2010 Group Project 4
Percutaneous Umbilical Cord Blood Sampling
Introduction
Percutaneous Umbilical Blood Sampling (PUBS) is an invasive pre-natal diagnostic procedure performed during the second trimester (between week 18 to 22) where a sample of fetal blood is extracted from the umbilical vein in the umbilical cord using a fine needle via the abdomen of the mother. The extracted blood can then be used to detect certain anomalies including chromosome abnormalities such as Down Syndrome, blood disorders such as Fetal Haemolytic Disease and intrauterine infection, growth retardation, and some birth defects as well as metabolic disorders. PUBS is often used when other diagnostic tests such as Ultrasound, Amniocentesis and Chorionic Villus Sampling do not yield conclusive results. This pre-natal diagnostic technique is also used to deliver certain therapies such as the administration of medicine and transfusion of blood directly to the fetus.
Although it is a very useful diagnostic technique, there are many complications associated with the procedure from haemorrhage and fetal bradycardia to premature birth and fetal death. The mortality rate associated directly to procedural factors has been found to be approximately 1 to 2 times out of every 100 procedures. The long list of associated risks have been found to be related to procedural factors such as duration and the number of punctures as well as individual circumstances of the patient for example gestational age.
Despite the risks involved, the one of the benefits of PUBS over that of other pre-natal diagnostic techniques such as Amniocentesis and Chorionic Villus Sampling (CVS), is that genetic information also known as Karyotypes is available much sooner after the procedure. This is especially important in cases requiring rapid diagnosis and/or management.
When is PUBS Performed?
PUBS is an invasive procedure and as a result, it carries with it a relatively high risk of complications. Therefore, it is generally to be used in the case of high-risk pregnancies.
A high-risk pregnancy is classified as such due to various factors that indicate a significantly increased likelihood of genetic defects. These may include:
- An advanced maternal age of 35 and over
- A previous pregnancy affected with chromosomal disorder
- Family history of genetic disorders (E.g. monogenic disease carrier status or balanced chromosomal translocation in a parent, history of X-linked or inborn metabolic disorders etc.)
- Abnormal results identified on a previously performed non-invasive procedure, such as ultrasound or maternal serum biochemistry screening [1]
PUBS in comparison with other diagnostic techniques
PUBS is usually performed after non-invasive procedures such as ultrasound and biochemical markers, have indicated the possibility of genetic disorders. Because, these tests generally produce highly sensitive results, they are not always reliable at giving an accurate diagnosis. Therefore, an invasive technique such as PUBS is employed to in an attempt to provide more conclusive and accurate information.[2]
PUBS may also be used when other invasive pre-natal diagnostic tests including chorionic villi sampling (CVS) and amniocentesis do not yield conclusive results. These methods are similar in that they involve the examination of cell samples obtained directly from the developing fetal structures.
| PUBS | Chorionic Villi Sampling | Amniocentesis | |
|---|---|---|---|
| risk of complications | 1-2% | 2% | 0.5-1% |
| recommended time period for testing | 18-23 weeks | 8-11 weeks | 16-18 weeks |
| available diagnostic analyses | karyotype and DNA analysis, biochemical studies, detection of blood disorders and intrauterine infections. unable to detect neural tube defects. | karyotype and DNA analysis, enzyme studies. least accurate in cytogenic analysis. | karyotype and DNA analysis, biochemical studies |
| time taken for samples to be cultured | 72 hours | 9-10 days | 10-11 days |
Advantages of PUBS:
- Accurate at detecting the presence of genetic disorders
- Sample is available for many different types of analysis, which allows for the detection of a wide range of defects
- Results are available relatively soon after procedure has taken place
Disadvantages of PUBS:
- Unable to accurately detect the severity of disorders
- Takes place only later in pregnancy
- Recognised as posing potential risks
- Unable to detect neural tube defects
History
Brief Timeline of Percutaneous Umbilical Blood Sampling (PUBS)
- 1964 - History of the Pre-natal Diagnostic Technique Percutaneous Umbilical Blood Sampling begins with the description of a hysterotomy with extra uterine umbilical transfusion of a hydropic fetus by V. J. Freda and S. K. Adamson
- 1972 - C. Valenti uses a 5mm needlescope which he modified from an 18 French pediatric cystoscope and which he called an endoamnioscope and ultrasound guidance to obtain a fetal biopsy specimen.
- 1974 - J.E Patrick, T.B Perry and R.A.H Kinch give a detailed description of the percutaneous placement of a 1.7mm fetoscope
- 1980 - C.H. Rodeck reports on 133 fetoscopic procedures performed using the fetal blood sampling technique.
- 1981 - Again C.H. Rodeck reports on his experiences while performing a fetoscopically guided intravascular transfusion between 23 to 25 weeks’ of gestation
- 1982 - J. Band, J.E. Bock and D. Trolle recognize the limitations of fetoscopy and thus turn and perform an ultrasound guided percutaneous transfusion into the fetal hepatic vein at 30 weeks of gestation.
- 1983 - A team under F. Daffos in France publish a description of fetal blood sampling by ultrasound guided puncture of the umbilical vein, at the point the cord inserts into the placental with the use of a 20mm gauge needle.
- 1984 - K. Nicolaides develops single operator method for Percutaneous Umbilical Blood Sampling
- 1985 - J.C. Hobbin and a group at Yale describe this technique and call the procedure Percutaneous Umbilical Blood Sampling (PUBS)
- 1988 - C. H Rodeck at the Charlotte's Maternity Hospital in London first described fetal blood sampling from the intrahepatic portion of the umbilical vein in the fetus as an alternative procedure where the cord needling was unsuccessful.
Key Scientist and Doctors in Percutaneous Umbilical Blood Sampling
Fernand Daffos
Fernand Daffos and a team of doctors such as François Forestier and Martine Capella-Pavlovsky in 1982 developed a new and improved technique for the collection of fetal blood samples. The new and improved technique for collection of pure samples of fetal blood were obtained from the umbilical cord more precisely the large vein using a twenty-gauge spinal needle that was guided by real time ultrasound images. Fetal blood was collected from the cord approximately 2.5cm from the connection to the placenta into a syringe which is attached to the need where 1 to 2 millilitres of blood is collected. Fernand Daffos’s procedure was a dramatic improvement in fetal blood collection compare to other methods for prenatal diagnosis of disease.
Professor Stuart Campbell
In 1982 Professor Campbell aside from looking at fetal malformation using real time ultrasound started systematic investigation in many other areas, pioneering work in areas such as ovarian cancer screening with ultrasound, Doppler fetal and utero-placental blood flow in many pre-natal pathological conditions. Stuart Campbell also investigated ovarian follicular developments, routine ultrasound population screening and umbilical and placental blood sampling. Yet most importantly Professor Stuart Campbell introduced the concept of actually screening for the later development of pre-eclampsia and intra-uterine growth retardation basing on early uteroplacental waveforms.
Kypros Nicolaides
Kypros Nicolaides was one of the first doctors that discarded the fetoscope and practiced all blood sampling procedures by extracting blood from the placental cord insertion which was then termed Percutaneous Umbilical Blood Sampling . Like stated above the technique of Percutaneous Umbilical Blood Sampling or Cordocentsis was initially pioneered in France in 1983 by Fernand Daffos yet it was Kypros Nicolaides that actually developed the single operator method. This allowed him and many other doctors to study many aspects of fetal physiology and pathophysiology such as fetal blood gases. The single operator method developed also allowed Nicolaides to investigate the correlations between fetal blood gases and Doppler, fetal metabolism, endocrinology, immunology, haematology, biochemistry in diabetic pregnancies.
Procedure
Percutaneous Umbilical Cord Sampling (PUBS) is the performed by the advancement of a needle within a ultrasound visual field to a targeted puncture site and consists of three fundamental steps.
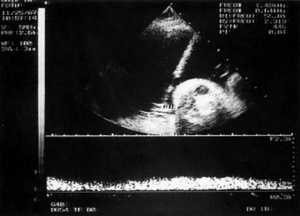
Step 1 - Imaging
An advanced imaging ultrasound is used to determine the location of where the umbilical cord inserts into the placenta. This ultrasound image is then used throughout the procedure in order to guide a thin needle through the abdomen and uterine wall of the mother and into the the umbilical vein running through the cord.
Step 2 - Retrieval of Fetal Blood Sample
The needle is then inserted into the cord to retrieve a small sample of fetal blood. There are two main routes for the retrieval of fetal blood. The method used to perform the procedure is determined by the position of the placenta in the uterus and point of connection with the umbilical cord. The ideal sample site for PUBS is located at the root of the umbilical cord due to its stable fixed position which is less susceptible to disturbances caused by fetal movement compared to the free loops of the cord.
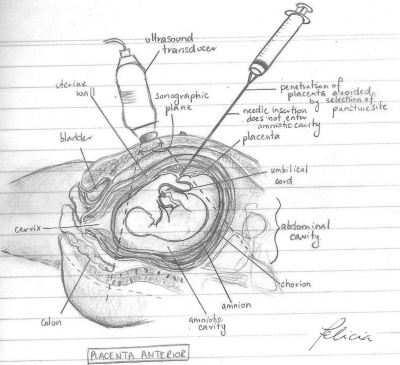
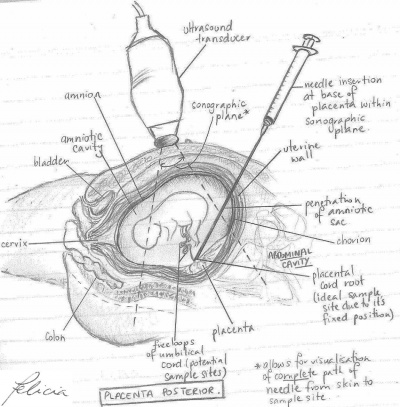
| Placenta Anterior | Placenta Posterior | |
| Description | Placenta attached to anterior wall of uterus - the needle is inserted straight into the umbilical cord without penetrating the amnion and amniotic cavity | Placenta located on posterior wall of uterus - the needle must travel through the amniotic sac to reach the umbilical cord. This may cause some temporary bleeding and cramps |
| Diagram |
There are two techniques that can be used when obtaining the sample: freehand and needle-guided. The choice of technique is dependent on a number of factors including the location of the cord root and the preferences of the physician performing the procedure.
1. Freehand - allows lateral readjustment of needle direction once within the uterus. A transducer is used to navigate the needle to the specific sample site and is the more preferred technique due to the increased range of movement
2. Needle-guided - involves the insertion of a separate needle straight into the targeted puncture site with the aid of the transducer, which forms a fixed passage through with a second smaller needle passes to retrieve the fetal blood. Despite permitting precise alignment of the needle tract with the vessel, the range of movement is limited to a single plane of travel
[5]
It is also important to note when performing PUBS, that if the mother is Rh–negative, Rh Immune-Globulin (RhIG) is administered to the mother in order to prevent the development of Rh incompatibility and further sensitization.
Step 3 - Sample Analysis
The fetal blood sample is sent to a lab where it is screened for genetic defects and other disorders. Prior to this, in order to confirm the the sample obtained is fetal blood, the Kleihauer—Betke test performed. [7] The results for the test are usually available within 72 hours however under some circumstances, may take a few weeks to obtain the results. In the event of diagnosis, implementation of the most suitable procedure for management of the condition occurs or in extreme cases, the pregnancy is terminated.
Percutaneous Umbilical Blood Sampling Procedure Animation
Disorders and Abnormalities Found by PUBS
Percutaneous Umbilical Blood Sampling also known as Cordocentesis like stated above is a pre-natal diagnostic test that is usually preformed to detect abnormalities such as Trisomy 21 (Down Syndrome) and Trisomy 18 (Edwards Disease) and blood disorders for example Fetal Hemolytic Disease. Yet on the whole Cordocentesis may be performed to help diagnose any of the concerns listed below:
- Fetal anemia
- Malfunction of the fetus
- Isoimmunisation
- Fetal platelet count of the mother
- Fetal infections like rubella or toxoplasmosis
- Respiratory illnesses
- Congenital heart defects
Yet one major disadvantage when comparing Percutaneous Umbilical Blood Sampling to other major testing method for example Choronic Villi Sampling (CVS) and Amniocentesis is that PUBS does not help test for neural tube defects such as Spina Bifida
Associated Risk and Complications
As mentioned earlier, PUBS is an invasive diagnostic procedure which carries a number of risks and complications which are associated with a number of factors from procedure-related, experience of the staff performing the procedure to gestational age. However the risks involved in each case varies according to the indications of the procedure. For example, fetuses which are structurally abnormal or had growth deficiencies were found to be more susceptible to the associated risks and complications of PUBS.[8] Some of the main risks include:
- Transient bleeding of the umbilical cord at the puncture site is common and occurs in approximately 20% of cases. Often the bleeding spontaneously stops within a short time period (within 1 minute) while in a small number of cases, continued bleeding may prove fatal especially for those with blood disorders i.e. alloimune thrombocytopenia
- Transient fetal bradycardia - where the heart rate of the fetus falls below 100bpm is also a common complication (about 8% of cases) has been found to occur during or immediately after PUBS was performed. This occurs due to the puncture causing changes in the circulation and/or inducing reflexes and release of substances within the fetal circulation. In most cases, short term changes in fetal heart rate during PUBS has not reported long term fetal injury except for when there are underlying fetal disorders. Manual compression through the maternal abdomen is currently the preferred method of fetus revival [9]
- Failure to obtain a sample is also a complication occurring in a small number of cases which may require further PUBS procedures that could potentially increase the likelihood of fetal distress and preterm labour
- Preterm labour may be induced upon which the medical team overseeing the procedure must be prepared to perform an immediate emergency caesarean delivery
- Fetal loss reported to occur in less than 2% of cases is attributed to a number of factors including procedural time, gestational age (those earlier in pregnancy due to the size of the fetus are believed to be at higher risk of procedure-related injury), underlying medical conditions, expertise of the operator, pregnancy complications and fetal movement [10]
Reasons For and Against the Use of Percutaneous Umbilical Blood Sampling
The reason for individuals to test or not to test using PUBS actually vary between each and every person with the individual's physicians also a playing a major role in the decision.
Performing this pre-natal diagnostic test and thus confirming diagnoses provide the parent or parents with certain opportunities that would not be available if test was not pursued. These include:
- Pursue potential medical intervention that may exist
- Begin planning for a child with special needs
- Addressing anticipated lifestyle changes
- Most importantly make a decision about whether or not to carry the child to term
However some individuals may choose not to pursue percutaneous umbilical blood sampling (PUBS) or any other addition pre-natal diagnostic tests for various reasons such as:
- The parent or parents are comfortable with result no matter the result
- Personal, moral or religious values of the individual which prevents a decision about carrying the child to term from being a viable option
- Some parents choose not to allow any testing that poses any risk of harming the developing baby
Yet it is important to discuss the risk and benefits of testing thoroughly with the individual’s healthcare professional or physician. The physician should help the individual evaluate if the benefits from the result could outweigh any risk from the procedure.
The Future of Percutaneous Umbilical Cord Sampling
It has been stated by many senior medical professionals that the Percutaneous Umbilical Blood Sampling will suffer the same fate as fetoscopy unless the indications or reasons for performing cordocentesis is gradually refined, limiting the practice of this test for when other pre – natal diagnostic techniques and genetic technologies do not yield conclusive results.
Yet it has been through the two decades that PUBS has been available we have been given the opportunity to extend your knowledge on the fetus by contributing to our understanding of human fetal physiology, metabolism and disease. The usage of PUBS has also allowed us to correlate blood gas data with Doppler as well as fetal heart rate patterns.
However, molecular genetics have shrunk the usage and the role of PUBS for prenatal diagnosis of hereditary diseases and the introduction of cytogenetic techniques have made inroads that actually displaces the need for blood sampling to obtain a rapid karyotype. Thus it can safely be said that it is likely that there will be less incidences where PUBS will be used in years to come. Yet PUBS will demand recognition as it will maintain and also further the knowledge base or fetal physiology and diseases.
Useful Links
Search Bookshelf Percutaeous Umbilical Cord Sampling
Search Pubmed Now: Percutaeous Umbilical Cord Sampling
References
- ↑ <pubmed>18292841</pubmed>
- ↑ <pubmed>8907774</pubmed>
- ↑ <pubmed>18292841</pubmed>
- ↑ <pubmed>20193481</pubmed>
- ↑ <pubmed>8739583</pubmed>
- ↑ Henderson, J, Weiner, C, Glob. libr. women's med.,(ISSN: 1756-2228) 2008; DOI 10.3843/GLOWM.10212
- ↑ <pubmed>16530195</pubmed>
- ↑ <pubmed>9793976</pubmed>
- ↑ Henderson, J, Weiner, C, Glob. libr. women's med.,(ISSN: 1756-2228) 2008; DOI 10.3843/GLOWM.10212
- ↑ <pubmed>16530195</pubmed>
Glossary
Amnion: An extraembryonic membrane ectoderm and extraembryonic mesoderm in origin and forms the innermost fetal membrane, produces amniotic fluid.
Amniotic Cavity: The fluid-filled (amniotic fluid) extraembryonic coelom (cavity) formed initially by epiblast and then ectoderm and surrounding extraembryonic mesoderm. In humans, it forms the innermost fetal membrane, produces amniotic fluid expanding to fuse with the chorionic membrane during week 8 of development.
Ultrasound: A non-invasive technique for visualizing and prenatal diagnosis of several features of development including: follicles in the ovaries, the gestational sac, fetus in the uterus, fetal parameters, and the placenta. The technique uses high-frequency sound waves that are reflected off internal structures.
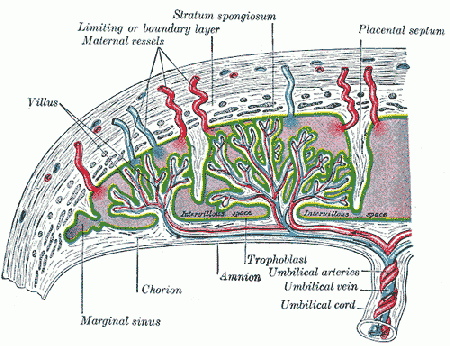
Umbilical Cord: (placental cord) The placental cord is the structure connecting the embryo/fetus to the placenta. It is initially extra-embryonic mesoderm forming the connecting stalk within which the placental blood vessels (arteries and veins) form. In human placental cords the placental blood vessels are initially paired, later in development only a single placental vein remains with a pair of placental arteries. This structure also contains the allantois, an extension from the hindgut cloaca then urogenital sinus. Blood collected from the placental cord following delivery is a source of cord blood stem cells.
2010 ANAT2341 Group Projects
Project 1 - Ultrasound | Project 2 - Chorionic villus sampling | Project 3 - Amniocentesis | Group Project 4 - Percutaneous Umbilical Cord Blood Sampling | Project 5 - Fetal Fibronectin | Project 6 - Maternal serum alpha-fetoprotein | Group Assessment Criteria
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 23) Embryology 2010 Group Project 4. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/2010_Group_Project_4
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G