pronuclear Fusion
|
The animation shows:
|
| In the mouse zygote, separation of chromatin according to parental origin is preserved up to the four-cell embryo stage and then gradually disappears. |
Fertilization Overview
Capacitation
- The mammalian spermatozoa once released, must remain for a time in the female genital tract before having the capacity to fertilize the oocyte. This process involves modifying the spermatozoa.
Acrosome Reaction
- Penetration of egg by spermatozoa is initiated by the acrosome reaction which takes different forms in different species.
- Mammalian acrosomal lysins contain proteinases which lyse the glycoproteins of the zona pellucida.
- The central part of the acrosome elongates into a tube which extends form the head of the spermatozoon. On contact with the egg the acrosomal membrane fuses with the sperm plasma membrane thus opening the acrosomal vesicle and liberating the granules containing acrosomal lysins.
- The inner portion of the acrosomal membrane everts and lengthens to form the acrosomal tubule through which the sperm nucleus enters the egg.
Sperm Contact
The act of fertilization changes the egg from a stage of slow structural and metabolic decline to one of renewed activation. Morphologically egg activation is a series of surface changes immediately following sperm contact.
- Mammals - No phenomenon comparable to the raising of the fertilization membrane is displayed. Mammalian eggs are surrounded by the zona pellucida which undergoes a structural change known as the zonal reaction after sperm penetration. On sperm contact with the egg plasma membrane, cortical granules break down as in above forms, substances liberated into the perivitelline space rapidly modify the zona pellucida resulting in a block to further sperm penetration.
Sperm Activation of Egg
- During fertilization sperm activates the egg by induction of a calcium ion (Ca2+) oscillation within the egg's cytoplasm.
- Induction occurs by a sperm protein factor (unidentified) which can stimulate only once calcium ion oscillations in metaphase eggs.
- Another sperm derived factor is then responsible for the inactivation of this oscillation.
- The activation of the egg by this calcium ion oscillation is essential for entry of the egg into the first mitotic cycle.
Zygote - Sperm Contribution
What the fertilizing sperm contributes in addition to the genetic material to the zygote differes between species.
- Centriole - most mammalian species, sperm contribute a centriole to reconstitute the zygotic centrosome. In rodents, only a maternal centrosomal inheritance occurs.
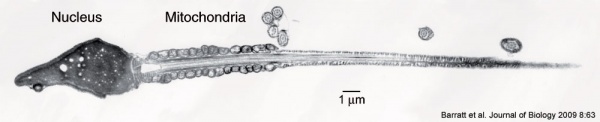
- Sperm Mitochondria - may enter the zygote, but are eliminated by a ubiquitin-dependent mechanism.
Perinuclear Theca - located in the sperm head perinuclear region. Contains a cytoskeletal element to maintain the shape of the sperm head and functional molecules leading to oocyte activation during fertilization.
Note - ART intracytoplasmic sperm injection techniques may introduce sperm components normally lost during in vivo fertilization.
Zona Pellucida
The specialized extracellular matrix layer lying directly around the oocyte underneath follicular cells. The structure consists of glcosaminoglycans and three main glycoproteins (ZP1, ZP2, ZP3).
After fertilization, the zona pellucida:
- blocks polyspermic fertilization
- physically protects the preimplantation embryo during early embryonic development (aided by an initial "hardening" after fertilization)
- aids uterine tube transport
- impacts upon blastocyst development
Zygote Contributions
Maternal - mitochondria, nucleolus, oocyte contributes one centriole during fertilization
Paternal - spermatozoon contributes one centriole during fertilization
Both Parents - chromosomes (inherent epigenetic differences between the paternal and maternal pronuclei), plasma membranes spermatozoon/oocyte mingle to form a mosaic plasma membrane
Links: Dev Biol - Fertilization | MBoC - Fertilization
Terms
- antral follicle - the stage following preantral in the decription of the sequence ovarian follicle development.
- antrum - (L. a cave), cavity; a nearly-closed cavity or bulge. In the ovary this refers to the follicular fluid-filled space within the follicle.
- atretic follicle - An ovarian follicle that fails to mature and degenerates. Also called "atresia" refering to the process of degeneration of the ovarian follicle. This process can occur at any stage of follicle development (folliculogenesis).
- clomiphene citrate - drug taken orally to promote the process of follicle/egg maturation.
- corona radiata - Layer of follicle cells of cumulus oophorus remaining attached to zona pellucida of oocyte after ovulation. Also called granulosa cells.
- corpus albicans - (L. corpus = body, L. albicans = whitish); a degenerating corpus luteum in ovary.
- corpus luteum - (L. corpus = body, L. luteum = yellow) The remains of ovarian follicle after ovulation that acts as an endocrine organ supporting pregnancy and preventing menstruation (loss of the endometrial lining). de Graaf first observed it in the ovary of a cow as a yellow structure.
- cortical - (L. corticalis) at the outside (like the bark of a tree), usually combined with medulla meaning the core.
- cumulus oophorus - (L. cumulus = a little mound G. oon = egg + phorus = bearing); part of the wall of an ovarian follicle surrounding and carrying the ovum (oocyte).
- follicle - (L. folliculus = little bag,dim. of L. follis). A structure which develops in the ovary and contains a developing egg (oocyte).
- follicular fluid - the fluid found in the antrum of a secondary follicle. Secreted by cells in the wall of the follicle. This fluid is released along with the oocyte at ovulation.
- germinal epithelium - cellular component covering surface of ovary, it is continuous with mesothelium covering mesovarium. Note that it is a historical misnomer, as it is not the actual site of germ cell formation.
- Graafian follicle - named after Regnier de Graaf (1641-1673), an historic Dutch physician embryologist who studied pregnancy using rabbits.
- granulosa cells - the supporting cells that surround the developing egg within the follicle thecal layers.
- mesovarium - mesentry of the ovary formed from a fold of the broad ligament that attaches the ovary
- medullary - (L. medius = in the middle) relating to the medulla; pith, marrow, inner portion of an organ. Usually combined with cortex (cortical) meaning the outer layer.
- oocyte - (Greek, oo = egg, ovum) The term used to describe the haploid egg or ovum formed within the ovary (female gonad) and released to enter the uterine tube and be transported to the uterus. The mature oocyte is the cell released from the ovary during ovulation.
- oocyte retrieval - (egg retrieval) A clinical in vitro fertilization (IVF) procedure to collect the eggs contained in the ovarian follicles.
- oogenesis - (Greek, oo = egg + genesis = origin, creation, generation) process of diploid oogonia division and differentiation into an haploid oocyte (egg) within the ovary (female gonad). Mammalian meiosis will only be completed within the oocyte if fertilization occurs.
- oogonia - (Greek, oo = egg) diploid germ cells within the ovary (female gonad) which provide the primary oocytes for oocyte (egg) formation. In humans, all oogonia form primary oocytes within the ovary before birth.
- oophorus - (Greek, oo = egg + phorus = carrying, egg-bearing) cumulus oophorus, used to describe the granulosa cells within the follicle that tether or link the oocyte to the wall of the follicle.
- ovulation - release of the oocyte from the mature follicle. In humans generally a single oocyte is released from a cohort of several maturing follicles.
- preantral follicle - the stage following primordial in the description of the sequence ovarian follicle development.
- primary follicle - the stage following primordial in the description of the sequence ovarian follicle development.
- primordial follicle - the first stage in the description of the sequence ovarian follicle development. Present in the ovary from birth, located in the stroma of the ovary cortex beneath the tunica albuginea. The primordial follicle is the oocyte and the surrounding follicular cells.
- primordial germ cell - oocyte present in the primordial follicle ovary from birth, located in the stroma of the ovary cortex beneath the tunica albuginea. The primordial follicle is the oocyte and the surrounding follicular cells.
- secondary follicles - the stage following primary in the description of the sequence ovarian follicle development.
- stromal cells - in the ovary, cells surrounding the developing follicle that form a connective tissue sheath (theca folliculi). This layer then differentiates into 2 layers (theca interna, theca externa). This region is richly vascularized and involved in hormone secretion.
- superovulation therapy - a fertility drug treatement (oral clomiphene citrate and/or injectable FSH with or without LH) aimed at stimulating development/release of more than one follicle during a single menstrual cycle.
- tertiary follicle - the stage following secondary in the description of the sequence ovarian follicle development.
- theca folliculi - stromal cells in the ovary, cells surrounding the developing follicle that form a connective tissue sheath. This layer then differentiates into 2 layers (theca interna, theca externa). This region is vascularized and involved in hormone secretion.
- theca externa - stromal cells forming the outer layer of the theca folliculi surrounding the developing follicle. Consisting of connective tissue cells, smooth muscle and collagen fibers.
- theca interna - stromal cells forming the inner layer of the theca folliculi surrounding the developing follicle. This vascularized layer of cells respond to LH (leutenizing hormone) synthesizing and secreting androgens which are processed into estrogen.
- tunica albuginea - dense connective tissue layer lying between germinal epithelium and cortical region of ovary.
- uterus - site of embryo implantation and development. Uterine wall has 3 major layers: endometrium, myometrium, and perimetrium. Endometrium can be further divided into the functional layer (shed/lost during menstruation) and basal layer (not lost during menstruation).
- zona pellucida - extracellular layer lying directly around the oocyte underneath follicular cells. Has an important role in egg development, fertilization and blastocyst development. This thick extracellular matrix consists of glcosaminoglycans and 3 glycoproteins (ZP1, ZP2, ZP3).
Online Course Site
- The site has a general introduction Help or http://embryology.med.unsw.edu.au/embryology/index.php?title=Help:Contents
- In addition there are pages with information on Help:Editing Basics
Exercise #1 - Online Work
- http://embryology.med.unsw.edu.au/embryology/index.php?title=ANAT2341_2011_Students
- Log in - student number/unipass
- Basic Editing - Formatting your ID, Making your own page, Lab attendance using the signature, copyright, online restrictions (no additional pages, uploads cannot be deleted, naming uploaded material).
Exercise #2 - Online exercise using the topic of "fertilization"
See also wiki editing sheet. Fertilisation/Fertilization (UK versus US spelling)
- Making a link.
- Pasting a picture (naming uploaded material).
- Making a table. (covered next week)
- Adding References. (covered next week)
- Resources - Searching the internet, identifying good sources, Medline (Pubmed), UNSW Library databases, referencing, journals copyright. (covered next week)
Individual Assessment
Tasks to be completed each week usually submitted online, or as written sheet for some guest tutors (20% of final course mark).
Group Assessment
This is a group project online work on a specific topic throughout semester (20% of final course mark). Assessment criteria will be listed online and discussed. Time will be made available within the labs for group discussions and some tutorials on techniques. Group project work should be completed and discussed mainly online and outside the timetabled laboratories. (Project Page / Discussion Page)
- Week 2 to 8 - project organisation, individual contributions, collaborative research and editing.
- Week 8 - project assessed online by individuals in other groups and providing both positive and negative feedback (part of individual assessment).
- Week 9 to 11 - update project on basis of peer assessments and own assessment.
- Week 12 - final submission date for the coordinator assessment. Project pages are locked.
- Each group will decide upon a specific topic from within the sub-list or of their own related choice.
- If 2 groups choose to do the same topic the course coordinator will allocate each group a different topic (not of their choosing).
Group Topics
The project should include the following basic components:
- Introduction (tell me about the topic)
- Historic background of topic (timeline, notable researchers or labs)
- Current associated research (new papers and findings)
- Simplified description of topic (related issues)
- Related genetic information (gene location, statistics)
- One student drawn figure or animation (well labeled)
- Reference List (formatted using the Pubmed reference link technique)
- Glossary (explanation of terms and acronyms used within your project)
- External Links (related online resources, labs, groups, news links etc)
Group Assessment Criteria
1. The key points relating to the topic that your group allocated are clearly described.
2. The choice of content, headings and sub-headings, diagrams, tables, graphs show a good understanding of the topic area.
3. Content is correctly cited and referenced.
4. The wiki has an element of teaching at a peer level using the student's own innovative diagrams, tables or figures and/or using interesting examples or explanations.
5. Evidence of significant research relating to basic and applied sciences that goes beyond the formal teaching activities.
6. Relates the topic and content of the Wiki entry to learning aims of embryology.
7. Clearly reflects on editing/feedback from group peers and articulates how the Wiki could be improved (or not) based on peer comments/feedback. Demonstrates an ability to review own work when criticised in an open edited wiki format. Reflects on what was learned from the process of editing a peer's wiki.
8. Evaluates own performance and that of group peers to give a rounded summary of this wiki process in terms of group effort and achievement.
9. The content of the wiki should demonstrate to the reader that your group has researched adequately on this topic and covered the key areas necessary to inform your peers in their learning.
10. Develops and edits the wiki entries in accordance with the above guidelines.
Co-ordinator Note
Dr Mark Hill |
ANAT2341 Embryology S2 2011
|
Course Content 2011
2011 Timetable: | Embryology Introduction | Fertilization | Cell Division/Fertilization | Week 1 and 2 Development | Week 3 Development | Week 1 to 3 | Mesoderm Development | Ectoderm, Early Neural, Neural Crest | Trilaminar Embryo to Early Embryo | Early Vascular Development | Placenta | Vascular and Placenta | Endoderm, Early Gastrointestinal | Respiratory Development | Endoderm and Respiratory | Head Development | Neural Crest Development | Head and Neural Crest | Musculoskeletal Development | Limb Development | Musculoskeletal | Renal Development | Genital | Kidney and Genital | Sensory | Stem Cells | Stem Cells | Endocrine Development | Endocrine | Heart | Integumentary Development | Heart and Integumentary | Fetal | Birth and Revision | Fetal
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 24) Embryology 2011 Lab 1. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/2011_Lab_1
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G