2010 Lecture 13
Redirect to:
Musculoskeletal Development
Introduction
This lecture is an introduction to the process of musculoskeletal development. In the body, this is mainly about mesoderm differentiation beginning with an embryonic connective tissue structure, the mesenchyme. In the head, this is a mixture of mesoderm and neural crest differentiation, from mesenchyme and ectomesenchyme respectively. The lecture will cover mainly cartilage and bone, as muscle will be covered in the limb lecture and in this week's laboratory.
Note that genes that control skeleton patterning and cell differentiation are different.
- Lectopia Audio Lecture Date: 14-09-2009 Lecture Time: 12:00 Venue: CLB 5 Speaker: Mark Hill Musculoskeletal
Lecture Objectives
- Understanding of mesoderm and neural crest development.
- Understanding of connective tissue development.
- Understanding of muscle, cartilage and bone development.
- Understanding of the two forms of bone development.
- Brief understanding of bone molecular development.
- Brief understanding of other bone roles.
- Brief understanding of bone abnormalities.
Textbook References
- The Developing Human: Clinically Oriented Embryology (8th Edition) by Keith L. Moore and T.V.N Persaud - Moore & Persaud Chapter 15 the skeletal system
- Larsen’s Human Embryology by GC. Schoenwolf, SB. Bleyl, PR. Brauer and PH. Francis-West - Chapter 11 Limb Dev (bone not well covered in this textbook)
- Before we Are Born (5th ed.) Moore and Persaud Ch16,17: p379-397, 399-405
- Essentials of Human Embryology Larson Ch11 p207-228
Musculoskeletal medical conditions
Health expenditure for arthritis and musculoskeletal conditions, 2004-05
- "Arthritis and musculoskeletal conditions affect more than 6 million Australians. In 2004-05, direct health expenditure on these conditions amounted to $4.0 billion or 7.5% of total allocated health expenditure in Australia."
Craniofacial abnormalities in Williams-Beuren syndrome
Williams-Beuren syndrome is a genetic disease caused by a hemizygous deletion of 28 genes on chromosome 7. Leads to a distinctive set of craniofacial features. Probably caused by defects in patterning rather than differentiation as all of the structures form normally, just in slightly different positions relative to each other. Neuromuscular and regenerative medicine unit, SOMS
Patterning of the axial musculoskeletal system
Expression of the Hox genes defines locations on the anteroposterior axis
Connective Tissue Development
Stage 1 - migrate to site of skeletogenesis
Stage 2 - associate with an epithelium
Stage 3 - Cell Condensation - mesenchymal dispersed cell population, gathers together to differentiate
Stage 4 - Overt Differentiation - chrondroblast, osteoblast, myoblast
Cartilage
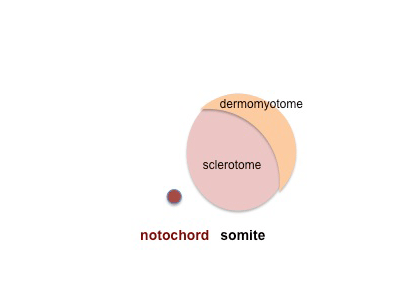
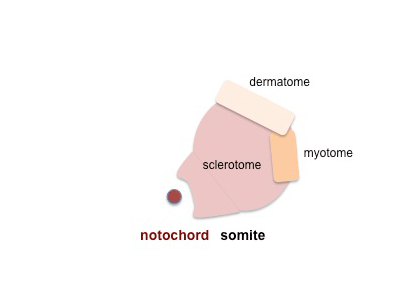
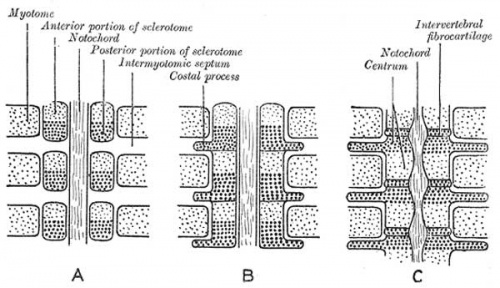
Sclerotome
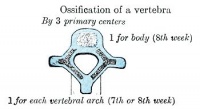
Vertebra
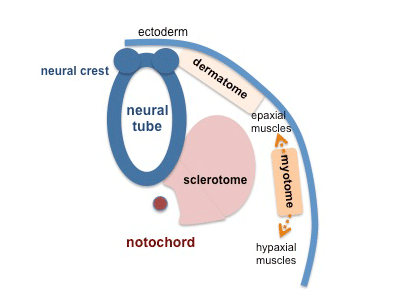
- Vertebral column formation - week 4, somite sclerotome surrounds notochord.
- notochord (and floorplate) induces sclerotome migration and vertebral body cartilages.
- neural tube induces vertebral arches.
- Scleretome has 2 components
- upper loose (pathway for artery and nerve) and lower compact
- Vertebral segmentation is shifted 1/2 somite caudally - by fusion cephalic compact with caudal loose to form vertebra from 2 sclerotomes.
- Caudal dense region also forms neural arch.
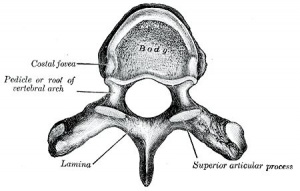
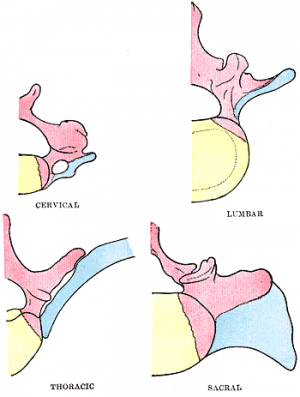
Adult vertebral column
- 33 total - 7 cervical, 12 thoracic, 5 lumbar, 5 sacral, and 5 coccygeal
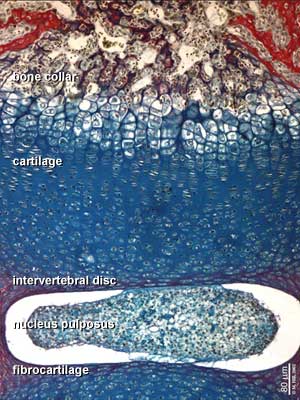
Intervertebral Disc
- Structure - annulus and nucleus pulposus
- dense region of sclerotome.
- notochord initially contributes to nucleus pulposus of each disc, contribution replaced and lost postnatally.
Ribs
- dense region of sclerotome contributes costal processes (thoracic region).
- chondrification commences day 45 and rib cage is cartilage by end of embryonic period.
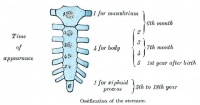
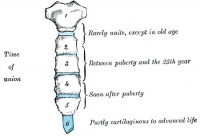
Sternum
- mesenchyme from ventral body wall (manubrium, body, ziphoid).
- sternal cartilage "bars" fuse with costal processes and developing clavicles by end of embryonic period.
Cartilage growth
- Interstitial growth - occurs mainly in immature cartilage. Chondroblasts in existing cartilage divide and form small groups of cells (isogenous groups) which produce matrix to become separated from each other by a thin partition of matrix.
- Appositional growth - occurs also in mature cartilage. Mesenchymal cells surrounding the cartilage in the deep part of the perichondrium (or the chondrogenic layer) differentiate into chondroblasts.
Hypertrophic Chondrocytes
- secrete VEGF, promoting vascular invasion
- hypertrophic calcified cartilage becomes resorbed, by recruited chondroclasts/osteoclasts via MMP9
Bone
Mice lacking Cbfa1 (Runx2) don't form bone
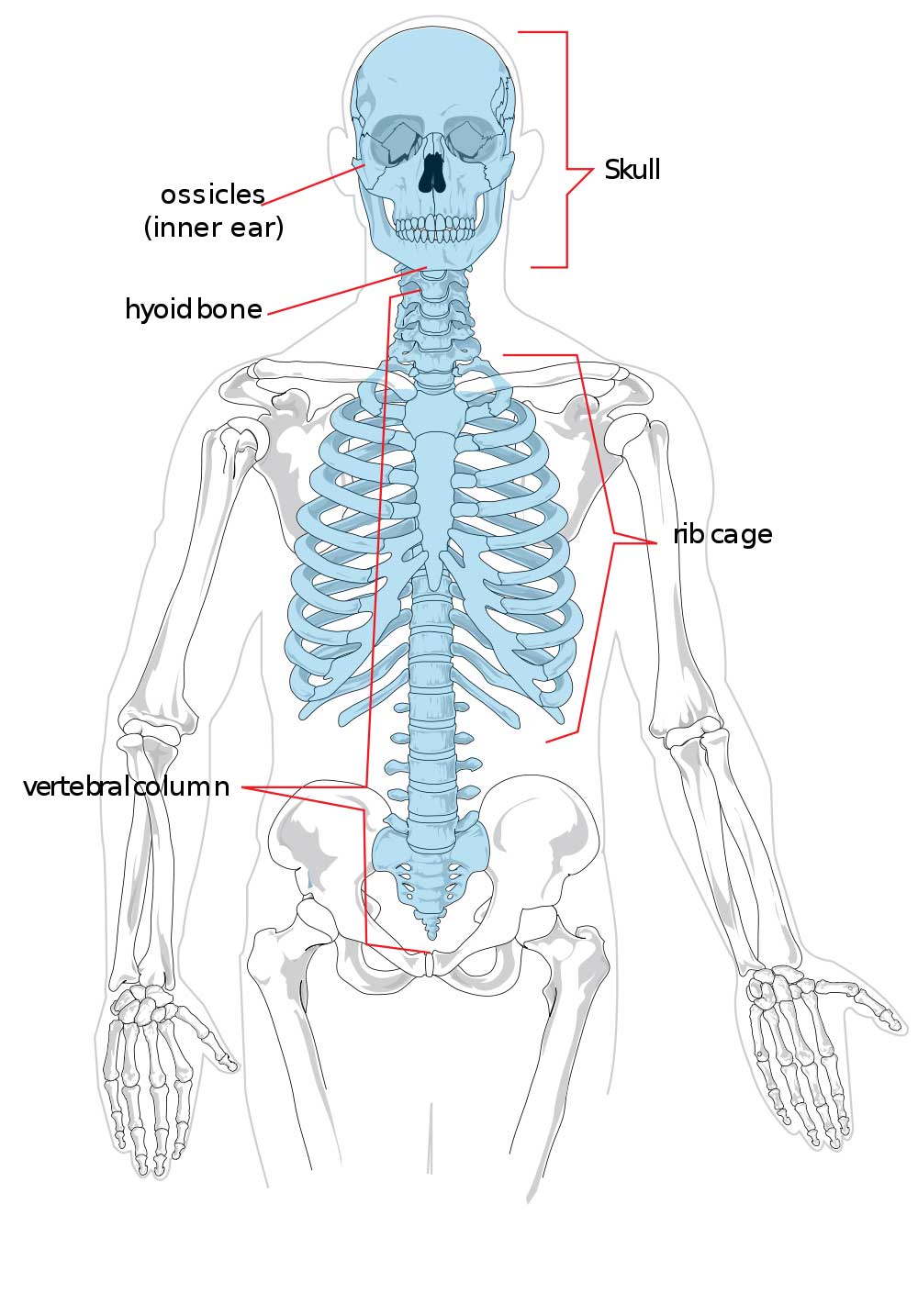
- Two major systems of bones: the axial skeleton and the appendicular skeleton.
- axial skeleton - 80 bones (skull, vertebrae, ribs, and sternum)
- appendicular skeleton - 126 bones (shoulders, pelvis, and limbs)
- Two main forms of bone formation: Endochondral and Intramembranous. Ossification process continues postnatally through puberty until mid 20s.
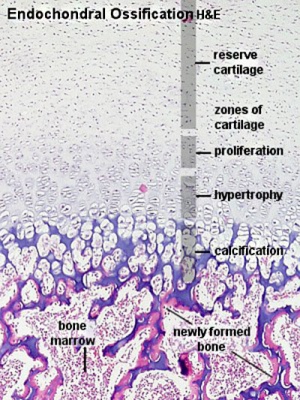
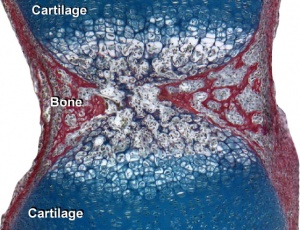
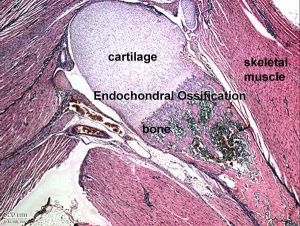
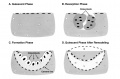
Endochondral Ossification
- Majority of skeleton formed by this process (vertebra, limb long bones)
- Osteoblasts derived from the bone collar replace cartilage matrix with a matrix rich in type I collagen leading to bone formation
- Ossification centres (primary and secondary)
- Early ossification occurs at ends of long bone
University of Bristol - ossification
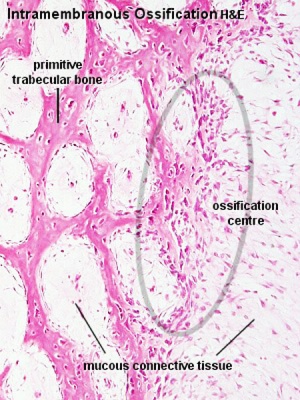
Intramembranous Ossification
- Specialized form of ossification from a mesenchymal membrane. (skull, clavicle)
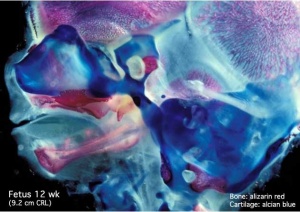
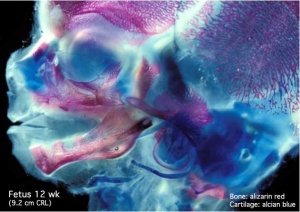
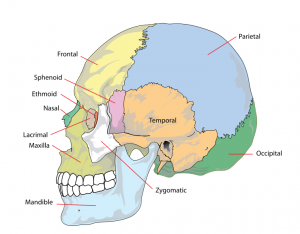
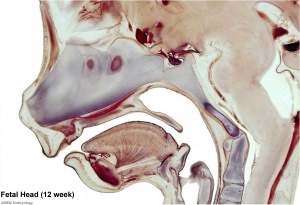
Skull
The Skull is a unique skeletal structure in several ways: embryonic cellular origin (neural crest), form of ossification (intramembranous and endochondrial) and flexibility (fibrous sutures). Musculoskeletal Development - Skull Development
The bones enclosing the brain have large flexible fibrous joints (sutures) which allow firstly the head to compress and pass through the birth canal and secondly to postnatally expand for brain growth.
These sutures gradually fuse at different times postnatally, firstly the metopic suture in infancy and the others much later. Abnormal fusion (synostosis) of any of the sutures will lead to a number of different skull defects.
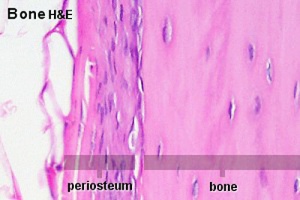
Osteogenesis
- Formation of mature osteoblasts - the mesenchymal stem cells initially form preosteoblasts that then differentiate.
- osteogenesis is inhibited by - Wnt signaling pathway antagonists (DKK-1, sclerostin, and SFRP1) and serotonin.
Cells
- Osteoprogenitor cell - periosteum and endosteum
- Osteoblast - Secrete bone matrix, differentiate into osteocytes
- Osteocyte - Mature bone cell, Embedded in matrix, matrix calcifies soon after deposition
Osteoclastogenesis
- Formation of mature osteoclasts - the osteoblasts regulate this process through the production of RANKL (Receptor Activator for Nuclear Factor κ B Ligand) by pre-osteoblast cells.
Osteoclast origin- fusion of monocytes or macrophages, Blood macrophage precursor, Attach to bone matrix
Lysosomes - released into space between ruffled border and bone matrix, enzymes break down collagen fibres, resorption bays or Howship's lacunae
Muscle
Myogenesis
- Smooth muscle - cells originate from undifferentiated mesenchymal cells. These cells differentiate first into mitotically active cells, myoblasts, which contain a few myofilaments. Myoblasts give rise to the cells which will differentiate into mature smooth muscle cells.
- Skeletal muscle - cells originate from the paraxial mesoderm. Myoblasts undergo frequent divisions and coalesce with the formation of a multinucleated, syncytial muscle fibre or myotube. The nuclei of the myotube are still located centrally in the muscle fibre. In the course of the synthesis of the myofilaments/myofibrils, the nuclei are gradually displaced to the periphery of the cell.
- Cardiac muscle - cells originate from the prechordal splanchnic mesoderm.
Skeletal Muscle Stages
Myoblast - individual progenitor cells
Myotube - multinucleated, but undifferentiated contractile apparatus (sarcomere)
Myofibre (myofiber, muscle cell) - multinucleated and differentiated sarcomeres
- primary myofibres - first-formed myofibres, act as a structural framework upon which myoblasts proliferate, fuse in linear sequence
- secondary myofibers - second later population of myofibres that form surrounding the primary fibres.
Muscle Fibre Types
- type IIB, IIA, IIX, and I fibres - based only on the myosin ATPase activity.
- Type I fibres appear red, due to the presence of myoglobin
- Type II fibres appear white, due to the absence of myoglobin and their glycolytic nature.
- A group of individual myofibres within a muscle will be innervated by a single motor neuron.
- The electrical properties of the motor neuron will regulate the contractile properties of all associated myofibres.
MH- you do not need to know the table below in detail, it is provided for information purposes only.
| Fibre Type | Type I fibres | Type II a fibres | Type II x fibres | Type II b fibres |
|---|---|---|---|---|
| Contraction time | Slow | Moderately Fast | Fast | Very fast |
| Size of motor neuron | Small | Medium | Large | Very large |
| Resistance to fatigue | High | Fairly high | Intermediate | Low |
| Activity Used for | Aerobic | Long-term anaerobic | Short-term anaerobic | Short-term anaerobic |
| Maximum duration of use | Hours | <30 minutes | <5 minutes | <1 minute |
| Power produced | Low | Medium | High | Very high |
| Mitochondrial density | High | High | Medium | Low |
| Capillary density | High | Intermediate | Low | Low |
| Oxidative capacity | High | High | Intermediate | Low |
| Glycolytic capacity | Low | High | High | High |
| Major storage fuel | Triglycerides | Creatine phosphate, glycogen | Creatine phosphate, glycogen | Creatine phosphate, glycogen |
| Myosin heavy chain, human genes |
MYH7 | MYH2 | MYH1 | MYH4 |
Myotome
This term is used to describe the region of the somite that contributes skeletal muscle to the embryo body. Each somite pair level gives rise to a group of skeletal muscles supplied by a specific segmental spinal nerve. The muscle arises from a specific somite and the spinal nerve arises from a specific level of the spinal cord (identified by vertebral column).
In humans this corresponds to the following spinal nerves (from top to bottom) and muscular functions:
- C3,4 and 5 supply the diaphragm for breathing.
- C5 supply shoulder muscles and muscles to bend our elbow.
- C6 for bending the wrist back.
- C7 for straightening the elbow.
- C8 bends the fingers.
- T1 spreads the fingers.
- T1 –T12 supplies the chest wall and abdominal muscles.
- L2 bends the hip.
- L3 straightens the knee.
- L4 pulls the foot up.
- L5 wiggles the toes.
- S1 pulls the foot down.
- S3,4 and 5 supply the bladder, bowel, sex organs, anal and other pelvic muscles.
Puberty
- Musculoskeletal mass doubles by the end of puberty
- regulated growth by - sex steroid hormones, growth hormone, insulin-like growth factors
- accumulation of (peak) bone mass during puberty relates to future osteoporosis in old age
Abnormalities
Additional abnormalities will be covered in the limb development lecture. see also Musculoskeletal Abnormalities
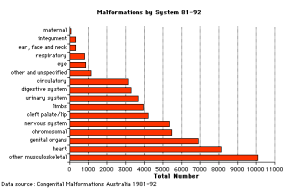
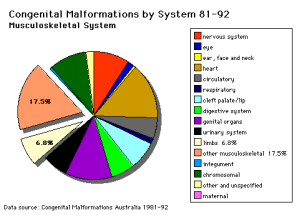
Bone
Vertebra
- Spina Bifida - neural tube failure to close, disrupts neural arch formation
- Block vertebra - failure of vertebra separation, lumbar region, chrondrification abnormality
- Klippel-Feil Syndrome - non-segmented cervical vertebra, more female
- see also scoliosis
Rib
- Accessory rib (extra rib cervical or lumbar uni- or bilateral), short-rib polydactyly syndrome (lethal, chondroplasia), pigeon chest (rib overgrowth), funnel chest (sternum depression and lower costal cartilages)
Osteogenesis Imperfecta
- brittle-bone syndrome
- abnormal collagen type I, fail to assemble triple helix, degrade imperfect collagen, leads to fragile bones
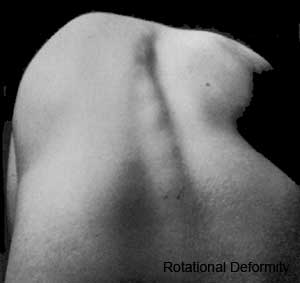
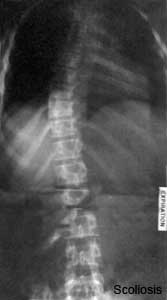
Scoliosis
- assymetric growth impairment of vertebral bodies
- lateral deviation of spine (Lateral flexion, Forward flexion, Rotation of vertebral column on long axis)
- compensated by movement of vertebral column above and below affected region (producing a primary and two secondary curves)
- progresses rapidly in adolescence and becomes fixed once bone growth is completed.
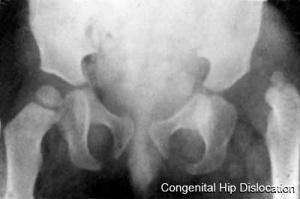
Congenital Hip Dislocation
- Instability: 1:60 at birth; 1:240 at 1 wk: Dislocation untreated; 1:700
- congenital instability of hip, later dislocates by muscle pulls or gravity
- familial predisposition female predominance
- Growth of femoral head, acetabulum and innominate bone are delayed until the femoral head fits firmly into the acetabulum
Muscle
MH - Covered in next lecture and lab.
Congenital Myopathies
Muscular Dystrophy
References
Textbooks
- The Developing Human: Clinically Oriented Embryology (8th Edition) by Keith L. Moore and T.V.N Persaud - Moore & Persaud Chapter Chapter 10 The Pharyngeal Apparatus pp201 - 240.
- Larsen’s Human Embryology by GC. Schoenwolf, SB. Bleyl, PR. Brauer and PH. Francis-West - Chapter 12 Development of the Head, the Neck, the Eyes, and the Ears pp349 - 418.
Online Textbooks
- Developmental Biology by Gilbert, Scott F. Sunderland (MA): Sinauer Associates, Inc.; c2000 Paraxial and intermediate mesoderm | Myogenesis: The Development of Muscle | Osteogenesis: The Development of Bones | Figure 14.10. Conversion of myoblasts into muscles in culture
- Molecular Biology of the Cell Alberts, Bruce; Johnson, Alexander; Lewis, Julian; Raff, Martin; Roberts, Keith; Walter, Peter New York and London: Garland Science; c2002 Search Molecular Biology of the CellBone Is Continually Remodeled by the Cells Within ItImage: Figure 22-52. Deposition of bone matrix by osteoblasts.Image: Figure 22-56. The development of a long bone.
Search
- Bookshelf mesoderm | somite | myogenesis | chondrogenesis | osteogenesis
- Pubmed mesoderm | somite | myogenesis | chondrogenesis | osteogenesis
UNSW Embryology Links
- Notes: Bone Development | Limb Development | Axial Skeleton Development | Bone Development | Skull | Development Limb | Axial Skeleton| Human Bone | Endochondral Ossification | Skeletal Muscle | Cartilage | Joints
- Lectures: ANAT2341 - Embryology 2008 - Lecture 16
- Movies: Mesoderm Movies | Somite - Myotome body wall | Vertebra
External Links
- UWA Blue Histology Skeletal Tissues - Muscle | Skeletal Tissues -Cartilage | Skeletal Tissues - Bone
- University of Kansas Histoweb Bone
- Loyola University Medical Education Network Part 9: Specialized Connective Tissue: Cartilage and Bone | Part 10: Endochondral Ossification
- UNSW Embryology Cartilage and Bone
- University of Bristol ossification
Terms
annulus fibrosus - the circularly arranged fibers (derived from sclerotome)that together with the nucleus pulposus (derived from notochord) form the intervertebral disc (IVD) of the vertebral column.
axial mesoderm - (=notochord)
cartilage - connective tissue from mesoderm in the embryo forms the initial skeleton which is replaced by bone. In adult, found on surface of bone joints.
Cbfa1 - Core-Binding Factor 1 (Runx2) transcription factor protein key to the differentiation of bone OMIM: Cbfa1
centrum - the primordium of the vertebral body formed initially by the sclerotome.
clavicle - (Latin, clavicle = little key) bone which locks shoulder to body.
dermatome -
dermomyotome - dorsolateral half of each somite that forms the dermis and muscle.
ectoderm - the layer (of the 3 germ cell layers) which form the nervous system from the neural tube and neural crest and also generates the epithelia covering the embryo.
endochondrial ossification - the process of replacement of the cartilagenous framework by osteoblasts with bone.
epaxial myotome - the dorsal portion of the myotome that generates dorsal skeletal muscles (epaxial muscles), which include other muscles associated with the vertebrae, ribs, and base of the skull.
extracellular matrix - material secreted by and surrounding cells. Consists if fibers and ground substance.
fibroblast growth factors - (FGF) a family of at least 10 secreted proteins that bind membrane tyrosine kinase receptors. A patterning switch with many different roles in different tissues. (FGF8 = androgen-induced growth factor (AIGF)
fibroblast growth factor receptor - receptors comprise a family of at least 4 related but individually distinct tyrosine kinase receptors (FGFR1- 4). They have a similar protein structure, with 3 immunoglobulin-like domains in the extracellular region, a single membrane spanning segment, and a cytoplasmic tyrosine kinase domain.
growth factor - usually a protein or peptide that will bind a cell membrane receptor and then activates an intracellular signaling pathway. The function of the pathway will be to alter the cell directly or indirectly by changing gene expression. (eg shh)
hox - (=homeobox) family of transcription factors that bind DNA and activate gene expression. Expression of different Hox genes along neural tube defines rostral-caudal axis and segmental levels.
hypaxial myotome - the ventral portion of the myotome that generates ventral skeletal muscles (hypaxial muscles) which include some vertebral muscles, the diaphragm, the abdominal muscles, and all limb muscles.
intercostal- the region between adjacent ribs, usually comprising intercostal muscles and connective tissue.
intervertebral disc- (IVD) the annulus fibrosus+nucleus pulposus together form the intervertebral disc (IVD) of the vertebral column. This is the flexible region between each bony vertebra that allows the column to be bent.
lumbar plexus - mixed spinal nerves innervating the lower limb form a complex meshwork (crossing).
mesenchymal progenitor cells - (MPCs) cells able to differentiate in various types of connective tissue, including cartilage, bone and adipose tissue.
mesoderm - the middle layer of the 3 germ cell layers of the embryo. Mesoderm outside the embryo and covering the amnion, yolk and chorion sacs is extraembryonic mesoderm.
myoblast - the undifferentiated mononucleated muscle cells that will fuse together to form a multinucleated myotube, then mature into a muscle fibre.
MyoD - transcription factor involved in the determination of muscle cells in the somite. A basic helix-loop-helix factor which binds DNA.
myotome - the portion of the dermamyotome that generates skeletal muscle. Has 2 components epaxial (dorsal muscles ) hypaxial (ventral muscles).
neural crest - cell region at edge of neural plate, then atop the neural folds, that remains outside and initially dorsal to the neural tube when it forms. These paired dorsal lateral streaks of cells migrate throughout the embryo and can differentiate into many different cell types(=pluripotential). Those that remain on the dorsal neural tube form the sensory spinal ganglia (DRG). Neural crest cells migrate into the somites.
osteoblast - The mesenchymal cells that differentiate to form the cellular component of bone and produce bone matrix. Mature osteoblasts are called osteocytes. (More? Musculoskeletal Development - Bone)
osteoclast - Cells that remove bone (bone resorption) by enzymatically eroding the bone matrix. These cells are monocyte-macrophage in origin and fuse to form a multinucleated osteoclast. These cells allow continuous bone remodelling and are also involved in calcium and phosphate metabolism. The erosion cavity that the cells lie iwithin and form is called Howship's lacuna. (More? Musculoskeletal Development - Bone)
osteocyte - The mature bone-forming cell, which form the cellular component of bone and produce bone matrix. Differentiate from osteoblasts, mesenchymal cells that differentiate to form bone. (More? Musculoskeletal Development - Bone)
osteon - The anatomical (histological) unit structure (principal structure) of compact bone. (More? Musculoskeletal Development - Bone)
Pax - name derived from Drosophila gene 'paired' (prd) the 'paired box' is a amino end 124 amino-acid conserved domain (signature aa 35-51: P-C-x(11)-C-V-S). Transcription factor of the helix-turn-helix structural family, DNA binding, and activating gene expression. In human, nine member proteins from Pax-1 to Pax-9. Regulate differentiation of many different tissues. Some members of the family (PAX3, PAX4, PAX6, PAX7) also contain a functional homeobox domain.
pedicle - (Latin, pediculus = small foot) part of the vertebral arch forming the segment between the transverse process and the vertebral body.
primary centre of ossification - the first area where bone growth occurs between the periosteum and cartilage.
sclerotome - ventromedial half of each somite that forms the vertebral body and intervertebral disc.
segmentation - to break a solid structure into a number of usually equal size pieces.
somatic mesoderm - derived from lateral mesoderm closest to the ectoderm and separated from other component of lateral mesoderm (splanchnic, near endoderm) by the intraembryonic coelom.
somite - segmental block (ball) of mesoderm formed from paraxial mesoderm adjacent to notochord (axial mesoderm). Differentiates to form initially sclerotome and dermamyotome (then dermotome and myotome).
somitic mesoderm-
somitocoel - a transient cavity that appears within each of the the early forming somites then is lost.
somitogenesis - the process of segmentation of the paraxial mesoderm to form "mesoderm balls" beginning cranially (humans day20) and extending caudally at 1 somite/90 minutes until approx. 44 pairs have been formed.
sonic hedgehog - (=shh) secreted growth factor that binds patched (ptc) receptor on cell membrane. SHH function is different for different tissues in the embryo. In the nervous system, it is secreted by the notochord, ventralizes the neural tube, inducing the floor plate and motor neurons. In the Limb it is secreted by the zone of polarizing activity (ZPA) organizing limb axis formation.
Tbx - T-box genes (transcription factor) involved in mouse forelimb (Tbx4) and hindlimb (Tbx5) specification.
transcription factor- a factor (protein or protein with steroid) that binds to DNA to alter gene expression, usually to activate. (eg steroid hormone+receptor, Retinoic acid+Receptor, Hox, Pax, Lim, Nkx-2.2).
vertebral body- formed by centrum, vertebral arch, facets for ribs. It is the mature vertebral structure formed by the 5 secondary ossification centers after puberty.
vertebral column - name given to the complete structure formed from the alternating segments of vertebra and intervertebral discs which support the spinal cord.
vertebral foramen - the dorsal cavity within each vertebra, generated by the vertebral arch that surrounds the spinal cord.
Wnt7a - The designation 'Wnt' was derived from 'wingless' and 'int'. The Wnt gene was first defined as a protooncogene, int1. Humans have at least 4 Wnt genes: Wnt7a gene is at 3p25 encoding a 349aa secreted glycoprotein. A patterning switch with different roles in different tissues. The mechanism of Wnt distribution (free diffusion, restricted diffusion and active transport) and all its possible cell receptors are still being determined. At least one WNT receptor is Frizzled (FZD). The Frizzled gene family encodes a seven-transmembrane receptor.
Images
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Course Content 2010
Embryology Introduction | Cell Division/Fertilization | Lab 1 | Week 1&2 Development | Week 3 Development | Lab 2 | Mesoderm Development | Ectoderm, Early Neural, Neural Crest | Lab 3 | Early Vascular Development | Placenta | Lab 4 | Endoderm, Early Gastrointestinal | Respiratory Development | Lab 5 | Head Development | Neural Crest Development | Lab 6 | Musculoskeletal Development | Limb Development | Lab 7 | Kidney | Genital | Lab 8 | Sensory | Stem Cells | Stem Cells | Endocrine | Lab 10 | Late Vascular Development | Integumentary | Lab 11 | Birth, Postnatal | Revision | Lab 12 | Lecture Audio | Course Timetable
Cite this page: Hill, M.A. (2024, April 18) Embryology 2010 Lecture 13. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/2010_Lecture_13
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G