2010 BGD Practical 3 - Week 3 Summary
Practical 3: Oogenesis and Ovulation | Gametogenesis | Fertilization | Early Cell Division | Week 1 | Implantation | Week 2 | Extraembryonic Spaces | Gastrulation | Notochord | Week 3 | Quiz
Introduction
This page is a overview of events that occur in human development up to week 3 post-fertilization. From this Practical understand concepts of: fertilization, blastocyst development, implantation, bilaminar and trilaminar embryo formation, development of embryonic cavities and brief understanding of early placenta development.
By the end of week 3, segmentation of the trilaminar embryo 3 germ layers has begun:
- Ectoderm - central neural plate and lateral parts form epidermis
- Mesoderm - midline notochord, adjacent somites, formation of the internal embryonic space (intraembryonic ceolom)
- Endoderm - epidermal lining of gastrointestinal tract and yolk sac lining
Note
Use the links to Carnegie stage 8 and Carnegie stage 9 to see a number of different views of the human embryo in the third week of development.
The timeline at the bottom of this page should give you a better perspective of the sequence of early developmental events. You would not be expected to know exact days (as they are only approximate anyway) it is more important to get the weeks and sequence right.
Carnegie Stage 8
Facts
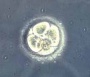
Human embryonic stage 8 occurs during week 3 between 17 to 19 days.
The embryo is now 1.0 - 1.5 mm in size.
Events
Gastrulation is continuing as cells migrate from the epiblast, continuing to form mesoderm.
Mesoderm lies between the ectoderm and endoderm as a continuous sheet except at the buccopharyngeal and cloacal membranes. These membranes have ectoderm and endoderm only and will lie at the rostral (head) and caudal (tail) of the gastrointestinal tract.
From the primitive node a tube extends under the ectoderm in the opposite direction to the primitive streak. This tube forms first the axial process then notochordal process, then finally the notochord.
The notochord is a key to embryonic folding and regulation of ectoderm and mesoderm differentiation. It lies in the rostrocordal axis and the embryonic disc will fold either side ventrally, pinching off a portion of the yolk sac to form the lining of the gastrointestinal tract.
Identify
- embryonic disc
- primitive node, primative streak, primative groove
- connecting stalk
- cut amniotic membrane
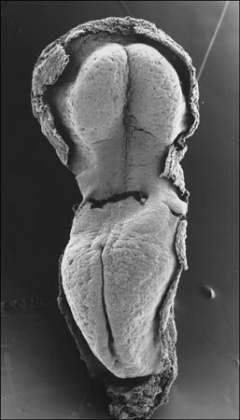
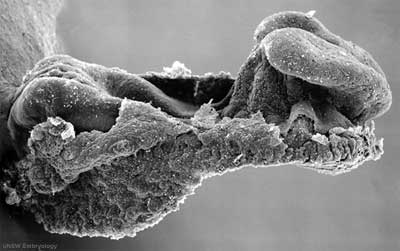
Carnegie Stage 9
Facts
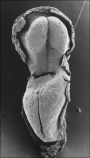
Human embryonic stage 9 occurs during week 3 between 19 to 21 days.
The embryo is now 1.5 to 2.5 mm in size and somites have begun to form and number between 1 to 3 somite pairs during this stage.
The initial images are displayed unlabeled to allow you to explore the embryo for yourself, linked labeled versions are also available for some images.
Events
Ectoderm - Neural plate brain region continues to expand, neural plate begins folding over the notochord. Gastrulation continues through the primitive streak region.
Mesoderm - Paraxial mesoderm segmentation into somites begins (1 - 3 somite pairs). Lateral plate mesoderm begins to vacuolate, dividing it into somatic and splanchnic mesoderm and to later form the intra-embryonic coelom. Prechordal splanchnic mesoderm begins to form the cardiogenic region, from which the primordial heart will develop.
Endoderm - Notochordal plate still visible which will form the notochord. Endoderm is still widely open to the yolk sac and germ cells form part of this layer. Extra-embryonic mesoderm on the yolk sac surface begins to form "blood islands".
Identify
- Neural groove and neural folds, the mesoderm, which segments beside the neural groove to form somites but extends laterally to margin of embryonic disc lateral plate mesoderm, where it merges with the covering extraembryonic mesoderm.
- The intra-embryonic coelom develops in the middle of the lateral plate mesoderm. Note amniotic ectoderm covered by extra-emebryonic mesoderm (empty spaces above and below the mesoderm are artefacts, as are the lateral folds in the ectoderm).
The first two images using bright field microscopy approximate the orientation of the scanning electron micrographs below. There are additional scanning electron micrographs showing selected features in detail.
- Carnegie Stages: 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | 15 | 16 | 17 | 18 | 19 | 20 | 21 | 22 | 23 | About Stages | Timeline
Human Development Timeline
The table below shows human development features and approximate timing during the menstrual cycle to fertilization and the first 3 weeks of development.
The timing assumes fertilization the day after ovulation and the "weeks" refer to embryonic development and differ from clinical weeks (shown in brackets, from last menstrual period) and "stages" refer to Carnegie stages of development.
Week -2
(Clinical Week 1)
| Event | ||
| Menstrual Phase |
Menstrual Cycle changes: Uterine endometrium (loss), Ovary (Follicle Development) | |

| ||
| Proliferative Phase |  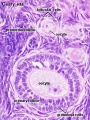 Menstrual Cycle changes: Uterine endometrium (proliferation), Ovary (Follicle Development) Menstrual Cycle changes: Uterine endometrium (proliferation), Ovary (Follicle Development)
| |
Week -1
(Clinical Week 2)
| Menstrual cycle | Event | |
| Proliferative Phase | ||
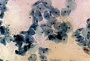 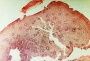 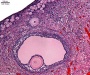  Menstrual Cycle - Mid proliferative Menstrual Cycle - Mid proliferative
| ||
   Menstrual Cycle - Late Proliferative Menstrual Cycle - Late Proliferative
| ||
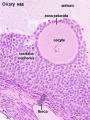
| Ovulation
Capacitation |
 |
Week 1
Week 1 (Clinical Week 3)
Week 2
Week 2 (Clinical Week 4)
| Event | ||
| Stage 6 | ||
Week 3
Week 3 (Clinical Week 5)
| Event | ||
| Stage 7 |  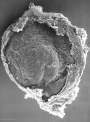 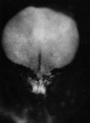
| |
| Stage 8 | 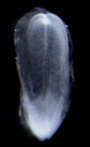 | |
| Stage 9 | 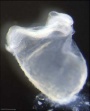 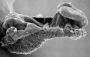 Musculoskeletal somitogenesis, first somites form and continue to be added in sequence caudally Musculoskeletal somitogenesis, first somites form and continue to be added in sequence caudally
Neural the three main divisions of the brain, which are not cerebral vesicles, can be distinguished while the neural groove is still completely open Neural Crest mesencephalic neural crest is visible PMID: 17848161 | |
| Heart cardiogenesis, week 3 begins as paired heart tubes. |
Next
Finished Lab 3 !
If you have finished and would like to apply your knowledge, I have also included some Clinical Questions based around this period of development.
If you have finished and need some more help understanding this period of development, I have included some links to Online References.
If you have finished and are interested in looking at tissues involved in this period of development, I have included some links to Histology Images.
Note that this Practical has discussed mainly development of the embryo as placental development will be covered in detail in another practical (Practical 8 - Placenta and Fetal Membranes).
The next Practical will continue on through embryonic development (Practical 6 - Implantation to 8 Weeks).
Terms
The selected list of terms below are extracted from the UNSW Embryology Glossary. The full list of glossary terms should be used for any new terms not listed below.
acroplaxome
The sperm structure which forms the acrosome plate with intermediate filament bundles of the marginal ring at the leading edge of the acrosome.
(More? Spermatogenesis | Fertilization)
acrosin
A spermatazoa acrosomal protein has a role in [F.htm#fertilization fertilization] including that of lysis of the zona pellucida (a serine protease) and in secondary zona pellucida (ZP) binding. Stored in mature spermatazoa as proacrosin.
(More? Spermatogenesis | Fertilization | OMIM Entry)
acrosome
The spermatazoa cellular structure containing a packet of enzymes located that allows it to dissolve a hole in the specialized extracellular matrix ([Z.htm#zona_pellucida zona pellucida], egg coat) surrounding the oocyte (egg). This enzymic digestion then allows the spermatazoa to penetrate and fertilize the egg. This structure is formed from the normal cellular organelle the [G.htm#golgi Golgi apparatus].
(More? Spermatogenesis | Fertilization)
acrosome reaction
The chemical change that enables release of acrosomal contents and allow a sperm to penetrate an egg.
(More? Spermatogenesis | Fertilization)
adnexa
(Latin, adnexae = appendages) Term used to describe any anatomical appendage (accessory structure, extension or outgrowth from the body). In reproductive anatomy used to describe appendages of the [U.htm#uterus uterus] "body"; ovaries, uterine tubes and uterus supporting ligaments.
Artificial Insemination
(AI) Fertility treatment, using placement of a sperm sample inside the female reproductive tract that can be carried out by a number of different techniques: intracervical insemination, intrauterine insemination, intratubal insemination.
(More? Week 1 Notes)
amenorrhea
The absence of a menstrual period, it can be either primary (not yet had a period by age 16) or secondary (regular period that has now stopped for 3 months).
(More? Human Menstrual Cycle)
androgens
The male sex hormones, eg testosterone.
(More? Genital System - Male)
aneuploidy
Term used to describe an abnormal number of chromosomes mainly (90%) due to chromosome malsegregation mechanisms in maternal meiosis I.
(More? Trisomy 21 | Meiosis)
antral follicle
(secondary follicle) Term used to describe the developmental stage of ovarian follicle development following preantral (primary) in describing the sequence (primordial, preantral, antral) of follicle development within the ovary. In humans, a number of primordial follicles will begin to develop into primary follicles, some of which will then form antral follicles (secondary), with only a single antral follicle developing into the ovulating follicle (Graafian) each menstrual cycle.
(More? Week 1 - Oogenesis)
antrum
(Latin from Greek, antron = a cave, cavity; a nearly-closed cavity or bulge). Identified anatomically in many structures (ovarian follicle, bone, cardiac, gastric). In the ovary this refers to the follicular fluid-filled space within the follicle.
(More? Week 1 - Oogenesis)
ART
acronym for Assisted Reproductive Technology. All treatments or procedures that involve the handling of human eggs and sperm for the purpose of helping a woman become pregnant. Types of ART include in vitro fertilization, gamete intrafallopian transfer, zygote intrafallopian transfer, embryo cryopreservation, egg or embryo donation, and surrogate birth.
(More? Week 1 - In Vitro Fertilization)
ART cycle
A process in which 1) an ART procedure is carried out, 2) a woman has undergone ovarian stimulation or monitoring with the intent of having an ART procedure, or 3) in the case of frozen embryos, embryos have been thawed with the intent of transferring them to a woman. A cycle begins when a woman begins taking fertility drugs or having her ovaries monitored.
(More? Week 1 Notes)
atresia
(Greek, a = without + tresis = perforation) Term used for anatomical closing or absence of a cavity or opening that should exist. Used as an antomical, pathological and clinical term: esophageal atresia, biliary atresia, duodenal atresia, jejunal atresia, choanal atresia, vaginal atresia, urethral atresia, pulmonary atresia, bronchial atresia, tricuspid atresia.
atretic follicle
An ovarian follicle that fails to mature and degenerates. Also called "atresia" referring to the process of degeneration of the ovarian follicle. At any one time the majority of follicles are destined not to complete maturation and degeneration can occur at any stage (from type 4-7).
(More? Week 1 Notes | Ovary Notes)
Balbiani body
(mitochondrial cloud) A collection of cell organelles (mitochondria, ER, and granulofibrillar material) asymmetrically located beside the nucleus in very young oocytes in some species. Appears similar to germinal granule precursors seen some species that contain a definitive germ plasm (flies, worms, and frogs).
(More? PNAS - Mouse oocytes within germ cell cysts and primordial follicles contain a Balbiani body)
Bulbourethral Gland
(= Cowper's Gland) A male genital tract gland which secretes a small amount of a thick clear mucous fluid prior to ejaculation, the alkaline content apparently buffers acidity of the urethra. The equivalent female gland are Bartholin's glands.
(More? Urogenital Notes)
Call-Exner bodies
A feature seen in the developing ovarian follicle granulosa layer of some species, including human. Appears as a spherical space staining as an eosinophilic region and contains basal lamina components (type IV collagen and laminin) similar to thiose of the follicular basal lamina.
(More? Week 1 - Oogenesis)
centriole
A pair of small cylindrical structures each about 0.2 micron in diameter and 0.4 micron long, that lie at right angles to one another; present at each pole of the mitotic spindle in animal cells and in some other eukaryotes.
ciliated epithelium
(Latin, cilium = eyelid) An epithelium named on the basis of the cells having surface hair-like appearance of a cilium; singular, cilium. In many tissues, cilia are found as epithelial cell apical surface motile specializations. In the uterine tube epithelium, after ovulation used to move the unfertilized egg, then the fertilized zygote, then blastocyst during the first week of development.
clomiphene citrate
(CC) A fertility drug taken orally to promote the process of follicle/egg maturation in superovulation therapy. (CC) an anti-estrogen (MRL-41) therapy for WHO group II (eu-oestrogenic) infertility associated with polycystic ovary syndrome. Used for more than 40 years it is a simple, cheap treatment, with low side effects and yields a 25% live birth rate. Alternative therapeutics being considered are metformin, aromatase inhibitors and low-dose FSH.
(More? Greenblatt RB, Barfield WE, Jungck EC, Ray AW. Induction of ovulation with MRL/41. Preliminary report. JAMA. 1961 Oct 14;178:101-4. | Homburg R. Clomiphene citrate--end of an era? A mini-review. Hum Reprod. 2005 Aug;20(8):2043-51.) | Notes - Ovary | Week 1 - In Vivo Fertilization | Week 1 - In Vitro Fertilization | Week 1 - Abnormalities)
cumulus oophorus
(Latin cumulus = a little mound G. oon = egg + phorus = bearing) The granulosa cells that form a column of cells that attaches the oocyte to the antral follicle wall within follicles of the ovary. This column of cells is broken or separates during ovulation to release the oocyte from its follicle attachment. Other granulosa cells within the follicle include: membrana granulosa and [#corona_radiata corona radiata].
(More? Week 1 - Oogenesis)
DAX1
Acronym for "D"osage sensitive sex reversal (DSS), "A"drenal hypoplasia congenita (AHC) critical region on the "X" chromosome, gene "1" , (gene NR0B1) is a nuclear hormone receptor involved in female ovary development.
(More? Urogenital Notes | OMIM Entry DAX1)
DAZL
Acronym for DAZ-like due to homology to DAZ (Deleted in AZoospermia), a gene on the long arm of the Y chromosome that is frequently deleted in infertile men with nonobstructive azoospermia.
(More? Spermatogenesis | OMIM Entry DAZL)
DET
Acronym for Double-Embryo Transfers, two embryos transferred when women undergo Assisted Reproduction Technology compared to single-embryo transfer (SET).
(More? Week 1 - In Vitro Fertilization)
ductuli efferentes
testis (male gonad) series of tubular structures which arise from the rete testis and conduct spermatazoa into the ductus epididymidis. Their columnar epithelium lining consisting of both absorptive and ciliated cells (giving rise to "cogwheel appearance) which removes much of the fluid associated with the spermatazoa leaving the testes (also by the upper epididymis) thereby increasing the spermatazoa concentration. (Spermatozoa Duct Pathway: seminiferous tubule‚ straight tubule‚ rete testis‚ ductuli efferentes‚ ductus epididymidis‚ ductus deferens)
(More? Spermatogenesis | Genital - Male | Genital Notes)
ductus epididymidis
(epididymidis) The male testes tubular structure which arise from the ductuli efferentes and conduct spermatazoa into the ductus deferens (vas deferens). The long duct is lined by a tall pseudostratified columnar epithelium.
(More? Genital - Male | Genital Notes)
dysmenorrhoea
A period pain which can be primary (increased sensitivity to the prostaglandins) or secondary (pathological), can be common with no associated abnormality or in association with ovarian cysts or endometriosis.
(More? Human Menstrual Cycle)
ectopic pregnancy
(Greek, ektopos = out of place) A pregnancy in which the fertilized egg implants outside of the [U.htm#uterus uterus] usually in the fallopian tube, but also on the ovary, or the abdominal cavity. Ectopic pregnancy is a dangerous condition that must receive prompt treatment.
(More? Week 2 - Abnormalities)
egg
([O.htm#oocyte oocyte] or ovum) An alternative term used to describe the haploid female reproductive cell Germ Cell). The term is also used to describe the avian and reptilian shell enclosed structure.
(More? Week 1 Notes | Chicken Development | Frog Development)
egg retrieval
(also called oocyte retrieval) A clinical in vitro fertilization (IVF) procedure to collect the eggs contained in the ovarian follicles.
(More? Week 1 - In Vitro Fertilization)
egg transfer
(also called oocyte transfer) A clinical in vitro fertilization (IVF) technique to transfer of retrieved eggs into a woman's fallopian tubes through [L.htm#laparoscopy laparoscopy]. This procedure is used only in gamete intrafallopian transfer (GIFT) (see definition).
(More? Week 1 - In Vitro Fertilization)
embryo
(Greek, en = in + bryein = to be full of) An egg that has been fertilized by a sperm and undergone one or more divisions. Also the set of early developmental stages in which a plant or animal differs from its mature form.
(More? [h.htm#human_embryo human embryo])
embryo transfer
Placement of an embryo or embryos into a woman's [U.htm#uterus uterus] through the cervix after in vitro fertilization (IVF) or in the case of zygote intrafallopian transfer (ZIFT) (see definition), into her fallopian tube.
(More? Week 1 Notes)
endocrine gland
(Greek, endon = within) A gland (organ, tissue) that is specialized for secretion of a hormone into the bloodstream for general circulation.
(More? Endocrine Notes)
endometrial gland
The mucous secreting gland associated with the epithelium lining the [U.htm#uterus uterus]. These glands develop and secrete each menstral cycle and are thought to provide initial blastocyst nutrition prior to implantation.
(More? Week 1 Notes)
endometriosis
Endometrium found incorrectly located possibly in the muscular layer of the [U.htm#uterus uterus]. Can also be seen as the presence of tissue similar to the uterine lining in locations outside of the [U.htm#uterus uterus], such as the ovaries, fallopian tubes, and abdominal cavity.
endometrium
The epithelium lining of the non-pregnant [U.htm#uterus uterus]. During pregnancy this epithelium undergoes changes described as the decidual reaction and is renamed the "decidua".
(More? Week 1 Notes | Human Menstrual Cycle)
epigenetics
(Greek, epi = above, upon) gene silencing that occur without changes in the genes (DNA) sequence, this changes can also be inherited.
(More? Molecular Mechanisms - Epigenetics | DNA Introduction | Science - Epigenetics: A web tour | The Welcome Trust - Epigenetics)
estrogens
Sex hormone found in both male and female. In the female, this hormone is produced by the ovaries and is responsible for development of secondary feminine sex characteristics. Together with progesterone these hormones also regulate changes that occur each menstral cycle. In the male, Leydig cells produce estrogen into the rete testis fluid at variable levels in different species. During male embryonic development exposure to high levels of estrogen can lead to genital abnormalities.
estrous cycle
The cyclic alterations in animal female tract and in sexual receptivity related to hormone changes. When searching both American (estrous) and British (oestrous) spellings are used in the literature.
(More? Menstrual Cycle - Estrous Cycle | Mouse estrous cycle)
gametes
(Greek, gamos = marriage) A specialized reproductive cell through which sexually reproducing parents pass chromosomes to their offspring; a sperm or an egg.
(More? Week 1 Notes)
gamete intrafallopian transfer
see GIFT
(More? In Vitro Fertilization Notes)
gameteogenesis
The production of either the haploid germ cells of spermatazoa (male) or eggs (female).
(More? Week 1 Notes)
genitalia
(Latin, genitalia = ) The term used to describe either the external or internal male and female sexual and reproductive organs.
(More? Urogenital Notes)
haploid
(Greek, haploos = single) Having a single set of chromosomes as in mature germ/sex cells (egg, spermatazoa). Normally cells are diploid, containing 2 sets of chromosomes.
(More? DNA Notes)
human chorionic gonadotrophin
(hCG) Placental hormone initially secreted by cells (syncitiotrophoblasts) from the implanting conceptus during week two, supporting the ovarian corpus luteum, which in turn supports the endometrial lining and therefore maintains pregnancy. Hormone can be detected in maternal blood and urine and is teh basis of many pregnancy tests. Hormone also stimulates the onset of fetal gonadal steroidogenesis, high levels are teratogenic to fetal gonadal tissues.
(More? Placenta Notes | Week 2 Notes)
last menstrual period
(LMP) Clinical term used to describe the menstrual period that occurs before a pregnancy and is used as the date to calculate clinical pregnancy development (gestational age). Note that in humans this is approximately two weeks different from embryonic development, which begins at [F.htm#fertilization fertilization] around the mid-point of the menstrual cycle.
Leydig cells
(interstitial cells) Testis (male gonad) cell which secrete testosterone, beginning in the fetus. These cells are named after Franz von Leydig (1821 - 1908) a German scientist who histologically described these cells.
(More? Testis Development | Spermatozoa Development)
male factor
Any cause of infertility due to deficiencies in sperm quantity, function, or motility (ability to move) that make it difficult for a sperm to fertilize an egg under normal conditions.
(More? Week 1 Notes)
manchette
A transient microtubule structure formed in spermatids involved in the process of assembly of the mammalian sperm tail and mechanical shaping and condensation of the sperm nucleus.
(More? Spermatozoa Development)
mediastinum testis
(Latin, medialis = middle) A single conical mass of connective tissue within the testis (male gonad) which extends from the tunica albuginea (cortical thick capsule surrounding the testis) into the seminiferous tubule region (medullary). Embedded within this connective tissue are the rete testis component of the duct conduction system for spermatazoa (Spermatozoa Duct Pathway: seminiferous tubule ‚ straight tubule ‚ rete testis ‚ ductuli efferentes ‚ ductus epididymidis ‚ ductus deferens)
(More? Testis Development | Spermatozoa Development)
medullary
(Latin, medialis = in the middle) Term relating to the medulla; pith, marrow, inner portion of an organ. Usually combined with cortex (cortical) meaning the outer layer.
meiosis
The cell division that occurs only in production of germ cells where there is a reduction in the number of chromosomes (diploid to haploid) which is the basis of sexual reproduction. Note all other non-germ cells divide by mitosis.
(More? Week 1 Notes)
meiotic sex chromosome inactivation
(MSCI) The process of transcriptional silencing of the X and Y chromosomes that occurs only during male meiotic spermatogenesis. This is a specialised form of [#MSUC meiotic silencing of unsynapsed chromatin]. This specific silencing has also be called the second form of X chromosome inactivation, the first form occurs in all female embryo cells.
(More? Meiotic sex chromosome inactivation. Turner JM. Development. 2007 May;134(10):1823-3
membrana granulosa
The granulosa cells that line the developing follicles of the ovary. These cells proliferate to form the stratum granulosa and other granulosa cells are given specific names based upon their position within the follicle. In the antral follicle, membrana granulosa sits on the follicular basal lamina and lines the antrum as a stratified epithelium. The [C.htm#cumulus_oophorus cumulus oophorus] is a column of granulosa cells that attaches the oocyte to the follicle wall. The [C.htm#corona_radiata corona radiata] are the granulosa cells that directly surround the oocyte, and are released along with it at ovulation. Following ovulation the corona radiata provide physical protection to the oocyte and granulosa cells within the ovulating follicle contribute to [C.htm#corpus_luteum corpus luteum].
(More? Week 1 - Oogenesis)
menopause
(Greek, mene = moon, men = month, pause = end or cessation) The decrease in ovarian production of estrogen and progesterone leading to cessation of menstrual cycles, decrease in fertility, and end of female reproductive life. Usually occurs in the mid-40's, the term was first used by the French physician, de Gardanne in 1812.
(More? Human Menstrual Cycle | Medline Plus - Menopause)
menorrhagia
Term used to describe heavy menstrual bleeding, is common in women of reproductive age (WHO data, affects 1011 out of 5322 women).
(More? Human Menstrual Cycle)
menstrual age
The gestation time calculated from the first day of the last menstrual period (LMP) prior to [F.htm#fertilization fertilization]. In humans, this differs from embryonic age by approximately two weeks.
(More? Week 1 Notes)
menstrual cycle
The human reproductive cycle, an endocrine regulated change in female anatomy and physiology that occur over 28 days (4 weeks, a lunar month) during reproductive life (between puberty and menopause). This cycle ceases during pregnancy and differs from other non-primate vertebrates (eg rats, mice, horses, pig) females that have a reproductive cycle called the estrous cycle (oestrous, British spelling).
(More? Human Menstrual Cycle | Estrous Cycle)
mitosis
The normal division of all cells, except germ cells, where chromosome number is maintained. Note germ cell division (egg, sperm) is reductive meiotic division.
(More? Week 1 Notes)
Mullerian Inhibiting Substance
(MIS, Anti-Mullerian Hormone, AMH, Mullerian inhibiting hormone, MIH). A sertoli cell secreted glycoprotein (transforming growth factor-beta, TGF-beta superfamily) that regulates gonadal and genital tract development. The main role is to inhibit paramesonephric (Mullerian) duct development in males. Postnatally, after puberty it is also expressed in females by ovarian granulosa cells and has a role in follicle development.
(More? OMIM - AMH)
oocyte
(Greek, oo = egg, ovum) The term used to describe the haploid egg or ovum formed within the ovary (female gonad) and released to enter the uterine tube and be transported to the [U.htm#uterus uterus]. The mature oocyte is the cell released from the ovary during ovulation.
(More? Week 1 - Oogenesis)
oogenesis
(Greek, oo = egg + genesis = origin, creation, generation) process of diploid oogonia division and differentiation into an haploid oocyte (egg) within the ovary (female gonad). Mammalian meiosis will only be completed within the oocyte if [F.htm#fertilization fertilization] occurs.
(More? Week 1 - Oogenesis)
oogonia
(Greek, oo = egg) diploid germ cells within the ovary (female gonad) which provide the primary oocytes for oocyte (egg) formation. In humans, all oogonia form primary oocytes within the ovary before birth.
(More? Week 1 - Oogenesis)
oophorus
(Greek, oo = egg + phorus = carrying, egg-bearing) cumulus oophorus, used to describe the granulosa cells within the follicle that tether or link the oocyte to the wall of the follicle.
(More? Week 1 - Oogenesis)
ovarian factor
A cause of infertility due to problems with egg production by the ovaries.
(More? Week 1 - Oogenesis)
ovarian hyperstimulation syndrome
(OHSS) Condition associated with fertility drugs for in vitro fertilization and other reproductive abnormalities.
(More? Week 1 - In Vitro Fertilization | Medlineplus - OHSS)
ovarian monitoring
The use of ultrasound and/or blood or urine tests to monitor ovarian follicle development and hormone production.
(More? Week 1 Notes | Week 1 - Oogenesis)
ovarian stimulation
The use of drugs to stimulate the ovaries to develop follicles/eggs. (More? Week 1 - Oogenesis | Human Menstrual Cycle)
ovary
The two female gonads where female germ cells (oocytes, eggs) are generated and also the source of estrogen and progesterone the female hormones regulating secondary sex characteristics and menstrual cycle uterine changes. The ovary is embryonically formed from primordial germ cells entering region of the paired mesonephric ducts (Wolffian ducts) which are lost in females.
(More? Week 1 Notes | Week 1 - Oogenesis | Human Menstrual Cycle)
oviduct
(uterine horn, fallopian tube, oviduct, salpinx) see [#uterine_tube uterine tube]. A pair of tubular structures designed to transport the oocyte (egg) from the ovary to the [U.htm#uterus uterus] body.
(More? Week 1 - Oogenesis | Week 1 Notes | Blue Histology - Female Reproductive System)
ovulation
The term used to describe the process of the mature follicle releasing the oocyte or ovum (and support cells) from the ovary surface into the peritoneal cavity. In humans, generally a single oocyte is released from a cohort of several maturing follicles. More than one follicle may be released (superovulation) following reproductive therapeutic treatment.
(More? Week 1 - Oogenesis | Week 1 Notes)
rectouterine pouch
(Pouch of Douglas or rectovaginal) Anatomical description of the female peritoneal cavity lying between the back wall of the [U.htm#uterus uterus] and rectum.
reductive division
Term describing meiosis where diploid DNA content becomes haploid (halved).
rete ovarii
A group of epithelial tubules located at the hilum of the ovary possibly mesonephric origin.
(More? Urogenital Notes)
rete testis
The duct (epithelial tubules) conduction system for spermatazoa embedded within the mediastinum (connective tissue) located in the center of the testis (male gonad) derived from the mesonephric duct, and allow spermatazoa to travel from the seminiferous tubules to the vasa efferentia. (Spermatozoa Duct Pathway: seminiferous tubule ‚Üí straight tubule ‚Üí rete testis ‚Üí ductuli efferentes ‚Üí ductus epididymidis ‚Üí ductus deferens)
(More? Testis Development | Spermatozoa Development)
RU 486
RU 486 (or Mifepristone) is a steroid hormone similar in structure to the natural hormone progesterone, which is used as a birth control drug.
(More? RU486)
Sertoli cells
The supporting cells in the testes (male gonad) that induce primordial germ cells to commit to sperm development. Support is nutritional and mechanical, as well as forming a blood-testis barrier. In development these cells secrete anti-Müllerian hormone, which causes the Müllerian (paramesonephric) duct to regress, and help to induce other somatic cells to differentiate into Leydig cells. The cells are named after Enrico Sertoli (1842 - 1910), and italian physiologist and histologist.
(More? Testis Development | Spermatozoa Development)
sperm
The male haploid reproductive cell, often used generically (and incorrectly) to describe these cells and the fluid of the ejaculate. Term is a shortened form of scientifically correct term #spermatazoa spermatazoa.
(More? Testis Development | Spermatozoa Development)
spermatazoa
The male haploid reproductive cell, produced by meiosis in the testis (male gonad).
(More? Testis Development | Spermatozoa Development)
spermatogenesis
(Greek, genesis = origin, creation, generation) The term used to describe the process of diploid spermatagonia division and differentiation to form haploid spermatazoa within the testis (male gonad). The process includes the following cellular changes: meiosis, reoorganization of DNA, reduction in DNA content, reorganization of cellular organelles, morphological changes (cell shape). The final process of change in cell shape is also called [#spermiogenesis spermiogenesis].
(More? Week 1 - Spermatogenesis)
spermiogenesis
(Greek, genesis = origin, creation, generation) The maturation process of the already haploid spermatazoa into the mature sperm shape and organization. This process involves reorganization of cellular organelles (endoplasmic reticulum, golgi apparatus, mitochondria), cytoskeletal changes (microtubule organization) and morphological changes (cell shape, acrosome and tail formation).
(More? Testis Development | Spermatozoa Development)
spermatogonia
The cells located in the seminiferous tubule adjacent to the basal membrane that either divide and separate to renew the stem cell population, or they divide and stay together as a pair (Apr spermatogonia) connected by an intercellular cytoplasmic bridge to differentiate and eventually form spermatazoa.
(More? Testis Development | Spermatozoa Development)
spermatogonial stem cells
The spermatagonia cells located beside the seminiferous tubule basal membrane that either divide and separate to renew the stem cell population, or they divide and stay together as a pair (Apr spermatogonia) connected by an intercellular cytoplasmic bridge to differentiate and eventually form spermatazoa.
(More? Testis Development | Spermatozoa Development)
sry
(Sry, human; Testis-Determining Factor, TDF; Testis-Determining Factor on Y, TDY ) Gene name ====s====ex-determining ====r====egion of ====Y====, the gene locus on the Y chromosome encoding the male "testis determining factor", a protein transcription factor and a member of the high mobility group (HMG)-box family of DNA binding proteins. See also the transcription factor SRY-related protein, SOX9 (SRY-related high-mobility group (HMG) box 9)
(More? Molecular Notes | Week 1 Notes | OMIM)
stimulated cycle
An ART cycle in which a woman receives drugs to stimulate her ovaries to produce more follicles.
(More? Week 1 Notes)
stroma
(Greek, stroma = "a cover, table-cloth, bedding") Histological term used to describe supportive cells within an organ, tissue or structure. The term is often paired with [P.htm#parenchyma parenchyma], which describes the functional cells of an organ, tissue or structure. All organs can therefore be functionally divided into these 2 components, stromal/parenchymal.
stromal cells
(Greek, stroma = "a cover, table-cloth, bedding") Descriptive term in the ovary, for cells surrounding the developing follicle that form a connective tissue sheath (theca folliculi). This layer then differentiates into 2 layers (theca interna, theca externa). This region is vascularized and involved in hormone secretion.
testes
(Latin testis = "witness") The two male gonads (singular testis) where male germ cells (spermatozoa) are generated and also the source of testosterone (male hormone). Embryonically formed from primordial germ cells entering region of the paired mesonephric ducts (Wolffian ducts) which are preserved in male gonad development and lost in females.
(More? Testis Development)
testis
(Latin testis = "witness", plural testes) The male gonad where male germ cells (spermatozoa) are generated and also the source of testosterone (male hormone). Embryonically formed from primordial germ cells entering region of the paired mesonephric ducts (Wolffian ducts) which are preserved in male gonad development and lost in females.
(More? Testis Development)
testis-determining factor
(TDF, Sry, Testis-Determining Factor on Y, TDY ) Protein name for the protein transcription factor product of the Sry gene on the Y chromosome responsible for maleness. This protein is a member of the high mobility group (HMG)-box family of DNA binding proteins. See also the transcription factor SRY-related protein, SOX9 (SRY-related high-mobility group (HMG) box 9)
(More? Molecular Notes | Week 1 Notes | OMIM)
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
- 2010 BGD: Lecture 1 | Lecture 2 | Practical 3 | Practical 6 | Practical 12
Cite this page: Hill, M.A. (2024, April 24) Embryology 2010 BGD Practical 3 - Week 3 Summary. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/2010_BGD_Practical_3_-_Week_3_Summary
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G