2011 Group Project 8
| Note - This page is an undergraduate science embryology student group project 2011. |
Friedreich’s Ataxia
2011 Projects: Turner Syndrome | DiGeorge Syndrome | Klinefelter's Syndrome | Huntington's Disease | Fragile X Syndrome | Tetralogy of Fallot | Angelman Syndrome | Friedreich's Ataxia | Williams-Beuren Syndrome | Duchenne Muscular Dystrolphy | Cleft Palate and Lip
Introduction
Friedreich’s Ataxia (FRDA) is an extremely debilitating progressive neurodegenerative disease. FRDA, an autosomal recessive disorder, is the most common of the inherited ataxias and affects an estimated 1 in 50000 people. [1] [2] Generally, FRDA is not diagnosed until the patient reaches their second decade of life, around the time of puberty, in which ataxic gait becomes noticeable. Progressive weakness is also noticeable due to loss of skeletal muscle, which can cause pateints to become wheelchair bound with in 10-15 years of onset of the disease. [2] The disruption of the frataxin gene is often caused by a trinucleotide repetition of GAA, which is located on chromosome 9q13. [1] The result of this gene is a mitochondrial protein, frataxin, which is known to play a role in iron homeostasis. [3] This causes major disabilities in the tissues containing the fraxtain deficient mitochondria, such as skeletal and cardiac muscle, as well as, the central and peripheral nervous systems. [4] The results of FRDA involve an increase chance of developing diabetes mellitus and premature death due to congestive cardiac failure and cardiac arrhythmia. [3] [5] [6]
History
Nikolaus (Nicholas) Friedreich (1825-1882) was born into a family of physicians and studied medicine at the University of Würzburg, Germany. Pathology and neurology were his main interests in medicine and in 1858 he became the director of medicine at the Heidelberg medical clinic. [2] [7] During his years at Heidelberg he became intrigued with the clinical presentation of some of his patients who he described as having “degenerative atrophy of the posterior columns of the spinal cord that could affect several children of unaffected parents”. [2] In 1863, Friedreich wrote his first journal article on his findings about six of his patients who belonged to two separate families. These patients presented with similar clinical signs and with his continued research Friedreich collated the symptoms of ataxic gait, sensory loss, dysarthria, skeletal muscle weakness, foot irregularities, scoliosis and cardiac abnormalities linking there cause to a common factor. [3] [7] Friedreich proceeded to write several articles on the disease, which now bares his name Friedreich’s Ataxia.
Timeline
| 1863 | 1882 | 1988 | 1996 |
| Friedreich describes the clinical presentation of patients and publishes his findings. [7] | Brousse suggests that many diseases have been mistaken for FRDA, such as Charcot-Marie-Tooth disease or syphilis, which calls for further investigation and classification techniques. [3] | The chromosomal locus for Friedreich’s ataxia was mapped to chromosome 9q13. [5] [7] | Frataxin the mutated gene responsible for FRDA was discovered, which allowed for molecular testing and full clinical classification of the disease. [2] [5] |
Epidemiology
Distribution - FRDA is the most common form of inherited ataxic disease, affecting an estimated 1 in 50,000 people. [3] [1] [2]
- Populations - It has been noted that Caucasian populations have a higher prevalence of FRDA with approximate carrier frequencies varying between 1:50 to 1:100. [8] Furthermore, Asian and African populations have a much lower prevalence of FDRA. [8] [3]
- Gender - There has been no gender differentiation at this point in time, therefore, males and females have the same chance of inheriting FRDA.
- Age - Onset of FRDA is relatively early in life with symptoms normally appearing between 5-15 years of age, typically, patients are diagnosed before the age of 20. [9] [10] There are cases of late onset FRDA in which symptoms begin to show around 28 ± 13 years of age, remarkably these patients are less affect by cardiac dysfunction but are most likely to fall ill to neurological disability. [11] Furthermore, there has been known cases of very late onset FRDA but these cases are fairly uncommon and occur beyond the age of 40. [12]
Morbidity & Mortality FRDA is a progressive disease causing 95% patients to become wheelchair-bound by approximately 45 years of age. [10] Commonly, patients tend to lose the capability to walk nearing the age of 25. [10] Death of FRDA patients is principally triggered by cardiac dysfunction. In a study performed by Tsou et al, (2011) [9] 59% of patients died due to cardiac dysfunction, such as congestive heart failure and arrhythmia. 27.9% of patients died due to non-cardiac dysfunction, including pneumonia, sepsis and renal failure and the remaining patients died of unknown causes. [9] Death of FRDA patients remains quite young with the age of passing around 37.7 years of age ±14.4 years with patients suffering from cardiac dysfunction dying at an earlier age. [10] [9]
Aetiology
Genetic Component
Inheritance
Genetic Expression
Pathogenesis
As FA is a ‘neurodegenerative disorder’ patients with FA are normal at birth until the ‘age of onset’ where symptoms present[13] due to (what is believed to be) iron build up in mitochondria. Studies on mouse models show that if the frataxin gene is totally knocked out, the embryo does not survive[14].
Cardiomyopathy
In the past, the pathogenesis of cardiomyopathy in FA patients was relatively unknown[15], however it is now believed that the buildup of iron in mitochondria within cardiac muscle is part of the pathogenesis in cardiomyopathy of FA patients[16]. The iron build up results in what is described as ‘Fenton Chemistry’ where the excessive amounts of iron that are recruited into the mitochondria will produce a lot of HO˙. The production of HO˙ is of concern as it is a hydroxyl radical which is toxic to cells and it reacts to a variety of intracellular components including DNA[3].
Pathophysiology
Clinical Presentation
Symptoms
Friedreich's Ataxia (FA) often manifests before puberty to early adulthood. Physical complaints such as chest pains [17] [18], progressive gait and limb ataxia, absent lower limb reflexes, extensor plantar responses (Babinski's sign), dysarthria, reduction in or loss of vibration sense and proprioception [19], [20]. scoliosis, foot deformity (pes cavus, hammer toe) and cardiomyopathy are common but not symptoms which FA is often diagnosed by[19].
Complications
Cardiomyopathy
Diabetes
Diabetes as a complication of FA is fairly straight forward with a clear reason as to why it occurs. In mouse models of FA, when the frataxin gene is disrupted the overall volume of beta-cells is reduced due to cell apoptosis, loss of beta-cell proliferation and increased Reactive Oxygen Speices (ROS)in islets[21].
Diagnosis
Friedreich's Ataxia (FA) is often diagnosed based on presenting clinical symptoms but testing for the gene defect that causes it is taken as a definitive diagnosis.
| Availability of genetic testing | Diagnostic symptoms |
| Prior to genetic testing availability | Only physical signs(eg: Scoliosis) and symptoms(eg: chest pains), age of onset and typical FA progression could identify it as FA. [20] |
| After genetic testing is available | Physical complaints are used in conjunction with genetic testing to confirm FA. Due to genetic testing, [13]it has been discovered that FA can occur in individuals older than the typical diagnostic age (first two decades of life[22]). |
A paper on cardiac evaluation of Friedreich's Ataxia patients found that cardiac evaluation was a useful tool to compliment genetic testing in terms for screening for patients who should be tested for Friedreich's Ataxia[23]
Treatment
As cardiomyopathy is believed to be caused by the production of toxic agents from the excess iron reacting within mitochondria, Iron-chelation had been studied for it's therapeutic action on removing excess iron on mouse models. Between treated mice and untreated mice, the treated mice showed a decrease in heart weight and heart to body ratio. This shows that chelation limits cardiomyopathy but it did not 'cure' the problem. While chelation did not lead to major iron depletion or toxicity reduction, it did prevent iron accumulation in mice with the mutated frataxin gene. This discovery is significant as it has opened up a possible treatment path of preventing mitochondrial iron build up - stopping the production of toxic agents and free radicals before they can be produced. Mice treated with chelation did not show any changes in the histology of the heart or any other major organ. It also did not lead to red blood cell loss, decreased hemoglobin concentration or hematocrit[24].
Alternative treatment of Friedreich ataxia (FA) is the use of Idebenone. Idebenone a new emerging treatment of FA reverses redox reactions, influencing the mitochondria electron balance preventing damage to the mitochondrial membrane [25]. Usage of Idebenone has been proven to reduce cardiac hypertrophy in FA indicating a 20% reduction on left ventricular mass from cardiac ultrasound in half the patients during trial[26], though the dosage of Idebenone give is at low dosage treatments of 5mg/kg/day which has shown reduction in cardiac hypertrophy[27]. Thus Idebenone has been strongly used a treatment method although other alternative are present including erythropoietin, histone deacetylase inhibitors and other gene-based strategies[28].
Genetic Screening
Current Research
References
- ↑ 1.0 1.1 1.2 <pubmed>11351269 </pubmed> Cite error: Invalid
<ref>tag; name 'PMID11351269' defined multiple times with different content - ↑ 2.0 2.1 2.2 2.3 2.4 2.5 <pubmed>19283344</pubmed>
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 <pubmed>10633128</pubmed>
- ↑ <pubmed>12547248</pubmed>
- ↑ 5.0 5.1 5.2 <pubmed>10607838</pubmed>
- ↑ <pubmed>5673214</pubmed>
- ↑ 7.0 7.1 7.2 7.3 <pubmed>15090560</pubmed>
- ↑ 8.0 8.1 <pubmed>21315377</pubmed>
- ↑ 9.0 9.1 9.2 9.3 <pubmed>21652007</pubmed>
- ↑ 10.0 10.1 10.2 10.3 <pubmed>7272714</pubmed>
- ↑ <pubmed>21128039</pubmed>
- ↑ <pubmed>16092110</pubmed>
- ↑ 13.0 13.1 <pubmed>21315377</pubmed>
- ↑ <pubmed>10767347</pubmed>
- ↑ <pubmed>3593615</pubmed>
- ↑ <pubmed>18621680</pubmed>
- ↑ <pubmed>7488466</pubmed>
- ↑ <pubmed>3593615</pubmed>
- ↑ 19.0 19.1 <pubmed>10633128</pubmed>
- ↑ 20.0 20.1 <pubmed>13872187</pubmed>
- ↑ <pubmed>12925693</pubmed>
- ↑ <pubmed>19283344</pubmed>
- ↑ <pubmed>12045843</pubmed>
- ↑ <pubmed>18621680</pubmed>
- ↑ <pubmed>19283347</pubmed>
- ↑ <pubmed>11907009</pubmed>
- ↑ <pubmed>19363628</pubmed>
- ↑ <pubmed>20856912</pubmed>
External Links
Video Showing Ataxic Gait [1]
Glossary
Apoptosis - Programmed cell death.
Ataxic Gait - Involves a wide-based stance, lack of muscle coordination, errors in range and force of movement, delay in initiating movement.
Cardiac Arrhythmia - Abnormal rate or beat of the heart, which can be either fast (tachycardia) or slow (bradycardia).
Chelation - chemicals that form soluble, complex molecules with certain metal ions, inactivating the ions so that they cannot normally react with other elements or ions... (ASTM)
Dysarthria -Slurring of speech.
FRDA - Friedreich's Ataxia.
Hematocrit - Measures the volume of red blood cells in blood.
Pes cavus - Feet with abnormally high arches.
Pneumonia - Inflammatory condition of the lungs.
Proprioception - Refers to the ability of sensing movement and position of muscles without visual guides. Required for hand-eye co-ordination.
Reactive Oxygen Speices (ROS) - It is a classification for chemically-reactive molecules containing oxygen.
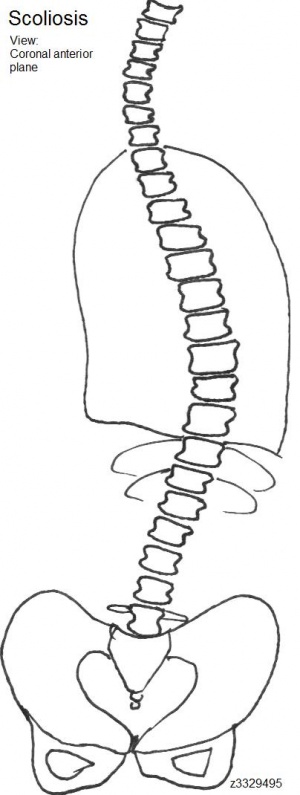
Scoliosis - Abnormal curving of the spine in the Coronal plane to form an 'S-shpe' when viewed from the front.
Sepsis - Infection of the blood, generally bacterial.