2011 Group Project 8: Difference between revisions
| Line 396: | Line 396: | ||
Currently For the degenerative congenital disorder Friedreichs Ataxia (FRDA) this is no current treatment to reverse, prevent and delay <ref name="PMID:19283349"><pubmed>19283349</pubmed></ref> FRDA. However there are various potential treatments which have shown signs of improvement from FRDA patients include, Iron chelation, Histone deacetylase inhibitors(HDACI) and antioxidant are the leading treatments towards FRDA<ref name="PMID:19283350"><pubmed>19283350</pubmed></ref><ref name="PMID:19283347"><pubmed>19283347</pubmed></ref><ref name="PMID:17968974"><pubmed>17968974</pubmed></ref>. | Currently For the degenerative congenital disorder Friedreichs Ataxia (FRDA) this is no current treatment to reverse, prevent and delay <ref name="PMID:19283349"><pubmed>19283349</pubmed></ref> [[#Glossary | '''FRDA''']]. However there are various potential treatments which have shown signs of improvement from FRDA patients include, Iron chelation, Histone deacetylase inhibitors(HDACI) and antioxidant are the leading treatments towards [[#Glossary | '''FRDA''']]<ref name="PMID:19283350"><pubmed>19283350</pubmed></ref><ref name="PMID:19283347"><pubmed>19283347</pubmed></ref><ref name="PMID:17968974"><pubmed>17968974</pubmed></ref>. | ||
'''Iron-chelation''' | '''Iron-chelation''' | ||
Iron [[#Glossary | '''chelations''']] potential as treatment for Friedrichs Ataxia (FRDA) is greatly focused. Within areas regarding to pathogenesis. FRDA effects Mitochondria leading to Mitochondrial accumulation of Iron, causing a usage of cytosolic iron<ref name="PMID:10805340"><pubmed>10805340</pubmed></ref>.There is evidence that due to the fractin deficiency resulted in FRDA patients is from the depletion of cytosolic iron, it has been suggested therapeutic treatment of iron supplements to replenish cytosolic iron to normal range<ref name="PMID:18424449"><pubmed>18424449</pubmed></ref> to counter the rate of depletion.Where most potential [[#Glossary | '''chelators''']] are those which specifically target mitochondrial pools of iron<ref name="PMID:20156111"><pubmed>20156111</pubmed></ref> for the reason of maintenance of Iron within cystol of the cell. | Iron [[#Glossary | '''chelations''']] potential as treatment for Friedrichs Ataxia (FRDA) is greatly focused. Within areas regarding to pathogenesis. FRDA effects Mitochondria leading to Mitochondrial accumulation of Iron, causing a usage of cytosolic iron<ref name="PMID:10805340"><pubmed>10805340</pubmed></ref>.There is evidence that due to the fractin deficiency resulted in FRDA patients is from the depletion of cytosolic iron, it has been suggested therapeutic treatment of iron supplements to replenish cytosolic iron to normal range<ref name="PMID:18424449"><pubmed>18424449</pubmed></ref> to counter the rate of depletion.Where most potential [[#Glossary | '''chelators''']] are those which specifically target mitochondrial pools of iron<ref name="PMID:20156111"><pubmed>20156111</pubmed></ref> for the reason of maintenance of Iron within cystol of the cell. | ||
Revision as of 23:09, 29 September 2011
| Note - This page is an undergraduate science embryology student group project 2011. |
Friedreich’s Ataxia
--Mark Hill 13:40, 8 September 2011 (EST) A well-structured project in terms of sub-headings. Student drag image included on project page. The problem, like all other projects, is a lack of section illustrations and figures. It currently just looks like a lot of writing, with each section slightly differently formatted.
- Timeline - would look better vertical rather than horizontal.
- Epidemiology - numbering should be either bullets or not at all. 1-3 and the separately Morbidity & Mortality?
- Clinical Presentation - too many sub-sub headings, rationalise structure.
- Postnatal Diagnosis - table formatting should be fixed.
- Treatment - the text is poorly written/structured, go through this and organise to make sense.
- Current Research - no text, a simple PubMed search would show you what is going on now.
- Glossary - does not include all terms and acronyms used in the project.
Introduction
Friedreich’s Ataxia (FRDA) is an extremely debilitating progressive neurodegenerative disease. FRDA, an autosomal recessive disorder, is the most common of the inherited ataxias and affects an estimated 1 in 50,000 people. [1] [2] Patients suffering from FRDA have a normal presentation at birth and for a period of time thereafter. When the patient reaches the age of onset, which is approximately around the time of puberty the clinical phenotypes become noticable, such as ataxic gait. [3] Progressive weakness is also noticeable due to loss of skeletal muscle, which can cause pateints to become wheelchair bound with in 10-15 years of onset of the disease. [2]
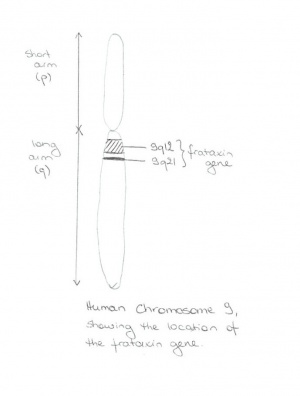
FRDA is caused by a mutation in the frataxin gene. The disruption of the frataxin gene is often caused by a trinucleotide repeat expansion of GAA, which is located on chromosome 9q13. [1] The product of this gene is a mitochondrial protein, frataxin, which is known to play a role in iron homeostasis. [4] This causes major disabilities in the tissues containing the frataxin deficient mitochondria, such as skeletal and cardiac muscle, as well as, the central and peripheral nervous systems. [5]
The results of FRDA involve an increase chance of developing diabetes mellitus and premature death due to congestive cardiac failure and cardiac arrhythmia. [4] [6] [7]
History
Nikolaus (Nicholas) Friedreich (1825-1882) was born into a family of physicians and studied medicine at the University of Würzburg, Germany. Pathology and neurology were his main interests in medicine and in 1858 he became the director of medicine at the Heidelberg medical clinic. [2] [8] During his years at Heidelberg he became intrigued with the clinical presentation of some of his patients who he described as having “degenerative atrophy of the posterior columns of the spinal cord that could affect several children of unaffected parents”. [2]
In 1863, Friedreich wrote his first journal article on his findings about six of his patients who belonged to two separate families. These patients presented with similar clinical signs and with his continued research Friedreich collated the symptoms of ataxic gait, sensory loss, dysarthria, skeletal muscle weakness, foot irregularities, scoliosis and cardiac abnormalities linking there cause to a common factor. [4] [8] Friedreich proceeded to write several articles on the disease, which now bares his name Friedreich’s Ataxia.
Timeline
| Date | Significance | |
| 1863 | Friedreich describes the clinical presentation of patients and publishes his findings. [8] | |
| 1882 | Brousse et al suggests that many diseases have been mistaken for FRDA, such as Charcot-Marie-Tooth disease or syphilis, which called for further investigation and classification techniques for FRDA [4] | |
| 1907 | A study by Mott et al gave the first detailed description of the dentate nucleus and the role it plays in FRDA pathology. [3] | |
| 1976 | The Québec Collaborative Group proposed a systematic way of classifying and diagnosing FRDA, such as the absence of tendon reflexes. [9] | |
| 1980 | FRDA patients were found to have iron-positive granules deposited within cardiomyocytes, as well as, skeletal muscle fibres. [10] | |
| 1988 | The chromosomal locus for FRDA was mapped to chromosome 9q13. [6] [8] | |
| 1989 | Wallis et al developed the first prenatal diagnostic test for FRDA via DNA markers. [11] | |
| 1990 | Two closer DNA markers were establish by Hanauer et al improving prenatal test to almost 99%. [12] | |
| 1995 | Monros et al refined prenatal testing in regards to new recombination techniques available with an accuracy close to 100%. [13] | |
| 1996 | Frataxin, the mutated gene responsible for FRDA, was discovered by Campuzano et al, which allowed for molecular testing and full clinical classification of the disease. [2] [6] | |
| 1997 | Rötig et al reported on the defective activity of the iron-sulphur clusters in FRDA patients, in relation to mitochondrial respiratory complexes I, II and III via a yeast homologue. They also discovered the protein aconitase to also be deficient with in patients, thus suggesting that iron accumulation is a key component in FRDA pathogenesis. [14] | |
| Whilst researching the GAA trinucleotide repeat expansion Cossée et al uncovered that nearly 17% of expansions consisted of repeats longer than 16 GAA. [15] | ||
| 2002 | Mühlenhoff et al demonstrated, via a yeast frataxin homologue (YFH1), that the decreased maturation of iron-sulphur proteins and accumulation of mitochondrial iron are critical factors in oxidative stress in FRDA. [16] | |
| Current | Research is looking into treatments for FRDA and Idebnone, which may reverse the redox reaction associated with FRDA looks very promising. [17] |
Epidemiology
Distribution
FRDA is the most common form of inherited ataxic disease, affecting an estimated 1 in 50,000 people. [4] [1] [2]
Populations
It has been noted that FRDA has a range of prevalence’s in accordance to the country of interest. Caucasian populations have a higher prevalence of FRDA with approximate carrier frequencies varying between 1:50 to 1:100. [3] This includes Australia, the United States of America and similar European countries, which have the aforementioned prevalence of 1 in 50,000. [18] FRDA also has a high prevalence in North Africa, the Middle East and India.
Studies performed in Italy revealed an extremely high birth incidence of FRDA with the disease affecting 4.9 in every 50,000 live births. [19]
Some Southern and Central American countries, such as Cuba, have a much lower prevalence of FRDA approximately 1 in 2,200,00 in addition to lower carrier frequencies of 1:745. [20] Furthermore, Asian, sub-Saharan African and Amerindian populations have a much lower prevalence or the FDRA genetic mutation is non existent. [3] [4] [19]
Gender
There has been no gender differentiation at this point in time, therefore, males and females have the same chance of inheriting FRDA. [3]
Age
Onset of FRDA is relatively early in life with symptoms normally appearing between 5-15 years of age, typically, patients are diagnosed before the age of 20. [21] [22] There are cases of late onset FRDA in which symptoms begin to show around 28 ± 13 years of age, remarkably these patients are less affect by cardiac dysfunction but are most likely to fall ill to neurological disability. [23] Furthermore, there have been known cases of very late onset FRDA but these cases are fairly uncommon and occur beyond the age of 40. [24]
Morbidity & Mortality
FRDA is a progressive disease causing 95% patients to become wheelchair-bound by approximately 45 years of age. [22] Commonly, patients tend to lose the capability to walk nearing the age of 25. [22] Death of FRDA patients is principally triggered by cardiac dysfunction. In a study performed by Tsou et al, (2011) [21] 59% of patients died due to cardiac dysfunction, such as congestive cardiac failure and arrhythmia. 27.9% of patients died due to non-cardiac dysfunction, including pneumonia, sepsis and renal failure and the remaining patients died of unknown causes. [21] Death of FRDA patients remains quite young with the age of passing around 37.7 years of age ±14.4 years with patients suffering from cardiac dysfunction dying at an earlier age. [22] [21]
Aetiology
Genetic Component
The frataxin gene is located on the proximal long arm of chromosome 9. Its location was identified for the first time by Chamberlain et al (1988) [25], using a linkage study for the mapping. Subsequent studies further refined the location to 9q13-q21 [15].
The most common mutation leading to the FRDA phenotype is an expansion of the GAA triplet repeat in the first intron of the frataxin gene. Repeats up to approximatively 40 are normal, and manifestations of the disease start at 70 repeats. The repeat number can reach up to 1700, and the most common number of repeats in FRDA patients is between 600-900[26] [15]. The mutation is recessive, thus heterozygous carriers of the repeat are clinically normal. Most FRDA patients are homozygous for a repeat expansion, although there are some rare cases of heterozygous patients who have a repeat expansion on one allele and a missense or nonsense point mutation on the other allele. [27]
Evolution
FRDA is the most common repeat-expansion caused disease, with as many as 1 in 90 carriers in the European population. While repeats up to 40 do not show any clinical manifestations, most normal repeats are smaller, consisting of only 8-9 repeats. In a study investigating the evolution of the repeat expansion, Cossée et al (1997) [15] found that only approximately 17% of clinically normal repeats consist of repeats longer than 16. The comparatively high prelevance of FRDA in European populations compared to other populations has been suggested to be the result of a founder event. The presence of long repeat alleles without clinical manifestations served as a pool for further length variations, including transitions to pathological repeat expansions. In same cases, this transition has been achieved within one single generation. [15]
Genetic Instability
Several other disorders, including Fragile X Syndrome, Huntington's Disease as well as other ataxias, are caused by repeat expansions, suggesting the possibility of a common underlying mechanism. Indeed, repeat regions, especially trinucleotide repeats, are generally unstable structures and can undergo additions or deletions of the repeated unit [28]. The cause for this instability is replication slippage: during DNA replication, one strand of the DNA template may loop out and become displaced, alternatively, DNA polymerase might slip or stutter. Both of these scenarios lead to either replication of already replicated sequences when the DNA polymerase rebinds to the template, which thus leads to expansions, or alternatively, DNA polymerase might rebind further down the strand, thus failing to replicate part of the sequence, leading to deletions. Replication slippage is a lot more common in repeat regions, and furthermore, the longer the repeat, the more likely slippage is to occur. (For further detail on the mechanisms of replication slippage, see Viguera et al (2001) [28].) This observation explains why a pathological repeat expansion can be achieved within very few generations if the parental alleles are longer variants of the normal repeat length. This further explains the anticipating pattern of inheritance in families with the disease, further discussed in the Inheritance section.
Inheritance
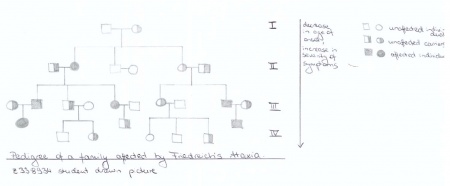
Friedreich's Ataxia is a recessive disease, meaning that an individual needs to carry two copies of the mutated frataxin allele to manifest the disease. As already mentionned, a normal long repeat can lead to a pathologically long expansion within only one generation. Thus a person can inherit a disease allele from a parent carrying two normal alleles. Alternatively, an individual may inherit a pathological allele from both parents who could be heterozygous, healthy carriers. Due to the length of the repeat making it more unstable and likely to expand further as well as the correlation between repeat length and the severity of symptoms, FRDA presents an anticipating pattern of inheritance. Over the course of a few generations in an affected family, the age of onset of the disease decreases while the severity of symptoms increases.
Genetic Expression
The frataxin gene is expressed in all cells, though the expression levels vary between different tissues and at different times during development.
In adult cells, frataxin levels are highest in the heart, brain and spinal cord, followed by the liver, skeletal muscle and the pancreas. Generally, the frataxin levels are higher in cells that are abundant in mitochondria, such as cardiomyocytes and neurons [26]. Nevertheless, some cell specificity, such as primary sensory neurons, still remains unexplained.
Developmental expression has been investigated in mouse embroys [29], and it was found that frataxin is expressed during embryonic development, though generally at a lower level than postnatally. The highest prenatal level of expression was found in the spinal cord, followed by the periventricular zone, the cortical plates and the heart. This distribution is in concordance with the distribution observed in adults, the only exception being expression in the cerebral cortex, which has not been manifested in adults. Overall, it seems that the tissues expressing frataxin during embryonic development are the ones that become dysfunctional in adults suffering from FRDA. Further studies on mouse models have shown that if the frataxin gene is completely knocked out, the embryo does not survive, indicating that the frataxin gene is needed for early development[30].
Silencing of the frataxin gene (consequences of the mutation)
In a study investigating the consequences of the repeat expansion for DNA transcription, Bidichandani et al (1998) [31] found that splicing of the expanded intron is not affected, and thus is not the cause for abnormal frataxin protein. Instead, they showed that mRNA levels of frataxin are very low in FRDA patients, speaking for ineffective transcription. Indeed, they showed in further experiments that the GAA triplet expansion interferes with transcription. This interference is length dependent, and here a threshold of 79 GAA repeats was found before interference occurs. Furthermore, the interference is orientation specific, it only occurs during the synthesis of the GAA transcript which is the physiological direction of transcription, and not in the complementary strand transcript. The reason for this interference is assumed to be the formation of unusual DNA structures. Both G (guanine) and A (adenine) are purines while T (thymine) and C (cytosine) are pyrimidines. Thus a GAA repeat leads to a strand of pure purines binding to a complementary strand of pure pyrimidines. Such structures have been found to form unusual DNA structures, and it is assumed that this is also the case in the GAA repeat in the frataxin gene. These unusual structures are also present in the shorter GAA repeats which don't lead to transcription interference, and it is thought that a longer repeat stabilises the unusual structure. It is thought that these unusual structures interfere with the transcription, thus making longer repeats more stable and more efficient in the transcription blockage, which leads to gene silencing. This would account for the negative correlation between repeat length and frataxin mRNA levels as well as frataxin levels as such. [31] More recent studies are looking at whether the elongation and/or the initiation of transcription are affected. While it is generally accepted that there are problems with the elongation in repeat expansions, some have found evidence for inhibited initiation, though this is still a matter of debate. [32] [33]
In the rare cases of heterozygous individuals with a repeat expansion and a point mutation, the point mutation most often leads to either a shortened or abnormal frataxin protein, which is unfunctional. [27]
The protein frataxin is a mitochondrial protein which is thought to be involved in mitochondrial iron metabolism. It is the deficiency in frataxin which leads to the clinical manifestations of FRDA.
Pathogenesis
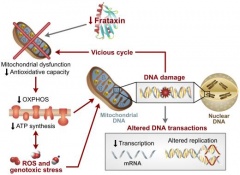
As FRDA is a ‘neurodegenerative disorder’ patients with FRDA are normal at birth until the ‘age of onset’ where symptoms present[34] due to (what is believed to be) iron build up in mitochondria. In humans, the GAA repeat expansion on the frataxin gene causes a transcription defect on the gene impairing it's ability to produce frataxin (a mitochondrial protein). Cardiomyopathy is caused by build up of iron in mitochondria producing excessive amounts of free radicals and anti-oxidants which damages cells. As Frataxin is most expressed in the heart, skeletal muscles, (as well as liver and pancreas)and nervous system [35], it impacts most significantly on the nervous system followed by musculature and cardiac muscles. For more information on nervous systems impacts see Neuropathology.
Cardiomyopathy
In the past, the pathogenesis of cardiomyopathy in FRDA patients was relatively unknown[36], however it is now believed that the buildup of iron in mitochondria within cardiac muscle is part of the pathogenesis in cardiomyopathy of FRDA patients[37]. The iron build up results in what is described as ‘Fenton Chemistry’ where the excessive amounts of iron that are recruited into the mitochondria will produce a large quantity of HO˙. The production of HO˙ is of concern as it is a hydroxyl radical which is toxic to cells and it reacts to a variety of intracellular components including DNA[4]. The length of the GAA repeat on the frataxin gene also has an impact on the pathogenesis of cardiomyopathy as it was discovered that the degree of ventricular hypertrophy is related to the length of the GAA repeat [38]. Patients with no signs of cardiomyopathy and late onset of symptoms have also been reported having shorter GAA repeats [39] [40].
Neuropathology
FRDA produces a complex neuropathological phenotype within the central nervous system (CNS), as well as, the peripheral nervous system (PNS) and it is the neuropathology that differentiates this disease from other forms of hereditary ataxia. FRDA patients present with distinctive lesions of dorsal root ganglia DRG, dorsal spinal roots, dorsal nuclei of Clarke, spinocerebellar and corticospinal tracts, cerebellum, dentate nuclei, and sensory nerves. [41]
FRDA patients have consistent lesions in the DRG, which trigger secondary degeneration of the fibers in the spinocerebellar tracts and atrophy of the neurons in the dorsal nuclei Clarke. Less consistent among FRDA patients are lesions occurring in the dentate nucleus, in addition to optic atrophy, and degeneration of the corticospinal tract.
The Dorsal Root Ganglia
The hallmark of FRDA involves atrophy of DRG and thinning of dorsal roots themselves within the PNS, refer to the figure of the Cross Section of the Spinal Cord. [42] The lesions of the large primary neurons in the DRG are an early clinical finding in the disease with neuropathological examinations of FRDA patients showing a decreased size of DRG along with grey staining of the thinned dorsal roots . [43] [2] Iron dysfunction, caused by mutation of the frataxin gene, highly affects the DRG causing a common characteristic of the disease, which includes demyelination and unsuitable regeneration of myelin of the dorsal root. [42] [44]
The study by Mott et al, (1907) [2] highlighted the importance of the DRG, in which Friedreich himself did not seem to think played any role in this disease. It has been suggested that DRG pathology involves an age determined buildup of the GAA triplet repeat sequence “…thus, somatic instability of the expanded GAA triplet-repeat sequence may contribute directly to disease pathogenesis and progression.” [45] Furthermore, the experiment conducted by Lu et al, (2009) [44] measured the significance of frataxin depletion in Schwann cell and oligodendrocyte cell lines. Results showed that mainly Schwann cell succumbed to cell death and reduced proliferation. This highlights that the Schwann cells, which enwrap DRG are affected greatly by frataxin deficiency. [44]
When abnormalities arise in Schwann cell, due to injury or genetics, they can cause demyelination, inappropriate proliferating and phagocytosis of debris. [46] The understanding of the pathological change within the peripheral nervous system is poorly understood, however, the damaged DRG seems be the basis of FRDA. [43]
Damage and/or loss of the neurons of DRG are seen to be the primary manifestations of FRDA many secondary affects stem from this area, such as;
- The depletion of the centrally projecting axons of the DRG into the dorsal root. [2]
- The loss of axons in the dorsal root explains the depletion of the dorsal column fibers and “…afferent connections to the dorsal nuclei of Clarke and the grey matter of the dorsal horns.” [2]
The Dorsal Nuclei of Clarke
The dorsal nuclei of Clarke are mainly found in the thoracic region of the spinal cord. These nuclei function to relay proprioceptive information from the lower extremities to the spinocerebellar tract. The information this nucleus receives arises from muscle spindles and Golgi tendon organs. Within the spinal cord the nuclei can be located in the intermediate grey matter, refer to the figure of the Cross Section of the Spinal Cord. It is within the grey matter that the dorsal nuclei of Clarke form synapses with the dorsal spinocerebellar tract, which will continue transmitting the sensory information in a rostral direction until it reaches the spinocerebellum.
When FRDA abnormalities occur in this area it will assist in proprioceptive sensory loss, of mainly the lower extremities. This would contribute to clumsiness and unexplained falls before FRDA patients are wheel chair bound. [3]
The Spinocerebellar Tract
This spinal pathways is involved in passing sensory information from the spinal cord to the brain and/or cerebellum. The function of this tract is to carry proprioceptive information to the cerebellum, which allows the integration of sensory information with movement. The spinocerebellum is the only area of the cerebellum that receives peripheral sensory input. Specifically, this tract aids in ongoing control of voluntary movement, motor control, locomotion, posture and ongoing execution via its connection to the spinocerebellum.
Notably, the lesions tend to occur in the dorsal spinocerebellar tract and are said to be secondary to DRG lesions. [2] Post mortem examination of patients suffering from FRDA are indicative of a small, atrophied spinal cord with degeneration in the dorsal columns, spinocerebellar and corticospinal tracts. [47]
Pathogenesis of the spinocerebellar tract includes axonal degeneration, which is characterized by demyelination of the myelin sheath encapsulating the axon, which normally allows for rapid propagation of electrical impulses. Followed by degeneration of the underlying axon, which will in turn disrupt the function of the spinocerebellum itself causing symptoms, such as:
- “…loss of spinocerebellar input to the cerebellar hemispheres due to transneuronal atrophy of the dorsal nuclei of Clarke.” [48]
- Hypotonia is the loss of muscle tone, which is variable between the upper and lower extremities, with muscle tone being usually normal in the arms but the tone of the legs, can differ. [3]
- Loss of position and vibration sense, which leads into dysmetria [2]
- Ataxia gait
- Intention tremor nearing target
- Hyperreflexia in the lower extremities is common among patients, in which there is unrestricted flow of excitation to the motoneurons causing spastic movements
- Decreased or abolished tendon reflexes along with sensory deprivation in corresponding dermatome, [2]
- Diminished ability to perceive touch, light, temperature and pain, which is more prominent in the lower extremities
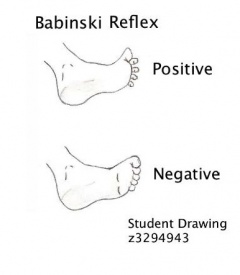
- Positive Babinski reflex (extensor plantar responses) and muscle weakness.
The Cerebellum
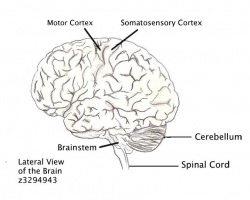
The cerebellum (Latin for “little brain”) is a small structure that creates the hindbrain and is enclosed by the occipital bone, refer to the figure of the Lateral View of the Brain. The cerebellum contains more than 50% of the brains neurons but only takes up 10% of the human brains total volume. This densely packed structure is involved in:
- Adjusting the outputs of the descending motor pathways, as it receives massive input from the motor cortex in the brain, as well as sensory receptors.
- Regulatory functions in movement and posture, which allows the cerebellum to compare and evaluate motor/sensory discrepancies, which provide corrective responses.
- Producing projections into the descending motor pathways.
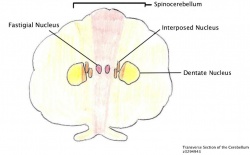
The three functional nuclei of the cerebellum, namely the dentate, interposed and fastigial all play a central role in relaying information between the cortex and other brain structures, refer to the figure of the Transverse Section of the Cerebellum. [47] In FRDA the degeneration of cerebellum appears late in the course of the disease becoming apparent upon neurological examination when Purkinje fibre depletion can be seen and atrophy of the dentate nuclei is observable. [43]
The Dentate Nucleus
Out of the three nuclei of the cerebellum the dentate nucleus undergoes considerable atrophy and has been said to be the most likely cause of the symptoms dysmetria, dysarthria, dysphagia. [48] The dentate nucleus has axonal “…projections into the motor, premotor, oculomotor, prefrontal and posterior parietal cortex,” [47] thus with degeneration at the dentate nucleus can cause secondary abnormalities at the aforementioned areas.
Frataxin deficiency causes iron accumulation with in the mitochondria, which in turn cases oxidative damage. This may be responsible for the neuronal loss but further research is needed in this area before any definitive answers can be given.
The cerebellum connects to the brainstem via the superior, middle and inferior peduncles. Upon post mortem dissection many FRDA patient’s display degeneration of the superior peduncles; this is where the efferent fibres of the dentate nucleus can be located. Interestingly, only large neuronal cells of this nucleus undergo atrophy, which highlights the selective nature of FRDA and the small neurons remain unaffected, however, further research needs to be complete before the reason for the selectivity is understood. [48]
The Corticospinal Tract
This descending pathway conveys information from the motor areas of the brain to the spinal cord. This spinal tracts is of great importance as it can direct or indirectly control the movement of muscles. The corticospinal tract is made up of two pathways:
- Lateral- which projects axon onto motoneurons and/or interneurons of distal muscles.
- Ventral- which projects axon onto motoneurons and/or interneurons of axial muscles.
It has been noted that in particular the distal portions of the corticospinal pathway fibers are severely affected, suggesting a dying-back degeneration. [43] Dying-back degeneration implies that degeneration occurs at the most proximal end of the axon and destructively works its way up toward the neuron. Within the cerebral cortex the corticospinal tract originates from pyramidal or Betz cells in which degeneration is apparent but to a reduced extent. [43]
Results of lesion of the corticospinal tract can produce:
- Muscle weakness, mainly of the lower extremities and is most prominent in extensors and abductors of the hip [49]
- Positive Babinski reflex indicate involvement of the corticospinal tracts.
Clinical Presentation
Symptoms
Friedreich's Ataxia (FRDA) often manifests before puberty to early adulthood. Previous papers setting guidelines for the diagnosis of FRDA and was first established by Geffory et al. (1976)[50] includes the symptoms of ataxia of limb and gait, onset before 20 years of age, absent reflexes in lower limbs, dysarthria, loss of peripheral sense (proprioception), muscle weakness and sensory loss on the back[51]. It was then revised by Harding (1981)[51] to exclude muscle weakness and sensory loss on the back, dysarthria and to include the onset of FRDA before the age of 25, ataxia of gait, and absent reflexes in the leg[51].
As evident between Harding and Geffory, there are variations between authors on symptoms considered to be primary. Physical complaints such as chest pains [52] [53] indicative of cardiomyopathy scoliosis, foot deformity (pes cavus, hammer toe), extensor plantar responses (Babinski's sign), and dysarthria* (Dysarthria was considered a secondary symptom by Harding but a primary symptom by Geffory) are common and are often classified as secondary symptoms before FRDA is suspected[35].
For more information on past diagnostic guidelines and current suggested diagnostic practice, see diagnosis. Other symptoms associated with FRDA such as a direct consequence of neurodegeneration such as hyperreflexia and hypotonia amongst the others already mentioned had not been mentioned by Harding or Geffory but are important to note as they are a direct consequence of FRDA. For more information see the section on neuropathology.
The table below summarises symptoms of FRDA as primary or secondary.
| Classification of symptom | Type of symptom |
| Primary | Ataxia of limb and gait
Absent reflexes in lower limbs Onset before 25 years of age Loss of peripheral sense (proprioception) |
| Secondary | Scoliosis
Pes Cavus
Extensor plantar responses (Babinski's sign) Dysarthria |
Complications
Complications of FRDA can have cardiac and pancreatic involvement as a secondary result of mitochondrial iron accumulation. Cardiac involvement is high (>90%)[54], and it is hypothesised that FRDA exacerbates existing cardiac risk factors and increases the chance of developing cardiomyopathy (eg: ventricular hypertrophy and tachycardia)[55]. Even in Friedreich's original description of his patients, 5 out of 6 patients had cardiac involvement[55]. Familial links in cardiomyopathy and familial groups affected with FRDA has been found to exist(P <0.01). Though it does not show as great a relationship of development to familial FRDA groups as diabetes [51]. For more information on cardiomyopathy in FRDA, see pathogenesis.
Diabetes as a complication of FRDA is fairly straight forward with a clear reason as to why it occurs. In mouse models of FRDA, when the frataxin gene is disrupted the overall volume of beta-cells is reduced due to cell apoptosis, loss of beta-cell proliferation and increased Reactive Oxygen Speices (ROS)in islets[56].
It was found that the incidence of diabetes increases with sibling-ship relationships (P< 0.001)[51].
Diagnosis
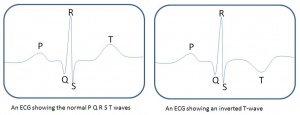
As diagnostic criterias were set before genetic screening was available, the diagnostic criteria was split into two categories of 'primary' and 'secondary' symptoms of which, primary symptoms were required for a diagnosis of FRDA and secondary symptoms acted as supporting evidence but diagnosis could not be made due to the possibility of other diseases which presented with those symptoms[35]. In a more recent review of FRDA diagnostic criteria, it is proposed that new three categories (not using the dated categories) of 'possible', 'probable' and 'definite' indicating the likelihood of FRDA should be used instead. Additionally, it was suggested to include lower limb areflexia and dysarthria, babinski's sign, or repolarisation abnormalities on the electrocardiogram (ie: abnormal T-wave) or repolarisation abnormalities in patients with retained lower limb reflexes to be able to make a possible diagnosis of FRDA[57]. Currently, patients who are suspected of having FRDA based on signs and symptoms (all adapted from previous FRDA diagnosis guidelines) are sent for genetic testing and are only diagnosed with FRDA after genetic testing confirms the diagnosis of FRDA.
Diagnostic Tools
The table below shows common diagnostic tools employed in the diagnosis of FRDA:
| Diagnostic tool | What it does | How it diagnoses FRDA | Image (if available) |
| Electromyogram (EMG) | Measures the electrical activity of muscle cells by inserting needles into muscle fibers that is to be tested and asking the patient to tense the muscle[58]. | EMG can detect denervation[58] such as present in motor neuron diseases or muscle denervation as present in FRDA. | Electromyograph test (video): [1] |
| Electrocardiogram (ECG) | Provides graphic presentation of the electrical activity or beat pattern of the heart | If T wave inversion is present, it may be an indication myocardial hypertrophy[59] which is a hallmark of cardiac involvment in FRDA. T wave inversions are also common findings in patients with FRDA[53]. | Normal ECG(video):[2] |
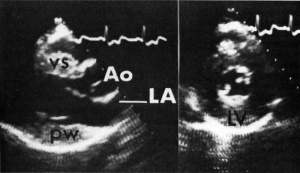
| Echocardiogram (ECHO) | Records the position and motion of the heart muscle | Identifies abnormalities in heart muscle such as hypertrophy of ventricles(useful for determining cardiac involvement)[60]. | Normal Echocardiogram (video): [3] |
| Blood tests | Checks for elevated glucose levels (in the event of diabetes developing) and vitamin E levels as individuals with FRDA often have low Vitamin E serum levels [61] | Blood tests work to identify any possible complication of FRDA (ie: diabetes) and identifies patients who require vitamin E supplements to increase the body's antioxidant capabilities[61]. | |
| Magnetic resonance imaging (MRI) | Provide brain and spinal cord images that are useful for ruling out other neurological conditions and confirming dorsal root degeneration. | Changes in the dorsal root or related neural structures involved in motor coordination can be monitored and identified with MRI. MRI has also been used to diagnose FRDA before the availability of genetic testing where the thinning of the cervical cord was an indication of neurodegeneration[34]. In a recent pilot study, the globus pallidus (involved in motor coordination) was found to improve with iron-chelation treatment using MRI technology[62]. Another paper found that MRI may be a useful tool in diagnosing FRDA and allows researchers to track neural atrophy[63]. | MRI of heart (video): [4] |
| Computed tomography scans (CT scan) | CT scans work similarly to the MRI in that it is used as an imaging tool to identify neurodegeneration. | While CT scans can be used in a similar fashion to MRIs, it has been noted that CT scans only identified mild cerebellar atrophy in advanced patients perhaps due to low CT resolution in the neck[63]. | CT scan of lung cancer (video): [5] |
| Nerve conduction studies (NCS) | Measures the speed with which nerves transmit impulses by using two electrodes (one to send the impulse and the other to measure the response)[58]. | Nerve conduction studies determines how far and if neurodegeneration has occurred by analysing amplitude, latency, duration, and conduction. Each item assessed will inform the clinician of the number of nerve fibers activated, integrity of myelin sheaths or axonal loss[58]. FRDA diagnosis may be considered if nerve conduction studies indicates nerve degeneration. | Nerve conduction test (video): [6] |
| Genetic Testing | Screens for mutations in the frataxin gene, either a repeat expansion or a point mutation. | FRDA is caused by deficient frataxin levels, which is most commonly caused by a GAA repeat expansion in intron 1 of the frataxin gene, and in some rare cases by a point mutation leading to a defective protein product. Both cases lead to deficient frataxin levels. When FRDA is suspected, a genetic test can be used to confirm the diagnosis. | Genetic screening (video): [7] |
| Prenatal Testing | A genetic test of the unborn infant. Cells from the developing child can be obtained through amniocentesis or from the maternal blood, which can then be subjected to genetic tests. | Same as in Genetic Testing. |
Prenatal Diagnosis
Following the localisation of the frataxin gene to chromosome 9 in 1988, a prenatal test was developed for the first time in 1989 by Wallis et al (1989) [11], who used two closely linked adjacent DNA markers, MCT112 and DR47, in their design of a genetic test. This allowed reliable prenatal diagnosis, a useful step for families at risk as the biochemical causes of FRDA were still unknown at the time. However, the informativeness of this first prenatal test was still limited to 10-15% of families, and subsequent research has made the effort to increase this initial informativeness. In 1990, Hanauer et al [12] identified two further markers that are even closer to the frataxin gene than the two initially used by Wallis et al (1989). These markers are D9S15 and D9S5. D9S15 alone provided 40% informativeness and only requires very little DNA, which makes it very suitable for prenatal testing. When combining the two markers, only 20% of the families remained uninformed, and when using all four markers, MCT112, DR47, D9S15 and D9S5, 100% informativeness was achieved. This initially seemed to make prenatal diagnosis of FRDA with 99% accuracy or more possible. Nevertheless, refinement of the genetic screens continued, especially after recombination events were detected in the D9S5-D9S15 markers in 1993 [13], rendering the tests suggested by Hanauer et al (1990) unreliable. Further markers were suggested by Monros et al (1995) [13], who found an accuracy approaching 100%.
Once the cause of the gene defect was identified as (most commonly) a repeat expansion of the GAA triplet, this provided a direct approach for molecular diagnosis. PCR and Southern Blot can be used to detect and thus quantify the repeat, allowing a reliable diagnosis. PCR is the more reliable tool and only needs small quantities of DNA, which make it particularly suitable for prenatal testing. [64]
Postnatal Diagnosis
Friedreich's Ataxia (FRDA) is often diagnosed based on presenting clinical symptoms but testing for the gene defect that causes it is taken as a definitive diagnosis. A paper on cardiac evaluation of Friedreich's Ataxia patients found that cardiac evaluation using any of the above cardiac testing techniques was a useful tool to compliment genetic testing in terms for screening for patients who should be tested for Friedreich's Ataxia[65]The table below summarises diagnostic steps prior to and after genetic testing was available.
| Availability of genetic testing | Diagnostic symptoms |
| Prior to genetic testing availability | Only physical signs(eg: Scoliosis) and symptoms(eg: chest pains), age of onset and typical FRDA progression could identify it as FRDA. [66] |
| After genetic testing is available | Physical complaints are used in conjunction with genetic testing to confirm FRDA. Due to genetic testing, [34]it has been discovered that FRDA can occur in individuals older than the typical diagnostic age (first two decades of life[67]). |
Treatment
Currently For the degenerative congenital disorder Friedreichs Ataxia (FRDA) this is no current treatment to reverse, prevent and delay [68] FRDA. However there are various potential treatments which have shown signs of improvement from FRDA patients include, Iron chelation, Histone deacetylase inhibitors(HDACI) and antioxidant are the leading treatments towards FRDA[69][17][70].
Iron-chelation
Iron chelations potential as treatment for Friedrichs Ataxia (FRDA) is greatly focused. Within areas regarding to pathogenesis. FRDA effects Mitochondria leading to Mitochondrial accumulation of Iron, causing a usage of cytosolic iron[71].There is evidence that due to the fractin deficiency resulted in FRDA patients is from the depletion of cytosolic iron, it has been suggested therapeutic treatment of iron supplements to replenish cytosolic iron to normal range[72] to counter the rate of depletion.Where most potential chelators are those which specifically target mitochondrial pools of iron[73] for the reason of maintenance of Iron within cystol of the cell.
As cardiomyopathy is believed to be caused by the production of toxic agents from the excess iron reacting within mitochondria, Iron- chelation had been studied for it's therapeutic action on removing excess iron in mouse models. Between treated mice and untreated mice, the treated mice showed a decrease in heart weight and heart to body ratio. This demonstrates that while chelation limits cardiomyopathy, it did not 'cure' the problem. As chelation did not lead to major iron depletion or toxicity reduction, and prevented iron accumulation in mice with the mutated frataxin gene it has opened up a possible treatment path of preventing mitochondrial iron build up - stopping the production of toxic agents and free radicals before they can be produced. Additionally, mice treated with chelation did not show any changes in the histology of the heart or any other major organ. It also did not lead to red blood cell loss, decreased hemoglobin concentration or hematocrit[74].
Histone deacetylase inhibitors(HDACI)
Treatment of FRDA through histone deacetylase inhibitor (HDACI) has shown potential as treatment in reversing heterochromatin of genes[75]. HDACI has shown sign of increasing levels of fractin to normal range within the nervous system and the heart, positive effects of fractin levels has given signs of decrease in progression of FRDA. Therapeutic use of HDACI led to the normalization of the genetic expression of FRDA patients from the minute levels of fractin. Clearly from mouse models depict therapeutic effect of HDACI, HDACI is able to cross through the blood brain barrier elevating levels of histone acetylation without having toxic effects upon the brain though has shown no affiliation to fractin levels instead affecting GAA repeat[76].
Antioxidants
The most promising antioxidant treatments are Idebenone and Coenzyme Q10 with Vitamin E. Antioxidants have shown degree of reduction on oxidative stress in mitochondria, however there are still ongoing trials to show its effectiveness.
- Conenzyme Q10 is an electron carrier with a reduction of oxidative stress effect from the combination of vitamin E, combination of Q10 and vitamin E displayed a positive effect[77]. Where Q10 and vitamin E conveyed the cardiac and skeletal improvement with the betterment of the mitochondrial synthesis[78].
- Idebnone operates with a duel function in which it reverses redox reactions that affects electron balance in the mitochondria while also supporting mitochondria functions to prevent damage[17]. Usage of Idebenone has been proven to reduce cardiac hypertrophy in FRDA indicating a 20% reduction on left ventricular mass from cardiac ultrasound in half the patients during trial[79], though the dosage of Idebenone give is at low dosage treatments of 5mg/kg/day which has shown reduction in cardiac hypertrophy[80]. Thus Idebenone is frequently used a treatment method although other alternatives are present including erythropoietin and other gene-based strategies[81].
Current Research
A lot of the current research is looking at the potential of idebone, an iron chelator as a treatment for FRDA:
- A phase 3, double-blind, placebo-controlled trial of idebenone in friedreich ataxia. [82]
- Assessment of neurological efficacy of idebenone in pediatric patients with Friedreich's ataxia: data from a 6-month controlled study followed by a 12-month open-label extension study. [83]
- Combined therapy with idebenone and deferiprone in patients with Friedreich's ataxia. [84]
- Antioxidants and other pharmacological treatments for Friedreich ataxia. [85]
The following recent publication provides an overview of the current therapeutic perspective:
- New advances in the treatment of Friedreich ataxia: promisses and pitfalls. [86]
The following papers are looking at evaluation criteria of the disease in children. These can differ to the ones used in adults, which nevertheless is commonly also used for younger ages:
- In children with Friedreich ataxia, muscle and ataxia parameters are associated. [87]
- Neurophysiological evaluation in children with Friedreich's ataxia. [88]
Furthermore, current research seaks to establish norms in the progression rate of the disease in order to allow accurate assessment and optimised treatment:
- Measuring the rate of progression in Friedreich ataxia: implications for clinical trial design. [89]
- Review: Evaluating the progression of Friedreich ataxia and its treatment. [90]
Improvements in genetic counseling for FRDA patients are suggested by this recent study:
- Exploration of transitional life events in individuals with Friedreich ataxia: implications for genetic counseling. [91]
External Links
Video of Ataxic Gait [8]
Video of a Positive Babinski Sign - [9]
Video of Dysmetria - [10]
Video of Hyperreflexia - [11]
Video of nerve conduction test - [12]
Video of Electromyograph test - [13]
Video of a normal Echocardiogram - [14]
Video of an MRI (brain and heart)- Brain:[15] Heart:[16]
Video of CT scan (lung cancer) - [17]
Video of Electrocardiogram (normal) - [18]
Video of Genetic Screening - [19]
Glossary
Aconitase - Is an iron-sulphur protein involved in iron homeostasis
Apoptosis - Programmed cell death.
Ataxic Gait - Involves a wide-based stance, lack of muscle coordination, errors in range and force of movement, delay in initiating movement.
Atrophy - Involves a decrease and/or wasting of an organ or tissue within the body.
Axon - The (usually long) process that transmits signals from the neuron it is connected to.
Cardiac Arrhythmia - Abnormal rate or beat of the heart, which can be either fast (tachycardia) or slow (bradycardia).
Carrier - An individual who is heterozygous for a recessive trait. Heterozygous carriers of a recessive disease allele are often uneffected.
Chelation - chemicals that form soluble, complex molecules with certain metal ions, inactivating the ions so that they cannot normally react with other elements or ions... (ASTM)
CNS - Central Nervous System.
Codon - A triplet of nucleotides that specifies an amino acid or a start or stop signal in the genetic code.
Cortical - Of or relating to the cortex.
Demyelination - The loss of the myelin sheath surrounding an axon.
DNA marker - a gene or DNA sequence with a known location on a chromosome that can be used to identify cells, individuals, or species.
DNA polymerase - An enzyme that catalyses the synthesis of DNA using a DNA template.
DRG -Dorsal Root Ganglion.
Dysarthria – A motor speech disorder causing slurring of words.
Dysmetria – Faulty judgment leads to the inability to perform basic movements, uncoordinated movement results.
Dysphagia – Involves difficultly of swallowing food, which can lead to coking of food or water, as well as, aspiration pneumonia.
Electrodes - A conductor which emits, controls, or collects the movement of electrons (ie: a current)
Erythropoietin - A hormone that stimulates red blood cell production.
FRDA - Friedreich's Ataxia.
Founder event - A form of genetic drift. The establishment of a population by a small number of indivduals whose genotypes carry only a fraction of the different kinds of alleles in the parental population.
GAA - Guanine Adenine Adenine Nucleotide Triplet.
Gene silencing - Inhibition of the gene expression.
Globus pallidus - A sub-cortical region of the brain, part of the extrapyramidal motor system.
Hematocrit - Measures the volume of red blood cells in blood.
Histone - A protein around which DNA coils to form chromatin.
Histone deacetylase inhibitors - These are compounds that interfere with enzymes that remove an acetyl group from histones.
Heterozygous - Possessing two different variants of a gene.
Homozygous - Possessing two identical variants of a gene.
Hyperreflexia – Over active reflexes responses, which can lead to spastic movements
Hypertrophy - Increasing in size of a organ or tissue.
Hypotonia - Decrease in muscle tone.
Intron - DNA sequence that lies between coding regions of a gene. Introns are transcribed but are spliced out of the primary RNA product and thus do not contribute to the polypeptide encoded by the gene.
Linkage - The condition in which genes have their loci on the same chromosome, causing them to be inherited as a unit, provided they are not separated by crossing over during meiosis. The closer two genes are located two each other on the chromosome, the "tighter" the linkage; the less likelihood there is for them to be separated during meiosis.
Linkage studies - exploit the idea that tightly linked genes are inherited together: if the location of one gene is known and it is suspected to be linked to a second gene, this can be used to determine the location of the second gene.
Missense mutation - A mutation that alters a codon to that of another amino acid and thus leads to an alteration in the resulting polypeptide.
mRNA - Messenger RNA. The product of gene transcription, which will be translated into protein.
Myelin sheath - An insulating cover that wraps around individual nerves to increase the speed of conduction.
Neurological - Pertaining to the nervous system or nerves.
Nonsense mutation - A mutation that creates a stop codon, thus leading to the halt of translation and a shortened gene product.
PCR - Polymerase Chain Reaction. A method for amplifying DNA segments.
Periventricular - Around or near a ventricle. (A ventricle is an opening or chamber in the body.)
Pes cavus - Feet with abnormally high arches.
Pneumonia - Inflammatory condition of the lungs.
PNS - Peripheral Nervous System.
Point mutation - A mutation affecting a single nucleotide.
Positive Babinski Sign – The big toe extends up and backward whilst the other toes splay outward (abduct). This is sign of upper motoneuron disease.
Proprioception - Refers to the ability of sensing movement and position of muscles without visual guides. Required for hand-eye co-ordination.
Purine - One of the two chemical classes to which nucleotides belong.
Pyrimidine - One of the two chemical classes to which nucleotides belong.
Reactive Oxygen Speices (ROS) - It is a classification for chemically-reactive molecules containing oxygen.
Recombination - The process that leads to the formation of new gene combinations on chromosomes.
Redox - A reversible chemical reaction in which one reaction is an oxidation and the reverse is a reduction.
Replication - The process whereby DNA is duplicated.
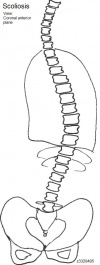
Scoliosis - Abnormal curving of the spine in the Coronal plane to form an 'S-shpe' when viewed from the front.
Sepsis - Infection of the blood, generally bacterial.
Southern Blot - A technique in which DNA fragments are separated and transferred to a nylon or nitrocellulose membrane. Specific DNA fragments can be identified by hybridisation to a complementary, radioactively labeled probe.
Splicing - The reaction in which introns are removed and exons are joined together in the mRNA molecule.
Tachycardia - A resting heart rate that exceeds the normal range.
Triplet repeat (trinucleotide repeat) - A tandemly repeated cluster of three nucleotides, such as GAA in FRDA, within or near a gene.
T-wave - On an ECG, it represents the recovery of the ventricles.
References
- ↑ 1.0 1.1 1.2 <pubmed>11351269 </pubmed> Cite error: Invalid
<ref>tag; name 'PMID11351269' defined multiple times with different content - ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 <pubmed>19283344</pubmed>
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 <pubmed>21315377</pubmed>
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 <pubmed>10633128</pubmed>
- ↑ <pubmed>12547248</pubmed>
- ↑ 6.0 6.1 6.2 <pubmed>10607838</pubmed>
- ↑ <pubmed>5673214</pubmed>
- ↑ 8.0 8.1 8.2 8.3 <pubmed>15090560</pubmed>
- ↑ <pubmed>20156111 </pubmed>
- ↑ <pubmed>6452194</pubmed>
- ↑ 11.0 11.1 <pubmed>2574535</pubmed>
- ↑ 12.0 12.1 <pubmed>1970404</pubmed>
- ↑ 13.0 13.1 13.2 <pubmed>7659688</pubmed>
- ↑ <pubmed>9326946</pubmed>
- ↑ 15.0 15.1 15.2 15.3 15.4 <pubmed>9207112</pubmed>
- ↑ <pubmed>12165564</pubmed>
- ↑ 17.0 17.1 17.2 <pubmed>19283347</pubmed>
- ↑ <pubmed>20374234</pubmed>
- ↑ 19.0 19.1 <pubmed>14767759</pubmed>
- ↑ <pubmed>20569261</pubmed>
- ↑ 21.0 21.1 21.2 21.3 <pubmed>21652007</pubmed>
- ↑ 22.0 22.1 22.2 22.3 <pubmed>7272714</pubmed>
- ↑ <pubmed>21128039</pubmed>
- ↑ <pubmed>16092110</pubmed>
- ↑ <pubmed>2899844</pubmed>
- ↑ 26.0 26.1 <pubmed>21827895</pubmed>
- ↑ 27.0 27.1 <pubmed> 20156111 </pubmed>
- ↑ 28.0 28.1 <pubmed>11350948</pubmed>
- ↑ <pubmed>9331900</pubmed>
- ↑ <pubmed>10767347</pubmed>
- ↑ 31.0 31.1 <pubmed>9443873</pubmed>
- ↑ <pubmed>21127046</pubmed>
- ↑ <pubmed>20373285</pubmed>
- ↑ 34.0 34.1 34.2 <pubmed>21315377</pubmed>
- ↑ 35.0 35.1 35.2 <pubmed>10633128 </pubmed> Cite error: Invalid
<ref>tag; name 'PMID:10633128' defined multiple times with different content Cite error: Invalid<ref>tag; name 'PMID:10633128' defined multiple times with different content - ↑ <pubmed>3593615</pubmed>
- ↑ <pubmed>18621680</pubmed>
- ↑ <pubmed>11269509</pubmed>
- ↑ <pubmed>9339708</pubmed>
- ↑ <pubmed>18759347</pubmed>
- ↑ <pubmed>19957189</pubmed>
- ↑ 42.0 42.1 <pubmed>19727777</pubmed>
- ↑ 43.0 43.1 43.2 43.3 43.4 <pubmed>12878293</pubmed>
- ↑ 44.0 44.1 44.2 <pubmed>19679182</pubmed>
- ↑ <pubmed>17262846</pubmed>
- ↑ <pubmed>21878126</pubmed>
- ↑ 47.0 47.1 47.2 <pubmed>21107777</pubmed>
- ↑ 48.0 48.1 48.2 <pubmed>21638087</pubmed>
- ↑ <pubmed>20301458</pubmed>
- ↑ <pubmed>1087179</pubmed>
- ↑ 51.0 51.1 51.2 51.3 51.4 <pubmed>7272714</pubmed>
- ↑ <pubmed>7488466</pubmed>
- ↑ 53.0 53.1 <pubmed>3593615</pubmed>
- ↑ <pubmed>12045843</pubmed>
- ↑ 55.0 55.1 <pubmed>17622372</pubmed>
- ↑ <pubmed>12925693</pubmed>
- ↑ <pubmed>11104216</pubmed>
- ↑ 58.0 58.1 58.2 58.3 <pubmed>21894276</pubmed>
- ↑ <pubmed>19486532</pubmed>
- ↑ <pubmed>2940284</pubmed>
- ↑ 61.0 61.1 <pubmed>11554913</pubmed>
- ↑ <pubmed>21791473</pubmed>
- ↑ 63.0 63.1 <pubmed>2759158</pubmed>
- ↑ <pubmed>9742572</pubmed>
- ↑ <pubmed>12045843</pubmed>
- ↑ <pubmed>13872187</pubmed>
- ↑ <pubmed>19283344</pubmed>
- ↑ <pubmed>19283349</pubmed>
- ↑ <pubmed>19283350</pubmed>
- ↑ <pubmed>17968974</pubmed>
- ↑ <pubmed>10805340</pubmed>
- ↑ <pubmed>18424449</pubmed>
- ↑ <pubmed>20156111</pubmed>
- ↑ <pubmed>18621680</pubmed>
- ↑ <pubmed>16205715</pubmed>
- ↑ <pubmed>18463734</pubmed>
- ↑ <pubmed>19049556</pubmed>
- ↑ <pubmed>15824263</pubmed>
- ↑ <pubmed>11907009</pubmed>
- ↑ <pubmed>19363628</pubmed>
- ↑ <pubmed>20856912</pubmed>
- ↑ <pubmed>20697044</pubmed>
- ↑ <pubmed>21779958</pubmed>
- ↑ <pubmed>20865357</pubmed>
- ↑ <pubmed>19821439</pubmed>
- ↑ W Nachbauer, S Boesch New advances in the treatment of Friedreich ataxia: promisses and pitfalls. Clinical Investigation: 2011, 1(8);1095-1106.
- ↑ <pubmed>21574990</pubmed>
- ↑ <pubmed>19775837 </pubmed>
- ↑ <pubmed>20063431</pubmed>
- ↑ <pubmed>19283349</pubmed>
- ↑ <pubmed>20979606</pubmed>