2011 Group Project 1
| Note - This page is an undergraduate science embryology student group project 2011. |
Turner Syndrome
--Mark Hill 10:44, 8 September 2011 (EST) Some of the existing sub-sections have appropriate content, but there are also empty sub-sections, a total lack of referencing/citation and no glossary.
- The referencing issue needs urgent progress.
- Existing figures/table are appropriate. Table appears to be directly used from an uncited source.
- There needs to be more images in this work.
- Where is the student drawn figure?
- Read http://embryology.med.unsw.edu.au/embryology/index.php?title=Help:Reference_Tutorial#Multiple%20Instances%20on%20Page
Introduction
Turner Syndrome (TS), named after Henry Hubert Turner who first described the syndrome in his paper in 1938,[1] is one of the most commonly occuring chromosomal disorders. It is caused by a complete or partial X monosomy in some or all cells and occurs in approximately 1 in 2000 live births in females only, however the morbidity rate of spontaneous abortions is 10% and only about 1% of fetuses survive to term.
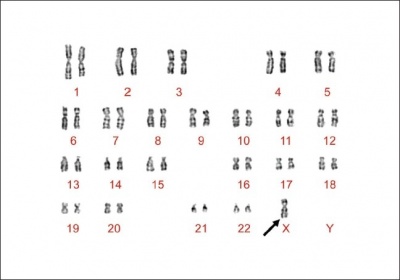
During normal fetal development, each ovary contain as many as 7 million oocytes. The oocytes gradually reduce to 400,000 during menarche and during menopause fewer than 10,000 remains. However, in Turner syndrome, the ovaries develop normally during embryogenesis but the absence of the second X chromosome leads to an accelerated loss of oocytes, which is complete by the time the infant is 2 years of age. Genetically menopause occurs before menarche and the ovaries are reduced to atrophic fibrous strands, devoid of ova and follicles (streak ovaries). Development of somatic (nongonadal) tissues that reside on the missing/abnormal X chromosome are also severely affected. For example short stature is caused by a deletion of the Xp chromosome and the deletion of Xq causes gonadal dysfunction [3].
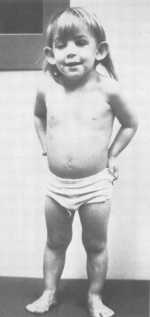
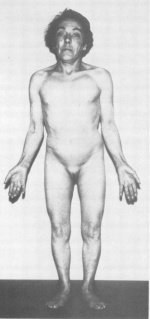
The most frequent clinical feature is short stature and gonadal dysgenesis. Other features may include coarctation of the aorta, renal anomalies, neck webbing, and lymphoedema. The affected organ systems and tissues may be effected to a lesser or greater extent. In most cases each person who has TS all vary in their clinical phenotype. In recent years there has been increased interest in TS due to the introduction of growth hormone treatment. There has been marked improvement in the understanding of this condition as advances in molecular genetic techniques occur. However, there still needs for further research. A multidisciplinary approach to treatment is important to improve the quality of life of girls with TS [4].
Epidemiology
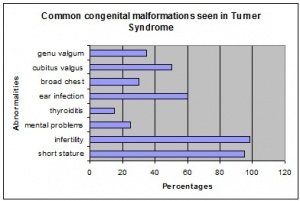
Turner Syndrome affects about 1 in 2000 live-born females. There are three types of karyotypic abnormalities but the most frequently seen is where the entire X chromosome is missing resulting in 45 X karyotype. The remaining third have structural abnormalities of the X chromosomes and two thirds are mosaics. Whereby, the maternal X is retained in two-thirds of women and the paternal X in the remainder. The phenotype of TS varies but involves anomalies of the sex chromosome. It could be caused by the limited amount of genetic material in these abnormal chromosomes. Turner Syndrome can be transmitted from mother to daughter, and thus could be described as a heredity linked syndrome [4].
The loss of one of the sex chromosomes of TS occurs after the zygote has formed or just after the fusion of the gametes. In 70-80% of cases the retained X is from the mother. In such circumstances it has lead to the different phenotypic expression of the genes present on the X chromosome depending if it came from the mother or father. The morphological differences from those retaining the maternal compared to retaining the paternal X have shown to have a greater incidence of cardiovascular anomalies and neck webbing. The missing sex chromosome could be either an X or a Y. This has clinical implications because if the Y material is present there is a risk of up to 30% of gonadoblastoma developing in the dysgenetic gonads. This is because the 'gonadoblastoma locus' is on the Y chromosome which is situated just below the centromere. The inactivation of the abnormal X chromosomes is another cause that primarily affects hypogonadism phenotypically in females. [6].
Etiology
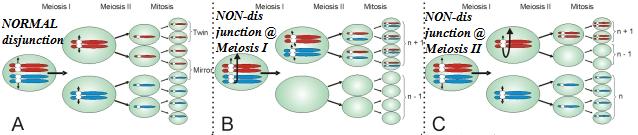
Causation of Turner Syndrome (TS) can be traced back to the stages of sex-cell development. When sex cells divide through a process called meiosis to create gametes, either a haploid egg (for females) or sperm (for males) two divisions occur, Meiosis I and Meiosis II. Meiosis is the main process which helps create the vast genetic diversity within all populations by allowing recombination and random assortment. During Meiosis I homologous chromosomes are separated; following Meiosis I, sister chromatids separate during Meiosis II. If during either stage of Meiosis I or II the homologous chromosomes or sister chromatids, respectively, do not fully separate, a phenomenon can occur called nondisjunction. Nondisjunction causes an uneven distribution of genetic material to each daughter nuclei. When an uneven distribution is such that one of the gametes does not have any of a chromosome, it can combine with another normal gamete to create a fertilized egg with only one chromosome as opposed to the normal two that are found in human cells; this is called a monosomy. When this occurs in the sex chromosomes leaving only a single X chromosome (X0 genotype) Turner Syndrome is created, leaving only 45 chromosomes in the zygote rather than the normal 46.
Turner Syndrome can also be created by partial monosomy or disjunctions, meaning that although a whole X chromosome is not missing, portions of it are not present or are non-functional, rendering the chromosome useless. Any disjunction seems to be completely sporadic and have yet to be attributed to any genetic link. The only thing known for sure is that during conception a portion of or the whole second sex chromosome is not conveyed to the zygote.[7] Because at least one X chromosome is necessary for vital functions, this condition can only be found in females.
Clinical Manifestations
The following are a list of characteristics and diseases which tend to accompany, be caused by, or be related to Turner Syndrome.
| Clinical Manifestations | Image(s) | |||||||||||||||||||||
| Physical Attributes |
| |||||||||||||||||||||
| Decreased Cognition | ||||||||||||||||||||||
| Increased Risk of | ||||||||||||||||||||||
| Prone to Develop Autoimmune Conditions | ||||||||||||||||||||||
| Cardiac Abnormalities (most serious/life threatening medical problems created by Turner Syndrome) |
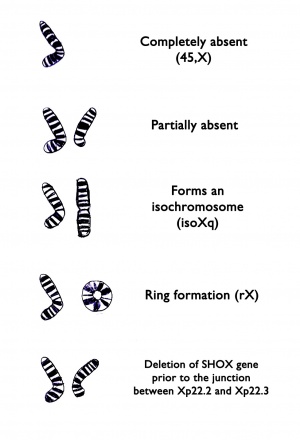
Diagnostic ProceduresDiagnostic DefinitionTurner syndrome is diagnosed through both an evaluation of physical features and by analysis of the second sex chromosome. The two criteria must be met for classification of Turner syndrome, an abnormality in the second sex chromosome must be found and the abnormality must be found to be expressed somehow in the individual's traits. Hence if physical characteristics are not present even when the cytogenetic criterion is met the patient is not diagnosed as having Turner syndrome.[18] In Turner syndrome the second sex chromosome is either:
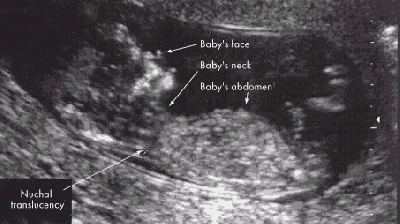
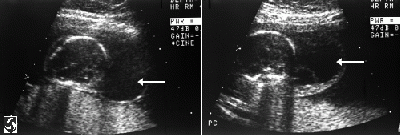
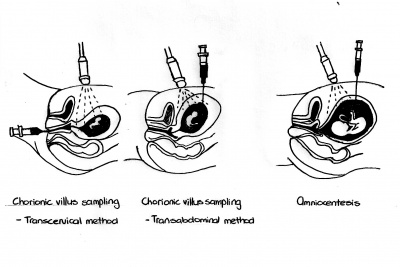
Any of these variations of the second sex chromosome may occur with or without cell line mosaicism. Turner syndrome may be diagnosed prenatally or postnatally, using this genetic diagnostic definition coupled with an appropriate phenotypic evaluation of the individual, as outlined below.[18] Prenatal DiagnosisThe prenatal diagnostic tool for Turner syndrome is karyotype screening and testing for phenotype abnormalities. If Turner syndrome is diagnosed prenatally, karyotype screening and an evaluation of the individual's traits should be conducted again postnatally for confirmation of this diagnosis. Turner syndrome is frequently diagnosed after karyotype screening during chorionic villous sampling or amniocentesis.[18] The table below outlines various prenatal tests conducted and the indications that may be present in babies with Turner syndrome. Although these techniques and the indications they reveal may highlight Turner syndrome signs, they should not be used as sole diagnostic tools.[18]
Postnatal DiagnosisIn postnatal diagnosis, karyotype investigation is undertaken for the individual. When a female presents with the following clinical findings, explained in table below, it is recommended that chromosomal analysis is undertaken, so that Turner syndrome may be eliminated[18]:
TreatmentCardiac TreatmentWhen patients are confirmed with Turner Syndrome, it is necessary to have a full cardiac evaulation including a physical exam and a echocardiogram. If cardiac abnormalities are found, monitoring by a cardiologist is recommended including regular blood pressure checks[18]. Coarctation of the aorta and hypoplastic left heart are quite often very serious issues are need to be dealt with surgically[26]. If no abnormalities are found, blood pressure in Turner Syndrome patients is still routinely checked and a follow up cardiac evaulation is recommended for girls around the age of puberty (12-15)[18]. SpeechMany Turner Syndrome patients have trouble with their speech. It is necessary for them to be refered to an Ear, Nose and Throat specialist and to a speech therapist to work on improve any speech problems[18]. Management of Puberty and GrowthThe main treatment for growth and pubertal development is Hormone Replacement Therapy. Growth Hormone is adminstered to girls with abnormal growth, resulting in postive growth that is consistent with the expected height of the patient. It is adminstered as early as 2 years of age, but more often in the age group of 9-12 which is in line with the growth spurt that occurs during puberty[18]. Natural estrogen and progesterone are administered to girls when they reach the age of puberty in early adolescence. The age at which this treatment commences varies between individuals, as does the dosage. The adminsteration of estrogen will begin the process of puberty in girls affected by Turner Syndrome and it is important that this begins around the same time as her peers[26]. The use of estrogen is often held off if the patient is also undergoing GH treatment so that maximum growth can be achieved, as estrogen will induce the fusion of the epiphyses and limit longitudinal bone growth[18]. Around 10% of nonmosaic and 20% of mosaic women with Turner’s will have spontaneous menses (periods) and may not need to undergo Hormone Replacement to initiate puberty. Around 2-5% of these women will have the potential to fall pregnant naturally[26]. AppearanceExtreme neck webbing maybe worrying or uncomfortable to women with Turner’s and in some cases plastic surgery is undertaken to fix this problem. Also if convex gorwth of toenails occurs, surgery is conducted so that the woman can wear normal shoes[26]. Ongoing Adult TreatmentClosely monitoring the health of Turner Syndrome adults is vital in the reduction of morbidity and mortality. An annual physical evalution should be undertaken which includes, blood pressure, heart auscultation, thyroid function, breast exam, and pap smear[18]. Particular attention needs to be taken in the area of weight and obesity in Turner Syndrome women due to their high risk of developing diabetes, osteoporosis and hypertension. Patients are to be encouraged to have a healthy lifestyle including healthy eating and exercise[18]. ResearchCurrent researchSince there is no preventative or cure, currently mainly research is being conducted into the areas of symptoms, possible treatments and risks involved with Turner syndrome. Growth hormone therapy in Turner syndrome: its affect on height, weight and stature.
Future researchFuture research needs to be conducted in the following areas: to follow up on the suggestions given in the conclusions of current research papers as outlined in the prior section and also into how the care system is functioning for Turner syndrome individuals as outlined below.
Glossary
References
2011 Projects: Turner Syndrome | DiGeorge Syndrome | Klinefelter's Syndrome | Huntington's Disease | Fragile X Syndrome | Tetralogy of Fallot | Angelman Syndrome | Friedreich's Ataxia | Williams-Beuren Syndrome | Duchenne Muscular Dystrolphy | Cleft Palate and Lip |